Regional Anaesthesia
KEY POINTS
- Serratus plane block is a simple, effective and safe thoracic fascial plane block.
- Its clinical effect is likely to be due, at least in part, to blockade of the lateral cutaneous branches of the intercostal nerves.
- Indications include breast surgery, chronic pain after mastectomy, rib fractures, thoracoscopy and thoracotomy.
- The exact point of injection and the volume of injectate are important determinants of the spread of local anaesthetic.
- It is a regional anaesthesia technique amenable to the insertion of a catheter.
INTRODUCTION
Before the advent of ultrasound-guided regional anaesthesia, chest wall blocks were mainly confined to intercostal nerve blockade, thoracic epidural analgesia and thoracic paravertebral blockade.1 The use of ultrasound in regional anaesthesia has facilitated the visualisation of anatomical structures, needle advancement and the spread of local anaesthetic. This has led to the further development and refinement of fascial plane blocks, in which local anaesthetic is injected into a tissue plane rather than around individual nerves. Introduced by Blanco et al,2 serratus plane block (SPB) is a novel form of ultrasound-guided regional anaesthesia fascial plane block that can achieve paraesthesia of the hemithorax.
In this tutorial, we will provide an overview of the SPB, considering the anatomy, indications, sonoanatomy and technique. It should be noted that many names, such as serratus intercostal plane block, do exist in the published literature for what is, in fact, a similar if not same regional anaesthetic technique to SPB, targeting the same tissue plane, but with only subtle differences in ultrasound probe placement and/or needle trajectory.
ANATOMY AND INNERVATION
Each thoracic nerve, at its exit from the intervertebral foramen, divides into a dorsal and a ventral ramus. The dorsal ramus follows a course posteriorly through the costotransverse foramen. The ventral ramus moves laterally as the intercostal nerve, initially deep to the internal intercostal membrane and then in the plane between the internal and the innermost intercostal muscle on the inner aspect of the rib. Just posterior to the angle of the rib, the lateral cutaneous branch arises from the
