Intensive Care Medicine
QUESTIONS
Before continuing, try to answer the following questions. The answers can be found at the end of the article, together with an explanation.
- Which of the following statements concerning adrenaline is correct?
- It causes vasodilation when infiltrated into skin
- IV injection may cause arrhythmias
- It should be administered as 1 mg bolus IV injection for the treatment of acute asthma
- It is metabolised by non-specific esterases in the blood
- Name five different clinical applications for adrenaline.
- Which of the following dosages are correct for adrenaline?
- VF cardiac arrest – 1 ml of 1:10 000 solution
- Anaphylaxis in a 5 year old child – 0.15 ml of 1:1000 solution IM injection
- Dilution with Bupivicaine for infiltration – 1:200 000
- Nebulised dose for a 2 year old with severe croup – 0.5 mg/kg
- IV dose for acute anaphylaxis – 1 mg
- The following are likely side effects of adrenaline injection (true or false?):
- Severe hypertension
- Maculopapular rash
- Bradycardia
- Tremor
- Bronchospasm
INTRODUCTION
Adrenaline, also known as Epinephrine, has rightly earned the title of ‘the doctor’s friend’, since it is the drug that is turned to at times of greatest need, and this is particularly so in anaesthetic practice. There are several clinical applications for adrenaline, most of them in situations where patients are acutely ill, and this requires all anaesthetists to be fully conversant with this essential drug. This tutorial is presented in two sections. The first describes the clinical pharmacology of adrenaline, and the second looks at its use in clinical situations that are especially relevant to anaesthetists.
