Patient Safety
QUESTIONS
Before continuing, try to answer the following questions. The answers can be found at the end of the article, together with an explanation. Please answer True or False:
- Regarding stress in the field of anaesthesia:
a. Stress is always perceived negatively
b. Stress is only inherent in the field of anaesthesia
c. The body reacts to stress by involving only mental responses
d. Incidence is estimated to be around 20%
e. Lacking professional qualification is a risk for occupational stress - The following statements are correct with regards to coping skills:
a. Emotion-focused coping is useful when dealing with sudden death in the family
b. Problem-focused coping generates anxiety, fear and frustration
c. Confrontation is an effective way to reduce the undesirable symptoms of stress
d. Patient care is affected when anaesthesiologists develop longstanding maladaptive coping
e. Poorly coping individuals are at risk of cardiovascular diseases - Concerning methods to reduce occupational related stress:
a. Occasional optimistic thinking is a good strategy to de-stress
b. Writing down a stress journal is effective for keeping a mental account
c. Taking a pause is helpful
d. Overworking is justified as long as it is accounted by adequate financial gains
e. Setting up a taskforce to safeguard professional well-being is helpful
Key Points
- Occupation-related stress is common in anaesthesia and the presence of multiple risk factors increases the risk of burnout
- Anaesthesiologists should be aware of the need to handle stress throughout their career
- Adaptive coping skills should be encouraged as a way to maintain professional well-being
- Medical organisations have the executive power and duty to provide a state of positive professional well-being for their staff
INTRODUCTION
Providing safe anaesthesia is challenging. Most healthcare providers in anaesthesia are expected to maintain efficient patient care and are subjected to intense occupational related stress as a routine. Their needs are often not considered due to the nature of their work environment. The Code of Ethics states that physicians have an ethical responsibility and duty to preserve and improve their own physical, social and mental health1.This article aims to promote insight about professional health and well-being amongst health care providers in the field of anaesthesia.
MENTAL HEALTH
Over the years, efforts to define mental health comprehensively have been divided. Some identified obstacles have been due to cultural barriers, variation in societal understanding and ignorance as well as opposing ideologies. The first formal attempt to define mental health came after the International Congress on Mental Health in 19502. Since then, the World Health Organization (WHO) has appropriately revised its Constitution’s definition of mental health as a state of well-being in which every individual realizes his or her potential, can cope with the normal stresses of life, can work productively and fruitfully, and is able to make a contribution to her or his community3.This emphasises the mental component of health which is a state of complete physical, mental and social well-being and not merely the absence of disease or infirmity.
STRESS
The term stress is familiar to all and used on a daily basis. The three components below highlight the dynamic definition of stress4:
- Deviation from a normal environment
- Evaluation of the changes in the environment
- Body’s natural protective mental, emotional or physical response
The components can be summarised into an equation shown below:
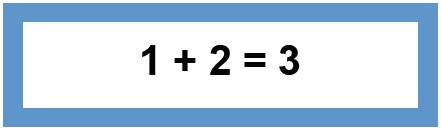
The definition features the importance of stress as a positive motivation and is an integral part of life5. However, the individual becomes strained when the arousal stress response becomes too great and has a negative impact on the individual, as shown in Figure 1. Stress may be cyclical, repetitive or chronic. Unchecked, the impact can be lasting and deleterious.
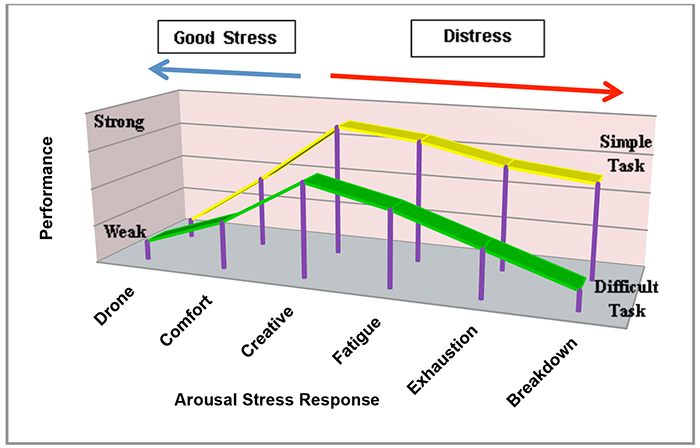
Figure 1: Yerkes-Dodson Law. Relationship between professional performance and arousal stress response
ANAESTHESIA & STRESS
Individuals who are inclined towards a career in medicine are often intelligent, compassionate and sensitive. Unfortunately, they also commonly exhibit type A personality traits such as increased hostility, impatience, ambition and obsession5. Such character traits are possibly required to complete medical training and to endure daily professional challenges. However, these characteristics may also make individuals prone to maladaptive coping when encountering repetitive or extremely difficult situations.