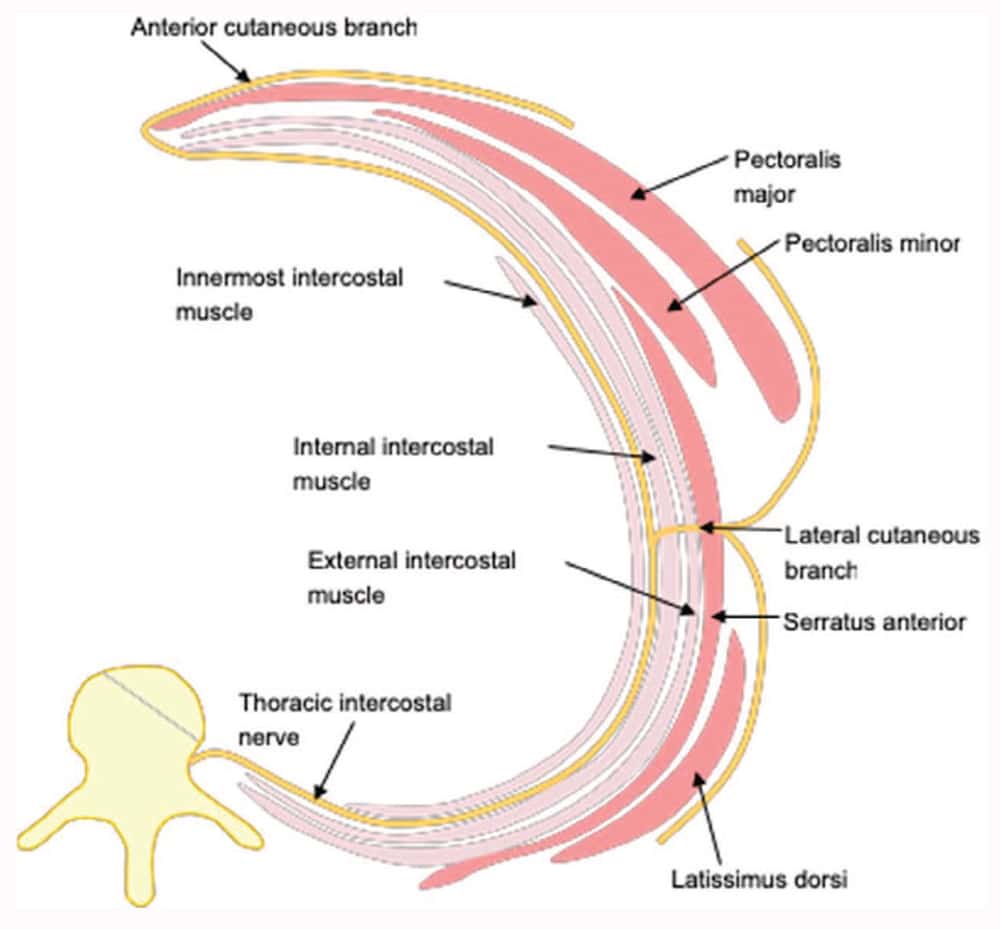
Figure 1. Axial cross-sectional illustration demonstrating the anatomy of the intercostal nerve and the surrounding structures.
intercostal nerve, piercing the intercostal and the serratus anterior muscles and dividing into its anterior and posterior branches (Figure 1). The remainder of the intercostal nerve continues to run forward in the intercostal space and terminates as the anterior cutaneous branch, piercing through the transverse thoracic muscle lateral to the sternum. Cutaneous innervation medial to the midclavicular line is derived from the anterior division of the lateral cutaneous branch of the intercostal nerve and the anterior cutaneous branch of the intercostal nerve. Sensory innervation lateral to the midclavicular line is derived from the posterior division of the lateral cutaneous branch of the intercostal nerve.
On the lateral aspect of the chest wall, the serratus anterior muscle originates from the lateral parts of the first to the eighth ribs and attaches to the costal surface of the medial border of the scapula. It is innervated by the long thoracic nerve. Medially, the pectoralis minor muscle, innervated by the medial pectoral nerve, lies superficial to the serratus anterior muscle. Laterally, the latissimus dorsi muscle, innervated by the thoracodorsal nerve, is located superficial to it. Deep to the serratus anterior muscle are the intercostal muscles and the ribs.
ANATOMICAL EVALUATION OF CLINICAL EFFECT
In SPB, local anaesthetic is injected into the fascial plane either superficial to the serratus anterior muscle, between the latissimus dorsi and serratus anterior muscles, or deep to the serratus anterior muscle, between the serratus anterior muscle and intercostal muscles and ribs. It can be performed in the area delineated by the anterior and posterior axillary lines and the second to seventh ribs.
