Intensive Care Medicine
QUESTIONS
Before continuing, try to answer the following true or false questions. The answers can be found at the end of the article, together with a brief explanation.
- Regarding the nature of maternal deaths in the UK:
a. The Confidential Enquiry into Maternal Deaths published in March 2011 highlights the decrease in the overall mortality rate of pregnant women from 13.9 (in 2003-2005) to 11.39 (in 2006-2008)
b. The above report found evidence of suboptimal care that could have contributed to the death of parturients
c. Thromboembolism is the most common direct cause of maternal death in the UK
d. Causes of maternal death in the UK are similar to those in the rest of the world - Which of the following situations demand level 2 care:
a. An obstetric patient receiving a remifentanil infusion for analgesia
b. A woman receiving a labetolol infusion for BP control in pre-eclampsia
c. An obstetric patient in which an arterial line is in use for BP monitoring and blood sampling
d. Oxygen support via facemask to maintain oxygen saturation - The 2000 UK Department of Health document “Comprehensive Critical Care” recommends the following:
a. The term “Critical Care” should replace the terms “High Dependency” and “Intensive Care”
b. Critical care required by a parturient should only be provided on the labour suite
c. The four levels of care depend on the diagnosis of the patient
d. The document included guidance for the care of the critically unwell parturient in the delivery suite
Most women experience few significant complications during pregnancy, delivery and the postpartum period. The few who become critically ill during this time should receive the same standard of critical care as non-pregnant patients. Recent Confidential Enquiries into maternal mortality highlight a number of deaths in which prior care was considered suboptimal1. There is a growing need to address the area of maternal critical care with respect to the best ways of delivering care to this vulnerable patient group.
CONFIDENTIAL ENQUIRIES INTO MATERNAL DEATHS 1
The Confidential Enquiry into Maternal Deaths is the longest-running audit in the world and has been published every three years for the past 60 years. The most recent review published in 2011 for the 2006-08 triennia highlights the decline in the overall mortality rate of pregnant women from 13.95 per 100,000 maternities in 2003-05 to 11.39 in 2006-08 (Table 1).1 The fall in mortality is mainly due to a decrease in the number of deaths from direct causes – conditions resulting from the pregnancy (e.g. thromboembolic disease, haemorrhage, amniotic fluid embolism). Mortality due to indirect causes (medical or mental conditions worsened by pregnancy) has either increased or remain unchanged. The report highlighted that some women died despite receiving excellent care. However, there was evidence that suboptimal care contributed to the deaths of a significant number of women. Examples of suboptimal care included delays in recognition of critical illness and involvement of intensive care teams.
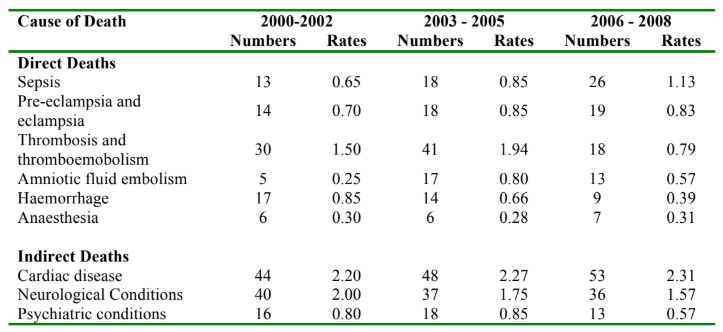
Table 1. Adapted from: Centre for Maternal and child Enquiries (CMACE). Saving Mothers’ Lives: reviewing maternal deaths to make motherhood safer: 2006-08. The Eighth Report of the Confidential Enquiries into Maternal Deaths in the United Kingdom BJOG 2011;118;1-203. Rates shown are per 100,000 Maternities
More than 1 in 10 women aged 16-50 admitted to UK Intensive Care Units (ICU) are obstetric patients. In addition, there are likely to be significant numbers of critically ill parturients who are cared for within the maternity unit.
A multidisciplinary Maternal Critical Care Working Group, commissioned by the Joint Standing Committee of the Royal College of Anaesthetists with representation from the Intensive Care Society, the Obstetric Anaesthetists’ Association, the Royal College of Obstetricians and Gynaecologists, The Royal College of Midwives and other UK organisations, published guidance on provision of maternal critical care; ‘Providing equity of critical and maternity care for the critically ill pregnant or recently pregnant woman’.2 This document defines standards and makes recommendations to help guide maternity and critical care providers in establishing and managing a maternal critical care service.
