Basic Sciences
QUESTIONS
Before reading this tutorial, try to answer the following questions. Answers and a short explanation can be found at the end of the article.
- Regarding neuraxial opioids, which of the following are true:
- Early respiratory depression is most likely to occur after delivery of highly lipid soluble epidural opioids
- Delayed respiratory depression is due to cephalad migration of opioid in CSF to the respiratory centre
- Analgesia from neuraxial opioids is primarily mediated by central nervous system uptake in the brain
- All opioids are approved for neuraxial use
- Regarding adrenaline 1:200,000 as an adjunct to local anaesthetic solutions, which of the following are true:
- Adrenaline reduces the systemic absorption of local anaesthetics in the epidural space
- Adrenaline is more effective at prolonging the duration of blockade of lidocaine compared with bupivacaine
- An immediate increase in heart rate after epidural administration may indicate epidural vein cannulation
- Adrenaline should be used cautiously with halothane anaesthesia
- Regarding the use of sodium bicarbonate to alkalinise local anaesthetic solutions, which of the following are true:
- Alkalinisation of local anaesthetic solutions reduces latency of blockade
- Alkalinisation of local anaesthetic solutions increases duration of blockade
- Alkalinisation of local anaesthetic solutions increases the ionised fraction of drug
- Sodium bicarbonate is added to bupivacaine when rapid onset of blockade is required
INTRODUCTION
Neuraxial anaesthesia describes the use of spinal (intrathecal/subarachnoid), epidural and caudal epidural techniques and is commonly used in a wide variety of procedures. Anaesthesia and analgesia can be achieved by single injection, intermittent bolus or continuous infusion of local anaesthetic. Additional medications are frequently added to the local anaesthetic to modify its effects. This tutorial aims to summarise some of the adjuvant agents that are in common use in neuraxial anaesthesia and analgesia. The reader should be aware that many agents, despite being commonly utilised, are not licensed for neuraxial administration and some preparations may contain additives such as preservatives that are potentially neurotoxic.
NEURAXIAL ADJUVANTS
Adjuvants are drugs that increase the efficacy or potency of other drugs when given concurrently. Neuraxial adjuvants are used to improve or prolong analgesia and decrease the adverse effects associated with high doses of a single local anaesthetic agent. In addition to their dose sparing effects, neuraxial adjuvants are also utilised to increase the speed of onset of neural blockade (reduce latency), improve the quality and prolong the duration of neural blockade. Neuraxial adjuvants include opioids, sodium bicarbonate (NaHCO3), vasoconstrictors, alpha-2 adrenoceptor agonists, cholinergic agonists, N-methyl-d-aspartate (NMDA) antagonists and γ-aminobutyric acid (GABA) receptor agonists.
OPIOIDS
Mechanism of Action
Opioids act as agonists at opioid receptors which are widespread throughout the body including the brain (cerebral cortex, thalamus, hypothalamus, amygdala, basal ganglia, brainstem, reticular activating system), spinal cord and non neural tissues such as the gastrointestinal tract. There are four main classes of opioid receptors; mu, kappa, delta and nociceptin, all of which are G-protein coupled inhibitory receptors. Each opioid has different affinities for these classes of receptors, and each class is associated with specific therapeutic and adverse effects.
Analgesia from neuraxial opioid administration is primarily mediated by binding pre and postsynaptic mu-opioid receptors in the substantia gelatinosa of the dorsal horn of the spinal cord. Activation of presynaptic receptors on primary afferent neurons carrying nociceptive information results in decreased conductance through voltage gated calcium channels and reduced calcium influx with subsequent decreased neurotransmitter release. This reduces signalling between primary and secondary afferent neurons in the dorsal horn. Binding of postsynaptic opioid receptors on secondary afferent neurons results in hyperpolarisation and decreased propagation of action potentials.
Intrathecal opioids
Intrathecal opioids potentially act as ligands on opioid receptors in three different areas to produce analgesia:
- They have direct access to the dorsal horn of the spinal cord (their main site of action).
- They are transported supra-spinally by bulk CSF flow where they modulate descending inhibitory pain pathways.
- A small amount of opioid diffuses into the epidural space with subsequent systemic absorption resulting in centrally mediated analgesia (minor effect).