Most occupations are associated with stress as it is an inherent part of work commitment and responsibility. While occupational related stress level is generally reported by 18% of individuals, studies have shown higher levels at 28% in the medical profession6. Specifically, the incidence is more alarming in anaesthesia. Some regions have reported 50-96% of anaesthesiologists suffering from high levels of stress7.
Risk factors for stress and burnout in anaesthesiologists are listed in Figure 25,7-8. The presence of multiple risk factors increases the risk of burnout.
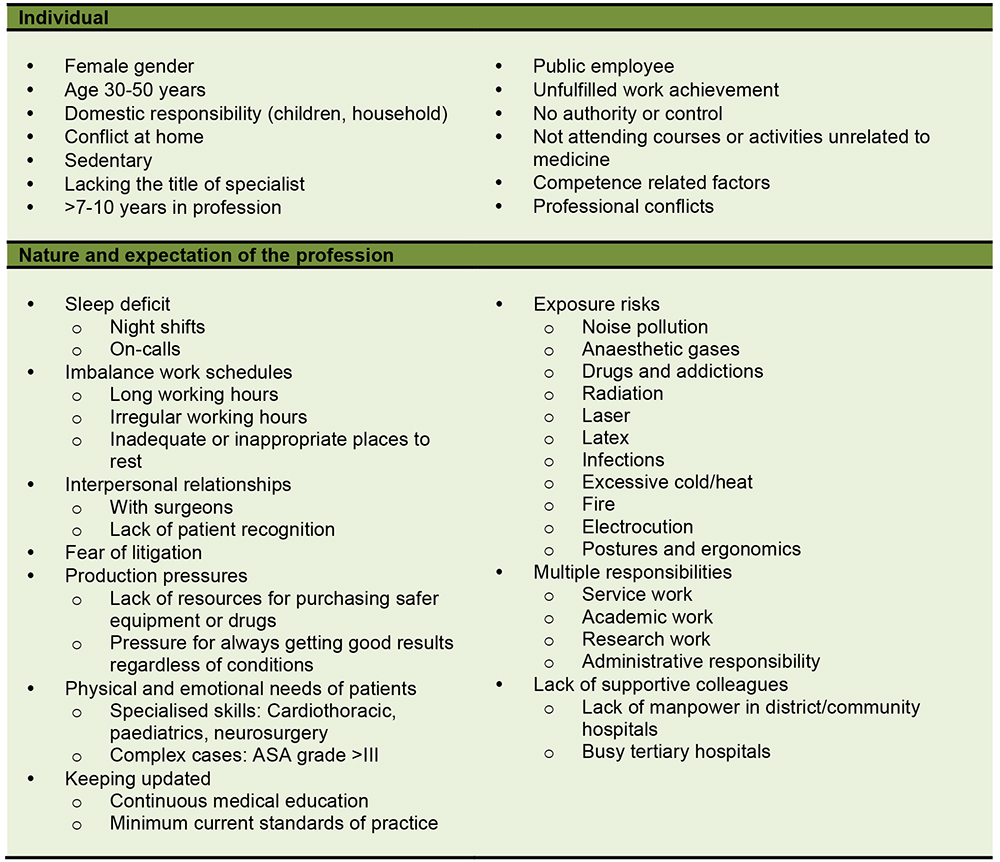
Figure 2: Risk factors for professional stress and burnout in anaesthesiologists
COPING SKILLS AND CAPACITY
Coping describes the dynamic thought and physical reactions required to solve disagreements related to the perceived threat(s) in the environment. It is a problem-solving technique that aims to reduce negative stress. Folkman and Lazarus described common methods of coping in 1985 (Figure 3)9.
