Paediatric Anaesthesia
QUESTIONS
Before reading the tutorial, try to answer the following questions. The answers can be found at the end of the tutorial.
Which of the following statements are true?
- The retropharyngeal space extends from the base of the skull to the level of the hyoid bone.
- The retropharyngeal space contains the major vessels of the neck.
- Retropharyngeal abscess usually affects children older than 10 years.
- Retropharyngeal abscess can arise secondary to a dental infection.
- Patients with retropharyngeal abscess almost always present with a bulging of the posterior pharyngeal wall.
- Exaggerated cervical lordosis (inward curvature) on a lateral neck radiograph is highly suggestive of a retropharyngeal abscess.
- Premedication is advisable prior to surgery.
- IV induction is the preferred method of induction.
- Muscle relaxants are not routinely administered.
- Retropharyngeal abscess has a benign course and is rarely associated with life threatening complications.
RETROPHARYNGEAL ABSCESS CASE HISTORY – presentation
A 2-year-old boy was brought to the emergency room in respiratory distress. He had a one-week history of cough and cold associated with fever and poor intake. On the day of presentation he developed increasingly noisy breathing. On examination, the child was irritable and uncooperative, with a heart rate of 140 and respiratory rate of 25. He was lying with his head extended and mouth open and with noisy breathing. There was a swelling in the posterior pharyngeal wall and a diagnosis of retropharyngeal abscess was made.
INTRODUCTION
Retropharyngeal abscess is a deep neck space infection that can deteriorate lead to life-threatening airway obstruction. It is an infrequent complication of upper respiratory infections (URI) in children but remains relatively common in low-income settings where access to antibiotics is restricted. This tutorial will discuss the anatomy of the neck spaces, epidemiology, pathophysiology, clinical features, diagnosis and treatment of retropharyngeal abscess, and the anaesthetic management of a child with retropharyngeal abscess.
ANATOMY
There are three major fascial layers of the head and neck: superficial, deep and visceral layers (Figs.1).These discrete layers limit the spread of infection, but once infection i s established, potential spaces between these fascial planes serve to direct its spread. (1) Table 1 summarizes the fascial layers of the neck

Table 1: Fascial layers of the neck
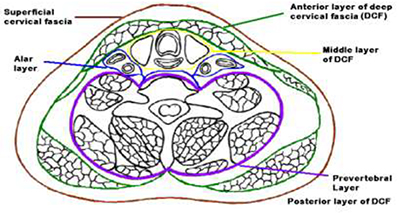
Fig. 1 Axial section of the neck through the level of T1 vertebra showing the superficial and deep cervical fascia
There are three important groups of deep neck spaces where infection may spread. They are described by their relationship to the hyoid bone in the neck:
- Those located above the level of the hyoid (peritonsillar, submandibular, parapharyngeal, masticator/temporal, buccal and parotid spaces)
- Those that involve the entire length of the neck (retropharyngeal, prevertebral, the „danger‟ space, and carotid spaces)
- Those located below the level of the hyoid (pretracheal space).
The retropharyngeal space extends from the base of the skull to the mediastinum. (Fig. 2 and Fig. 3) Laterally, it is bound by the carotid sheaths. The retropharyngeal space is fused down the midline and contains two chains of lymph nodes extending down each side of the space. These nodes typically atrophy after 6 years of age.
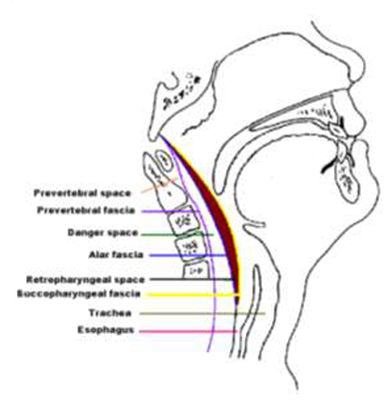
Fig. 2 Lateral view of the deep spaces of the neck
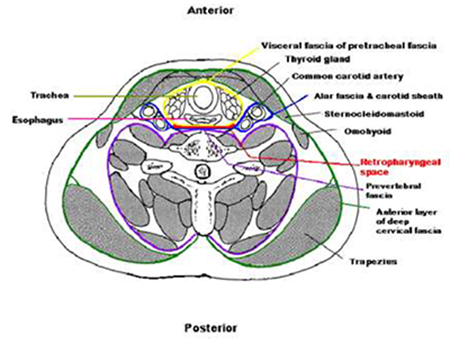
Fig. 3 Cross-sectional view of the deep spaces of the neck
Complications of retropharyngeal abscess are related to compression of adjacent structures, rupture of the abscess, or spread of infection. Complications include:
- Tracheal compression
- Pharyngeal compression
- Aspiration pneumonia
- Mediastinitis, pericarditis, tamponade
- Empyema
- Jugular vein thrombosis, carotid rupture
- Osteomyelitis, vertebral subluxation, spinal cord damage
RETROPHARYNGEAL ABSCESS
Epidemiology
Retropharyngeal abscesses occur mostly in children aged 6 months to 6 years with a peak incidence at 3 years of age. It is slightly more common in boys (2,3).