Intrathecal opioids undergo minimal metabolism within the CSF. The onset and duration of analgesia and the degree of cephalad spread are dependent on lipid solubility. Highly lipid soluble (lipophilic) opioids such as fentanyl and sufentanil diffuse into the spinal cord and bind dorsal horn receptors rapidly. This produces a rapid onset of analgesia with minimal cephalad spread and subsequently a low risk of delayed respiratory depression, however the duration of analgesia is relatively short. Morphine is poorly lipid soluble (hydrophilic) and is much slower to bind dorsal horn receptors resulting in a slower onset but more prolonged duration of analgesia, increased cephalad spread and subsequently an increased risk of delayed respiratory depression.
Epidural opioids
After epidural administration, variable quantities (depending on which opioid is used) will diffuse across the dura and arachnoid mater into the subarachnoid space to bind opioid receptors in the dorsal horn of the spinal cord. Lipid solubility is the most important factor affecting the rate of diffusion and the subsequent onset and duration of analgesia. Lipophilic opioids such as fentanyl and sufentanil diffuse rapidly across the dura into the CSF compared to hydrophilic opioids such as morphine. Lipophilic opioids produce rapid onset of analgesia which is of short overall duration. After epidural delivery, CSF opioid levels peak at 6 minutes for sufentanil, 20 minutes for fentanyl and 1-4 hours for morphine.
The epidural space is extremely vascular and there is extensive absorption of opioids via the epidural venous plexus into the systemic circulation. Systemic opioids reach the CNS and bind receptors in areas of the brain that modulate pain perception and response. Epidural administration of sufentanil, fentanyl and morphine produces plasma levels of opioid similar to those seen after intramuscular injection of similar doses. Centrally mediated analgesia after systemic absorption is an important mechanism of analgesia for epidural opioids. Lipophilic opioids such as sufentanil and fentanyl are absorbed the most rapidly, and are therefore more likely to cause early respiratory depression. After epidural delivery, plasma levels peak at less than 5 minutes for sufentanil, 5-10 minutes for fentanyl and 10-15 minutes for morphine.
Dose
The appropriate dose depends on the type of opioid (potency, efficacy, lipid solubility), indication for use, addition of other adjuvants, patient factors and route of administration. Intrathecal drugs have direct access to the central nervous system (CNS) and need relatively small doses for analgesic effect compared to epidural dosing. Intrathecal doses are usually approximately 1/10th of the epidural dose.
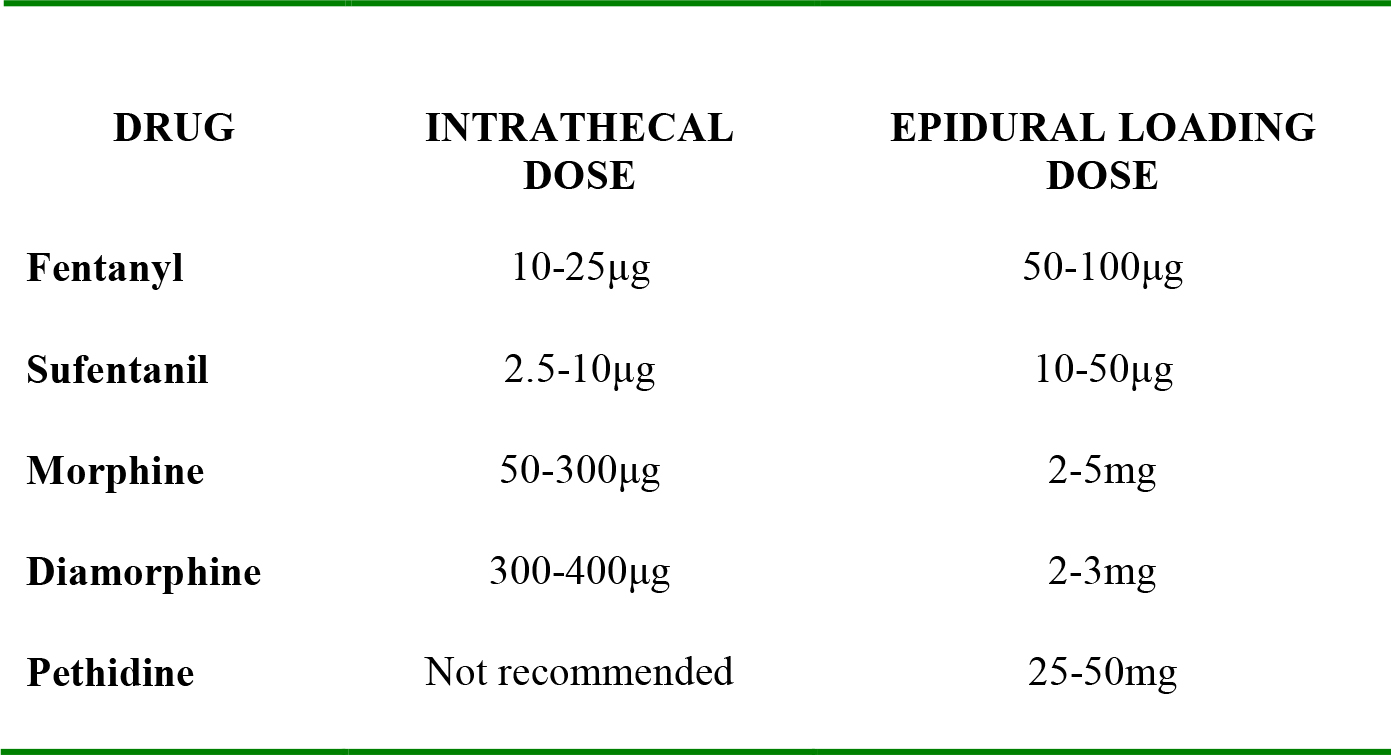
Table 1: Indicative doses of neuraxial opioids
Efficacy
