General Topics
QUESTIONS
Before continuing with this tutorial, try to answer the following questions. The answers can be found at the end of the article, together with an explanation.
- Which of the following is most reliable in assessment of residual neuromuscular blockade?
a. Train of four ratio < 0.7
b. Train of four ratio < 0.9
c. Clinical signs
d. Patient symptoms - When monitoring the adductor pollicis muscle, which statements are correct?
a. The thenar branch of the median nerve is being stimulated
b. The positive (red/white) electrode should be placed proximally on the forearm
c. It is more accurate to use tactile than visual assessment for twitches and fade
d. Assessment using this muscle correlates well with diaphragmatic function - Select true or false for these statements
a. Long-acting neuromuscular blockers are relatively low risk for residual neuromuscular blockade
b. For safest results, neostigmine should be given at all train of four ratios
c. Sugammadex offers additional, but limited, benefits in reversal of neuromuscular blockade
d. Residual neuromuscular blockade is an uncommon problem of minor consequence
DEFINTION AND CONTEXT
Residual neuromuscular blockade can be defined by inadequate neuromuscular recovery as measured by objective neuromuscular monitoring. It is also referred to as residual paralysis, residual curarisation, and residual neuromuscular block. More specifically, recent opinion suggests a definition of inadequate train of four recovery of less than 0.9 (TOF <0.9)1.
The train of four method of peripheral nerve stimulation was introduced in the 1970s. The use of a threshold ratio of 0.7 was derived from several studies aiming to establish the concept of “acceptable recovery”. This ratio was derived from certain clinical signs and subjective neuromuscular monitoring including the ability of patients to open their eyes widely, cough, protrude their tongue, attain vital capacity breaths of 15-20 mL/kg, and sustain tetanic stimulation without fade for 5 seconds1.
With advances in monitoring and continued studies, a TOF <0.9 is now considered as residual neuromuscular blockade. This more stringent ratio was arrived at after several studies demonstrated an increased risk of aspiration and pharyngeal dysfunction at TOF <0.9, and impaired inspiratory flow and partial airway obstruction at TOF <0.81
It should be noted that there is a large variability between patients. Some patients may display obvious muscle weakness despite a TOF>0.9, whilst complete clinical recovery of muscle strength can be observed in others with a TOF<0.9. Importantly, distressing symptoms in awake patients may be observed even at subtle levels of neuromuscular block of TOF >0.91.
On a practical level, the concept of adequate neuromuscular recovery is intended as the return to a basline muscular function, particularly the ability to breathe normally, maintain a patent airway, and retain protective airway reflexes.
INCIDENCE
It has been difficult to prove the association of residual neuromuscular blockade with significant morbidity and mortality. This is largely due to the relatively low incidence of major adverse outcomes after anaesthesia and surgery. There are also a limited number of randomized controlled trials concerning this topic, and inadequate numbers of well designed cohort studies. There are many variables in clinical practice that will influence residual neuromuscular blockade, which has led to a heterogenous pool of evidence.
However, current estimates are that around 40% of post-operative patients (who have been paralised) arrive in PACU with TOF <0.9, and 12% with TOF <0.73. This is in comparison to estimates in the 1970s, where around 45% of patients arrived with TOF <0.75. Based on studies examining morbidity from residual blockade, a rough estimate of 1-3% of these patients would be expected to develop clinically aparent events1. Considering the large percentage of patients estimated to have residual blockade, it could be easily inferred that most patients tolerate residual block of modest depth without untoward results. However, there exists a small proportion of patients, particularly those with existing limited physiological reserve where residual neuromuscular blockade has serious consequences.
ADVERSE EFFECTS OF RESIDUAL NEUROMUSCULAR BLOCKADE
The following tables detail the implications of residual neuromuscular blockade (these are more illustrative than exhaustive)1.
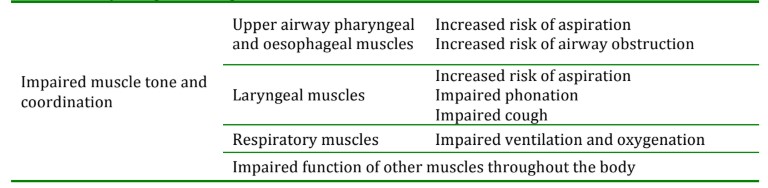
Table 1: Physiological changes
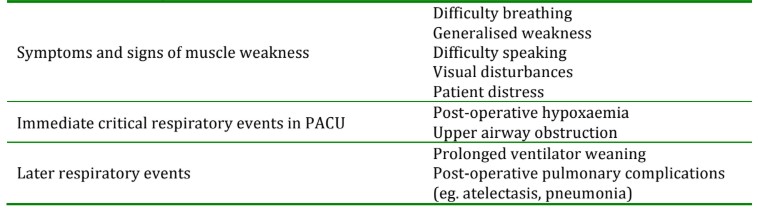
Table 2: Clinical implications
INVESTIGATIONS
The ideal test of neuromuscular recovery would not require an awake, cooperative patient and would be easily applied, reliable and inexpensive.