The widespread use of antibiotics has dramatically reduced the overall incidence of deep neck infections (2). Unusual pathogens such as mycobacterium tuberculosis should always be considered.
Causes
The retropharyngeal space can become infected in two ways, either local spread of infection or secondary to penetrating trauma.
- “Classic” retropharyngeal abscess in children tends to spread from infected lymph nodes following upper respiratory tract infection such as pharyngitis, tonsillitis, sinusitis, cervical lymphadenitis or dental infections.
- Penetrating pharyngeal trauma is relatively common in children (e.g. falling with a sharp object in the mouth). Foreign bodies (e.g. fishbones) have also been implicated. Infection may be iatrogenic (e.g. trauma following laryngoscopy, endotracheal intubation, endoscopy, feeding tube placement and dental injections and procedures).
Offending pathogens depend on the origin of the infection and frequently include multiple aerobic and anaerobic organisms. The most common infections are due to group A ß-haemolytic Streptococcus, anaerobic organisms and Staph. Aureus.
Clinical features
The clinical presentation of retropharyngeal abscess may be nonspecific or may be related to airway or pharyngeal problems
- Symptoms of an upper respiratory tract infection, fever, irritability, decreased oral intake
- Drooling, difficulty in swallowing, pain on swallowing, trismus,
- Neck swelling and stiffness or refusal to move the neck (particularly hyperextension).
- Older children may complain of sore throat and neck pain.
- Muffled “hot potato” voice, stridor
- Respiratory distress.
Physical examination may reveal bulging of the posterior pharyngeal wall, although this is present in <50% of infants with retropharyngeal abscess. Palpation should be avoided as it might lead to rupture and spillage of the contents into the upper airway. Cervical lymphadenopathy (usually unilateral) may also be present. The neck stiffness and limitation of the neck movement may be misinterpreted as nuchal rigidity and lead to a misdiagnosis of meningitis. As the purulent material collects, a fluctuant mass may compress the pharynx or trachea. Children with severe infections may position themselves to maintain a patent airway for instance by mouth breathing, tongue protrusion or mandibular protrusion.
The clinical presentation can be insidious; maintain a high index of suspicion especially in patients with upper respiratory illnesses that do not appear to be resolving over a normal time course or with conventional therapy.
Differential diagnosis includes:
- Acute epiglottitis
- Foreign body aspiration
- Pharyngitis
- Cervical adenitis
- Meningitis.
Diagnosis
- Assess the degree of respiratory distress. If significant compromise is present, the airway must be secured as a priority. If the child is anxious, diagnostic investigations can be withheld as increased anxiety may worsen the respiratory distress and even lead to complete obstruction of the already tenuous airway. A child with significant airway compromise should be accompanied at all times by a specialist able to safely secure the airway should the child develop complete obstruction. If the child has only a mild degree of respiratory distress, further investigation may proceed safely.
- Routine laboratory tests often yield nonspecific results (e.g. leukocytosis) and are not useful in the diagnosis of retropharyngeal abscess. Blood cultures should be taken to guide appropriate antibiotic therapy.
- A lateral neck radiograph is the first line investigation in the stable child. The study should ideally be performed during inspiration with the neck held in a normal position. In general, the anteroposterior diameter of the retropharyngeal space should not exceed that of the adjacent vertebral body (Fig. 4). Widening of the retropharyngeal space suggests a mass effect. However, the space may be falsely enlarged during neck flexion or crying. The radiograph can also show an air or fluid level in the mass, suggesting an anaerobic infection. In addition, the cervical spine may also be straightened with loss of the normal lordosis (so-called „Ram Rod‟ spine). Patients presenting with chest pain should also have a chest radiograph in the PA view. A widened mediastinum may indicate mediastinal involvement.
