Pain
QUESTIONS
- Long term administration of a strong opioid can lead to
(a) Dependence
(b) Tolerance
(c) Immune suppression
(d) Hypoalgesia - Possible anaesthetic and analgesic techniques in patient on long term opioids
(a) Spinal anaesthesia
(b) Epidural anaesthesia
(c) Plexus blockade
(d) Wound infiltration - Suitable adjunctive medication for post-operative analgesia in a patient taking strong opioids include
(a) Clonidine
(b) Tramadol
(c) Gabapentin
(d) Pethidine
It is very common to encounter patients on strong opioid medication. These patients present particularly challenging pain management difficulties in the peri-operative period due to behavioural, psychological and pharmacological consequences of opioid treatment. This article discusses the key concepts in the anaesthetic management of patients taking strong opioids and steps that can be taken to ensure optimum peri-operative care.
Introduction
Strong opioids are a fundamental component of acute and cancer pain management. However, this class of medication is commonly taken illicitly and have become increasingly prescribed in the management of chronic non-malignant pain (CNMP) syndromes despite on-going controversy on their use in this setting. With such widespread use of strong opioids in the community it is therefore very common to encounter patients on long term, high dose, opioid therapy in anaesthetic practice. Awareness of the physiological and pharmacological consequences of chronic opioid usage is necessary to successfully manage this challenging patient group.
How Common is Opioid Use?
Opioids have been used for medicinal purposes since at least 3000 B.C. In modern times however, opioids have been widely used for illicit purposes and specifically for their psychotropic properties. The scale of this problem is highlighted by the fact that despite stringent regulation, one recent report estimates that there are in excess of 2 million patients dependent on opioids in the USA alone. Figure 1 shows the annual increases in opioid use since 1965 in the USA.
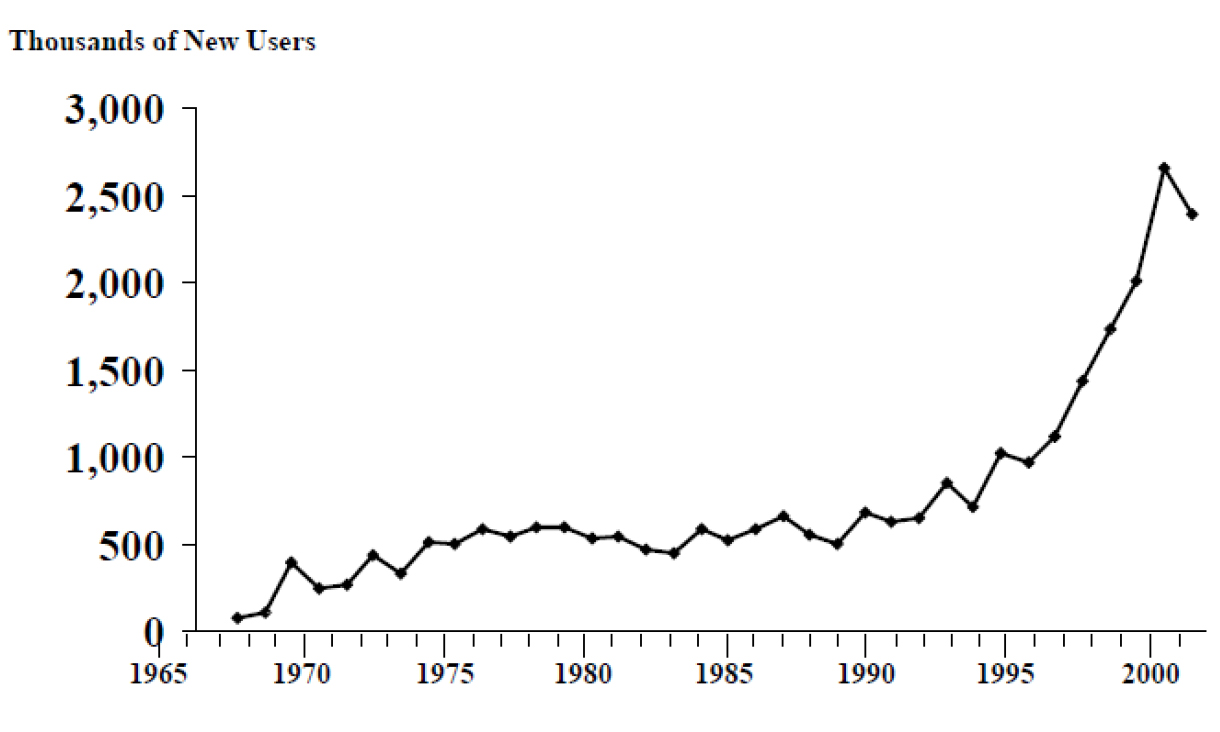
Figure 1. Annual number of new abusers of psychotherapeutics from 1965-‐2002 (Source: National Survey on Drug use and Health (SAMHSA) 2004)
Despite proven efficacy in acute nociceptive pain, the use of opioids for chronic non-malignant pain was not recommended for many years. This was due to a perceived lack of efficacy and concerns over the potential for addiction. However, over time, a small body of research and influential expert opinion gave some acceptance that strong opioids had a role in the management of chronic pain when used in a controlled fashion.