WHAT IS MATERNAL CRITICAL CARE?
Maternal critical care, rather than obstetric critical care, describes patient-centred multidisciplinary care rather than specialty-focused care.3 The 2000 UK Department of Health document ‘Comprehensive Critical Care’ recommends the terms ‘High Dependency’ and ‘Intensive Care’ should be replaced by the term ‘Critical Care’.4 The document also proposes that the care required by an individual should be independent of location – the concept of ‘critical care without walls’. Care is subdivided into four levels, depending on the organ support and level of monitoring required independent of diagnosis. The level of care required by pregnant or recently pregnant woman can also be classified according to the Intensive Care Society’s ‘Level of Care’ document.5 Examples of levels of care provided within a maternity unit include:
Level 0 or normal ward care
- Care of the low risk woman
Level 1 or additional monitoring or step down from higher level of care
- Neuraxial analgesia
- Risk of haemorrhage
- Oxytocin infusion
- Remifentanil infusion
- Mild pre-eclampsia on oral antihypertensives/fluid restriction
- Chronic medical condition at risk of deterioration e.g. diabetes mellitus requiring IV insulin
Level 2 or single organ support
Basic cardiovascular support (BCVS)
- Infusion of antihypertensives (e.g. labetalol or hydralazine) to control BP in pre- eclampsia
- Arterial line used for BP monitoring and blood sampling
- Central venous catheter for central venous pressure monitoring or vascular access
Basic respiratory support (BRS)
- Oxygen support via facemask to maintain oxygen saturation
- Non-invasive ventilation (CPAP, BiPAP etc)
Advanced cardiovascular support (ACVS)
- Simultaneous use of at least two intravenous antihypertensive or vasoactive drugs
Neurological support
- Use of magnesium infusion to control seizures
Hepatic support
- Severe hepatic failure (e.g. secondary to HELLP syndrome or acute fatty liver of pregnancy)
Level 3 or advanced respiratory support alone or support of two or more organ systems as above
- Advanced respiratory support – Invasive mechanical ventilation
- Support of two or more organ systems- Renal support and BRS; BRS/BCVS and an additional organ supported
WHAT GROUPS OF PREGNANT WOMEN MAY REQUIRE CRITICAL CARE?
Recent UK ICNARC data (Intensive Care National Audit and Research Centre) in 2009 showed that 11.4% of women aged 16-50 years admitted to an adult general Intensive Care Unit (ICU) were either pregnant or recently pregnant.6 There were a total of 513 obstetric patients admitted to ICU, an incidence of 260 admissions per 100,000 maternities. The majority were postpartum, 418 patients (81.5%), and major haemorrhage was the primary diagnosis in 34%. Other postpartum critical care admissions comprised patients with pre-eclampsia (7%), pneumonia (3.6%) and HELLP syndrome (2.4%). Non-obstetric pathology was the main reason for admission in 95 women (18.5%) recorded as ‘currently pregnant’. The single most common diagnosis in this group was pneumonia (20%), followed by asthma (7.4%) and ectopic pregnancy (5.3%). The ICNARC data confirmed that obstetric patients admitted to ICU had a better outcome than matched controls (critical care mortality 2% vs. 11% in control population).
Although ICNARC provides valuable information about pregnancy-related ICU admissions, relatively little is known about the women who receive higher level of care on maternity units. It is estimated that as many as 5% of deliveries require level 2 care.3,7,8
WHERE SHOULD MATERNAL CRITICAL CARE BE PROVIDED?
Delivering high quality critical care or obstetric management outside designated specialty specific areas is challenging. The UK National Service Framework for Children, Young People and Maternity Services recommends consultant-led services with adequate facilities, expertise, capacity and back-up for timely and comprehensive obstetric emergency care, including intra-hospital transfer to critical care. One of the most important recommendations by the Maternal Critical Care Working Group was to ensure that critically ill pregnant or postpartum woman receive an equitable standard of care for both their pregnancy-related and critical care needs. Arrangement models may be developed on the basis of local configuration, size and complexity of maternity and critical care services. These may include:
- Providing critical care in a designated area on, or near the delivery suite by trained midwives, obstetricians and anaesthetists with additional training in critical care.