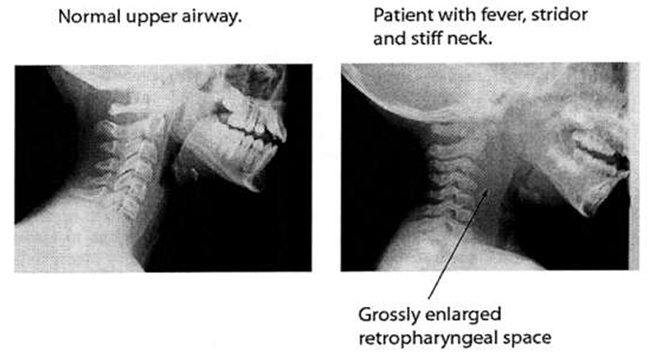
Fig. 4 Comparison of lateral neck radiograph showing a normal Xray on the left and one with retropharyngeal abscess on the right. (Reprinted from Emerg Med Clin N Am Vol. 28 Issue 1, James D’ Agostino, Pediatric Airway Nightmares, 119 – 126, 2010, with permission from Elsevier.)
- CT scan with IV contrast medium is currently the imaging modality of choice. It reveals a hypodense lesion, ‘ing enhancement’ or ‘scalloping’ of the walls of a lymph node. It is also helpful in demarcating the lesion and determining if vascular involvement is present.
- MRI provides better soft tissue definition than a CT scan but it is usually unnecessary and rarely used, unless there is a concern for potential CNS spread. In addition, this diagnostic imaging takes longer and usually requires sedation/anaesthesia with the attendant airway implications.
- Ultrasonography has been advocated by some authors as an alternative to CT for evaluating retropharyngeal abscess as well as monitoring its progression. It is portable, less traumatic to the child and rarely requires the use of sedation. This modality, especially when combined with color Doppler, can diagnose infections in the early non-suppurative stage. However, for surgical planning, it provides limited additional assistance.
MEDICAL/SURGICAL MANAGEMENT
A child with retropharyngeal abscess requires continuous close monitoring and urgent medical +/- surgical intervention.
The management priorities are:
- Maintain the airway
- Insert a reliable IV catheter
- Keep the child nil by mouth
- Constant, close observation to detect incipient airway compromise, possibly heralded by increased pain.
- IV antibiotic therapy should be given while awaiting culture and sensitivity results. Clindamycin is the first-line antibiotic. This is given in combination with a ß-lactamase inhibitor (such as clavulanic acid) or cefoxitin, cefuroxime, imipenem for ß-lactamase- resistant organisms. Vancomycin should be considered for patients who have profound neutropenia or immune dysfunction. IV antibiotic therapy should be continued until the patient has been improving clinically/afebrile for at least 48 hrs, followed by oral therapy using amoxicillin with clavulanic acid, clindamycin, ciprofloxacin, trimethoprim- sulfamethoxazole or metronidazole.
- Surgical incision and drainage. Indications include progressive airway obstruction and failure to improve within 24 to 36 hours of antibiotic therapy. This can be done either through an intraoral incision or through an external cervical approach.
Intraoral aspiration and drainage is recommended under general anaesthesia if the abscess is limited to the upper retropharyngeal space (4). The initial localization of the abscess should be performed with needle aspiration to rule out the presence of blood and to confirm the presence of purulent material which should be sent for culture and sensitivity. A vertical incision is made through the oedematous mucosa of the posterior pharyngeal wall. Blunt dissection is then continued into the cavity to drain it completely. If blood is encountered during localization, the external approach should be used for vascular control.
External drainage is used when the abscess extends inferiorly to the hyoid bone. The incision is made in a modified apron-like fashion with a horizontal limb at the mid-portion of the abscess cavity (judged on a lateral x-ray and CT scan) and the vertical portion is carried along the anterior border of the sternocleidomastoid muscle superiorly. If there is inferior extension, the neck incision can be continued to the clavicle. The anterior border of the SCM muscle is readily identified and lateralized. The carotid sheath is identified and medialized. Following the prevertebral fascia with medial retraction of the larynx, trachea and thyroid, the abscess cavity is opened and drained. Irrigation drains are inserted and removed after 24 – 48 hrs. Transthoracic drainage is necessary when the infection spreads below the carina.