Neuraxial opioids differ primarily in their potency, onset, duration of action and side effects. The choice of opioid depends on the indication for neuraxial analgesia (e.g. labour analgesia, caesarean delivery, postoperative analgesia), the addition of other adjuvants, and whether epidural or spinal analgesia is required. Opioids may be used alone, or more commonly as adjuncts to local anaesthetics with which they have a synergistic effect. When used alone, the utility of most lipophilic neuraxial opioids is limited by a short duration of effect and dose related side effects. The most frequently used neuraxial opioids include morphine, diamorphine, fentanyl, sufentanil and pethidine.
Intraoperative analgesia
Opioids are commonly added to local anaesthetic for operations performed under epidural and spinal anaesthesia. Neuraxial opioids improve the quality of intraoperative analgesia, delay regression of sensory blockade and prolong postoperative analgesia.
Epidural labour analgesia
Opioids have a synergistic effect with local anaesthetics. This allows the use of lower doses of local anaesthetics which subsequently decreases the frequency and severity of maternal hypotension and motor blockade. Epidural opioids improve quality of analgesia and reduce the number of failed epidurals due to patchy blocks. Different opioids can be used, however those with low lipid solubility such as morphine are associated with delayed respiratory depression and should be used with caution. Fentanyl is the most frequently used opioid for labour analgesia. Intrathecal opioids are also effective for labour analgesia, however no single intrathecal drug can reliably provide analgesia for the duration of labour.
Postoperative analgesia
Epidural infusions of local anaesthetics are rarely used as single agents for postoperative analgesia. Multiple trials have shown that the addition of opioids to local anaesthetic solutions significantly improves pain relief after thoracic, abdominal and orthopaedic surgery. The incidence of motor blockade and hypotension is also decreased due to the dose sparing effects of opioids, and postoperative analgesic requirements are reduced.
Specific opioids
Fentanyl
Fentanyl is a highly potent lipophilic phenylpiperidine derivative. It has a rapid onset of action (5 minutes intrathecal, 10 minutes epidural) and relatively short duration of action due to redistribution (2-4 hours intrathecal and epidural). It has no active metabolites and is approximately 800 times more lipid soluble then morphine. It has a long terminal elimination half life (190 minutes) and repeated high doses may result in accumulation. Due to its high lipid solubility it rapidly binds dorsal horn receptors in the spinal cord after neuraxial administration. Cephalad migration and delayed respiratory depression are uncommon. Epidural bolus doses may result in early respiratory depression due to systemic absorption. Its rapid onset is advantageous for labour analgesia and emergency caesarean delivery, however its short duration of action limits its postoperative analgesic effect after single dose spinal anesthesia.
