Intensive Care Medicine
Introduction
Poisoning is a significant global public health problem. According to the World Health Organisation data, an estimated 350 000 people died from unintentional poisoning in 2002. Accidental poisoning occurs most often in the age group 1-5 years although less than one per cent of poisoning in children is serious. More than 94% of fatal poisonings occur in low- and middle-income countries. It remains a challenge to identify those at risk at an early stage. Education of the general public and also the provision of child-proof containers for household chemicals and medicines play a key role in prevention.
(Toxic plants, insect and snake bites are not discussed in this tutorial, but see www.rch.org.au/poisons for more information)
Questions
True or false:
- Emesis or nasogastric aspiration are indicated after sodium hydroxide ingestion.
- Regarding paraffin ingestion – abnormalities on the chest film may be seen in the absence of symptoms.
- A fever after paraffin ingestion is always due to a secondary infection.
- Ingestion of small amounts of paraquat is usually harmless.
- High FiO2 should be avoided in paraquat ingestion to prevent pulmonary fibrosis.
- Organophosphate forms an irreversible complex with cholinesterase.
- Carbon monoxide is irritant with a distinctive odour.
- The SpO2 reading in carbon monoxide poisoning is usually less than 85%.
- A plasma paracetamol level should be taken within 2 hours of ingestion.
- Iron poisoning is effectively treated with charcoal.
Accidental poisoning in children: general principles
A history of poisoning usually makes the diagnosis obvious but poisoning should be considered in any child presenting with altered consciousness, cardiorespiratory depression, hypothermia, seizures or gastrointestinal symptoms. The possibility of more than one poison should always be considered.

1. Household chemicals
Children frequently ingest household substances and most of these are nontoxic. However, some products contain alcohol which may cause seizures and hypoxia.
Household solutions of bleach contain approximately 10% hypochlorite. They are rarely ingested as they are extremely unpalatable. Commonly, they cause nausea, vomiting and diarrhoea. Less than 100ml of household bleach is unlikely to cause serious problems. Fluids should be encouraged, particularly milk. Oesophageal damage occurs rarely and is associated with concentrated solutions.
Ingestion of small quantities of strong alkalis such as drain cleaner containing sodium hydroxide may cause devastating injuries. Oesophageal injury is most common and evolves over the course of a few days. Ingestion causes immediate burning pain, swelling of the lips, and depending on the quantity ingested, salivation, haematemesis, dyspnoea, stridor or shock.
The burn injury is classified by endoscopy:
- mucosal (first degree burn) – usually resolves after 2-3 days
- submucosal (second degree burn) – requires total parenteral nutrition
- full thickness (third degree burn) – shocked, will require intensive care
Third degree burns may lead to gastrointestinal perforation or airway complications or long term, severe oesophageal stricture causing absolute dysphagia which evolves over a period of several months.
Treatment is supportive; emesis is contraindicated and nasogastric aspiration unhelpful as the injury is oesophageal. Patients with first degree burns may be discharged after 2-3 days once tolerating oral fluids. Patients with third degree burns will be in shock and will require intensive care: tracheostomy is indicated for patients with evidence of supraglottic/epiglottic burns. Steroids may reduce the risk of stricture formation if given within 12-24 hours but their use is controversial. Antibiotics are indicated for perforation. Long term gastrostomy or oesophageal replacement surgery (gastric pull-up) may be required for oesophageal stricture.
2. Hydrocarbons (Paraffin, white spirit)
Most of the hydrocarbons are petroleum distillates, containing a variable amount of saturated and unsaturated aliphatic (open-chain) and aromatic (cyclic) hydrocarbons. The aliphatics are not readily absorbed from the gastrointestinal tract and therefore cause minimal systemic toxicity. Paraffin, petrol, thinners, diesel and benzene are low viscosity aliphatic-based petroleum distillates.
