Regional Anaesthesia
KEY POINTS
- Reasons for failure of regional anaesthesia for awake hand surgery are multifactorial and include performing an inappropriate block, poor patient or local anaesthetic selection, and anatomical variation.
- A thorough discussion of the surgical plan and consideration of the involved dermatomes and osteotomes will help to guide an appropriate choice of regional anaesthetic technique.
- Identification of an incomplete block is vital and allows issues to be detected and potentially corrected preoperatively.
- Continuous active management of the patient is required intraoperatively to prevent and treat pain and anxiety.
INTRODUCTION
The use of regional anaesthesia for hand surgery offers several advantages over general anaesthesia including superior analgesia, decreased opioid consumption, less postoperative nausea and vomiting, shorter postoperative nursing care time, and expedited discharge from hospital.1 However, regional anaesthetic techniques can fail for several reasons. A firm understanding of the potential causes of failure can allow anaesthetists to maximise their chances of block success and address a partially working block rather than converting to a general anaesthetic straightaway. This tutorial will not discuss techniques for nerve blocks to the hand. Readers are encouraged to review Anaesthesia Tutorial of the Week 2082 for detailed anatomy and techniques to perform forearm blocks.
REVIEW OF RELEVANT ANATOMY
Cutaneous Innervation
See Table 1 for the sensory distal cutaneous branches of the median, radial, and ulnar nerves.
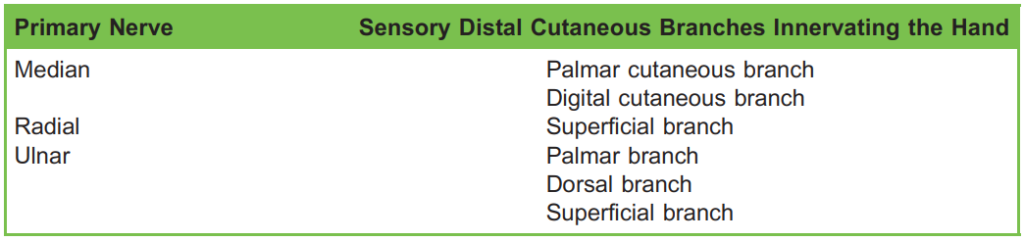
Table 1. Sensory distal cutaneous branches of the median, radial, and ulnar nerves innervating the hand
Median Nerve
The palmar cutaneous branch of the median nerve arises approximately 5 cm proximal to the wrist crease. The median nerve then passes under the carpal tunnel and terminates as the digital cutaneous branch. The median nerve therefore needs to be blocked proximally to the division of the palmar branch in order to anaesthetise this area (Figure 1).
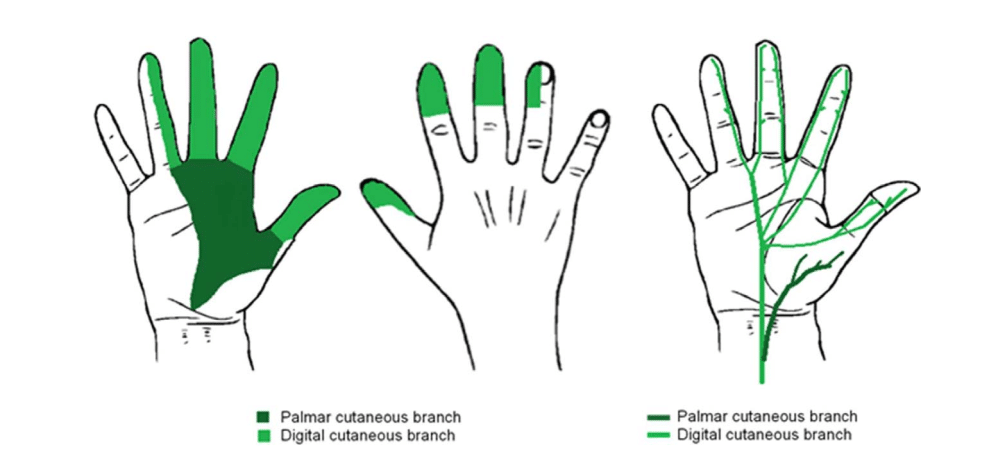
Figure 1. Cutaneous innervation of the median nerve and course of its sensory distal cutaneous branches.
