Basic Sciences
QUESTIONS
- Lithium :
- should be stopped 1 week preoperatively to avoid complications
- rarely causes side effects within the therapeutic range
- may cause hypothyroidism
- commonly causes tremor
- Clozapine:
- commonly causes extrapyramidal side effects
- is a traditional antipsychotic
- causes seizures and neutropenia
- does not cause weight gain
- Concerning antipsychotic drugs:
- Most drugs act at dopamine D1 receptors
- Most drugs cause sedation
- Newer atypical drugs are less likely to cause extra-pyramidal side effects
- It is advisable to stop treatment before surgery
- Neuroleptic malignant syndrome:
- is associated with malignant hyperthermia
- is treated with dantrolene
- results in raised creatinine kinase
- has a high mortality
INTRODUCTION
Psychiatric illness is common, affecting up to 10% of the population, with around 1 % diagnosed with a major psychiatric disorder. Many patients are prescribed long-term drug treatment, and the anaesthetist must be aware of potential interactions with anaesthetic agents.
Antidepressant drugs have been discussed in a previous tutorial. The classes of drugs which will be considered in this tutorial are mood stabilisers and antipsychotics. The use of tramadol in patients taking psychiatric drugs will also be mentioned briefly.
MOOD STABILISERS
Mood stabilisers are used to treat bipolar affective disorders which have a lifetime incidence of 1% in the UK. A manic or hypomanic episode is required for the diagnosis to be made. Some patients also suffer depressive episodes. Mood stabilisers include lithium and anticonvulsant drugs such as carbamazepine and sodium valproate. Mood stabilisers should not be stopped abruptly as there is a significant risk of relapse.
Lithium
Lithium is an inorganic ion. Its main therapeutic role is as a prophylactic agent in bipolar affective disorder. Occasionally it is used to enhance antidepressant therapy in recurrent depression. It mimics the action of sodium in the membranes of excitable cells and decreases the release of neurotransmitters. It has a low therapeutic ratio and plasma levels should be maintained at 0.6-1.0 mmol/l. Lithium is eliminated by the kidneys, and therefore if renal function is compromised or there is dehydration lithium levels rise dramatically. Side effects are very common within the therapeutic range and increase markedly above 1mmol/l. They include hand tremor, muscular weakness, nausea, polydipsia, and polyuria. ECG changes may occur such as T wave inversion, but clinically important cardiac effects are rare. Thyroid enlargement and hypothyroidism may also occur.
Lithium toxicity
Lithium toxicity occurs at >1.5mmol/l, and is exacerbated by hyponatraemia, dehydration, diuretics and renal impairment. Features of toxicity include vomiting, lethargy or restlessness, thirst, polyuria, ataxia and later hypokalaemia, renal failure, convulsions, coma and death.
The management of lithium poisoning is supportive, with correction of electrolyte imbalance and convulsions. Haemodialysis is required if renal failure is present, which may need to be repeated as tissue lithium enters the circulation.
Drug interactions with lithium
Thiazide diuretics reduce the clearance of lithium by the kidneys. Loop diuretics have a similar but weaker effect. NSAIDs may increase lithium levels by up to 40%, which can result in toxicity. The mechanism for this is not fully understood but it is thought to relate to the effect of NSAIDs on fluid balance.
ACE inhibitors not only reduce the excretion of lithium but may also cause renal failure. Care is also required when co-prescribing lithium and angiotensin 2 antagonists.
Anaesthetic implications of lithium therapy
Lithium does not need to be stopped for minor surgery; it has been suggested that it should be stopped 24 – 48 hours before major surgery but this is disputed. From a psychiatric perspective interruptions in lithium therapy are bad for the patient since there is good evidence that they lead to a worse course of affective disturbance than if the patient was left untreated. Lithium prolongs both depolarising and non depolarising neuromuscular block, therefore a nerve stimulator should be used. It may also reduce anaesthetic requirements as it blocks brain stem release of noradrenaline and dopamine. Drugs which may exacerbate renal impairment should be used with caution, including NSAIDs which as mentioned above may also increase lithium levels. Careful attention should be paid to fluid and electrolyte balance. If discontinued, lithium should be restarted 24 hours post-op.