CLINICAL PHARMACOLOGY
Metabolism and Structure
Adrenaline is a naturally occurring catecholamine that is produced in the medulla of the adrenal glands, and acts as a hormone and neurotransmitter. All catecholamines are monoamines that are derived from the amino acids phenylalanine and tyrosine. The series of metabolic reactions that occur in its synthesis are: oxidation of tyrosine to L-DOPA, decarboxylation to dopamine, oxidation to noradrenaline, and finally methylation to adrenaline (figure 1). Adrenaline is broken down by monoamine oxidase (MAO) and catechol-O-methyltransferase (COMT), and may also be excreted unchanged by the kidney. The structure of the adrenaline molecule is given in figures 2 and 3.
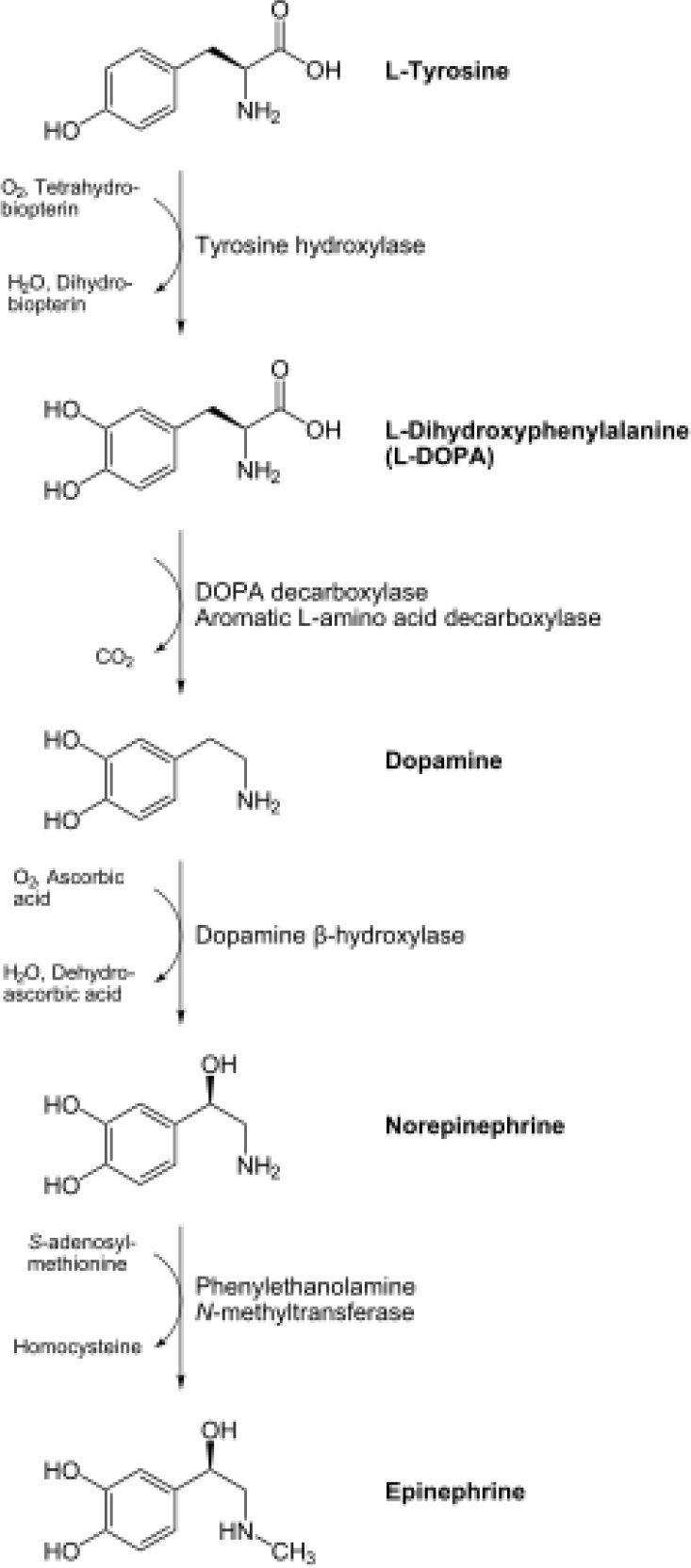
Figure 1. Metabolic pathway for synthesis of the catecholamines
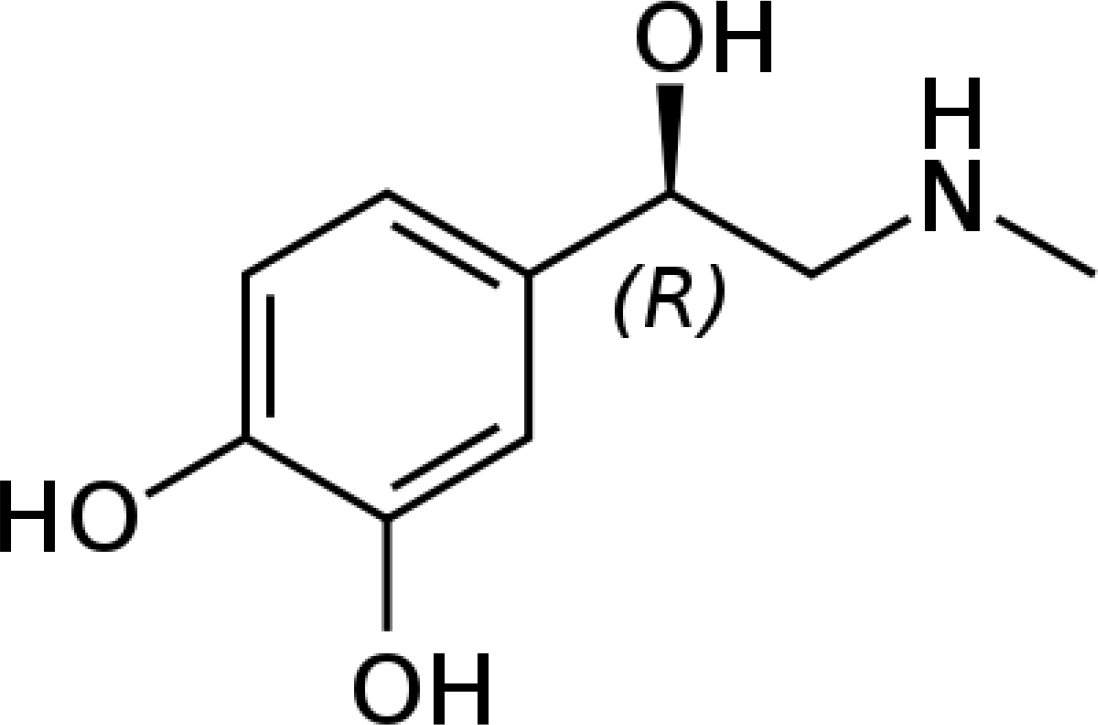
Figure 2. 2-dimensional structure of Adrenaline
Figure 3. 3-dimensional structure of Adrenaline
Presentation
Adrenaline is most frequently presented as a clear solution in a concentration of 1:1000 (1ml ampoule) or 1:10 000 (10 ml mini-jet for resuscitation). Both of these formulations contain 1 mg of adrenaline. It may also be formulated with local anaesthetic solutions for infiltration, most frequently in concentrations of 1:200 000, but may be as high as 1:80 000 (with Lignocaine 2% for dental injection). It can also be presented in Auto-injectors for use in anaphylaxis (see below) in doses of 0.3 mg and 0.15 mg (EpiPen®) for intramuscular injection.