Ulnar Nerve
The dorsal and palmar cutaneous branches of the ulnar nerve arise in the forearm. The dorsal branch emerges 5 to 10 cm proximal to the wrist crease and the palmar branch about 5 cm proximal to the wrist crease. The superficial branch arises within the hand itself. This means that if an ulnar nerve block is performed too close to the wrist joint the dorsal and palmar cutaneous branches may be missed (Figure 2).
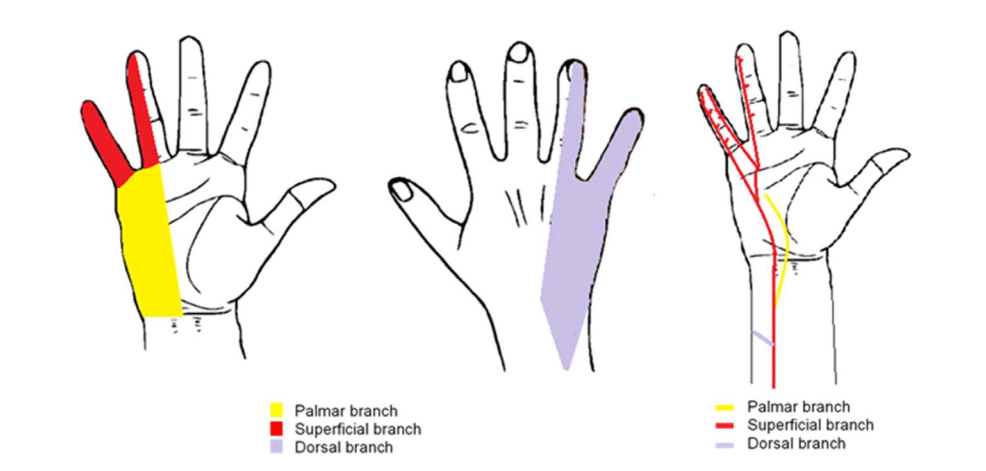
Figure 2. Cutaneous innervation of the ulnar nerve and course of its sensory distal cutaneous branches.
Radial Nerve
The radial nerve divides in the antecubital fossa into its superficial and deep branches. The superficial branch innervates the dorsum of the lateral 3½ digits of the hand. It can be blocked in the antecubital fossa or more distally as it joins the lateral side of the radial artery in the forearm (Figure 3).
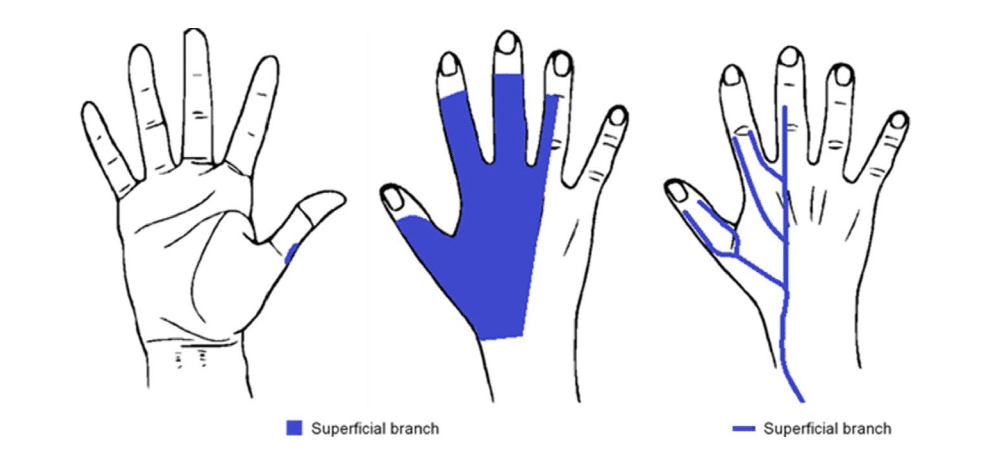
Figure 3. Cutaneous innervation of the radial nerve and course of its sensory distal cutaneous branches.
Muscular Innervation and Osteotomes
See Table 2 for the median, radial, and ulnar nerves that innervate the hand muscles; for those that innervate the bones of the left hand, see Figure 4.