In its initial evaluation, a single-shot injection of local anaesthetic superficial or deep to the serratus anterior muscle provided reliable ipsilateral anaesthesia from T2 to T9 in volunteers (Figure 2).2 It appears that this clinical effect is likely to be consequent, at least in part, to blockade of the lateral cutaneous branches of the intercostal nerves, as evidenced by cadaveric studies.3 The intercostobrachial nerve, long thoracic nerve and the thoracodorsal nerve are located deep to the latissimus dorsi muscle and superficial to the serratus anterior muscle. Of interest, the medial and lateral pectoral nerves were not often stained by dye after SPB.4
In the four patients included in the initial study, the mean duration of paraesthesia was demonstrated to be longer after injection superficial compared with deep to the serratus anterior muscle at 752 minutes and 386 minutes, respectively.2 It is still not clear, however, whether the injection of local anaesthetic superficial or deep to the serratus anterior muscle causes any clinically significant difference in the effectiveness or the duration of regional blockade. In a small case series examining the effect of SPB in postmastectomy pain syndrome, three of the four patients had previously had a superficial SPB that was not as effective as a deep SPB.5 In a cadaveric study, on the other hand, the plane of injection, whether superficial or deep to the serratus anterior muscle, did not influence the anteroposterior, cephalocaudal or total surface area of injectate spread.6
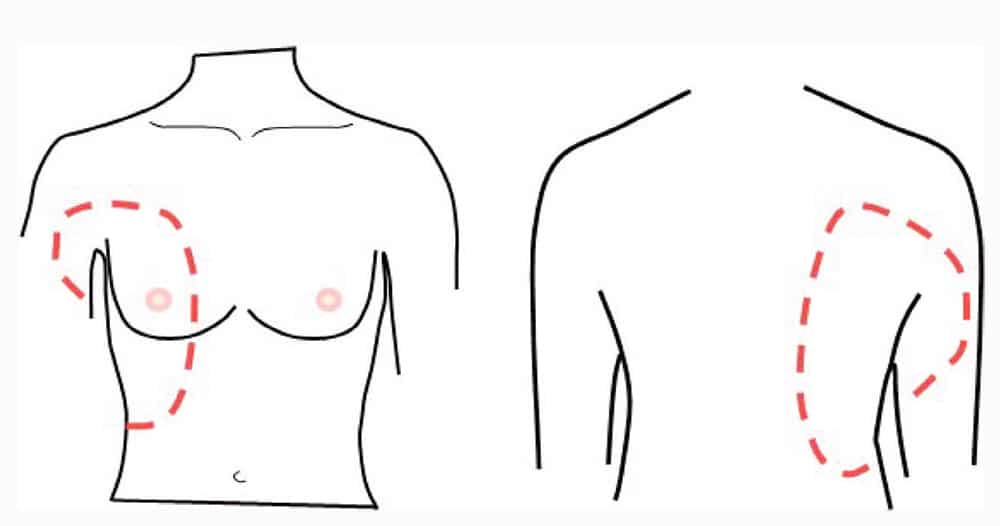
Figure 2. Illustration of the expected area of sensory loss following serratus plane block.
Further, in a cohort study of patients having surgery for breast cancer, deep SPB was found to be non-inferior to superficial SPB with respect to pain scores at rest and postoperative oral morphine equivalent consumption.7 Some concerns have been raised, however, about the intraoperative distortion of patient anatomy, interfering with surgery, subsequent to a superficial versus a deep SPB.
The volume of injectate is an important determinant of its spread. In a cadaveric study, doubling the volume of injectate from 20 mL to 40 mL was associated with greater cephalocaudal spread and a similar increase in the area of spread, but it did not influence posterior spread.6 Moreover, in a randomised controlled trial in patients undergoing surgery for breast cancer, increasing the volume of 0.375% ropivacaine from 20 mL to 40 mL was related to greater dermatomal block in the cephalocaudal distribution yet did not extend the time to first postoperative analgesic rescue dose.8
COMPARISON WITH OTHER REGIONAL ANAESTHESIA TECHNIQUES
SPB avoids some of the contraindications, potential complications, adverse effects and disadvantages associated with other regional anaesthesia modalities, such as intercostal nerve blockade, thoracic epidural analgesia and thoracic paravertebral blockade, as well as providing some advantages of its own.9 It is a superficial technique, amenable to catheter insertion, that is simple to learn and perform in the supine position, without the need for repositioning of the patient. On the one hand, unlike neuraxial techniques, SBP can be performed in patients with coagulopathy, sympathetic block with resultant hypotension is not produced and complications of neurological injury should be theoretically less likely and severe. On the other hand, neuraxial techniques can provide bilateral analgesia and result in a larger area of anaesthesia due to more proximal block of the nerves close to their exit from the intervertebral foramen, involving all branches of the intercostal nerves and the dorsal rami. SPB remains a relatively novel modality, and its comparative effectiveness to other more well-established regional techniques has not been fully determined.