Complications
These include airway compromise secondary to mass effect, rupture of the abscess with inhalation of contents leading to aspiration pneumonia (or rarely asphyxiation), spread of infection to adjacent structures in the neck (including carotid sheath), osteomyelitis of the cervical spine and mediastinal infection. Necrotizing fasciitis is also a potential serious (and rare) complication.
ANAESTHETIC MANAGEMENT OF A CHILD WITH RETROPHARYNGEALABSCESS
The primary anaesthetic concerns are anticipated difficult airway secondary to airway distortion by the retropharyngeal abscess and possible rupture and aspiration of abscess contents. It is imperative to have all equipment necessary for difficult airway management checked and ready (including that for tracheostomy). The ENT surgeon and operating room personnel should also be present and ready to perform an emergency surgical airway if needed.
Preoperative
Preoperative assessment should primarily focus on determining the severity of any airway compromise. Is fluid resuscitation underway, and if so, is it adequate? If the patient is dehydrated, isotonic fluids should be administered. Premedication should not be used, especially if airway compromise is evident as this could rapidly lead to partial or complete airway obstruction. Reduction of fever (e.g. with acetaminophen) should also be considered prior to surgery.
Intraoperative
Standard monitoring (minimum NIBP, ECG, pulse oximetry, ETCO2) should be employed. Intravenous access should ideally be available/functional. The patient may be placed head down on a tipping bed to prevent possible aspiration of abscess contents.
The preferred technique is gaseous induction of anaesthesia, maintaining spontaneous respiration. Remember that the patient may not have any symptoms of airway obstruction in the awake state but this can manifest under anaesthesia with relaxation of the pharyngeal muscles (5). After preoxygenation, gaseous anaesthesia is induced with incremental halothane or sevoflurane in 100% oxygen. An anti-sialogogue e.g. glycopyrrolate (10 mcg/kg) or atropine (20 mcg/kg) may be administered intravenously. The patient should be allowed to breathe spontaneously until a sufficient depth of anaesthesia is reached to permit airway instrumentation. No muscle relaxants are given as this might cause complete airway obstruction. Rapid, gentle and atraumatic intubation is necessary in such cases to prevent abscess rupture, aspiration and acute airway obstruction. Once the ETT has been secured, a throat pack may be inserted to prevent aspiration of blood/pus particularly if an uncuffed ETT is used. If available, a cuffed ETT is preferred over uncuffed in an effort to protect the airway from such contamination.
If during the conduct of inhalation induction, the patient develops airway obstruction unresponsive to airway opening maneuvers, the options are emergency tracheostomy or a transtracheal cannulation (see case history below).
Anaesthesia should be maintained with volatile anesthetic plus judicious incremental doses of opioid for analgesia. Muscle relaxants are perhaps best avoided because of the potential for airway obstruction even once intubated (6). Patients with significant haemodynamic compromise due to sepsis may require vasopressors.
Extubation plans are based on the severity of the patient‟s preoperative condition i.e degree of airway obstruction/ contamination/manipulation/oedema as well as the availability of postoperative ventilation. The child should be fully awake if extubation is planned at the end of the procedure.
Postoperative
These patients should be closely monitored in the critical care unit for 24 – 48 hours post-extubation. During this time close attention should be paid to ongoing oxygen, fluid and analgesia requirements. Appropriate antibiotic coverage should be continued for 5 – 7 days or as guided by microbiologists.
RETROPHARYNGEAL ABSCESS CASE HISTORY – continued
The operating theatre was prepared, and a range of sizes of tracheal tubes was prepared. The ENT surgeons were standing by. The child was monitored with an ECG and pulse oximetry. Intravenous access was obtained. Inhalational anaesthesia was induced with halothane in oxygen but as the child was drifting off to sleep, he developed complete airway obstruction. Airway manoeuvres (jaw thrust) failed to regain the airway, and it was not possible to ventilate the child. It was not possible to view the cords by direct laryngoscopy, and the child began to desaturate.