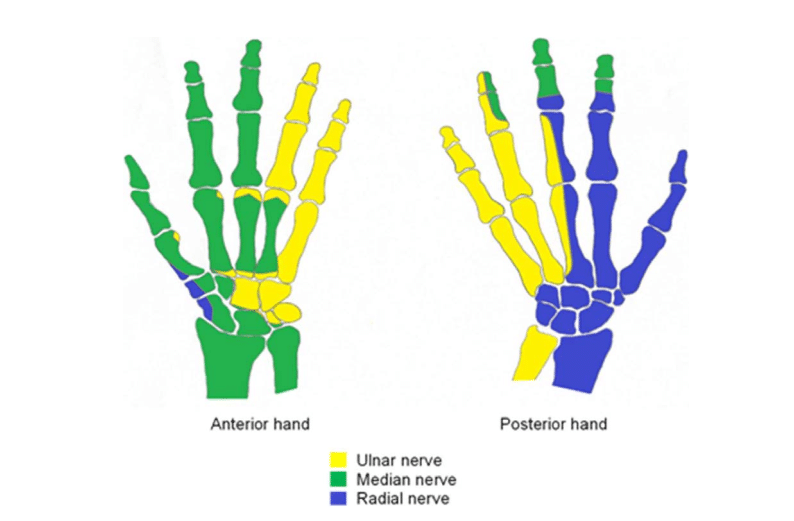
Figure 4. Innervation of the bones of the left hand (osteotomes).
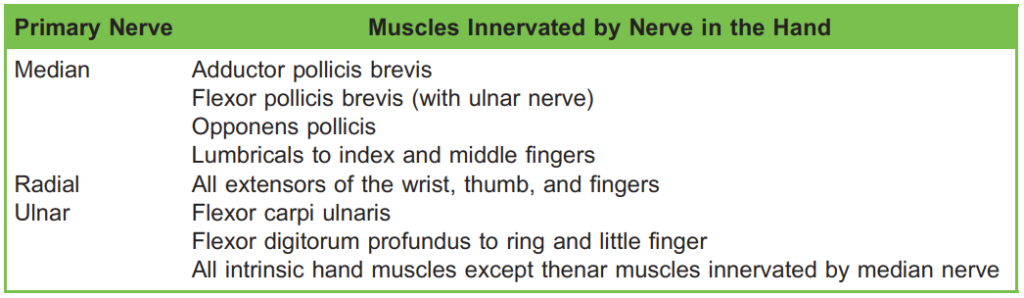
Table 2. Innervation of the muscles within the hand
WHY REGIONAL ANAESTHETIC BLOCKS FAIL
Patient Factors
For some patients a regional anaesthetic technique may not be appropriate. Language barriers may increase the degree of difficulty when performing regional anaesthesia and also limit effective communication when testing the effect of the block preand intraoperatively.3 Some patients are resistant to local anaesthetics. This can be due to multi-systemic disorders such as Ehlers-Danlos syndrome, where the mechanisms that cause this resistance are poorly understood, or due to channelopathies with genetic variations in voltage-gated sodium channels. Evidence of local anaesthetic resistance should be elicited from the patient’s history.
Comorbidities such as obesity, arthritides, and diabetes may affect positioning, access, and nerve location and identification.4 Whilst these factors may make success less likely, they do not prohibit attempting a regional technique and in some situations an awake regional technique may still be favoured to avoid the risk of general anaesthesia in high-risk patients. Awake surgery can be stressful and cause significant anxiety to some patients. Anxiety in patients having surgery has a prevalence of up to 80%.5 Patients are exposed to unaccustomed sounds, smells and surroundings of the operating room. This anxiety may affect the patient’s ability to cooperate and increase the incidence of restlessness perioperatively. Whilst in most cases this anxiety can be managed with communication and/or conscious sedation, there are some patients who remain adamant they do not want a regional anaesthetic: convincing them otherwise can lead to a more challenging and less successful regional anaesthetic.
