Self Assessment
- Inguinal hernias:
a) Are more common in boys
b) Cause fewer problems than umbilical hernias
c) Do not require surgery in children less than 1 year
d) Are associated with undescended testis
e) Should be repaired electively - Strangulated hernia:
a) Produces severe pain
b) Symptoms include nausea and vomiting
c) Should always have non-operative reduction attempted
d) Should always be operated on immediately - Sighs of severe dehydration in children include:
a) Cool peripheries
b) Decreased core-peripheral temperature gap
c) Capillary refill time <2s
d) Thready pulse
e) Reduced conscious level - Fluid resuscitation:
a) Initial fluid bolus of 80ml should be given to 8kg child
b) Hartmann’s solution/ Ringers lactate are appropriate fluids
c) Normal saline should not be used
d) The patient should be reassessed after each fluid bolus
e) 5% dextrose is an acceptable alternative - Anaesthesia for emergency obstructed inguinal hernia repair in a 2 year old:
a) Inhalational anaesthesia is the method of choice
b) Cricoid pressure would be ineffective
c) Tracheal tube size can be calculated using the formula age/4 +4
d) Correct length of oral tube can be approximated to internal diameter x 2
Case History
An eight month old boy presented to paediatric filter clinic as a referral from a peripheral hospital about 300km away. The child had a diagnosis of strangulated hernia with symptoms for two days and had been referred for surgery. The referring facility had started an IV 5% dextrose drip for transfer, but during the long 12 hour transfer on bad roads this had come out. Further history was limited as the parents did not speak the local dialect.
On arrival to the hospital the child was drowsy, dehydrated, tachypnoeic and had a distended abdomen. The capillary refill time was 20 seconds, the pulse thready with a heart rate of 167/min.
Abdominal examination revealed a grossly distended abdomen with scrotum filled with loops of bowel.
Investigations showed an Hb 8g/dl (PCV of 26%) and Na 126mmol/l, K3.1mmol/l.
The diagnosis of strangulated inguinal hernia was confirmed and the child prepared for theatre.
Introduction
Hernias are very common and can occur anywhere where the muscles of the abdomen become weak or tear. This may result in the contents of the abdominal cavity pushing through the weakness and producing a bulge or protrusion.
In children, hernias result form a weakness that is present from birth and may only be noticed when the child is coughing, crying or straining. The majority of hernias in children occur in the groin.
Inguinal hernias
Inguinal hernias are more common in boys (80%), are always indirect and often bilateral. In boys they are often associated with undescended testis and in girls under two the hernial sac often contains the ovary.
A simple hernia in itself does not cause any problems. Umbilical hernias reduce in size over time and the only problem is cosmetic. Conversely, inguinal hernias tend to increase in size over time and can lead to serious complications such as bowel obstruction. Ideally, all inguinal hernias in children should be repaired electively. Children less than one year should be operated on as urgent elective cases as the hernia is at a high risk of obstruction.
Strangulated Hernia
If a portion of bowel pushes through the abdominal wall and becomes trapped it can produce symptoms of severe pain, nausea and vomiting. The blood supply to the trapped bowel may become compromised. Emergency surgery is essential to prevent irreversible ischaemic damage to the bowel.
Symptoms and signs of strangulated hernia
- Severe pain
- Vomiting
- Redness over abdominal wall and groin
- Distended abdomen
- Fever
- Dehydration
If there is a short history without bowel obstruction, initial management can include attempted reduction of the hernia without sedation. However, if the hernia remains irreducible or if there is a prolonged history or there is abdominal distension, the hernia should be operated as soon as possible after the patient has been appropriately resuscitated.
Pre operative assessment
Children presenting with a strangulated inguinal hernia may be extremely distressed in severe pain and dehydrated. Assessment and appropriate resuscitation is essential before considering taking the child to theatre. Assessment of dehydration and hypovolaemia is made on clinical grounds. Severe dehydration is usually associated with shock.