The aromatic hydrocarbons are well absorbed, and therefore may cause systemic toxic affects but are less inclined to aspiration-related complications. The main hazard of accidental ingestion of the aliphatic hydrocarbons (paraffin) is that of chemical pneumonitis characterised by ventilation/perfusion imbalance and hypoxia. The aspirated hydrocarbons inhibit surfactant and also cause direct broncho-alveolar injury. This can occur even in the absence of vomiting or impaired consciousness and as little as 1ml aspirated hydrocarbon can result in a chemical pneumonitis.
Paraffin is often sold or stored in unlabeled containers which may be within children’s reach. Volumes ingested tend to be small because of a burning sensation in the mouth and the bad taste of the liquid. Nausea and vomiting are common. Aspiration pneumonitis occurs in 12-40% of patients. Signs and symptoms appear after 30 minutes of ingestion but may be delayed for 8 hours. A non-productive cough, tachypnoea and tachycardia are signs of a developing chemical pneumonitis. There may be wheeze, coarse crackles as well as signs of respiratory distress (intercostals and subcostal retraction). Hypoxia and cyanosis may be present in severe cases. Patients may be lethargic or irritable. A fever may also be present. The clinical picture generally deteriorates over the first 24 hours. A temperature that persists or only develops after 24 hours usually suggests a secondary infection.
Abnormalities on the chest film may be seen within 30 minutes after aspiration even in the absence of clinical signs or symptoms. Common radiological findings of chemical pneumonitis include bilateral perihilar infiltrates which progress to form patchy infiltrates and later become large areas of consolidation.
Management of hydrocarbon poisoning
- ABC principles
- Observe all asymptomatic patients for at least 8 hours. Carefully examine patients for the development of respiratory signs. A chest film at 6 hours is recommended.
- If asymptomatic after 8 hours and the chest film is normal, the patient may be discharged.
- Symptomatic patients should be x-rayed on admission.
- Emesis and gastric lavage is contra-indicated as it increases the risk of aspiration. The use of milk is not recommended but clear fluids are not contra-indicated.
- Oxygen should be administered to all patients with respiratory signs or symptoms. Other respiratory support modalities should be instigated as required, according to standard indications.
- Corticosteroid therapy may increase the risk of secondary bacterial
infection and has not been shown to be of any benefit. - Antibiotics should be given if there are suggestions of a secondary infection (persistent fever or a fever that develops after 24 hours.) Prophylactic antibiotics have not been shown to prevent secondary infection and are not advocated.
3. Pesticides
Paraquat
Paraquat ingestion remains a problem in a large number of countries. Most of these cases are intentional suicide attempts (73% in a Malaysian study) or occupational exposure and therefore not that frequently seen in the paediatric population. It is the most toxic herbicide known, producing multi-organ failure. After oral ingestion, patients develop a severe gastroenteritis with oral, oesophageal and gastric ulceration. Depending on the dose ingested, multiorgan failure may develop within 48-72 hours. As little as 10ml may be fatal. Those who survive the initial phase develop pulmonary fibrosis as a response to the acute alveolitis in the first phase. This leads to respiratory failure and patients die of anoxia.
Management of paraquat poisoning
- Any history of oral exposure should be considered potentially fatal. Treatment strategies are aimed at prevention of absorption, enhancement of elimination and prevention of pulmonary damage.
- Treat immediately with Fuller’s earth (Fuller’s earth 300g and magnesium sulphate 50g in a litre of water). Give 5-10ml/kg orally every 2-3 hours for 2-3 days.
- Activated charcoal may be used if Fuller’s earth is not available. Mix with saline and a laxative like lactulose to prevent constipation. Repeat every 4 hours until paraquat is no longer detected in the urine.
- If neither is available, careful gastric emptying may be done but be aware of possible pharyngeal and oesophageal ulceration and perforation
- Haemoperfusion or dialysis may be used (if available).
- Appropriate management of respiratory complications includes PEEP/CPAP. Low FiO2 should be used as high concentrations of oxygen lead to worse pulmonary toxicity. Paraquat accumulates in the lung where it generates superoxide anions through the reaction with oxygen.
Organophosphate poisoning
Organophosphate poisoning (OP) remains an issue in developing countries. In one study, 35% of OP poisoned victims were children.