Experience of the Operator
Regional anaesthesia is a practical skill and success will vary depending on the individual clinician’s skills, the number of cases they have performed and the teaching they have been exposed to. Success rates will also depend on their chosen technique. When ultrasound is used rather than landmark or nerve stimulation techniques, direct visualisation of the nerves and distribution of local anaesthetic can increase success rates, improve the quality, and minimise complications of the block.
Inappropriate Block
For hand surgery, nerves can be blocked proximally at the level of the brachial plexus or more distally at the elbow, forearm, wrist, or base of the digits. When considering which regional anaesthetic technique to perform it is vital to have an in-depth discussion with the surgeon regarding the procedure to be performed, the incision site and the use of a tourniquet. This will allow consideration of which dermatomes and osteotomes will be involved surgically (Figures 1–4) and the appropriate regional technique to use. The median, ulnar, and radial nerves provide the cutaneous supply to the hand (Figure 1–3). When considering which nerves to anaesthetise, and where to block them, it is important to consider the distal cutaneous branches and where they branch from so that branches are not missed (Table 1).
The axillary, infraclavicular, and supraclavicular approaches to the proximal brachial plexus are commonly used and all 3 approaches have a similar quality of surgical anaesthesia for operations below the shoulder.6 While the supraclavicular and infraclavicular approaches provide better tourniquet tolerance,7 the axillary block is popular for hand surgery as it is associated with fewer serious complications such as phrenic nerve palsy and pneumothorax. The supraclavicular block has a slower rate of onset of ulnar blockade and a higher degree of ulnar sparing.8 Therefore, this block is the least preferable of the proximal brachial plexus approaches if the surgery requires ulnar blockade (Figure 2).
It is also important to consider the duration of surgery as the patient may not tolerate being in the same position for a long period of time despite having a good working block.
Tourniquet Use
Patients are usually able to tolerate a tourniquet on the arm without anaesthesia for a maximum of 20 minutes.9 If the tourniquet use is expected to be longer, proximal brachial plexus blocks, and not distal nerve blocks, should be used to cover the tourniquet discomfort. Take note, an effective peripheral nerve block will help with tourniquet discomfort due to local pressure effects but will not help tourniquet pain due to ischaemia. If performing an axillary brachial plexus block, the musculocutaneous nerve must also be blocked to cover tourniquet pain. An intercostobrachial nerve block (which is never covered in any brachial plexus block) can be additionally used but will only alleviate the pressure discomfort resulting from an upper-arm tourniquet, it will not block the ischaemic component that causes tourniquet pain.10
If the surgical team is planning to use a wrist tourniquet, this causes less muscle ischaemia and pain, so can be tolerated without anaesthesia for approximately 120 minutes.9 When an arm tourniquet is not required, more distal regional blocks can be used. This has the advantage of causing less extensive motor blockade for the patient postoperatively.
Anatomical Variation
The path and area of innervation of peripheral nerves can be variable in different patients.4 The overlap of innervation means that depending on the location of surgery, it can be unwise to rely on the block of a single nerve and doing this may mean that the regional technique is less likely to succeed. It is advisable to block all nerves that could be involved.
Selection of Local Anaesthetic
The choice of local anaesthetic is guided by safety profile, speed of onset, and duration of action.11 The commonly used local anaesthetic agents and their properties are listed below (Table 3).9 If a local anaesthetic with a slower onset time is used, allow sufficient time before testing for the anaesthetic effect, otherwise it may appear that the regional block has not worked if tested prematurely.

Table 3. Commonly used local anaesthetic agents and their onset, duration of anaesthesia, and duration of analgesia
TROUBLESHOOTING ISSUES: WHAT TO DO IF A BLOCK FAILS
An incomplete block can range from one that fails completely to one that is not dense enough or one where a segment of innervation is missed. A thorough assessment should always be carried out. The effect of regional blockade can be assessed using light touch, pain, motor block, or cold sensation (Table 4). In our institution we routinely use motor movements and cold spray to test the motor and sensory block.