Sufentanil
Sufentanil is an extremely potent lipophilic phenylpiperidine derivative. It has a faster onset (2-3 minutes intrathecal, 4-6 minutes epidural) and shorter duration of action then fentanyl (1-3 hours intrathecal and epidural). Its analgesic potency is 5-7 times greater than fentanyl, and it is 1600 times more lipid soluble then morphine. Its terminal elimination half life is shorter than fentanyl (150 minutes) so accumulation is less likely. Its high lipid solubility reduces the risk of cephalad migration and delayed respiratory depression after neuraxial use, but increases its risk of early respiratory depression after epidural bolus. Like fentanyl, the intrathecal administration of sufentanil for postoperative analgesia is limited by its short duration of action.
Pethidine
Pethidine is a lipophilic phenylpiperidine derivate 10 times less potent and 30 times more lipid soluble then morphine. It has a faster onset (5 minutes intrathecal, 10 minutes epidural) and shorter duration (4-8 hours intrathecal and epidural) of action than morphine. Pethidine has an active metabolite (norpethidine), which in high concentrations may cause seizures and hallucinations. Pethidine differs from other opioids in that it possesses local anaesthetic properties (motor and sensory fibre block). An intrathecal dose of 1mg/kg produces surgical anaesthesia, however the incidence of adverse effects is high and its use by this route is not recommended. Epidural pethidine is effective as a single agent for postoperative analgesia after caesarean delivery and may be administered as a patient controlled epidural analgesia technique. In this setting the incidence of adverse effects is relatively low.
Morphine
Morphine is a hydrophilic phenanthrene derivative and is approximately 100 times less potent then fentanyl. Its onset is slow compared to the lipophilic opioids (15 minutes intrathecal, 30 minutes epidural), and it has a significantly longer duration of action (approximately 12-24 hours). Its terminal elimination half life is approximately 170 minutes. Intrathecal morphine is slow to bind dorsal horn receptors in the spinal cord due to its poor lipid solubility and free opioid in the CSF may migrate supra-spinally resulting in delayed respiratory depression. Neuraxial morphine has been shown to be as effective as fentanyl at improving the quality of analgesia for labour pain, caesarean delivery, and more effective than a single dose of fentanyl at providing postoperative pain relief. Unfortunately both intrathecal and epidural morphine are associated with a higher incidence of nausea, vomiting, pruritus, urinary retention, sedation and delayed respiratory depression when compared to fentanyl. In the setting of post caesarean analgesia, both single dose intrathecal and epidural morphine have been shown to have a ceiling analgesic effect; at doses greater then 100μg (intrathecal) and 3.75mg (epidural) there is minimal additional analgesic benefit, but increased incidence of adverse effects (particularly pruritus). Anaesthetists must be cautious in utilising only preservative free morphine for neuraxial anaesthesia and analgesia.
Diamorphine
Diamorphine is primarily used in the UK. It is a lipophilic semi-synthetic opioid that is twice as potent as morphine. It is a prodrug that is converted to its more active metabolites (morphine and 6-monoacetylmorphine) by deacetylation in the liver and neural tissues. Diamorphine is 280 times more lipid soluble then morphine, therefore delayed respiratory depression is less common. The incidence of nausea and vomiting is significantly less then morphine. Diamorphine has a fast onset (<10 minutes) of analgesia and a long duration of action (10-20 hours intrathecal and epidural). It has a similar efficacy to fentanyl when used for intraoperative analgesia. It is commonly used for pain relief after caesarean delivery. In this setting the duration and quality of analgesia produced by intrathecal diamorphine is similar to epidural diamorphine, however the incidence of pruritus is higher with intrathecal administration. Although epidural administration of bupivacaine and diamorphine mixtures have been shown to provide good analgesia for labour, its use in this setting is limited.