Comparison With PECS I and II
In common with SPB, PECS I and II are fascial plane blocks. PECS I consists of an interpectoral injection between the pectoralis major and minor muscles, and PECS II involves the same interpectoral injection as well as an additional subpectoral injection between the pectoralis minor and serratus anterior muscles.10,11 PECS I causes blockade of the medial and the lateral pectoral nerves, while PECS II results in blockade of these nerves as well as those affected by SPB, the intercostobrachial nerve, lateral cutaneous branches of the intercostal nerve, long thoracic nerve and the thoracodorsal nerve (Table 1). Consideration should be given to the different nerves that need blockade for any particular operative surgery, such as mastectomy, in choosing between SBP and PECS I and II for the provision of perioperative analgesia.
INDICATIONS
It should be considered that the evidence for SPB is best in the context of breast and thoracic surgery but is limited to case reports and series for indications such as rib fractures. Nevertheless, the evidence base for SPB continues to develop, with an increasing number of reported indications to include cardiac device implantation and upper abdominal incisions:
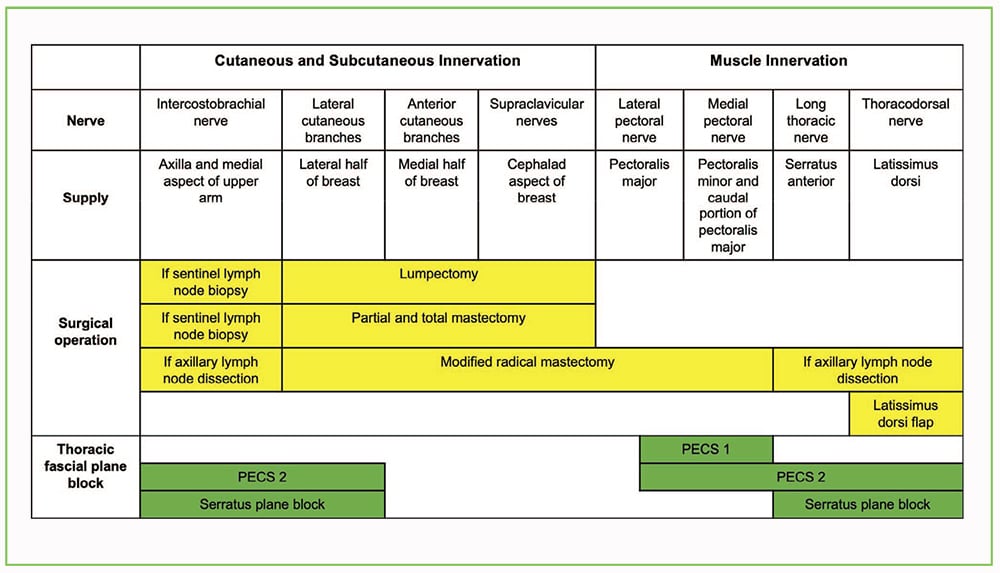
Table 1. Summary of the innervation of the chest, nerves involved in different breast surgeries and nerves blocked with the various thoracic fascial plane blocks
- Breast Surgery
- Chronic pain after mastectomy
- Rib fracture(s)
- Thoracoscopy
- Thoracotomy
CONTRAINDICATIONS
Absolute
- Patient refusal
- Allergy to local anaesthetics
Relative
- Coagulopathy, in which an individualised risk-benefit analysis of the regional anaesthesia technique for the patient should be evaluated
- Disruption of the local anatomy, secondary, for instance, to the presence of chest drains or surgical emphysema, resulting in difficulty in ultrasound interpretation and distortion of tissue planes
HOW TO PERFORM A SPB
Preparation
Consistent with all regional anaesthesia blocks, the patient must have intravenous access and standard monitoring, including electrocardiogram, non-invasive blood pressure and oxygen saturation probe, applied. In addition to the anaesthetist conducting the SPB, appropriately trained personnel should be present, and resuscitation facilities must be available. In order to decrease the risk of wrong-side and/or wrong-site block, the World Health Organization surgical safety checklist and Stop Before You Block initiative should be followed.12 In the performance of the SPB, standard aseptic precautions must be followed, and the patient and the ultrasound machine should be positioned in an ergonomic manner (Table 2).