Table 4. Sensory area and motor movement used to test a median, ulnar, and radial nerve block after regional anaesthetic
Preoperative Troubleshooting
Allow More Time
If the patient has started to feel a pins and needles sensation in the required area but the block is not sufficiently dense, try allowing more time for the block to develop. The onset of anaesthesia in isolated nerves slows with increasing LA lipid solubility and increasing pKa. There are no set recommendations of how long to wait before testing each block. In our institution we aim to wait approximately 20 minutes before testing. If the local anaesthetic is deposited further away from the nerve then it will be affected by the vascularity of surrounding tissue and fascial layers and will be absorbed by fat. Therefore, more time may be needed before the block has a full anaesthetic effect.
Top Up With More Distal Blocks
If a proximal brachial plexus block has been performed, one of the nerves within the plexus may not be blocked with local anaesthetic sufficiently, meaning that one or more distal nerves may be spared. This is particularly true of a supraclavicular block where the ulnar territory can be missed. It is important to ascertain if the missed area is required for the surgery as it may be possible to proceed with a missed segment. However, if the missed nerve territory needs to be blocked, this may be achieved by topping up with a distal nerve block.
Intraoperative Troubleshooting
If the patient starts to experience pain intraoperatively, it is important to clarify whether the source of the pain is the surgical site, the tourniquet, or due to uncomfortable positioning on the operative table.
Local Anaesthetic Supplementation by Surgeons
After testing the regional block, it is possible to have an incomplete block. This is where the patient has some numbness in the area of nerve distribution that is not adequate for the incision, so the patient will experience some surgical site sensation. As an alternative to further regional anaesthetic, surgeons can infiltrate the surgical site with a fast-acting local anaesthetic. It is important to ensure that the toxic dose of local anaesthetic is not exceeded with the combined use of local infiltration and the initial regional blockade (Table 5).
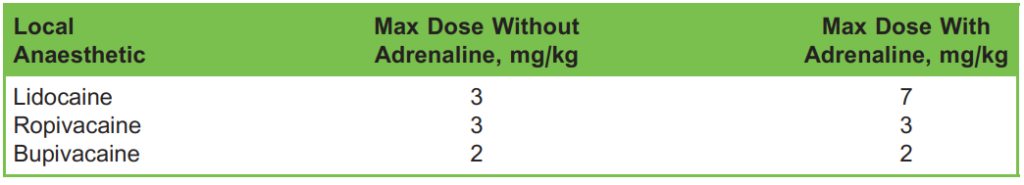
Table 5. Toxic doses of commonly used local anaesthetic drugs with and without adrenaline
Distraction Techniques
Awake surgery can be stressful and cause significant anxiety to some patients. Patients are exposed to unaccustomed sounds, smells, and surroundings of the operating room. This anxiety may hamper the success of a regional block and should be minimised. A screen should always be used so that the patient is unable to see the surgical procedure. Distraction techniques such as engaging patients in conversation and using audio-visual headsets can significantly decrease the level of anxiety and allow the procedure to continue.12
Sedation
Sedation should only be used to cover anxiety, tourniquet discomfort or positional discomfort, not to overcome pain or an inadequate block.4 Commonly used sedative agents include intravenous midazolam or propofol. Propofol sedation can be administered using continuous target control infusion, which uses pharmacokinetic models to deliver a variable rate of propofol in order to obtain and maintain a specified effect site drug concentration, patient controlled sedation (PCS), where the patient can deliver themselves boluses of propofol using a handheld trigger, or patient-maintained sedation (PMS), which involves a TCI system where the effect site concentration is influenced by the patient using a handheld trigger.13
Managing Tourniquet Pain
Patients may start to experience positional or tourniquet pain as the procedure continues despite a working block. Tourniquet pain is related to the duration of inflation and is caused by noxious stimuli from ischaemia and compression.14 Depending on the stage of the procedure, the surgical team may be able to deflate the tourniquet to allow perfusion to the limb. In a long procedure, intermittent tourniquet deflations may be discussed with the surgical team preoperatively. If deflation is not possible then systemic analgesia or sedation could be used as a temporary measure. This should only be used for a short time as this may not be effective and make the patient less compliant to commands. If this does not work a general anaesthetic may then be required.