Emotion-focused coping depends on managing emotions triggered by the stressful environment. The unwanted negative emotions are fear, anxiety, embarrassment, depression and frustration. This coping method is used when the perceived threat is beyond the individual’s control and is aimed at reducing the exaggerated emotional response. Problem-focused coping depends on deriving an active solution to solve a specific problem. It is best applied on modifiable stressors. This coping style is not useful if the individual perceives the threat as non-controllable. Both forms of coping are mutually exclusive but can co-exist and can be complimentary. An individual may show simultaneous overlapping skills such as obtaining social support to solve a specific issue.
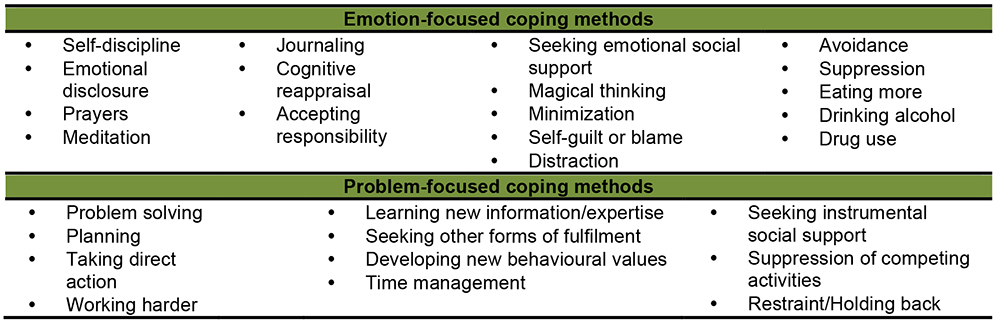
Figure 3: Types of coping mechanisms
Unhealthy forms of coping occur when the stressor is perceived adversely. Maladaptive coping only reduces undesirable symptoms temporarily. It does not remove the source of the stressor. This perpetuates the vicious cycle associated with strengthening of negative behavioural responses. The outcome for the individual may be poor, and/or they may neglect institutional responsibilities if the problem is not addressed (Figure 4).
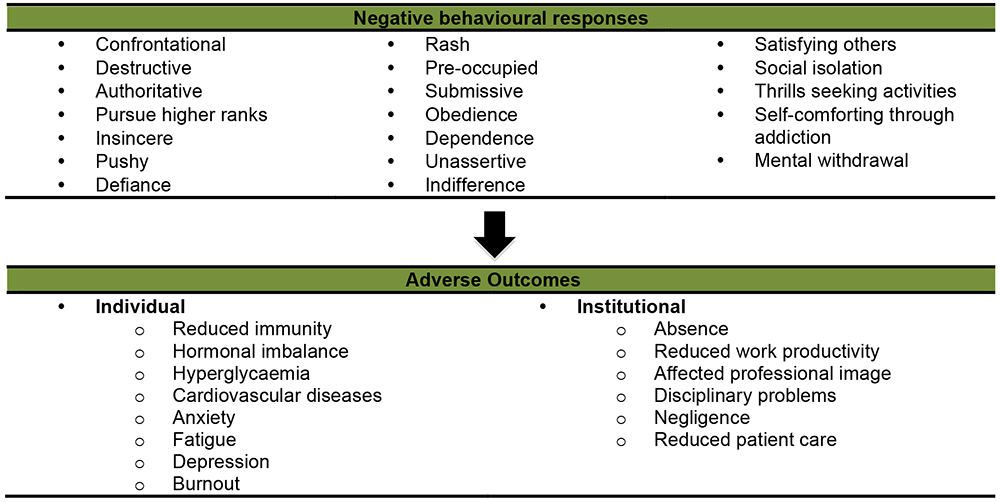
Figure 4: Types of maladaptive coping and its associated adverse outcomes
ASSESSING INDIVIDUALS AT RISK
There are various objective models to measure professional well-being. Unfortunately, most are aimed at measuring general tendencies to mental disorders amongst physicians, and none are robust enough to measure professional wellbeing specifically related to anaesthesiologists. Professional well-being is a broad multifaceted topic which poorly fits into current measurement tools. Scientifically, the concept of subjective well-being encompasses emotional response, domain satisfactions and global judgement of life satisfaction10. Hence, future research should look into producing validated, reliable and reproducible measurement tools relating to anaesthesiologists’ professional well-being. Emphasis should be placed in these categories of subjective well-being while being relevant to the anaesthesiologists’ occupational conditions.