Table 2. Characteristics of the performance of the serratus plane block
Ultrasound Probe Position and Sonography
SPB is a progression from the PECS block with similar initial anatomical landmarks and ultrasound imaging steps.10,11 The reader is encouraged to review the tutorial for the PECS block (ATOTW Tutorial 346, PECS Blocks) before proceeding to review this part of the tutorial on SPB13:
- Commence the ultrasound scan by placing the ultrasound probe in a parasagittal plane immediately inferior to the clavicle and in the deltopectoral groove adjacent to the coracoid process. Here, identify the pectoralis major and minor muscles, the axillary artery and vein as well as the underlying second rib.
- Move the ultrasound probe inferiorly and posteriorly with increasing coronal orientation until the fifth rib is found in the midaxillary line (Figure 3). In this position, identify a superficial and thick muscle, the latissimus dorsi, overlying the deeper serratus anterior muscle (Figure 4). Since the thoracodorsal artery is located in the fascial plane between the latissimus dorsi and the serratus anterior muscles, its identification with ultrasound imaging and use of colour Doppler is helpful to delineate the plane and decrease the risk of inadvertent accidental arterial puncture on introduction of the needle.
Needling Technique
- Prior to the insertion of the needle, identify the location of the pleura
- Introduce the needle in plane, advancing it from a superoanterior to posteroinferior direction.
- If performing a superficial SPB, use hydrolocation with either local anaesthetic or saline to confirm the needle tip is positioned in the space between the latissimus dorsi and the serratus anterior muscles in the mid-axillary line.
- If performing a deep SPB, direct the needle toward the fifth rib, as this will form a bony safety back stop and reduce the risk of puncture of the pleura. Use hydrolocation with either local anaesthetic or saline to verify the needle tip is positioned in the space between the serratus anterior muscle and the fifth rib in the mid-axillary line.
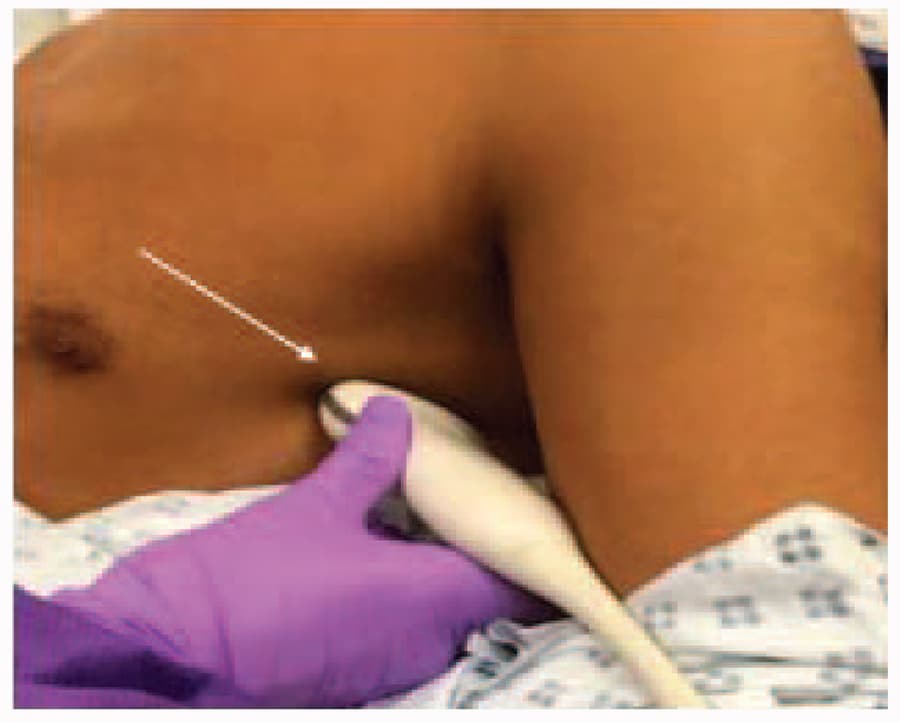
Figure 3. Ideal ultrasound probe position for the serratus plane block at the level of the fifth rib in the mid-axillary line. The arrow indicates the point of insertion and the direction of the needle.