Conversion to a General Anaesthetic
If attempts to salvage a partially working regional block have not been successful, struggling with an inadequate regional technique can cause anxiety or trauma to the patient. In this situation a general anaesthetic should always be offered. Almost always the regional technique will allow for the depth of general anaesthetic to be reduced and provide a reduction in postoperative pain and morphine consumption.4
SUMMARY
When performing regional anaesthesia for awake hand surgery ultrasound-guided techniques are advised as this has been shown to improve success rates and decrease complications. A thorough discussion with the surgical team preoperatively about the surgical procedure and tourniquet use will help to ensure that the correct regional technique is performed. Allow sufficient time for the block to take full effect before testing for surgical readiness. If a block is incomplete, supplement with distal nerve blocks if the missed area is necessary for surgery. Intraoperatively, local anaesthetic supplementation can be useful if pain is experienced during the surgical incision. If pain develops as the surgery continues, systemic analgesia, sedation, distraction techniques, or tourniquet deflation may help. However, a general anaesthetic should always be offered if the patient is experiencing surgical pain or anxiety despite troubleshooting techniques.
REFERENCES
1. Chan VW, Peng PW, Kaszas Z, et al. A comparative study of general anesthesia, intravenous regional anesthesia, and axillary block for outpatient hand surgery: clinical outcome and cost analysis. Anesth Analg. 2001;93:1181-1184.
2. Brennan A, Jones M, Gordon J. ATOTW 208. Ultrasound-guided local anaesthetic blocks of the forearm. Accessed November 25, 2020. https://resources.wfsahq.org/components/com_virtual_library/media/e873f607001acfd4ffb397e23d43723d-208-US-guided-local-anaesthetic-forearm-blocks.pdf
3. Shapeton A, O’Donoghue M, VanderWielen B, et al. Anesthesia lost in translation: perspective and comprehension. J Educ Perioper Med. 2017;19(1):E505.
4. Nicholls B. ‘My block doesn’t work’—analysis of possible reasons, avoidance and emergency strategies. Accessed October 19, 2019. https://www.esahq.org/~/media/ESA/Files/Refresher%20Courses/2011/My%20block%20does%20not%20work%20%20Analysis%20of%20possible-%20reasons%20avoidance%20and%20emergency%20strategies%202011.ashx
5. Jlala HA, Bedforth NM, Hardman JG. Anesthesiologists’ perception of patients’ anxiety under regional anesthesia. Local Reg Anesth. 2010;3:65-71.
6. Stav A, Reytman L, Stav MY, et al. Comparison of the supraclavicular, infraclavicular and axillary approaches for ultrasound-guided brachial plexus block for surgical anesthesia. Rambam Maimonides Med J. 2016;7:2.
7. Shanthanna H, Rajarathinam M. Regional anesthesia for hand surgeries, essentials of hand surgery. Accessed October 19, 2019. https://www.intechopen.com/books/essentials-of-hand-surgery/regional-anesthesia-for-hand-surgeries
8. Raju PK, Coventry DM. Ultrasound-guided brachial plexus blocks. Cont Educ Anaesth Crit Care Pain. 2014;14(4):185-191.
9. New York School of Regional Anesthesia. Wrist block—landmarks and nerve stimulator technique. Accessed October 19,2019. https://www.nysora.com/techniques/upper-extremity/wrist/wrist-block/
10. New York School of Regional Anesthesia. Cutaneous blocks for the upper extremity—landmarks and nerve stimulator technique. Accessed October 19, 2019. https://www.nysora.com/techniques/upper-extremity/distal-nerves/cutaneousblocks-upper-extremity/
11. Snaith R, Dolan J. Ultrasound-guided peripheral upper limb nerve blocks for day-case surgery. Cont Educ Anaesth Crit Care Pain. 2011;11(5):172-176.
12. Sven-Olof Tra¨ ngeberg O¨ , Stomberg MW. Listening to music during regional anesthesia: patients; experiences and the effect on mood. J Perianesth Nurs 2013;28(5):291-297.
13. European Society of Anaesthesia. Pro-con debate: sedation is routinely used in patients having surgery under regional anaesthesia. Accessed October 19, 2019. http://newsletter.esahq.org/pro-con debate-sedation-is-routinely-used-in-patients-having-surgery-under-regional-anaesthesia/
14. Hagenouw RRPM, Bridenbaugh PO, Van Egmond J, et al. Tourniquet pain: a volunteer study. Anesth Analg. 1986;65:1175-1180.