The organophosphates and carbamates are cholinesterase inhibitors, thereby eliciting cholinergic signs and symptoms. They can be absorbed by ingestion, inhalation or via the skin. The organophosphates form an irreversible complex with cholinesterase but the carbamyl-enzyme complex is reversible. Thus a less severe clinical picture of shorter duration is presented. It also causes fewer CNS effects because of less penetration of the blood brain barrier.
OP poisoning causes:
- Muscarinic effects – hypersecretion, vomiting, diarrhoea, constricted pupils, bronchoconstriction and urinary incontinence.
- Nicotinic effects – muscular weakness, fasciculations and respiratory muscle weakness (may override muscarinic effect and cause tachycardia, hypertension and mydriasis).
- CNS effects – irritability, seizures, coma (and accompanying respiratory depression).
Management of organophosphate poisoning
- ABC
- Patient may require intubation (avoid suxamethonium because of prolonged effect)
- Gastric lavage, activated charcoal.
- Remove all contaminated clothes (take care not to get exposed yourself)
- Wash patient with soap and water.
- Start intravenous atropine administration as soon as possible. Initial test dose of 0.01mg/kg. Then 0.05mg/kg every 15 minutes until full atropinisation is reached. Maintenance therapy is usually around 0.05mg/kg/hr. Adequate therapy is achieved when there is control of excessive bronchial and oral secretions. When the patient improves, the dose should be tapered slowly over 24 hours. Atropine should never be stopped abruptly. Close observation is required as rebound organophosphate toxicity may occur due to their lipid solubility.
- Watch out for chemical aspiration pneumonia as a lot of the organophosphate pesticides have a petroleum base.
4. Inhaled poisons
Carbon monoxide
Carbon monoxide is produced through incomplete combustion processes. It is colourless, tasteless and non-irritant. The commonest sources of carbon monoxide poisoning are smoke inhalation, poorly maintained domestic gas appliances and deliberate inhalation of car exhaust fumes (less common in children). Carbon monoxide causes tissue hypoxia by the interruption of electron transport in the mitochondria. It also reduces oxygen delivery by competing with O2 for binding to Hb and altering the shape of the HbO2 dissociation curve (making it less sigmoidal, a shift to the left). Its affinity for Hb is >200-fold that of O2.
Carbon monoxide causes injury by hypoxia, with symptoms referable to tissues with greatest oxygen consumption, notably the heart and brain. Patients present with hypoxia without cyanosis. Skin and mucosal surfaces may appear cherry red. Symptoms correlate roughly with the COHb level:
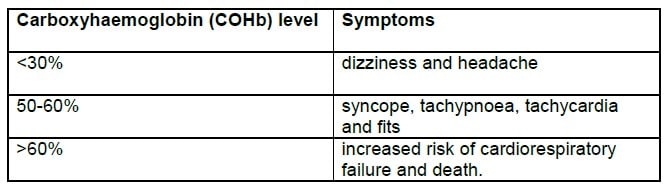
Anaemia, increased metabolic rate (e.g. children) and underlying ischaemic heart disease all increase susceptibility to CO. Neurological recovery depends on the duration of hypoxic coma.
Management of carbon monoxide poisoning
- Pulse saturation monitoring does not distinguish between HbO2 and COHb and will read falsely high.
- Arterial blood gases should be done. PO2 may be normal but any evidence of metabolic acidosis indicates serious poisoning (useful even in the absence of COHb measuring facilities.) COHb measurements are diagnostic but not always available.
- Treat according to ABC principles.
- Apply tight-fitting mask with 100% oxygen. This reduces the half life of COHb from 320 mins (in room air) to 80 minutes. Intubation and ventilation may be necessary in severe cases.
- Hyperbaric oxygen is useful but access and transfer times to a hyperbaric chamber make it an impractical option.
- Check 12 lead ECG – if there are signs of myocardial ischaemia, the patient needs intubation/ventilation.
- Supportive care should include continuous cardiac monitoring, treatment of arrhythmias and correction of acid/base and electrolyte abnormalities.