Side Effects
Adverse effects from neuraxially administered opioids are potentially due to the cephalad spread of opioid in the CSF or via systemic absorption from the epidural space which can lead to similar adverse effects observed following parenteral administration. Intrathecal and hydrophilic opioids are more likely to cause adverse effects secondary to cephalad migration, while epidural and lipophilic opioids are more likely to cause central effects after systemic absorption. Most side effects are dose related and are due to opioid receptor interactions, however some are unrelated. The classical side effects of neuraxial opioids include:
Pruritus
Pruritus is the most common adverse effect of neuraxial opioids. It occurs within the first few hours and is usually localised to the face, neck and thorax. The mechanism for pruritus is not fully understood but is thought to be mediated by cephalad migration of opioid which binds to opioid receptors in the trigeminal nucleus. It is more common when poorly lipid soluble agents are used (for example there is a 70% incidence of pruritus with intrathecal morphine compared to 10% for fentanyl). Histamine-1 receptor antagonists may be helpful even though the pruritus is not mediated by histamine release. Opioid receptor antagonists such as naloxone are most effective at managing pruritus but may diminish analgesic effects.
Nausea and vomiting
The incidence of nausea and vomiting associated with neuraxial opioids is reported as being between 20-50%. It is more common in females and with intrathecal morphine. It is thought to be mediated by cephalad migration of the opioid to the chemoreceptor trigger zone where the opioids can act as a partial dopamine-2 receptor agonist.
Urinary retention
The incidence of urinary retention is approximately 30-40%. It is more common in young men and with intrathecal morphine. It is mediated by opioid receptors in the sacral spinal cord. This inhibits sacral parasympathetic outflow that leads to detrusor relaxation.
Respiratory Depression
Respiratory depression is potentially the most serious adverse effect caused by neuraxial opioids. The incidence after neuraxial administration is similar to that of parenterally administered opioids. Factors increasing the risk of respiratory depression include high opioid dose, elderly patients, concomitant use of sedative and analgesic drugs, lack of opioid tolerance and the presence of comorbid factors (for example sleep apnoea and pulmonary disease). Treatment with opioid antagonists such as naloxone may be required in some cases.
Early respiratory depression generally develops within 2 hours of epidural administration of lipophilic opioids such as sufentanil and fentanyl. It is due to systemic absorption from the epidural space, and is less common after intrathecal administration and hydrophilic opioids such as morphine.
Delayed respiratory depression usually develops between 6-12 hours after intrathecal administration of poorly lipid soluble opioids such as morphine. It is due to cephalad migration of the opioid in the CSF which reaches opioid receptors in the respiratory centre. It is uncommon with lipophilic opioids because they rapidly penetrate the spinal cord, leaving minimal free opioid in the CSF.
Other
Other adverse effects include sedation, CNS excitation, viral reactivation (herpes simplex labialis virus), gastro-intestinal dysfunction, sexual dysfunction, ocular dysfunction and thermoregulatory dysfunction.
SODIUM BICARBONATE
Mechanism of Action
Sodium bicarbonate can be used to speed the onset of action of epidural lidocaine. It is not commonly used with other neuraxial agents. For epidural lidocaine to exert its effects, the extra-neural local anaesthetic must diffuse across the neural membrane to access voltage gated sodium channels to reversibly block sodium channel conductance. Lidocaine exists as a weak base. In solution there is equilibrium between the ionised and unionised fraction, which is dependent on the pka and the pH of the solution. Only the unionised form is lipid soluble and can easily diffuse across the lipid phase of the neural membrane. The more alkaline the solution, the greater the unionised fraction of lidocaine. The addition of sodium bicarbonate 8.4% to lidocaine increases the pH, thereby increasing the unionised fraction. This allows a greater proportion of local anaesthetic to diffuse across the neural membrane.
Dose
- 1ml of 8.4% NaHCO3 per 10ml of lidocaine.
Efficacy
Alkalinisation of a lidocaine solution results in a more rapid onset of neural blockade (reduced latency), improved depth of block and may increase the spread of epidural blockade. This is particularly useful for epidural anaesthesia in the obstetric setting when urgent caesarean delivery is required. Increasing the unionised fraction will allow the local anaesthetic to diffuse into the spinal nerves in the epidural space as well as aid diffusion through the dura and arachnoid to reach the subarachnoid space. This can speed the onset of the block by between 2-5 minutes.