Clinical signs of dehydration
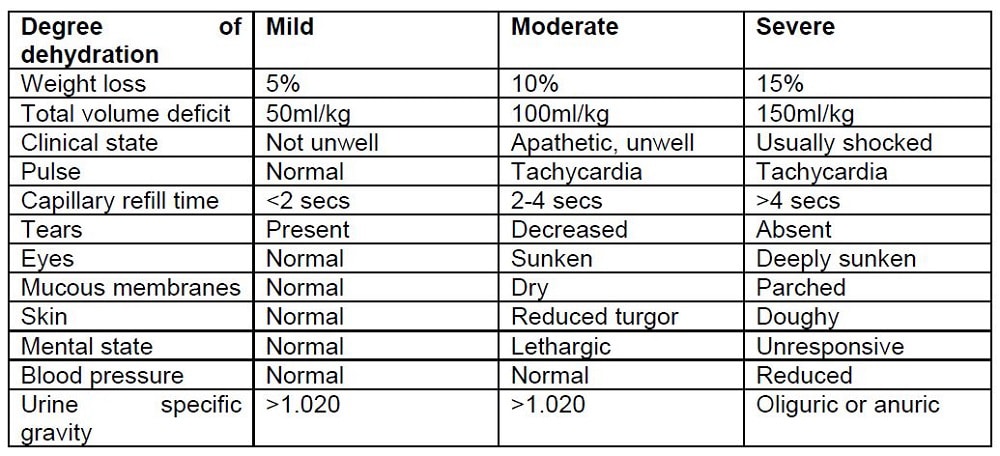
Clinical signs of shock
Shock occurs when there is potential circulatory failure. It may be due to a number of reasons (blood loss, sepsis, burns, cardiac disease, anaphylaxis), including severe dehydration as in this case.
- Tachycardia
- Tachypnoea
- Reduced peripheral perfusion, cool peripheries
- Reduced pulse volume – absent or weak peripheral pulses, weak central pulses
- Delayed capillary refill >2 secs
- Agitation, then reduced level of consciousness
- Hypotension
- Oliguria or anuria
The child described in the case history is showing signs of severe dehydration and shock and requires urgent resuscitation. Hypotension is a late sign and indicates a significant amount of fluid loss.
Resuscitation
Although surgery is urgent as the bowel may be compromised, resuscitation cannot be overlooked and a few hours of appropriative fluid replacement is essential in achieving a successful outcome.
Fluid resuscitation initially should consist of fluid boluses of either isotonic crystalloid (normal saline, Hartmann’s/Ringers lactate) or colloid at a dose of 20ml/kg (i.e. 160ml bolus for 8kg child). The patient should then be reassessed looking for improvement in clinical signs – improved perfusion, reduced capillary refill time, reduced heart rate with the child becoming more alert. Several repeated fluid boluses may be required during resuscitation to correct the signs of shock, but the total estimated fluid deficit in dehydration need only be replaced over 24 hours.
5% dextrose should never be used in the resuscitation of the shocked patient.
If there is pre-existing anaemia blood may be used for resuscitation if large volumes of fluid are required.
The child is at risk of aspiration due to the obstruction and vomiting. An NG tube should be placed and left on free drainage. If NG aspirates are large they should be taken into consideration when calculating fluid requirements.
Regular blood glucose monitoring is essential especially neonates. If the blood sugar is less than 3 mmol/l, treat with 3-5 ml/kg 10% dextrose as a bolus.
Preoperative assessment
In addition to resuscitation and preparation of the patient for theatre, a full pre anaesthetic assessment should be sought.
History
- Duration of symptoms
- Last meal taken
- Past medical conditions including birth history
- Previous admissions
- Intercurrent infections: cough, URTI, malaria
- Cardiovascular assessment – failure to thrive, heart murmurs
- Drug history and allergies
Examination
- Sighs of shock, as described above
- Airway – mouth opening, loose teeth
- Cardiovascular – murmurs
- Respiratory – wheeze, breath sounds, signs of infection
- Abdominal – distension
Preoperative fasting
Fasting aims to reduce risk of regurgitation of gastric contents and subsequent pulmonary aspiration. For elective surgery children should be fasted for 6 hours following solid food or formula milk, 4 hours for breast milk and 2 hours for clear fluids.
In the case of emergency surgery, consider the risks and benefits of proceeding if the child is not fasted. Gastric emptying is delayed in obstructed hernia so even if the child has been starved for 6 hours or more they should be treated as if they have a full stomach.
Preoperative Investigations
Full blood count should be checked, especially haemoglobin. This is particularly important when the symptoms have been for a long duration and bowel resection and anastomosis is anticipated. Blood should be taken for typing and cross match.
Plasma electrolytes should be checked, especially sodium and potassium.
In the case history described the child is demonstrating severe hyponatraemia due to electrolyte loss into the distended bowel and/or the inappropriate use of 5% dextrose for resuscitation (Na+ 126 mmol/l, normal value 135 -145 mmol/l). The only crystalloid solutions that should be used for resuscitation are Hartmann’s solution/ Ringers lactate or normal saline. There is no place for 5% dextrose in resuscitation or normal maintenance fluid in children. The potassium is low – this should be monitored and potassium added to maintenance fluids after surgery, if required.