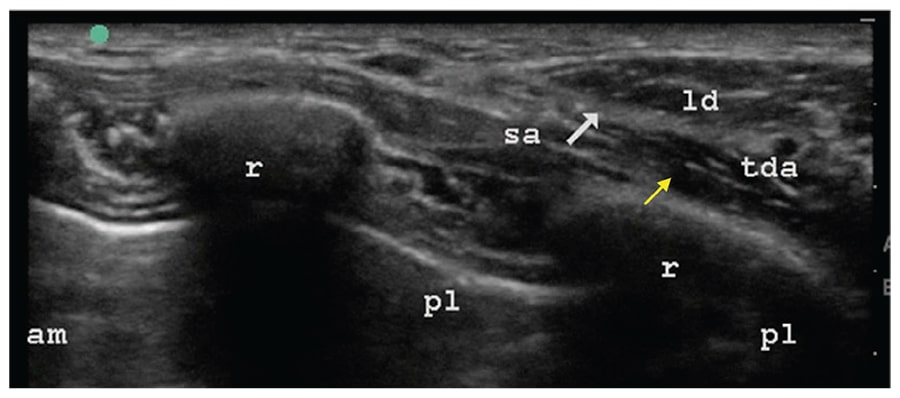
Figure 4. Ultrasound image demonstrating the serratus anterior muscle deep to the latissimus dorsi muscle and superficial to the ribs and the intercostal muscles. The yellow arrow indicates the fascial plane between the serratus anterior muscle and the rib, where the local anaesthetic should be deposited for the deep serratus plane block. The white arrow points to the fascial plane between the serratus anterior and the latissimus dorsi muscles, where the local anaesthetic should be deposited for the superficial serratus plane block. am, anteromedial; ld, latissimus dorsi; pl, posterolateral; r, rib; sa, serratus anterior; tda, thoracodorsal artery.
- Once the needle tip is in a satisfactory position and subsequent to negative aspiration, taking into account the potential for multiple small blood vessels to be present here, inject the remainder of the local anaesthetic and in small aliquots of 5 mL (Figures 5 and 6).
- Given that SPB is a fascial plane block, the distribution of analgesia is dependent on the diffusion of local anaesthetic and therefore its volume. In view of this, a minimum local anaesthetic volume of 20 mL should be used, adjusting the concentration of local anaesthetic if needed so that the maximum recommended dose is not exceeded.
If it is required, bilateral SPBs can be undertaken, but the maximum recommended dose of local anaesthetic must not be exceeded, and should moderate to severe postoperative pain be anticipated for more than 12–16 hours, a catheter can be considered for insertion.