VASOCONSTRICTORS
Mechanism of Action
Vasoconstrictors act as agonists on G-protein coupled receptors located in vascular smooth muscle. Ligand binding stimulates phospholipase C, resulting in calcium influx and vasoconstriction of blood vessels. This reduces vascular absorption of local anaesthetic and maintains a higher concentration at the nerve roots for a longer period. This can significantly prolong the duration of blockade, particularly in highly vascular areas like the epidural space. Adrenaline is the most commonly used vasoconstrictor adjunct for local anaesthetics. It is also an alpha-2 receptor agonist and has its own analgesic effect mediated in the spinal cord.
Dose
- Adrenaline 1:200,000 (5 μg/ml of an epidural solution)
Efficacy
Reducing vascular absorption of local anaesthetic to maintain a higher concentration at the nerve root results in an improved quality of block and prolonged duration of blockade. Delayed vascular absorption reduces systemic plasma levels of local anaesthetics and therefore the risk of systemic local anaesthetic toxicity. This allows the safe use of higher doses of some agents when combined with adrenaline; i.e. the maximum recommended dose of lidocaine when used alone is 4mg/kg compared with 7mg/kg if combined with adrenaline 1:200,000. This is useful in situations where large or repeated doses of lidocaine are required.
It is important to remember that the addition of adrenaline does not confer the same benefits for all local anaesthetics in all spaces. The addition of adrenaline to lidocaine or chloroprocaine for use in the epidural space has been shown to decrease systemic absorption by approximately 30% and significantly prolong the duration of blockade. Agents with high lipid solubility such as bupivacaine bind more avidly to tissues and have less systemic absorption compared to less lipid soluble agents. The addition of adrenaline to bupivacaine for use in the epidural space decreases systemic absorption by around 10-20%, and is less effective at prolonging the duration of blockade when compared to lidocaine.
Most local anaesthetic agents possess intrinsic vasodilatory properties at low doses. Ropivacaine differs as it has mild vasoconstrictive properties and the addition of adrenaline has minimal effect on reducing systemic absorption or prolonging neural blockade.
Side effects
An increase in plasma levels of adrenaline can be seen after neuraxial administration of local anaesthetic solutions containing adrenaline. Adrenaline is an agonist at both alpha and beta adrenoceptors and may cause tachycardia and hypertension in a dose dependent manner. Its use may not be advisable in patients with unstable angina, uncontrolled hypertension or a recent myocardial infarct. Solutions containing adrenaline should be used with caution in patients undergoing general anaesthesia with halothane due to the risk of cardiac arrhythmias. The use of high doses of adrenaline in the epidural space may potentially increase the risk of spinal artery thrombosis, however there is no conclusive evidence of this. Preservative containing adrenaline solutions should not be used for intrathecal and epidural anaesthesia. Solutions containing adrenaline should be used cautiously in patients taking tricyclic antidepressants and monoamine oxidase inhibitors. In addition, care should be taken in women suffering from pre-eclampsia as systemic absorption of adrenaline may cause further elevations in blood pressure.
CLONIDINE
Mechanism of Action
Clonidine is a centrally acting partial alpha-2 adrenoceptor agonist. Its analgesic effect is thought to be mediated by binding postsynaptic alpha-2 receptors (G-protein coupled inhibitory receptors) in the dorsal horn of the spinal cord, resulting in decreased nociceptive transmission. It does not affect proprioception or produce motor blockade.
Dose
- Epidural: Bolus dose 75-150μg
- Spinal: Bolus dose 30-60μg
- Caudal: Bolus dose 1 μg/kg
Efficacy
When used as a neuraxial adjunct for pain relief after caesarean delivery, major abdominal and orthopaedic surgery, clonidine prolongs the duration of analgesia and anaesthesia. Obstetric studies have shown that for caesarean delivery with spinal anaesthesia, intrathecal clonidine 30-60μg increases the duration of sensory block by approximately 30%, delays the onset of postoperative pain and reduces overall postoperative opioid requirements. Neuraxial opioids and alpha-2 agonists exhibit synergism. The addition of clonidine to opioids for postoperative analgesia as a continuous epidural infusion reduces opioid requirements by between 20-60%. Dosage regimens that include a bolus dose followed by continuous infusion appear to produce superior analgesia.