Racemic adrenaline is a mixture of dextro (D)- and levo (L)-rotatory isomers of adrenaline, where it is the L-adrenaline which is the active form. Therefore the racemic mixture is less active and may have fewer cardiovascular side effects when nebulised.
Pharmacodynamics
Adrenaline acts non-selectively at all the adrenergic receptors (α1, α2, β1, β2, β3) to produce a ‘flight or fight’ response. Its mechanism of action is via membrane receptors, which trigger a second messenger response as illustrated in figure 4. Its main effects are summarised in Table 1.
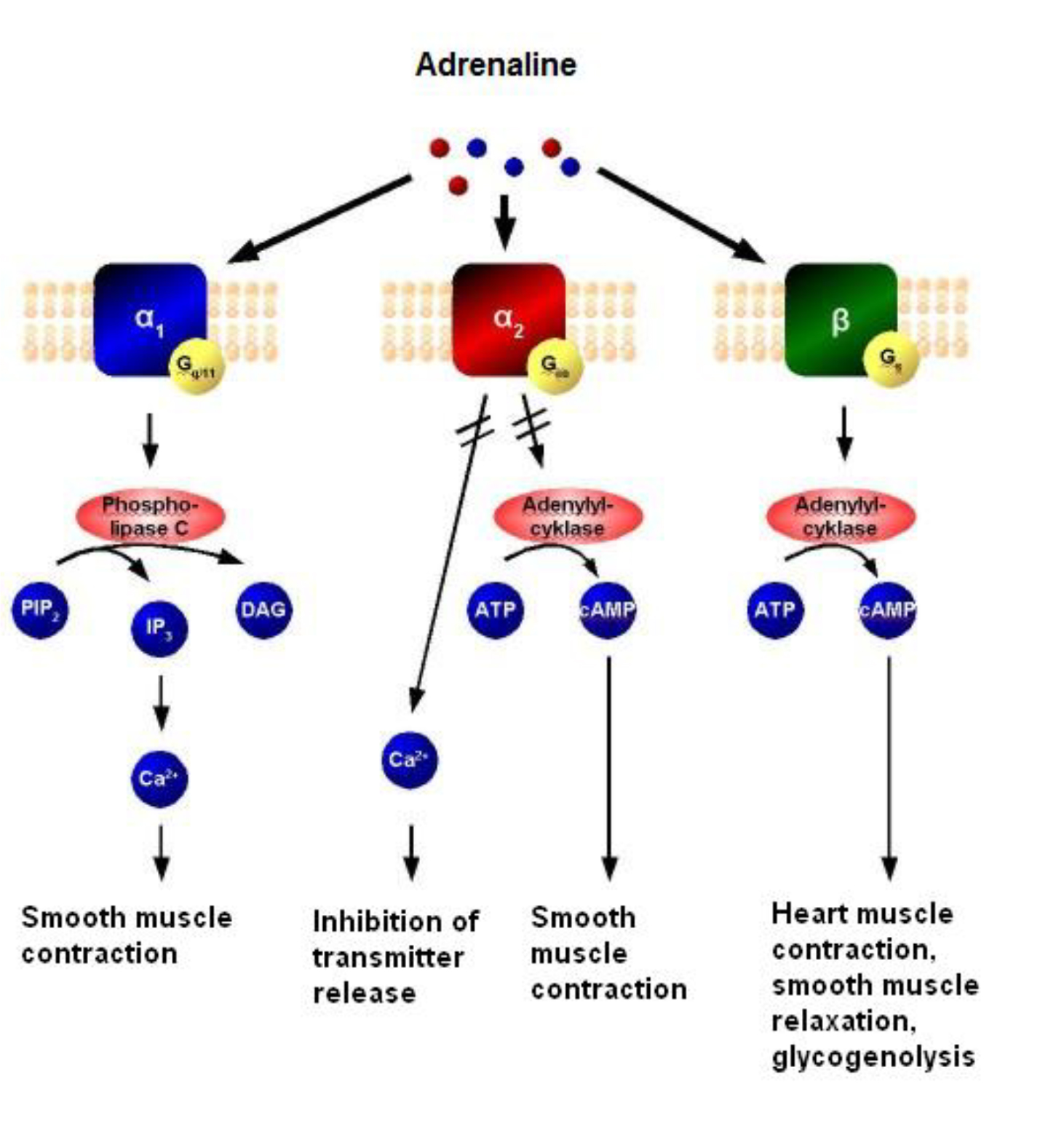
Figure 4. Receptors and 2nd messengers involved in Adrenaline actions.
Dose
The dose and route of administration of adrenaline depends upon the clinical indication for which it is used, and will be more fully discussed in the next section.
Side effects
Side effects relate directly to the exaggerated effects of adrenaline, most commonly owing to overdosage, inadvertent intravascular injection, or inappropriate use. These include palpitations, tremor, light headedness, tachycardia, arrhythmias, hypertension, cerebral haemorrhage and acute pulmonary oedema. Biochemical abnormalities may include lactic acidosis.