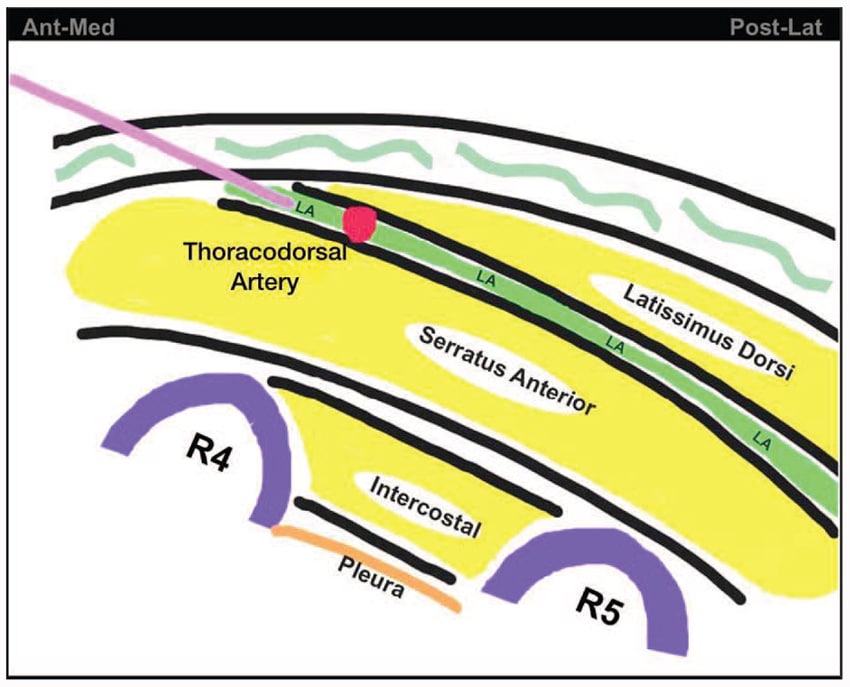
Figure 5. Illustration of the ultrasound image obtained for the performance of the serratus plane block. The line indicates the needle trajectory with the in-plane needling technique. LA, local anaesthetic; R4, fourth rib; R5, fifth rib.
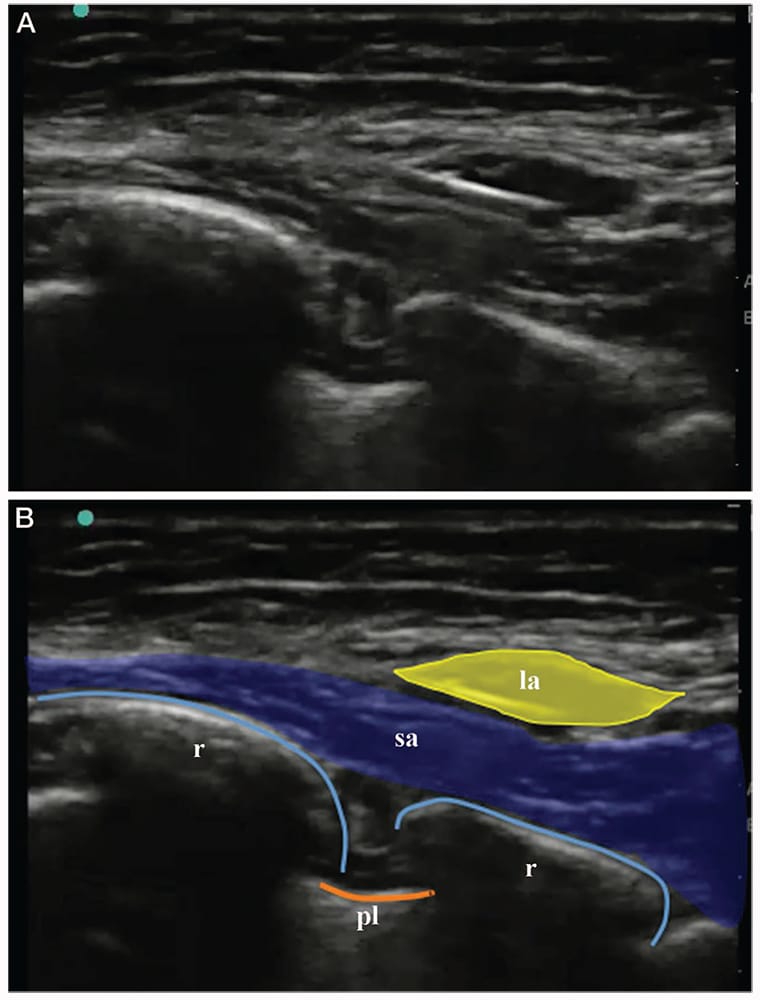
Figure 6. Ultrasound images showing the distension and the opening up of the fascial plane between the serratus anterior and the latissimus dorsi muscles subsequent to the injection of local anaesthetic. la, local anaesthetic; pl, pleura; r, rib; sa, serratus anterior.