- Importing critical care skills into the labour ward via critical care outreach.
- Transfer of women to a general critical care unit. Obstetric and midwifery input and competencies will be imported into the critical care environment, and if postpartum, direct contact with their baby should be maintained wherever possible.
The above models can be implemented by maternity and critical care services depending on local pathways to ensure women have access to high quality services irrespective of where they have delivered.
The UK Department of Health recommends all clinical staff caring for critically ill pregnant or recently pregnant women should be trained and competent in recognising and responding to acutely ill patients.9
THE MATERNITY AND GENERAL CRITICAL CARE INTERFACE
The pregnant woman being cared for in a general critical care area requires daily review by a multidisciplinary team including a named obstetric consultant and senior midwife. The multiple care providers must balance the needs of critical care with the needs of the woman with regard to obstetric care.
Important additional points for antenatal critical care include:
- Ensuring adequate lateral maternal tilt to avoid aorto-caval compression
- Thromboprophylaxis in line with local or national guidelines
- Regular mid-stream urine specimens should be taken due to the increased risk of urinary tract infections
- Meticulous fluid balance in cases of severe pre-eclampsia/eclampsia and following massive haemorrhage
- A contingency plan with detail of necessary equipment should delivery be required outside the maternity unit
- Availability of common drugs used in the obstetric population e.g. hydralazine, MgSO4, uterotonics (e.g. oxytocin, ergometrine, prostaglandin F2α)
- Consider antenatal steroids if preterm delivery anticipated
- Daily communication and combined ward rounds with named obstetrician and midwife
- Appropriate plans for fetal monitoring and surveillance
Additional points for postpartum care include:
- No lateral tilt required
- Breastfeeding support
- Thromboprophylaxis measures
- Regular follow-up by the multidisciplinary team and usual postpartum checks including: neonatal checks, anti-D if required, breastfeeding support etc
- Attention to drug safety if breastfeeding
It is vital to appreciate the physiological changes of pregnancy and how they impact on critical illness. Such changes include aorto-caval compression, reduced functional residual capacity, potentially difficult airway and intubation and increased risk of pulmonary aspiration. In the event of a maternal cardiac arrest after 20 weeks gestation, cardio-pulmonary resuscitation should be conducted according to ALS guidelines with uterine displacement and perimortem caesarean section commenced after 4 minutes and delivery within 5 minutes of the cardiac arrest.10
STANDARDS FOR THE RECOGNITION AND CARE OF THE ACUTELY ILL PARTURIENT
All admissions to the maternity unit should have their physiological observations recorded on arrival, together with a clear written plan for monitoring and management. The plan should take into account:
- High or low risk pregnancy
- Reason for admission
- Presence of co-morbidities
- Agreed treatment plan
A physiological track and trigger system should be used to monitor all antepartum and postpartum admissions. The introduction of a national modified early obstetric warning score (MEOWS) chart for use in all pregnant and postpartum women who become unwell may aid the more timely recognition, treatment and referral of women who are becoming critically ill.11 MEOWS charts should be used in all areas of the hospital where pregnant and recently pregnant women may present, including the Emergency Department. Abnormal scores should prompt an appropriate response.
Education, training and assessment should be provided to ensure that staff have competencies appropriate to the level of care they are providing.
A graded response strategy for patients identified as being at risk of clinical deterioration is recommended:
Low-score group (EWS=3)
- Increased frequency of observations
- Midwife in charge alerted
Medium-score group: (EWS=4 or 5)
- Urgent call to personnel with core competences for acute illness, e.g. critical care outreach team, anaesthetist, obstetrician, acute medical or surgical specialties
High-score group: (EWS>6)
- Emergency call to team with critical care and maternity competences. The team should include a practitioner with advanced airway management and resuscitation skills
CHALLENGES TO DEVELOPING A MATERNAL CRITICAL CARE SERVICE
- Increasing workload: Many countries are experiencing an increase in the number of high-risk pregnant women on account of a rising birth rate and changes in obstetric demographics including an increase in maternal age and co-morbidities, morbid obesity and assisted conception. The rise in caesarean section rate in many countries has resulted in an increase in the incidence of abnormal placentation (accreta, increta and percreta) and subsequent postpartum haemorrhage.