Carbamazepine
Carbamazepine is an anticonvulsant which is used in the prophylaxis of bipolar affective disorder. It is a second line treatment since it is proven to be less efficacous than lithium. It is also used to reduce aggression and anger.
Carbamazepine causes dizziness, drowsiness, ataxia and nausea. It is a potent inducer of hepatic enzymes, and thus reduces the plasma levels of many drugs including benzodiazepines, thyroxine, theophylline, and oestrogens, It may cause a chronically low white cell count and in 1 in 20,000 patients this can develop into agranulocytocis or aplastic anaemia. Furthermore it can cause derangement of liver enzymes (raised ALP and GGT) and drug-induced hepatitis. There is an increased risk of hyponatraemia when carbamazepine is given with a diuretic. It is also teratogenic.
Sodium valproate
There are two forms of sodium valproate commonly used in psychiatry: sodium valproate (Epilim) and semi-sodium valproate (Depakote). Sodium valproate is used both as a prophylactic agent in bipolar affective disorder and to treat acute mania. It is generally well tolerated, but possible side effects include nausea, gastric irritation, diarrhoea, weight gain, hyperammonaemia and thrombocytopenia. It is also teratogenic.
Sodium valproate is highly protein bound and therefore displaces other protein bound drugs such as warfarin, leading to increased therapeutic levels and possible toxicity. It undergoes hepatic metabolism, therefore increased levels may occur when given with other drugs which are enzyme inhibitors such as erythromycin and cimetidine.
ANTIPSYCHOTIC DRUGS
Antipsychotic drugs are used in the treatment of psychoses such as schizophrenia and mania. They treat the acute symptoms of hallucinations and delusions and in the case of schizophrenia are used prophylactically often for long periods. Most drugs act by antagonism at the dopamine (D2) receptors in the central nervous system. They can be classified into two groups:
(1) Neuroleptic or typical antipsychotics (chlorpromazine, haloperidol, trifluoperazine) which have a propensity to cause extrapyramidal side effects: acute dystonia, akathisia, parkinsonism and tardive dyskinesia.
(2) Atypical antipsychotics (clozapine, olanzapine, respiridone, amisulpride, quetiapine and aripirazole) which do not have a tendency to cause extrapyramidal side effects. They too act via D2 receptor blockade but also have effects on other receptors including histamine (H1), serotonin (5-HT2), acetylcholine (muscarinic) and alpha-adrenergic receptors. Clozapine causes seizures and neutropenia, (the latter necessitating regular monitoring of the neutrophil count).
Adverse effects of antipsychotic drugs
Side effects from antipsychotic drugs are extremely common. In addition to those described above, most drugs cause sedation due to blockade of central histamine H1 and/or α1 receptors. Weight gain, gynaecomastia and postural hypotension are also very common.
Cardiac risk
Patients suffering from chronic schizophrenia have a high incidence of cardiovascular disease associated with increased body weight, diabetes and smoking. In addition, antipsychotic drugs cause an increased risk of sudden death due to changes in the electrical conduction within the myocardium. Common ECG changes associated with antipsychotic drugs include prolongation of the QT and PR intervals and T wave changes. QT prolongation is a marker for torsades de pointes.
Table 1 lists the relative incidence and/or severity of a number of side effects which increase anaesthetic risk.