Clonidine is a useful adjunct for labour epidural analgesia. It has been shown to reduce local anaesthetic requirements and improve pain scores when combined with 0.125% bupivacaine +/- fentanyl 2 μg/ml. When used in a concentration of 1-2 μg/ml, it has not been shown to have significant effects on fetal heart rate, Apgar scores or umbilical cord gases. It may have additional beneficial effects in women with pre-eclampsia.
Side effects
Sedation, hypotension and bradycardia are the main adverse effects of neuraxial clonidine. Cardiovascular effects are usually seen within 15 to 30 minutes of epidural administration and last for up to 3 hours. Changes in blood pressure are dose dependent. Clonidine does not produce respiratory depression or appear to increase the risk of nausea, vomiting, urinary retention or pruritus when combined with neuraxial opioids.
NEOSTIGMINE
Mechanism of action
Neostigmine acts by inhibiting acetyl-cholinesterase and preventing the breakdown of acetylcholine. Increasing the concentration of acetylcholine available to bind muscarinic and nicotinic receptors in the dorsal horn of the spinal cord provides analgesia with no motor or sympathetic blockade. It is most useful as an adjunct rather then a sole agent.
Dose
- Epidural (for postoperative pain): single bolus 50-100μg
- Epidural (for labour analgesia): single bolus 300-500μg
Efficacy
Intrathecal
Intrathecal neostigmine enhances analgesia from systemically and neuraxially administered opioids and alpha-2 adrenoceptor agonists but a high incidence of severe nausea and vomiting precludes its use by this route.
Epidural
Epidural neostigmine provides modest analgesia in postoperative patients as evidenced by mildly reduced pain scores and reduced opioid consumption. The magnitude of this effect is similar to that achieved by simple analgesics. Epidural neostigmine also enhances the duration and intensity of analgesia from systemic and neuraxial alpha-2 adrenoceptor agonists, opioids and local anaesthetics.
Side effects
Unlike intrathecal neostigmine, epidural neostigmine is not associated with an increased risk of nausea and vomiting, however doses greater then 100μg have been associated with sedation. It does not cause respiratory depression or pruritus either alone or in combination with neuraxial opioids.
KETAMINE
Mechanism of Action
Ketamine is a non-competitive NMDA receptor antagonist. Its primary analgesic effect is mediated by antagonising NMDA receptors located on secondary afferent neurons in the dorsal horn of the spinal cord. This reduces the transmission of nociceptive information in the spinal cord and has an important role in preventing central sensitisation, windup and long term potentiation which are all involved in chronic pain. In high doses it may have additional minor analgesic effects by binding opioid mu receptors and modulating descending inhibitory pathways through inhibition of reuptake of neurotransmitters.
Dose
- Intrathecal: not recommended
- Epidural: 0.5-1.0mg/kg
Efficacy
There are limited human studies on the use of intrathecal ketamine due to the potential risk of neurotoxicity from its preservative benzalkonium chloride. In one human study of intrathecal ketamine, doses above 50mg resulted in local anaesthetic effects. The results of animal studies suggest that intrathecal administration of ketamine may cause complete sensory and motor blockade.
There are multiple studies on the efficacy of epidural ketamine when used as a sole agent or in combination with opioids and local anaesthetics for postoperative pain. Epidural ketamine appears to speed up the onset of analgesia and prolong the duration of analgesia, especially when combined with epidural morphine. When used as an adjunct to local anaesthetics for postoperative pain, epidural ketamine has been shown to improve pain scores and have a dose sparing effect.
Side Effects
Reported side effects of epidural ketamine include sedation, headache, and transient burning back pain during injection with doses greater than 0.5mg/kg. No clinical trials have reported respiratory depression, hallucinations, cardiovascular instability, bladder dysfunction or neurologic deficit with epidural doses up to 1mg/kg. There is no increased incidence of nausea, vomiting or pruritus when combined with neuraxial opioids.