Indications
Clinical indications are discussed in the next section.
Contra-indications
There are no absolute contraindications to the use of adrenaline, but extreme caution should be shown whenever it is used owing to its profound effect on the cardiovascular system. Particular care must be taken when using it in patients suffering from arrhythmias, hypertension or ischaemic heart disease since these conditions may be acutely exacerbated. Caution should also be shown in patients taking monoamine oxidase inhibitors.
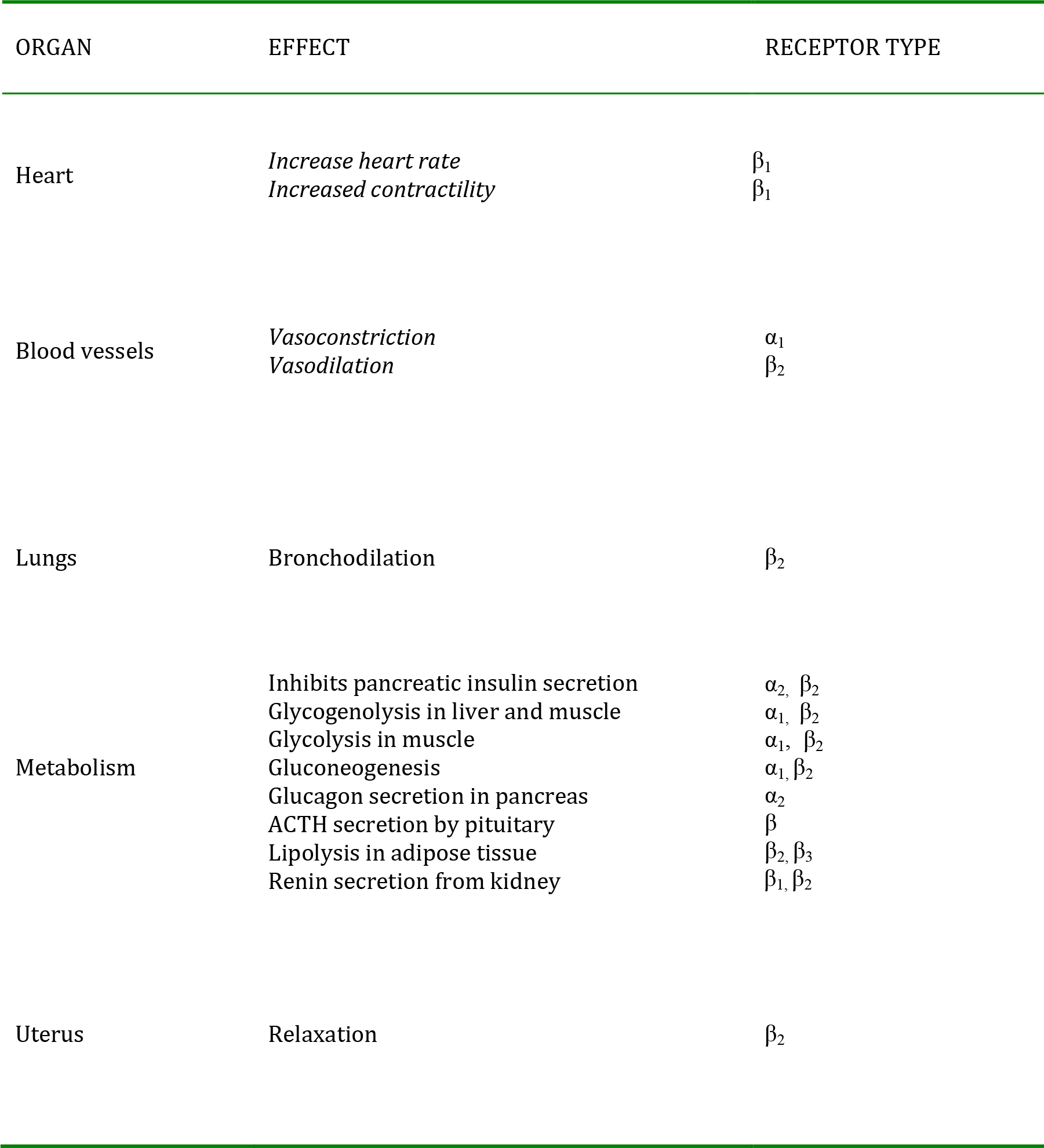
Table 1. Effects of adrenaline on organs and tissues in the body.
CLINICAL APPLICATIONS
The following conditions represent potential problems the anaesthetist may encounter in practice.
Resuscitation
Adrenaline is the drug of choice for the treatment of cardiac arrest. Its main action is to increase vascular resistance via alpha-1 receptor vasoconstriction, which improves perfusion pressure to the myocardium and brain.
Dose
When treating VF/VT cardiac arrest, 1mg is given once chest compressions have restarted after the third shock and then every 3-5 minutes (alternate CPR cycles).
For PEA arrest 1 mg is given as soon as intravascular access is achieved, and then every 3-5 minutes (alternate cycles).
If the cardiac output is severely compromised but there is still a recordable blood pressure, smaller doses should be titrated to effect, using a concentration of 1:100 000.
Current resuscitation guidelines should always be consulted since these are updated from time to time.
Route of administration
Adrenaline has its greatest effect when given intravenously, but in the event of failure to achieve access it may be given by the intraosseous route. Tracheal drug administration is no longer recommended because of its variable absorption and poor efficacy.
Anaphylaxis
Adrenaline is the drug of choice for the treatment of anaphylaxis. As an alpha-1agonist, it reverses the peripheral vasodilation caused by inflammatory mediator release, and also reduces oedema. Its beta-receptor activity dilates bronchial airways, increases myocardial contractility, suppresses histamine and leukotriene release and attenuates the severity of IgE-mediated allergic reactions.