This limited amount of evidence led to a change in attitude and beliefs within the medical profession in many countries and public de-stigmatisation of strong opioids. Consequently the use of opioids in chronic nonmalignant pain increased considerably up to the present day where an estimated 48% of patients with chronic pain are maintained on some form of strong opioid. In routine anaesthetic practice, one survey found that in preoperative elective orthopaedic patients, 67% of patients were maintained on long term opioid treatment while in elective general surgical patients this figure was 25%.
With this in mind, the anaesthetist should be careful to question patients about strong opioid use, whether illicit or licit. Recognising this pre-operatively will help with management of the physiological and pharmacological consequences of opioid use.
Consequences of Strong Opioid Use
The regular administration of strong opioids has a large number of psychological and physiological consequences. The most commonly recognised side-effects of strong opioids include nausea, constipation, sedation and respiratory depression. However, with long term use there are other important sequelae that are important to consider. These are discussed below.
Psychological Consequences
Addiction
Addiction is defined as a primary, chronic neurobiological disorder characterised by particular patterns of behaviour and physiological adaptations. Behavioural alterations include impaired control over use (e.g. unsanctioned dose escalation), compulsive use, continued use despite causing harm and craving. Addiction is a major concern for both patients and medical professionals who are considering prescribing strong opioids. Even when appropriately prescribed to carefully selected patients, one source estimates that between 20-58% of patients will become addicted to medically prescribed strong opioids.
Dependence
Physical dependence is not the same as addiction. Dependenceis a neuro-pharmacological disorder characterised by neuronal adaptation and plasticity. Unlike addiction, this does not necessarily involve a behavioural component (although addiction may co-exist with dependence). Physical dependence is characterised clinically by a drug-class specific withdrawal syndrome. This will occur with a fall in plasma levels or receptor occupancy of the relevant drug. Common reasons for this are abrupt withdrawal, rapid dose tapering or administration of an antagonist. If baseline opioid consumption is not maintained then withdrawal symptoms may begin to manifest.
It is important to consider that while there is a significant overlap between addiction and dependence, not all dependent patients are addicts.
Physiological Consequences
Tolerance
Tolerance is commonly encountered in clinical practice and refers to a diminished analgesic effect from a given dose of opioid. Pharmacologically this represents a rightward shift in the dose-response curve for a particular opioid i.e. a greater dose is required to achieve the same analgesic effect. This is represented in Figure 2 below. With long term use, tolerance develops to the analgesic, sedative, nausea and respiratory effects of opioids but not miosis or bowel dys-motility tend to be resistant.
The degree of tolerance is generally related to the duration of opioid exposure, daily opioid consumption and receptor kinetics. Tolerance is seen to develop more slowly in opioids with a high degree of intrinsic activity (e.g. fentanyl) compared to those with low intrinsic activity such as morphine. As a general rule, patients requiring 1 mg per hour intravenous morphine or 3mg per hour oral morphine for a period of over one month can be considered to have high grade opioid tolerance.
A number of different types of tolerance have been described and may be categorised as learned, pharmacokinetic and pharmacodynamic. Innate tolerance is also recognised and refers to a pre-existing insensitivity to opioids brought about by the presence or absence of a particular gene.