Midazolam
Mechanism of Action
Midazolam is a benzodiazepine and a GABA-A receptor agonist. GABA-A receptors are ligand gated receptors located throughout the CNS and GABA is the major inhibitory neurotransmitter of the CNS. GABA binding results in a change of receptor configuration, causing an ion channel to open which allows chloride ions to flow down their electrochemical gradient into the cell. This results in hyperpolarisation of the neuron and reduced action potential propagation. Benzodiazepines have their own binding site (called the benzodiazepine receptor) on the GABA-A receptor. The effect of binding is to increase the frequency of chloride channel opening, which enhances the effects of GABA. The substantia gelatinosa of the dorsal horn of the spinal cord contains a high density of GABA-A receptors. Benzodiazepines are likely to mediate their analgesic effect by increasing inhibition of nociceptive neurons in this area.
Dose
- Intrathecal: 20μg/kg (up to 2.5mg)
- Epidural: 10-20μg/kg/hr for up to 12 hours
Efficacy
Intrathecal midazolam prolongs duration of spinal anaesthesia, decreases postoperative analgesic requirements and reduces the incidence of nausea and vomiting. Although there are limited studies, epidural midazolam used as a continuous infusion for postoperative analgesia has also been shown to reduce postoperative analgesic requirements and incidence of nausea and vomiting. In addition to local anaesthetics, midazolam can be combined with other drugs such as opioids, clonidine and ketamine for additive effects.
Side effects
There are limited studies assessing the clinical safety of intrathecal midazolam. The most serious side effect in animal studies is neurotoxicity. Doses up to 2.5mg have not been shown to cause any neurological deficit in humans.
OTHER
There are many other potential adjuvant drugs which are relatively new or still undergoing human trials and hence cannot be recommended for use at this stage. These drugs include adenosine, calcium channel blockers, non-steroidal anti-inflammatory agents, calcitonin and cannabinoid receptor agonists.
ANSWERS TO QUESTIONS:
- TTFF- Early respiratory depression is due to systemic absorption of opioid and is increased by the vascularity of the space (epidural > intrathecal) and high lipid solubility (rapid diffusion and vascular uptake). Delayed respiratory depression is due to cephalad migration of opioid in CSF and is more common with poorly lipid soluble intrathecal opioids which are slower to bind receptors in the dorsal horn, thereby increasing the amount of free opioid in the CSF. Analgesia from neuraxial opioids is primarily mediated by opioid receptors in the dorsal horn of the spinal cord. Some opioid preparations contain neurotoxic preservatives (i.e. remifentanil) and should not be used neuraxially.
- TTTT- Adrenaline reduces systemic absorption of local anaesthetics in the epidural space by alpha-1 mediated vasoconstriction. It is more effective at reducing systemic absorption and prolonging duration of blockade for lidocaine compared to bupivacaine due to differences in lipid solubility and protein binding. An increase in HR immediately after epidural administration of local anaesthetic containing adrenaline may indicate the catheter is in an epidural vein. Adrenaline should be used cautiously with halothane and enflurane as there is increased risk of cardiac arrhythmias.
- TFFF- Sodium bicarbonate increases the pH of the local anaesthetic solution. This increases the unionised fraction of drug (local anaesthetics are weak bases) which then diffuses across the neural membrane and results in faster onset of block (reduced latency). There is no effect on duration of block. Sodium bicarbonate is not added to bupivacaine or ropivacaine as these local anaesthetics precipitate at alkaline pH.
REFERENCES
- Hindle A. Intrathecal opioids in the management of acute postoperative pain. Continuing Education in Anaesthesia, Critical Care & Pain. 2008; 8: 81-85
- McDonnell N, Keating M, Muchatuta N, Pavy T, Paech M. Analgesia after caesarean delivery. Anaesthesia and Intensive Care. 2009; 37: 539-51
- Van de Velde M, Berends N, Kumar A, Devroe S, Devlieger R, Vandermeersch E, De Buck F. Effects of epidural clonidine and neostigmine following intrathecal labour analgesia: a randomised, double-blind, placebo-controlled trial. International Journal of Obstetric Anesthesia. 2009: 3: 207-214