INDIVIDUAL INITIATIVES: BE IN CHARGE OF YOUR STRESS
No person can control the stressors in their life. However, being in charge of one’s own stress response is a conscious choice and effort. Taking control over one’s stress response is an important way to ensure success in improving one’s well-being. There is no validated or singularly agreed method to de-stress. There are a variety of techniques to help and improve those who feel overwhelmed. Below are some practical suggestions applying coping techniques (Figure 5)11-12.


Figure 5: Techniques to manage negative responses to stress
ORGANISATION INITIATIVES: DUTIES & OBLIGATIONS
Medical Academies, Anaesthesiology Associations and hospitals have an executive duty to promote awareness and to lower the incidence of occupational stress. This includes adaptability and being aware of the importance of fulfilment in work-related activities, including medical education programmes. The ultimate goal is to ensure not only patients’ but physicians’ safety as well. The main issues that need to be addressed are included in Figure 67.
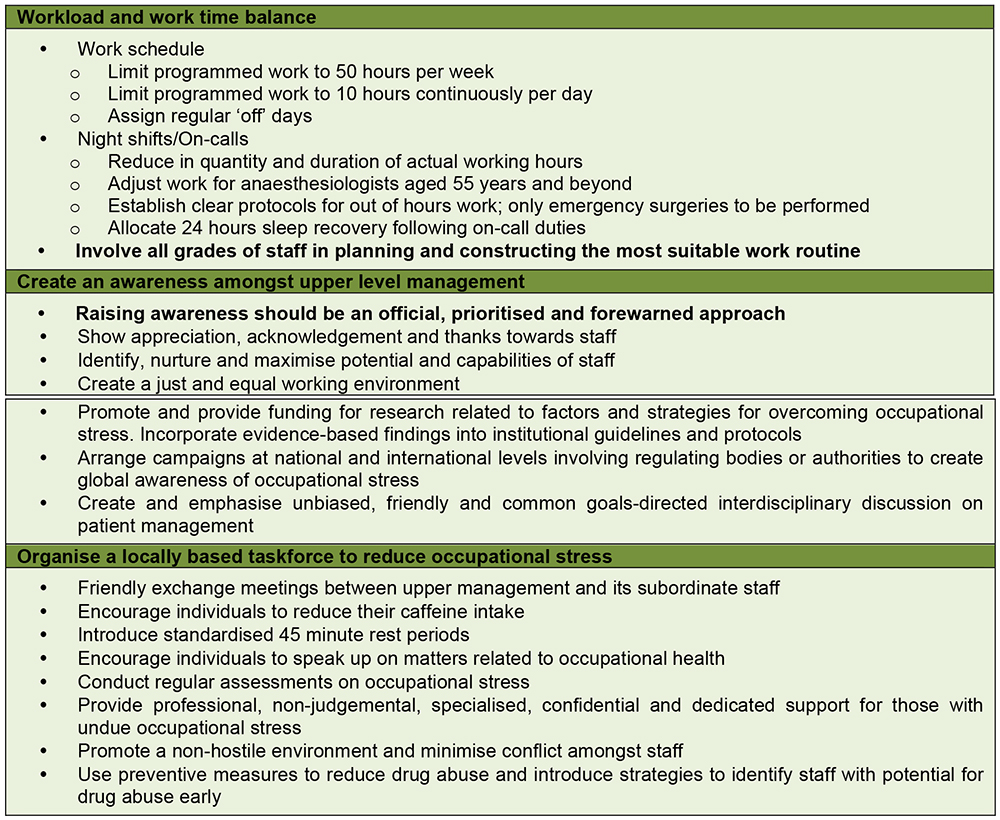
Figure 6: Organisational responsibilities to provide a healthy work environment for professional well-being
SUMMARY
Occupational related stress is inherent in all professions. The first step is to recognise that anybody, including senior ranking anaesthesiologists, may be subjected to profound stress. Addressing the issues related to professional wellbeing head-on brings awareness and empowers compassion towards ourselves and others. Most risk factors for burnout are modifiable. By acknowledging these risk factors, the individual and the institution can optimise their levels of stress and avoid undue fatigue. Cultivating adaptive coping techniques is an indispensable skill. This learned behaviour is the key to protect one’s sanity. Ultimately, the content and happy anaesthesiologist will be more productive than the grumpy one.