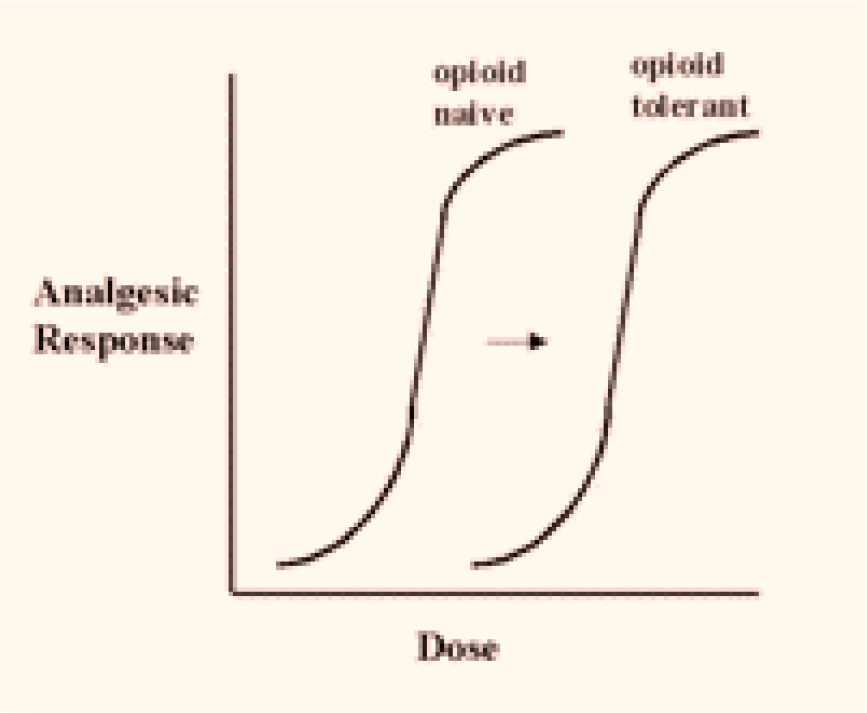
Figure 2. Dose-‐response curve comparing opioid naïve to opioid tolerant subjects
Learned tolerance
This refers to a reduction in the apparent effect of a drug due to adaptive behaviour on the part of the patient. An individual may develop compensatory mechanisms allowing an opioid abusing individual to behave normally despite being intoxicated. In such individuals this can be used to the end of attaining more medication.
Pharmacokinetic tolerance
This mechanism of tolerance may result from altered distribution and metabolism of the drug, typically as a result of enzymatic induction or inhibition. Biotransformation of opioids occurs in the liver and involves two processes: Phase 1 metabolism involves the oxidation or reduction of a drug and is commonly catalysed by the cytochrome P450 system; Phase 2 metabolism involves the conjugation of a drug to a metabolic substrate to create a hydrophilic molecule suitable for renal excretion.
The cytochrome P450 system is readily inducible by a variety of drugs including opioids, barbiturates and antiepileptics. Long term exposure to these agents may lead to more rapid metabolism and increased tolerance. Genetic variability exists within the cytochrome P450 gene such that some individuals may display enhanced or inhibited metabolism of opioids and hence display altered tolerance.
Pharmacodynamic tolerance
Pharmacodynamic changes occur after long-term exposure to a drug and are seen to occur at two distinct levels. The first of these is desensitisation of the opioid receptor. This is brought about by a fall in the absolute number of opioid receptors mediated by a number of mechanisms including active endocytosis of receptors from the cell surface.
A second mechanism postulated in opioid tolerance is the effect on the NMDA receptor. Chronic opioid exposure leads to a down-regulation of glutaminergic transport mechanisms and an indirect activation of the NMDA receptor. This can lead to calcium influx, activation of protein kinase C and production of nitric oxide that contributes to opioid tolerance and abnormal pain sensitivity.
Opioid Induced Hyperalgesia
It has become increasingly recognised within recent years that chronic opioid administration can lead to a paradoxical effect whereby a patient displays increased sensitivity to painful and non-painful stimuli. This is thought to arise because of complicated neurochemical changes in the central nervous system brought about by expression of pro-nociceptive neuropeptides. These neuropeptides arise in a physiological attempt to restore equilibrium in response to increased anti-nociceptive activation from exogenous opioid administration.
This condition is typically seen after rapid dose escalation of opioids and is characterised by widespread, generalised pain and sensitivity. Counter-intuitively, in this circumstance, a reduction in opioid dose will be required.