A 16G cannula was used to access the trachea, placing the cannula between the tracheal rings. The cannula was attached to a connector from a size 2.5 tracheal tube and the child was ventilated with 100% oxygen. The oxygen saturation reached 100% within a few minutes and halothane administration was resumed.
The child was placed in the Trendelenberg position and under direct laryngoscopy with suction available, the ENT surgeon made a longitudinal incision to drain the abscess. After draining the abscess, the pharyngeal mass disappeared, and the child was easily intubated. The tracheal cannula was removed after intubation. The child was extubated awake and transferred back to the emergency ward where he received antibiotics and was discharged in perfect condition after three days.
Dr Emmanuel Munyarugero
Consultant Anaesthetist
Mbarara University Hospital, Uganda
ANSWERS TO QUESTIONS
- The retropharyngeal space extends from the base of the skull to the level of the hyoid bone. False
- Just like the ‘danger’ and prevertebral space, the retropharyngeal space is a deep neck space that involves the entire length of the neck extending from the base of the skull up to the level of the mediastinum.
- The retropharyngeal space contains the major vessels of the neck. False
- The retropharyngeal space contains connective tissue and lymph nodes draining the adjacent structures.
- Retropharyngeal abscess usually affects children older than 10 years. False
- The lymph nodes present within the retropharyngeal space commonly involute after 6 years of age explaining the decline of retropharyngeal abscess after 6 years of age. Retropharyngeal abscess commonly affects children 6 months to 6 years of age.
- Retropharyngeal abscess can arise secondary to a dental infection True
- The retropharyngeal space can be infected either as an extension of an ongoing upper respiratory or dental infection or as a result of direct penetrating trauma.
- Patients with retropharyngeal abscess almost always present with a bulging of the posterior pharyngeal wall. False
- Although the presence of a bulging of the posterior pharyngeal wall clinches the diagnosis of a retropharyngeal abscess, it is present in < 50% of affected patients.
- Exaggerated cervical lordosis (inward curvature) on a lateral neck radiograph is highly suggestive of a retropharyngeal abscess. False
- Aside from widening of the retropharyngeal space, loss of the cervical lordosis („Ram Rod‟ spine) is suggestive of a retropharyngeal abscess.
- Premedication is advisable prior to surgery. False
- Maintaining a patent airway is of utmost importance in these patients so it is best not to give any premedication.
- IV induction is the preferred method of induction. False
- Maintaining a patent airway is of utmost importance in these patients so you want to be able to put the patient to sleep without losing spontaneous respiration. Careful gas induction technique is the preferred method.
- Muscle relaxants are not routinely administered. True
- Preventing airway obstruction is a priority in these patients so muscle relaxants are not routinely administered. Airway obstruction has been reported in an infant that was already intubated necessitating emergency tracheostomy to preserve the airway. Thus, it is best to shy away from muscle relaxants in these patients even after intubation.
- Retropharyngeal abscess has a benign course and is rarely associated with life threatening complications. False
- Retropharyngeal abscess is a life-threatening airway illness. All patients must be closely monitored. Complications can arise from compression of adjacent structures, rupture of the abscess and spread of the infection to nearby deep neck spaces.
REFERENCES and FURTHER READING
- Cotton, Robin T, Myer III Charles M. Practical Pediatric Otolaryngology. Lippincott-Raven Publishers, Philadelphia, 1999.
- Acevedo JL, Shah RK. Retropharyngeal Abscess. Available at http://emedicine.medscape.com/article/995851-overview
- Balasubramanian T. Retropharyngeal Abscess. Available at http://www.drtbalu.co.in/ret_abs.html
- Bluestone CD, Rosenfeld RM. Surgical Atlas of Pediatric Otolaryngology. BC Decker Inc., Hamilton, London, 2002.
- Singh R, Gupta R, Jain A, Vajifdar. Anesthesia Management of Paediatric Retropharyngeal Abscess – Our Experience. J Anaesth Clin Pharmacol, 2008, 24 (1): 57 – 60. Available at http://joacp.org/index.php?option=com_journal&task=check_subscription&id=669
- Balhara S, Malik Premila, Malhotra N, Chhabra B. Retropharyngeal Abscess in an Infant – An Anaesthetic Challenge. . J Anaesth Clin Pharmacol, 2003, 19 (1): 95 – 97. Available at http://www.joacp.org/index.php?option=com_journal&task=check_subscription&id=342