- Lab bloods should be done for UE, FBC, CPK and cardiac enzymes.
- Brain hypoxia leads to cerebral oedema and fits. Diazepam 5-10mg iv is used to control the fits.
- Initial CXR may be normal even in severe smoke inhalation.
Patients need to be followed up as some of the neuropsychiatric complications may take weeks to develop.
Combustion of household materials can also generate a number of other toxic substances such as sulphur dioxide, nitrogen dioxide, acrolein, cyanide and various acids from PVC and polyurethane. This may cause direct lung, skin and conjunctival injury.
Cyanide poisoning
Most commonly seen in victims of smoke inhalation as a combustion product of polyurethane foams. Cyanide derivates are also used in industrial processes and fertilizers. Children may ingest amygdalin, a cyanogenic glycoside contained in kernels of almonds and cherries.
Cyanide acts by irreversibly blocking mitochondrial electron transport.
HCN gas can lead to cardiorespiratory collapse and arrest within a few minutes. Patients surviving to reach hospital are unlikely to have suffered significant poisoning.
Early signs include dizziness, chest tightness, dyspnoea, confusion and paralysis, followed by cardiovascular collapse, apnoea and seizures.
Management of cyanide poisoning
- Do not attempt mouth to mouth resuscitation as the skin will be contaminated.
- Apply 100% O2 with a tight fitting mask. Treatment is supportive.
- Decontaminate the skin with soap and water.
- Gastric lavage could be attempted where there are no signs of cyanide poisoning.
- Dicobalt ededate, sodium thiosulphate and sodium nitrate are used as antidotes.
Medicines
Children frequently ingest medicines. Dangerous substances for children include salicylates, paracetamol, iron, theophylline and tricyclic antidepressants.
Aspirin / Salicylate poisoning
Commonly ingested by children. Also probably the commonest drug to be ingested deliberately in overdose. Oil of wintergreen is 98% methyl salicylate. Its primary toxic effect is by uncoupling of oxidative phosphorylation.
Patients present with restlessness, hyperventilation, tinnitus, deafness, tachycardia, nausea, vomiting, sweating, hyperthermia and dehydration. Pulmonary oedema, acute renal failure, hypokalaemia, hypoglycaemia and hypothrombinaemia may also develop. In adults there is an early increase in respiration rate causing a respiratory alkalosis that precedes the later development of metabolic acidosis. However this is not seen in children.
Management of aspirin / salicylate poisoning
- Gastric lavage should be attempted up to 12 hours or longer post ingestion. In overdose, salicylates may form concretions in the stomach and delay absorption.
- Activated charcoal every four hours.
- Severity of the poisoning can be determined by measuring blood salicylate levels 6 or more hours after ingestion but may be misleading in severe acidosis. Ideally should be done on admission and 4 hours later to asses continued absorption. Therapeutic levels of salicylate are generally less than 300mg/l. Levels more than 750mg/l represents severe poisoning.
- Check electrolytes. Blood glucose monitoring should be done every 2 hours.
- Dehydration, acidosis, hypoglycaemia and electrolyte disturbances should be corrected. Pay particular attention to potassium. Care should be taken to avoid fluid overload and renal function should be closely monitored.
- Alkalinisation of the urine (pH 7.5-8.5) by administering sodium bicarbonate orally or by infusion is recommended to increase excretion of salicylates.
- Haemodialysis or charcoal haemoperfusion may be required in severe poisoning (levels > 1000mg/l or 7.25mmol/l) or in patients with decreased urine output, pulmonary oedema or progressive deterioration.
Paracetamol overdose
Paracetamol ingestion is common but seldom leads to severe toxicity in children due to the diluted concentration of the paediatric syrup formulation. The children at risk are those with glutathione depletion, such as children with cystic fibrosis, adolescents with eating disorders and those also on enzyme inducing agents such as anticonvulsants.