Preparation for theatre
It is important to prepare the drugs and equipment that you will require prior to the child arriving. Check your equipment is available and working. Check the anaesthetic machine and suction. Ensure that you have an assistant and formulate an anaesthetic plan.
Calculate the doses and draw up any drugs you intend to use.
Check you have appropriate sized tracheal tube (and have one half size larger and smaller just in case). Tube size can also be approximated to the size of the little finger.
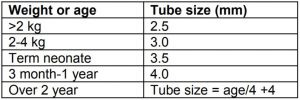
Ideally, theatre temperature should be about 21°C. Hypothermia is difficult to treat and care should be taken to prevent it. Children should be kept covered and exposure kept to a minimum.
Induction of anaesthesia
Induction of anaesthesia should only take place when the child is fully prepared and resuscitated and you are fully prepared. Precordial stethoscope and pulse oximeter should be applied prior to induction of anaesthesia.
The NG tube should be aspirated using a syringe to ensure the stomach is as empty as possible and precautions taken against regurgitation.
Anaesthesia is induced using a modified rapid sequence induction with the application of cricoid pressure before securing the airway with a tracheal tube. Adequate preoxygenation during rapid sequence induction is impossible in children; mask ventilation with continued cricoid pressure will be required prior to intubation. Induction of anaesthesia may be achieved using sodium thiopentone 3-5mg/kg or ketamine 1-2mg/kg or propofol 3-5mg/kg. Reduced doses may be needed in the severely unwell child. Occasionally inhalational induction is necessary, but deep inhalational anaesthesia should be avoided, especially in an unwell child. It is advisable to give a dose of atropine (20mcg/kg) to avoid bradycardia prior to suxamethonium 1-2mg/kg.
Care should be taken to ensure that the tracheal tube is secured at the correct length to avoid endobrochial intubation or inadvertent extubation. The position of the tube should be checked clinically by auscultation of the chest to ensure bilateral and equal air entry. As a guide, tube length in cm can be estimated using formula: Tube length = 3 x internal diameter
Confirm the IV cannula is working and that you have access to it. Connect any fluids to the line and make sure you have an easily accessible point to administer drugs. Only let the surgeon start operating when you are completely ready.
Maintenance of anaesthesia
Anaesthesia should be maintained using intermittent positive pressure ventilation with a volatile agent or intermittent ketamine, ideally using a nondepolarising muscle relaxant such as atracurium or vecuronium. Ideal minimal monitoring includes precordial stethoscope, pulse oximetry, blood pressure monitoring, ECG, end tidal carbon dioxide, volatile agent and ventilator disconnect alarm. The presence of an alert anaesthetist is crucial!
Intra-operative fluids
Intraoperative fluid used should be isotonic crystalloids (Ringers lactate/Hartmann’s or normal saline), colloids or blood. Assuming the child has been adequately resuscitated preoperatively, give fluid boluses of 20ml/kg according to the clinical state of the child (heart rate, pulse pressure, capillary refill) and observed fluid losses from the surgical fluid. For a full laparotomy, volumes of 40-60ml/kg are commonly required (blood volume 80ml/kg).
Children tolerate anaemia relatively well, but transfusion should be considered when the haemoglobin approaches 6 g/dl, especially if there is on-going blood loss. If blood is required, a useful formula to estimate the volume required is shown below:

Analgesic Plan
A combination of simple analgesics, intravenous opioids or ketamine, and local anaesthesia provides the best pain relief (multimodal analgesia). NSAIDs are effective analgesics but may precipitate renal failure in patients with severe dehydration. NSAIDs should be avoided in the case described here – paracetamol is a suitable alternative.