- Training: Each hospital should establish guidelines and in-service training to suit their own local arrangements. Implementation of simulation and ‘skills and drills’ training has been shown to improve human factors such as leadership, teamwork and communication. Midwives looking after critically ill women should have additional training in critical care competencies.2
- Staffing: Midwifery courses vary with respect to the amount of associated training in general nursing skills and knowledge. This combined with midwifery recruitment shortages in some areas make provision of adequate numbers of midwifery staff with appropriate critical care training and experience challenging.
- Critical care team: The care of women with complex medical conditions mandates that obstetricians, anaesthetists, neonatologists, critical care specialists and midwives work in effective multidisciplinary teams. Early involvement of a critical care team is at times vital to avoid an adverse outcome and effective lines of communication and inter-disciplinary working are essential.
SUMMARY
Standards of delivering maternal critical care have been defined.2 The cornerstone of management should involve early multidisciplinary teamwork between clinicians and specialties with effective lines of communication. The role of MEOWS and outreach services is invaluable in early recognition and prevention of maternal morbidity and mortality. There is an increasing need to ensure that care providers on maternity units have adequate training and competencies in maternal critical care.
ANSWERS TO MULTIPLE CHOICE QUESTIONS
- TTTF
- FTTT
- These have been classified by the Intensive Care Society’s “ Levels of critical care” document of 2009. 5
- TFFF
- The individual care should be independent of location of the patient
- Care is subdivided into four levels depending on organ support and level of monitoring required. It is independent of diagnosis.
REFERENCES
- Centre for Maternal and Child Enquiries (CMACE). Saving Mothers’ Lives: reviewing maternal deaths to make motherhood safer: 2006-08. The Eighth Report of the Confidential Enquiries into Maternal Deaths in the United Kingdom. Brit J Obstet Gynaec 2011; 118: 1-203
- Providing equity of critical and maternity care for the critically ill pregnant or recently pregnant woman, July 2011 http://www.rcog.org.uk/files/rcogcorp/Prov_Eq_MatandCritCare.pdf Accessed 09 March 2014
- Wheatly S. Maternal critical care: what’s in the name? Int J Obst Anesth 2010; 19: 353-5
- Department of Health. Comprehensive critical care: a review of adult critical care services. 2000 http://webarchive.nationalarchives.gov.uk/+/www.dh.gov.uk/en/publicationsandstatistics/publications/publicationspolicyandguidance/dh_4006585 Accessed October 2014
- Levels of Critical Care for Adult Patients. Standards and Guidelines. Intensive Care Society 2009.
http://www.ics.ac.uk/intensive_care_professional/standards_and_guidelines/levels_of_adult_patients. Accessed 09 March, 2014 - Female admissions (aged 16-50 years) to adult, general critical care units in England Wales and Northern Ireland, reported as ‘currently pregnant’ or ‘recently pregnant’. 1 January 2007 to 31 December 2007. ICNARC 2009.
http://www.oaaanaes.ac.uk//assets/_managed/editor/File/Reports/ICNARC_obs_report_Oct2009.pdf. Accessed 01 March 2014 - Saravanakumar K, Davies L, Lewis M, Cooper GM. High Dependency care in an obstetric setting in the UK. Anaesthesia 2008; 63: 1081-6
- Veeravalli D, Scholefield H, Fitzpatrick C, Stanton R. Admissions to a specialist maternal high dependency unit. Arch Dis Child Fetal Neonatal edition 2009; 94 (Suppl): Fa 27
- Competencies for recognising and responding to acutely ill Patients in hospital. Department of Health, London 2008.
http://www.dh.gov.uk/en/Publicationsandstatistics/Publications/PublicationsPolicyAndGuidance/DH_096989. Accessed 27 February 2014 - Maternal collapse in pregnancy and the puerperium. RCOG, London 2011 http://www.rcog.org.uk/files/rcog-corp/GTG56.PDF. Accessed 27 February 2014
- Singh S, McGlennan AP. Validation of the CEMACH recommended modified early warning system (MEOWS). Int J Obstet Anesth 2010; 19: S11