ANSWERS TO QUESTIONS
- Regarding stress in the field of anaesthesia:
a. False: Stress can be a motivation if interpreted positively.
b. False: Stress is inherent in all occupations to maintain work commitment and responsibility.
c. False: Mental, emotional and physical protective bodily responses occur during stress.
d. False: Occupational related stress level is reported by 18% of individuals, studies have shown higher levels at 28% in the medical profession, and reaching as high as 50-96% amongst anaesthesiologists.
e. True: Lack of the title of specialist contributes to occupational stress as it is associated with powerlessness over professional decisions. - The following statements are correct with regards to coping skills:
a. True: Emotion-focused coping is useful when the perceived threat is beyond the individual’s control such as sudden death, which is irreversible.
b. False: Emotion-focused coping can reduce unfavourable emotions such as anxiety, fear and frustration.
c. False: Confrontation is a form of maladaptive coping which can transiently reduce undesirable symptoms but maintains the vicious cycle of negative behavioural responses.
d. True: Physicians’ poor mental health has direct negative implications on patients’ care and well-being.
e. True: Poorly coping individuals are exposed to adverse complications such as reduced immunity, hormonal imbalance, cardiovascular diseases and mental disorders. - Concerning methods to reduce occupational related stress:
a. False: Regular optimistic thinking instead of only occasional is a good strategy to de-stress.
b. False: Writing down a stress journal to keep a mental account only serves to reinforce the stress response. The objective of keeping a stress dairy is to help individuals identify stress triggers in order to cultivate positive response to stress.
c. True: Slowing down and stepping back allow control over emotions and actions.
d. False: Adequate rest and relaxation are necessary for recharging and to recover from fatigue.
e. True: Medical regulators and institutions have the executive power to regulate service and academic workload to safeguard professional well-being.
REFERENCES AND FURTHER READING
- Canadian Anesthesiologists’ Society. The Healthy Anesthesiologist. http://www.cas.ca/English/Healthy- Anesthesiologist (accessed on 10/10/2016).
- Bertolote JM. The roots of the concept of mental health. World Psychiatry 2008; 7(2): 113-116.
- World Health Organization. Mental health: a state of well-being. http://www.who.int/features/factfiles/mental_health/en/ (accessed on 12/10/2016).
- Chipas A, Cordrey D, Floyd D et al. Stress: perceptions, manifestations, and coping mechanisms of student registered nurse anesthetists. AANA J 2012; 80(4): S49-55.
- Lyons SM, Atkinson RE, Aitkenhead AR et al. Stress in anaesthetists.1st edn. London, United Kingdom. The Association of Anaesthetists of Great Britain and Ireland. 1997.
- European Society of Anaesthesiology. The risks of being an anaesthesiologist. http://www.esahq.org/Day2_02 (accessed on 12/10/2016)
- Neto GFD, Torchiaro GC, Sig-Tu FV et al. Occupational well-being in anesthesiologists. 1st edn. Rio de Janeiro, Brazil. Brazilian Society of Anesthesiology. 2014.
- Khetarpal R, Chatrath V, Kaur J et al. Occupational stress in anesthesiologists and coping strategies: a review. Int J Sci Stud 2015; 3(6): 188-192.
- Folkman S, Lazarus R, Dunkel-Schetter C et al. The dynamics of a stressful encounter: cognitive appraisal, coping and encounter outcomes. J Pers Soc Psychol 1986; 50(5): 992-1003.
- Diener E, Suh EM, Lucas RE et al. Subjective well-being: three decades of progress. Psychol Bull 1999; 125(2): 276-302.
- Nedd K. Power over stress. 35 quick prescriptions for mastering the stress in your life. 1st edn. Toronto, Canada. QP Press. 2003.
- Raber MF, Dyck G, Preheim B. Stress management: strategies for emotional fitness. 3rd edn. Boston, Massachusetts. Course Technology, Thomson Learning. 2005.