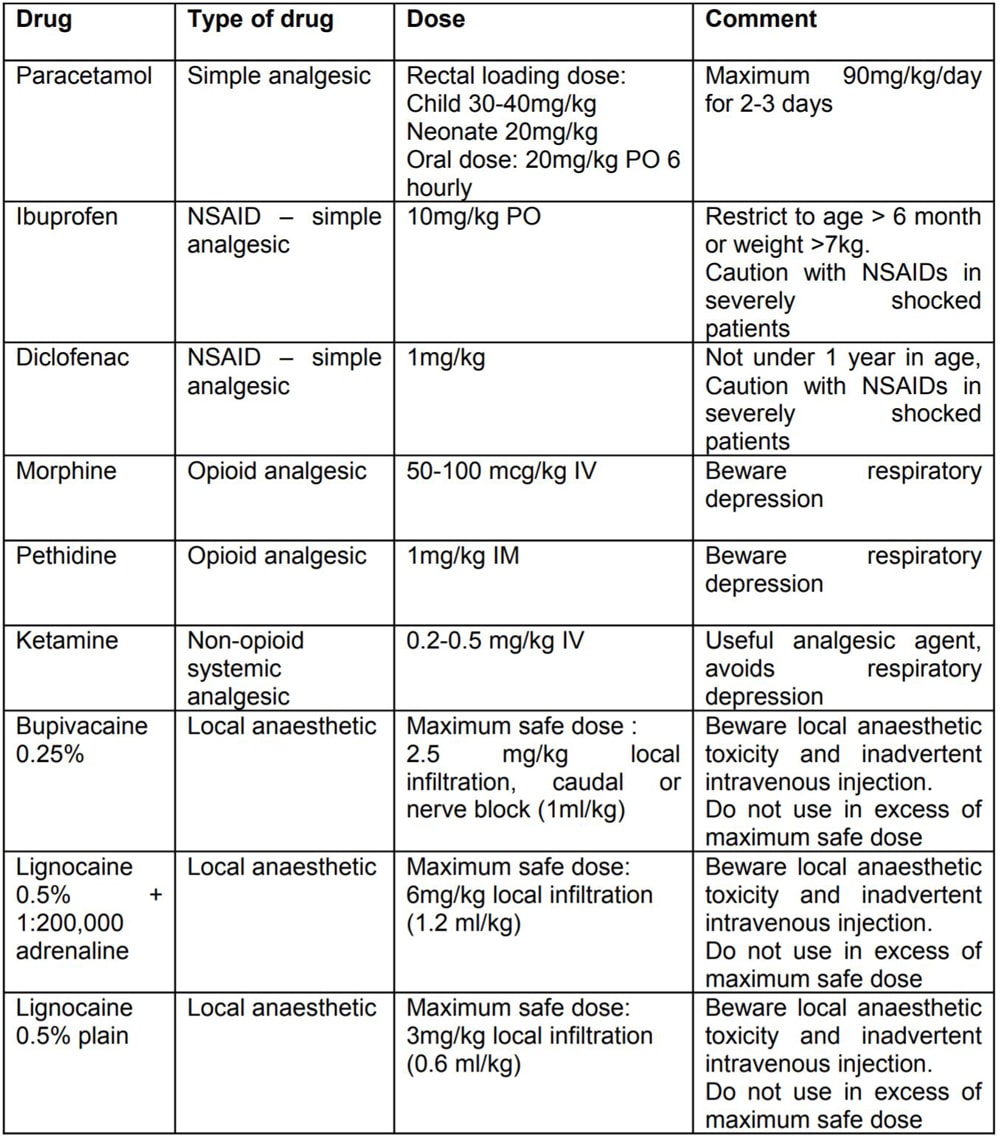
Regional anaesthesia
A caudal or ileoinguinal block would provide appropriate analgesia for inguinal hernia repair. Both should be performed once the child is anaesthetised prior to the start of surgery.
Caudal block (see www.nysora.com for further reading)
Aseptic technique is essential. With the patient in the left lateral position the legs are flexed and the sacral hiatus identified. Direct a short bevelled needle or 22G cannula at 60° to the skin, through the sacrococcygeal membrane and then flatten and advance slowly into the caudal epidural space. Aspirate gently to check the needle has not entered a blood vessel or caused inadvertent dural puncture.
Inject bupivacaine 0.25% at a dose of 1ml/kg to achieve a block level T9-S5 (maximum volume 20ml). An alternative is 1% lignocaine with adrenaline 1:200,000 at a maximum dose of 6mg/kg, although the duration of the block is shorter than that with bupivacaine.
With practice caudal block is a good safe block. However, motor block, urinary retention, dural puncture and intravascular injection can occur rarely.
Ilioinguinal block (see www.nysora.com for further reading)
This is a useful alternative to the caudal block. Direct a blunted 23G needle at a point equivalent to the child’s finger breadth medial to the anterior iliac spine, at right angles to the skin. Resistance is felt at the aponeurosis to the external oblique and then a pop as it passes through. Aspirate and then inject up to 0.5ml/kg of 0.25% bupivacaine. It is useful to save 1-2ml of bupivacaine to inject subcutaneously.