Other Effects
The long-term administration of opioids has been shown to have effects on immune function, by inhibiting Tcell and macrophage activity, and can result in adrenocortical suppression. The exact clinical significance of these findings is not clear. Interestingly, some recent studies on patients undergoing cervical discectomy and knee arthroplasty reported poorer subjective and objective outcomes from surgery in patients taking regular strong opioids pre-operatively compared to opioid naïve subjects.
Peri-operative Management
Pre-operative assessment
Patients on long-term opioids frequently present to theatre with a complex background of psychological, physiological and pharmacological circumstances. Pre-existing anxiety in this patient group is commonplace and fear of further injury and pain is often apparent. A common observation is that patients maintained on long term opioids have far higher pain scores and opioid consumption post-operatively than would be expected from simply replacing a pre-operative opioid dose. This is particularly apparent in patients on strong opioids for CNMP where severity of post-operative pain correlates closely with severity of pre-operative pain.
The pre-operative visit is therefore essential in identifying relevant risk factors for pain, allowing the organisation of services and an appropriate management plan to be formulated. Patient education is an essential step in this process to provide re-assurance, establish rapport and clarify any misconceptions the patient may have regarding the role of the Anaesthetist in peri-operative pain management. Key points to remember in the peri-operative management of patients on long term opioids are detailed below.
Key Factors in Pre-operative Assessment of patient on strong opioids
- Educate the patient on what to expect and proposed management plan
- Expect dependence and opioid tolerance if requiring >30mg intravenous morphine equivalent per day for over 1 month
- Continue regular opioids and give normal dose on morning of surgery
- Continue all adjuvant analgesics e.g tricyclic antidepressants and anticonvulsants
- Choose regional or general techniques on an individual basis
- Remember that under-medicating patients may provoke withdrawal
- Uncontrolled fear and anxiety lead to over-reporting of painful stimuli
- Expect that post-operative opioid requirements can be increased by up to 400% over baseline
- Prolonged post-operative analgesia requirements are common
Intra and Post-operative management
It is essential that chronic opioid medication is maintained throughout the peri-operative period. This is equally applicable regardless of the anaesthetic technique used. In moderate to major surgery where administration of opioids by the patients’ usual oral route is not possible, a suitable alternative should be utilised and the dosage adjusted accordingly for an intravenous, transdermal or epidural route. Published dose equivalency tables should be referred to when converting opioid doses.
Pain assessment is fundamental to successful peri-operative management in all patient groups but particularly in those taking strong opioids. This is not only to assess pain but also to monitor for signs of opioid withdrawal. While patients self-reporting of pain scales are important, objective measurements such as ability to cough, deep breathe and comply with physiotherapy are extremely useful assessments both to the patient and the medical team to gauge progress and response to treatment.
It must be appreciated that no one strategy or anaesthetic technique is applicable to all patients. As such, an individualised approach to the peri-operative period is necessary depending on a multitude of patient factors. Some of the key considerations are given below.
Regional Anaesthesia
There is general consensus that wherever possible, a regional anaesthetic technique should be considered for patients on long term opioids. This not only includes central neuraxial blockade but also peripheral nerve catheters, plexus blockade or even tissue infiltration. These techniques will enable a reduction in opioid requirements and improve tissue perfusion.
Opioid receptors within the central nervous system are subject to down-regulation with spinal and epidural opioid dose requirements being increased proportionately. Interestingly, despite patients experiencing satisfactory pain relief from intra-thecal opioids, supra-spinal binding and plasma concentration of opioid may decline to the point that withdrawal symptoms may still develop. For this reason, it is important that even with epidural administration of opioids, baseline levels of opioid should still be maintained either by the oral or parenteral route.
PAC code –
Patient Controlled analgesia
The use of patient controlled analgesia (PCA) was often held as controversial in patients on chronic opioid therapy.
However, the use of a PCA in such circumstances is generally safe and provides a means of ensuring tailored dosing above a stable background level of opioid.
Background opioid should be provided by the most suitable method for the individual patient. This may be the usual preparation if oral intake is uninterrupted by surgery, but in some cases an intravenous background infusion will be required. In addition to this a larger bolus dose than that used in a standard PCA protocol may be needed. The exact doses required are subject to variation and should be adjusted to effect on an individual basis.
As well as the pharmacokinetic advantages of a PCA, this mode of administration offers the patient reassurance that opioid levels will be maintained and a degree of autonomy in their pain management. It is important that regular observations are carried out as well as pain scoring to assess progress. These patients require frequent expert assessment.