Route of administration
The preferred route is intramuscular (IM) since adverse effects are less common, but for practitioners skilled at intravenous access and the use of IV adrenaline, it may be titrated cautiously (see table 2). For IM use, the anterolateral aspect of the middle third of the thigh is the best site for injection. The dose can be repeated at 5 minute intervals if there is no improvement and according to the patient’s response.

Table 2. Intramuscular and intravenous doses of adrenaline for the management of acute anaphylaxis
Inotropic support
Adrenaline may only be administered as a continuous infusion in the intensive care environment, and should only be administered via a central venous catheter with invasive blood pressure monitoring. The indications include: profoundly low blood pressure, shock, low cardiac output states and status asthmaticus.
Dosage
There is no single appropriate concentration, and the local ITU policies and guidelines should be observed. An example would be 4 mg Adrenaline diluted to 50 ml in saline or 5% dextrose, which is infused by means of a syringe driver. The target dose is usually given as microgram per minute (mcg/min) or microgram per kilogram per minute (mcg/kg/min). The rate of infusion is titrated to effect, usually to achieve a predetermined target blood pressure.
Airway obstruction
Severe croup is the most common airway indication for adrenaline, but it has been used in many other conditions where there is acute, life threatening upper airway obstruction which has an element of angio-oedema or inflammation. In these situations racemic adrenaline is delivered by the nebulized route. Its mechanism of action is to reduce the local inflammatory process and to provide local vasoconstriction, thereby reducing the obstruction caused by oedema.
Dosage
The dose for children is 0.5 ml/kg of a 1:1000 solution (maximum of 5 ml) of L-Adrenaline (the standard adrenaline used for resuscitation), placed undiluted into the chamber of the nebulizer. If racemic adrenaline is used the dose is 0.05 ml/kg (maximum 1.5 ml) of 1% solution diluted to 4 ml with normal saline. Smaller doses are described for conditions other than croup, but these may be increased or repeated until the desired effect is achieved. All the anticipated side effects of systemic adrenaline may occur (described above), so the patient should be carefully monitored in a high care environment.
Topical or local vasoconstriction
Owing to its local vasoconstricting action, adrenaline may be used as a topical application or combined with a local anaesthetic to be infiltrated. The addition of adrenaline to a local anaesthetic prolongs its action, as well as reducing bleeding for operations at the site of injection. The adrenaline may also be applied topically by the surgeon (e.g. to the nasal mucosa as part of Moffat’s solution) to reduce bleeding.
- To use adrenaline safely it is vital to understand the concentration and total dose of the adrenaline you are using
- 1ml of 1:1000 = 1 mg
- 1ml of 1:10 000 = 0.1 mg = 100 mcg
- 1ml of 1:100 000 = 0.01 mg = 10 mcg
- 1 ml of 1:200 000 = 0.005 mg = 5 mcg
ANSWERS TO QUESTIONS
- Which of the following statements concerning adrenaline is correct?
- False: it casuses vasoconstriction at alpha receptors
- True
- False: this is the cardiac arrest dosage. An infusion may be suitable for acute severe asthma
- False: It is metabolised by MAO and COMT
- Name five different clinical applications for adrenaline.
- Resuscitation for cardiac arrest
- Inotropic support in the ITU
- Anaphylaxis
- Severe croup
- As a local or topical vasoconstrictor
- Which of the following dosages are correct for adrenaline?
- False: Dose should be 10 ml of 1:10 000, or 1 mg
- True
- True
- True: or 0.5 ml/kg of 1:1000, to a maximum of 5 ml
- False: should be 0.05-0.1 mg boluses titrated to effect
- The following are likely side effects of adrenaline injection (true or false?):
- True
- False
- False: bradycardia may occur secondary to severe alpha vasoconstriction, but this is unusual and tachycardia is more likely
- True
- False; it causes bronchodilation
WEBLINKS
- Pharmacodynamics animation: http://www.wiziq.com/tutorial/32342-Action-of-epinephrine
- Resuscitation Council (UK) guidelines: http://www.resus.org.uk/siteindx.htm