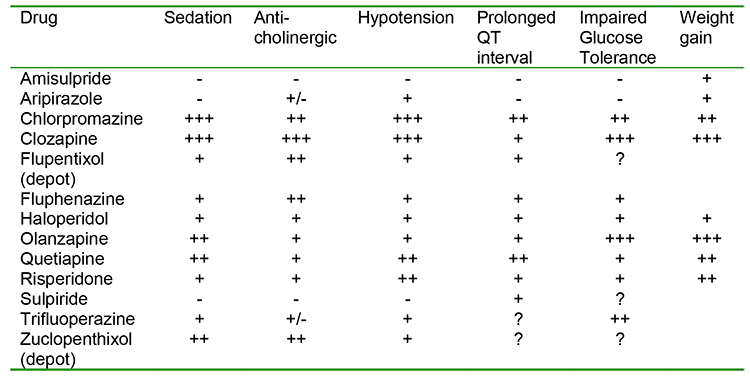
Table 1: Adverse effects of antipsychotic drugs
Neuroleptic malignant syndrome
This is an unusual idiosyncratic reaction to antipsychotic drugs, characterised by acute increase in body temperature, muscle rigidity and autonomic disturbance (unstable blood pressure, sweating, salivation, loss of sphincter control). Creatinine kinase and white cell count are usually raised. Mortality is up to 20%. Patients should be treated in ICU; dantrolene is used along with supportive treatment. Despite the clinical similarities with malignant hyperthermia, there is no proven association between the two conditions.
Anaesthesia for patients taking antipsychotic drugs
Antipsychotic medication should be continued perioperatively, as abrupt withdrawal may result in recurrence of psychotic symptoms. It may also increase the incidence of postoperative confusion, which is high in those suffering with schizophrenia. Antipsychotic drugs potentiate the hypotensive and sedative effects of general anaesthetic agents; therefore care is required with induction of anaesthesia. Temperature regulation during anaesthesia may be impaired due to the effects of dopamine blockade on the hypothalamus. Patients with schizophrenia appear to be less sensitive to post operative pain. They have a higher than usual incidence of developing postoperative paralytic ileus, which is thought to be due to sympathetic hyperactivity, and can be reduced by epidural analgesia. They also have increased rates of infection due to immune suppression, and are at risk of water intoxication due to hypersecretion of ADH, both effects thought to be a consequence of antipsychotic medication. Increased mortality rates in the post operative period have also been shown in those on long term antipsychotic treatment, attributable to a variety of causes, including cardiac complications, respiratory arrest and complications after paralytic ileus.
TRAMADOL AND PSYCHIATRIC DRUGS
The use of tramadol in patients taking psychiatric medication is of particular interest as tramadol may itself cause psychiatric symptoms: altered mood (elation or dysphoria) hallucinations, confusion, sleep disturbance and nightmares. As mentioned in our previous article tramadol may precipitate the serotonin syndrome when combined with antidepressant medication, which raise the level of this neurotransmitter.
When combined with antipsychotics, selective serotonin re-uptake inhibitors or tricyclic antidepressants, tramadol reduces the seizure threshold.
Carbamazepine induces the metabolism of tramadol and therefore co-administration of these drugs leads to a reduced efficacy of tramadol.
ANSWERS TO QUESTIONS
- FFTT
- FFTF
- FTTF
- FTTT
SUMMARY
- Mood stabilisers and antipsychotic drugs should be continued throughout the perioperative period to avoid the risk of relapse.
- Lithium has a low therapeutic index and high incidence of toxicity.
- Patients taking lithium require care with fluids and electrolytes, and avoidance of drugs which may cause renal failure.
- Cardiac risk factors are increased in patients taking long term antipsychotic drugs due to a combination of side effects and high smoking levels in these patients.
- Patients taking long term antipsychotics are at risk of increased complications (including death) during and after surgery.
WEBLINKS
- Perioperative Management of Schizophrenic patients. Kudoh A. Anaesthesia and Analgesia 2005; 101: 1867-72 www.anesthesia-analgesia.org/cgi/reprint/101/6/1867
REFERENCES and FURTHER READING
- Allman KG, Wilson IH. Oxford Handbook of Anaesthesia (2nd Edition). 2006.
- Peck TE, Hill SA, Williams M. Pharmacology for Anaesthesia and Intensive Care (3rd Edition). 2008.
- Taylor D, Paton C, Kerwin R. The Maudsley Prescribing Guidelines (9th Edition). 2007.