Additional strategies
Maintaining baseline opioid requirements is vital in successful peri-operative management in patients on long term opioids, however, it is important to consider additional therapeutic options. Acute nociceptive pain has multiple mechanisms and adding in another form of analgesic can provide additional benefit. Multimodal analgesia provides better pain relief than reliance on a sole agent. Some further options are outlined as follows:
Opioid rotation
Post-operatively, when confronted with a patient on long term strong opioid therapy with rapidly escalating doses of opioids with no appreciable improvement in pain control, it is often worthwhile considering a switch to an alternative strong opioid. The rationale being that there is considerable inter-individual variability between different opioids which exhibit slightly different degrees of receptor occupancy. Approximately 50% of patients derive an improvement in analgesia by rotation to another strong opioid. It is important to consult conversion tables for guidance on an appropriate equivalent dose of a new drug and is generally safer to start off at 75-80% of that recommended dose.
Ketamine
Ketamine is an antagonist at the NMDA receptor. Ketamine has many theoretical benefits in peri-operative pain management including a reversal of opioid tolerance and decreasing hypersensitivity surrounding a surgical wound. Ketamine may be given in a variety of ways but most commonly is given as a continuous infusion starting in the immediate pre-operative period and continued for 24-48 hours post-operatively. Typical dose range for infusion is from 5-15 mg/hr. Regular monitoring of vital signs is essential. Hallucinations are relatively common and occur in at least 50% of patients which may limit treatment
Clonidine
Clonidine acts as an agonist at the Alpha-2 adrenoceptor. It is beginning to find increased use in the perioperative period to augment the effects of opioid drugs, attenuate opioid withdrawal reactions and decrease the neurohumeral stress response to surgery. Clonidine is commonly given by the intravenous or epidural route at a dose of up to 1-2 mcg/kg peri-operatively to enhance analgesia and provide a mild sedative effect. Caution must be exercised as clonidine can induce hypotension with up to a 20% fall in baseline systolic blood pressure. Patients maintained on long term clonidine must not suddenly discontinue the drug as a hypertensive crisis may result.
Paracetamol and NSAID’s
These simple analgesics should be remembered as they exert significant opioid sparing effects. Providing no contra-indications exist to their use, all patients should have at least 48 hours of combination therapy.
Gabapentin
There is a growing body of evidence to support the use of gabapentin in the peri-operative period. Gabepentin is an anticonvulsant that is thought to act upon the α2δ subunit of calcium channels and at the GABAB receptor. When given at a dose of either 600 or 900mg pre-operatively a reduction in morphine requirements and opioid induced side-effects such as nausea and vomiting are observed in the post-operative period. Its role in the prevention of chronic pain when used in this way has not yet been proven. Gabapentin may also be used as rescue analgesia in the recovery room at a dose of 600mg or, if frail or elderly, 300mg.
Summary of Intra and Post-operative management
- Start background opioid infusion via PCA early if required
- Regularly re-assess pain post-operatively and check for signs of withdrawal e.g. unexplained tachycardia, restlessness, confusion
- Switch parenteral opioids to oral or transdermal medication as early as possible using the last 24 hours opioid consumption as a guide: give 50–75% of total dose as slow-release opioid orally or via transdermal route with the remainder given as required
- Consider a trial of an opioid rotation if pain control inadequate
- Consider the use of adjunctive medication including ketamine, clonidine and gabapentin for opioid sparing effects.
- Do not try to solve a chronic pain problem in the post operative period
Conclusion
Patients maintained on strong opioids present a unique set of challenges to the Anaesthetist. Patients’ behavioural and psychological profiles as well as issues surrounding dependency and altered pharmacokinetics need to be considered. The pre-operative visit, patient education and forward planning of opioid provision are all simple steps that can be taken to achieve successful management. No anaesthetic technique has shown a clear advantage in the literature but clinical experience suggests that where appropriate, regional anaesthesia should be employed, close attention paid to maintaining baseline levels of opioid analgesics and selective use of adjunctive analgesics for opioid sparing effects should be considered.
Multiple choice Answers
- T,T,T, F (will lead to hyperalgesia)
- T,T,T,T
- T,F,T,F. Tramadol and Pethidine are not sufficiently potent to replace conventional strong opioids postoperatively.