The liver is the main target organ in paracetamol poisoning. Patients are generally asymptomatic up to 24 hours post ingestion. Mild nausea, vomiting and anorexia may occur. Hepatic necrosis becomes apparent in 24-36 hours with right subchondral pain and tenderness, jaundice, vomiting and acute liver failure. Confusion and encephalopathy develop over 36-72 hours. Oliguria and renal failure may occur from acute tubular necrosis in the absence of liver failure. Lactic acidosis may be seen early or late.
Management of paracetamol poisoning
Patients presenting within 4 hours of ingestion should undergo gastric lavage. Activated charcoal should not be given orally if the specific antidote is also given orally.
Measure paracetamol levels at least 4 hours post ingestion and plot on ‘plasma paracetamol concentration – time graph’ to determine treatment line.
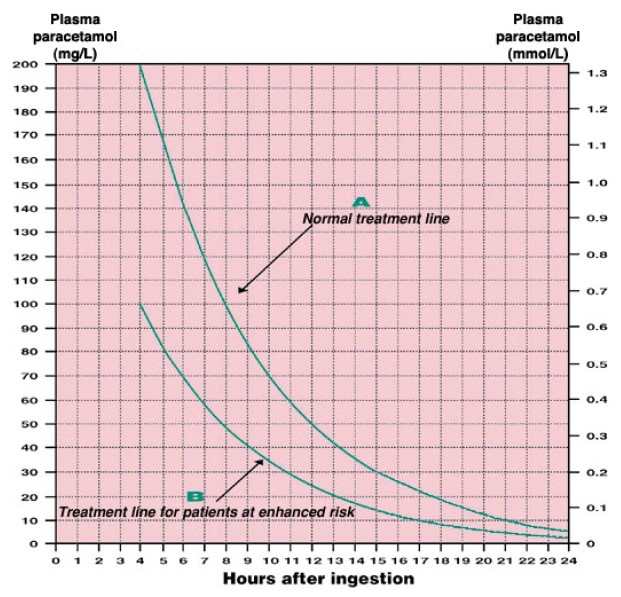
- If the initial levels indicate no treatment, repeat after 4 hours to check for delayed absorption.
- All patients on or above the ‘Normal treatment line’ should be given Nacetylcysteine.
- Patients on enzyme-inducing drugs should be treated if above the ‘Enhanced risk treatment line’.
- Where levels are not available, liver damage should be assumed after ingestion of a single dose of more than 150mg/kg paracetamol.
- Acetylcysteine is the antidote of choice and is usually given iv. Oral methionine may be used if the patient is allergic to acetylcysteine and is also a suitable alternative in remote areas if vomiting is not a problem. Oral acetylcysteine and carbocysteine have also been used.
- Monitor urea and electrolytes, PT and LFT.
- Give vitamin K but avoid giving fresh frozen plasma unless there is active bleeding. The PT is the best indicator of the severity of liver failure.
- All patients with encephalopathy or a rapidly rising PT should be referred to a liver unit (where available).
- Supportive treatment and treatment of liver and renal failure as indicated.
Iron poisoning
Ingestion of more than 20mg/kg of elemental iron is considered potentially toxic and the lethal dose is estimated at about 180mg/kg.
Iron is extremely irritant. The clinical features can be divided into three phases (not always very clear). Patients present with vomiting, diarrhoea, abdominal pain, haematemesis and rectal bleeding in the early phase (0-2 hours). This is followed by a period of stabilisation (up to 12 hours) during which a deceptive recovery occurs. This is followed by a life-threatening period during which coma, fits, jaundice, hepatic failure renal failure, clotting abnormalities, hypoglycaemia and cardiovascular collapse may occur.
Patients alive 72 hours after ingestion usually make a full recovery. Late complications of gut stricture, gastric fibrosis and pyloric obstruction have been reported.
Management of iron overdose
- The stomach should be emptied with gastric lavage.
- Blood samples for FBC, glucose, UE, iron levels and ABG where available.
- Serum iron only peaks four hours after ingestion.
- An abdominal X-ray helps to determine the number of tablets ingested and also the success or failure of gastrointestinal evacuation.
- A patient with serum iron >90mmol/l may be treated with a chelating agent.