This is an easy block to perform and has a low complication rate, however if the injection is too medial, perforation of the bowel can occur.
In the case described as the abdomen is distended it may be safer to get the surgeon to infiltrate local anaesthetic at the end of surgery.
Extubation
Following emergency abdominal surgery children should be extubated awake to ensure airway reflexes are intact.
Postoperative management
The child can be transferred back to the ward when they are fully awake, no longer have an oxygen requirement and are warm and pain free. Ideally fluids should be replaced in theatre but if intravenous fluids are requiredpostoperatively, clear instructions should be given to the ward nurses.
Maintenance fluid is calculated using the Holliday and Segar ‘4-2-1’ formula. 5% dextrose 0.9% saline or 5% dextrose 0.45% saline are acceptable solutions; only 5% dextrose 0.9% saline should be used initially in this case as the child is hyponatraemic. Fluid should be restricted to 2/3 maintenance in the first 24 hours.
The Holliday and Segar Formula: the average maintenance requirement for fluid in healthy children
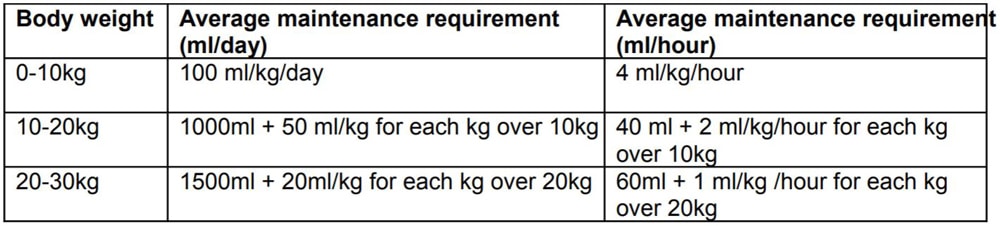
For example, a 25kg child needs (60+5) 65ml/hr maintenance fluid. Remember that maintenance makes no allowance for increased losses due to intestinal obstruction or pyrexia so patients may continue to require addition fluid boluses to maintain normovolaemia. Additional potassium may also be required. It is essential that fluid and electrolyte balance is closely monitored.
Case History Continued
The child weighed 6kgs. He was given an initial bolus of Hartmann’s solution 120mls. His clinical status improved but at assessment after 20 minutes still had delayed capillary refill and cool peripheries. Two more boluses of Hartmann’s 20ml/kg were given. Blood for cross match was taken and one unit whole blood requested. The baby was wrapped in warm sheets.
In theatre, a warming electric blanket and warm fluid both for infusion and cleaning the abdomen was available.
ECG, pulse oximetry and NIBP monitoring were placed on the child and induction of anaesthesia performed using a rapid sequence induction with sodium thiopentone, suxamethonium and atropine in appropriate doses after preoxygenation. Maintenance was with oxygen and halothane, with atracurium for muscle relaxation. Manual IPPV using an Ayre’s T-piece was used.
A caudal block with 6mls 0.25% bupivacaine was given.
Intraoperatively, the strangulated bowel was found to be unviable and a resection and primary anastomoses done. Hartmann’s 40ml/kg and blood 20ml/kg were required intraoperatively. The child was reversed at the end of surgery and taken back to the ward.
Maintenance fluids were given for 48hours postoperatively with careful monitoring of fluid balance and electrolytes. Post-op recovery was uneventful.
Summary
Obstructed hernia in children is a common surgical emergency. A successful outcome depends appropriate assessment and resuscitation of the patient prior to theatre with normal saline, Hartmann’s or Ringers lactate. An NG tube is essential prior to induction of anaesthesia.
Airway protection from aspiration during anaesthesia is essential. Take care to ensure the child is kept warm and has adequate fluid replacement during surgery. Following emergency surgery children should always be extubated awake.
Post operative analgesia is should be provided with a combination of simple analgesics, systemic analgesia and regional analgesia (either with a caudal, ilioinguinal block or infiltration of local anaesthetic). NSAIDs should be avoided in children with severe dehydration or sepsis – paracetamol is a suitable alternative.
Further reading
Simon Berg. Paediatric and neonatal anaesthesia. In: Oxford Handbook of Anaesthesia Ed K.G. Allman, I.H. Wilson Oxford University Press 2006
Answers to MCQ
- a) T b) F c) F d) T e) T
- a) T b) T c) F d) F
- a) T b) F c) F d) T e) T
- a) F b) T c) F d) T e) F
- a) F b) F c) T d) F