COMPLICATIONS
Generic
- Bleeding, bruising and/or haematoma
- Difficulty and inadequate or failed block
- Intravascular injection
- Local anaesthetic systemic toxicity
- Infection
Specific
- Pneumothorax, secondary to the proximity of the pleura
CLINICAL PEARLS
- Identify the main anatomical landmarks, the latissimus dorsi and the serratus anterior muscles as well as the ribs and the pleura.
- To avoid inadvertent intravascular injection, use colour Doppler to identify blood vessels and aspirate before injection.
- Find the thoracodorsal artery as its identification can be helpful to delineate the plane superficial to the serratus anterior muscle.
- If performing superficial or deep SPB, use hydrolocation to confirm the correct position of the needle tip.
- When performing deep SPB, direct the needle toward the fifth rib to reduce the risk of puncturing the pleura.
SUMMARY
In conclusion, SPB is a simple, effective and safe thoracic fascial plane block that is a valuable addition to the regional anaesthesia armamentarium of the anaesthetist and allied specialities. It still remains a relatively novel modality, and our understanding of its evidence-based indications as well as effectiveness relative to systemic analgesia and other regional anaesthesia techniques continues to increase.
REFERENCES
- Chin KJ. Thoracic wall blocks: from paravertebral to retrolaminar to serratus to erector spinae and back again—a review of evidence. Best Pract Res Clin Anaesthesiol. 2019;33:67-77.
- Blanco R, Parras T, McDonnell JG, et al. Serratus plane block: a novel ultrasound-guided thoracic wall nerve block. Anaesthesia. 2013;68:1107-1113.
- Mayes J, Davison E, Panahi P, et al. An anatomical evaluation of the serratus anterior plane block. Anaesthesia. 2016;71:1064-1069.
- Kunigo T, Murouchi T, Yamamoto S, Yamakage M. Spread of injectate in ultrasound-guided serratus plane block: a cadaveric study. JA Clin Rep. 2018;4:10.
- Piracha MM, Thorp SL, Puttanniah V, et al. ‘‘A tale of two planes’’: deep versus superficial serratus plane block for postmatectomy pain syndrome. Reg Anesth Pain Med. 2017;42:259-262.
- Biswas A, Castanov V, Perlas A, et al. Serratus plane block: a cadaveric study to evaluate optimal injectate spread. Reg Anesth Pain Med. 2018;43:854-858.
- Abdallah FW, Cil T, MacLean D, et al. Too deep or not too deep? A propensity-matched comparison of the analgesic effects of a superficial versus deep serratus fascial plane block for ambulatory breast cancer surgery. Reg Anesth Pain Med. 2018;43:480-487.
- Kunigo T, Murouchi T, Yamamoto S, et al. Injection volume and anesthetic effect in serratus plane block. Reg Anesth Pain Med. 2017;42:737-740.
- El-Boghdadly K, Wiles MD. Regional anaesthesia for rib fractures: too many choices, too little evidence. Anaesthesia. 2019;74:564-568.
- Blanco R. The ‘pecs block’: a novel technique for providing analgesia after breast surgery. Anaesthesia. 2011;66:847-848.
- Blanco R, Farjado M, Parras Maldonado T. Ultrasound description of pecs II (modified pecs I): a novel approach to breast surgery. Rev Esp Anestesiol Reanim. 2012;59:470-475.
- Slocombe P, Pattullo S. A site check prior to regional anaesthesia to prevent wrong-sided blocks. Anaesth Intensive Care. 2016;44:513-516.
- Parras T, Blanco R. Pecs blocks. https://resources.wfsahq.org/components/com_virtual_library/media/7ef4612aa547d759a2e 24087424e9bba-ATOTW346.pdf. Accessed 1 October 2019.