- If <20mg/kg are ingested, treatment is supportive. Patients with iron level below 54mmol/l and who remains asymptomatic 6 hours post ingestion would not be expected to develop significant toxicity and require no active treatment.
- For ingestion of between 20-60mg/kg elemental iron, gastric emptying may be considered if within one hour of ingestion. Whole bowel irrigation may be used in patients with ingestion of more than 60mg/kg and more than one hour post ingestion. It is especially useful if a slow release preparation has been ingested. Charcoal is of no benefit as iron does not bind to it.
- Desferrioxamine chelates iron and is the recommended treatment.
- Give 1 gram im every 6-12 hours for children (2g for adolescents). (100mg of desferrioxamine binds 8.5mg of elemental iron).
- If the patient is hypotensive, give desferrioxamine iv at a rate of 15mg/kg/hour, until the serum iron falls (maximum daily dose 80mg/kg)
- Haemodialysis is indicated in very high serum iron levels that respond poorly to chelation therapy or if the urine output is not maintained. (the iron-chelate is excreted entirely in the urine).
Theophylline poisoning
This type of poisoning is rare but serious. Most preparations are slow release so that problems develop 12-24 hours after ingestion.
Features of acute ingestion reflect the local irritant GI effects – nausea, vomiting, haematemesis and diarrhoea. The child may be hyperactive with dilated pupils, hypereflexia, hypotonia and myoclonus. There may also be severe hypokalaemia, arrhythmias, metabolic acidosis, hyperglycaemia, hypotension and seizures.
Management of theophylline poisoning
- Gastric lavage should be considered if ingestion occurred within 1-2 hours.
- Repeated administration of activated charcoal to prevent further absorption and enhance systemic clearance. (May be difficult in the presence of nausea and vomiting).
- Whole bowel irrigation is considered if a slow-release preparation is ingested.
- Haemoperfusion should also be considered.
- Seizures are treated with diazepam.
- Assess hydration and correct hypokalaemia and electrolyte disturbances.
- Cardiac monitoring to detect arrhythmias.
- Verapamil and propanolol may be required to treat supraventricular and ventricular tachyarrhythmias. Lignocaine appears to have little effect on ventricular ectopy.
Tricyclic antidepressants
Cardiovascular toxicity is the main cause of death in tricyclic antidepressant overdose. It is caused by the blockade of noradrenaline uptake as well as the anticholinergic, membrane-stabilising and alpha-blocking effects. Nervous system toxicity includes drowsiness, agitation, hallucinations, hyperreflexia, myoclonus, rigidity, convulsions, respiratory depression and coma.
Anticholinergic effects include flushing, dry mouth, dilated pupils, hyperpyrexia and bladder/bowel paralysis. Cardiovascular toxicity includes sinus tachycardia, hypotension, conduction abnormalities and arrhythmias. Respiratory complications include respiratory depression, aspiration pneumonia, ARDS and pulmonary oedema.
Management of tricyclic overdose
- Gastric emptying is delayed by tricyclic antidepressants and therefore gastric lavage should be attempt as late as 12 hours post ingestion.
- Due to CNS depression and inadequate ventilation, intubation may be required.
- Keep up cardiac monitoring for up to 48 hours.
- Inotropic support should be given as necessary.
- Correct metabolic acidosis to enhance protein binding of the drug.
- Control seizures with diazepam.
Summary
Prevention of childhood poisoning is vital. There must be adequate supervision, safe placement of medications, child safe cabinets and containers, blister packaging and education. Most paediatric cases are not severe. Recognition of potentially life-threatening ingestions is important so that appropriate early treatment can be instituted. Aggressive supportive care is vital.
Answers
- False
- True
- False
- False
- True
- True
- False
- False
- False
- False
Useful websites
- World Health Organisation – The International Programme on Chemical Safety : Poisoning Prevention and Management (www.inchem.org)
- TOXBASE.org www.spib.axl.co.uk (NHS only, requires registration)
- TOXNET (toxnet.nlm.nih.gov)
- Royal Children’s Hospital Melbourne: Victorian Poisons Information Centre (www.rch.org.au/poisons)