Clinical criteria for evaluating adequacy of muscle function include: assessment of a patient’s ability to maintain adequate head lift, jaw clench, grip strength, and tidal volume. These are unreliable predictors of neuromuscular recovery. For example, it is possible to maintain a 5 second head lift with TOF <0.52. In addition, many of these tests are not specific for respiratory function. The table below describes the diagnostic value of 2 common clinical tests2
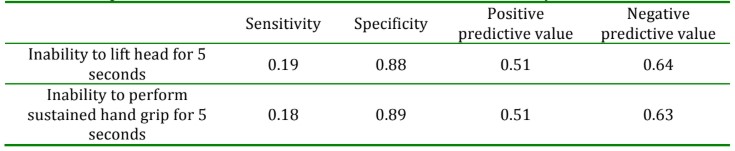
Table 3: Diagnostic attributes of clinical tests of neuromuscular recovery
Train-of-four neuromuscular monitoring is commonly conducted with a subjective measurement, either as a simple train of four count (TOFC) or train of four ratio (TOF). The latter refers to when there is already a TOFC of 4, and subsequent assessment is made for fade in T4 compared to T1. Tactile evaluation (movement of patient’s thumb against the observer’s fingers) is more accurate than visual assessment2. However, neither are reliable in detecting fade (37% versus 57% in one study6), and themajority of evaluators are unable to detect fade when TOF ratios > 0.47.
Double Burst Stimulation (DBS) is another method of neuromuscular monitoring, but is also commonly measured in a subjective manner.. This improves detection of fade to up to 0.6 – which is significant, but doesn’t eliminate the incidence and degree of residual neuromuscular blockade8.
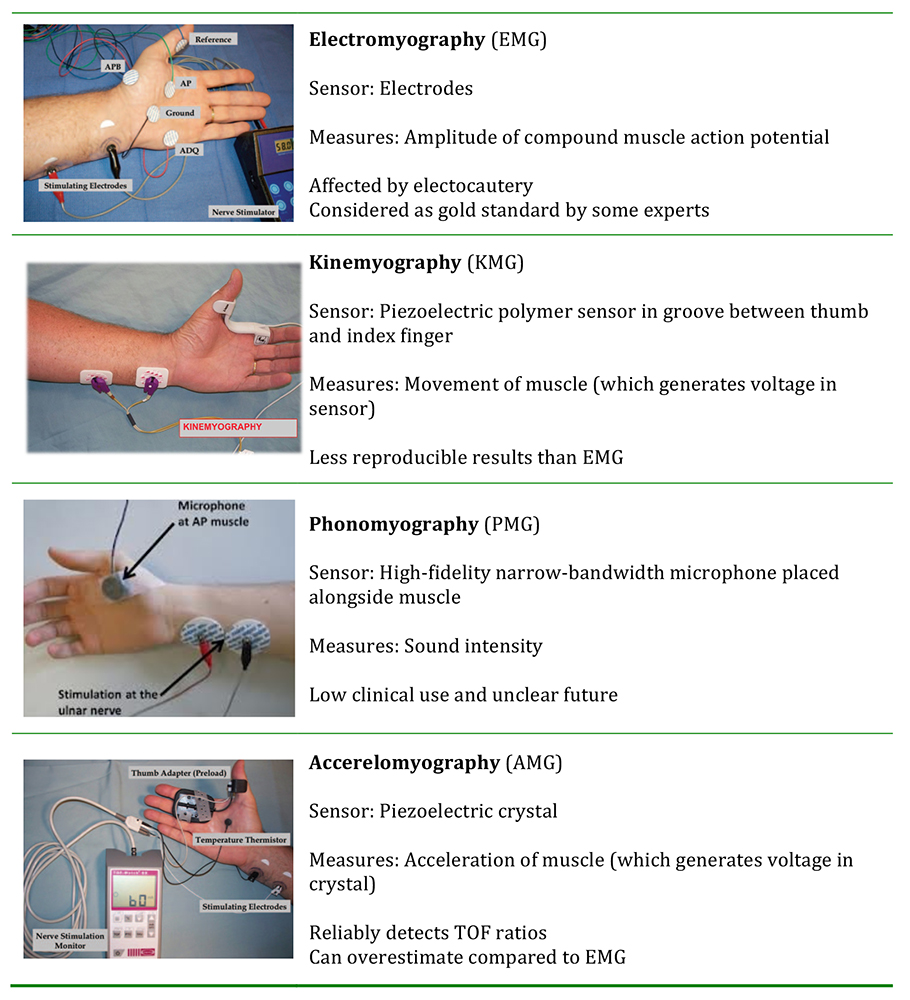
Objective measurement of neuromuscular monitoring is the only way of accurately assessing residual neuromuscular blockade. In general, it is conducted via quantitative measurement of the strength of contraction of a peripheral muscle (eg. adductor pollicis muscle in thumb) in response to peripheral nerve stimulation (eg. ulnar nerve at wrist) produced by 2 stimulating electrodes. Each measurement technique measures the force of contraction, either directly or by a factor that is proportional to force.

Table 4: Different types of objective neuromuscular monitoring devices (photos courtesy of Dr Sorin J Brull, MD, and Dr Thomas M Hemmerling, MD.)
PRACTICAL NERVE STIMULATOR TIPS
With multiple options for site and method of neuromuscular monitoring, the question becomes which site is best for establishing depth of paralysis. Two sites are commonly utilized, each having its own advantages. Measurment at the adductor pollicis correlates well with the tone in the upper airway and upper oesophageal muscles4. The muscles around the eye (orbicularis oculi and corrugator supercilii) recover early (much like the diaphragm), and a TOFC of four here is often correlated with a TOFC of two or less at the adductor pollicis4.
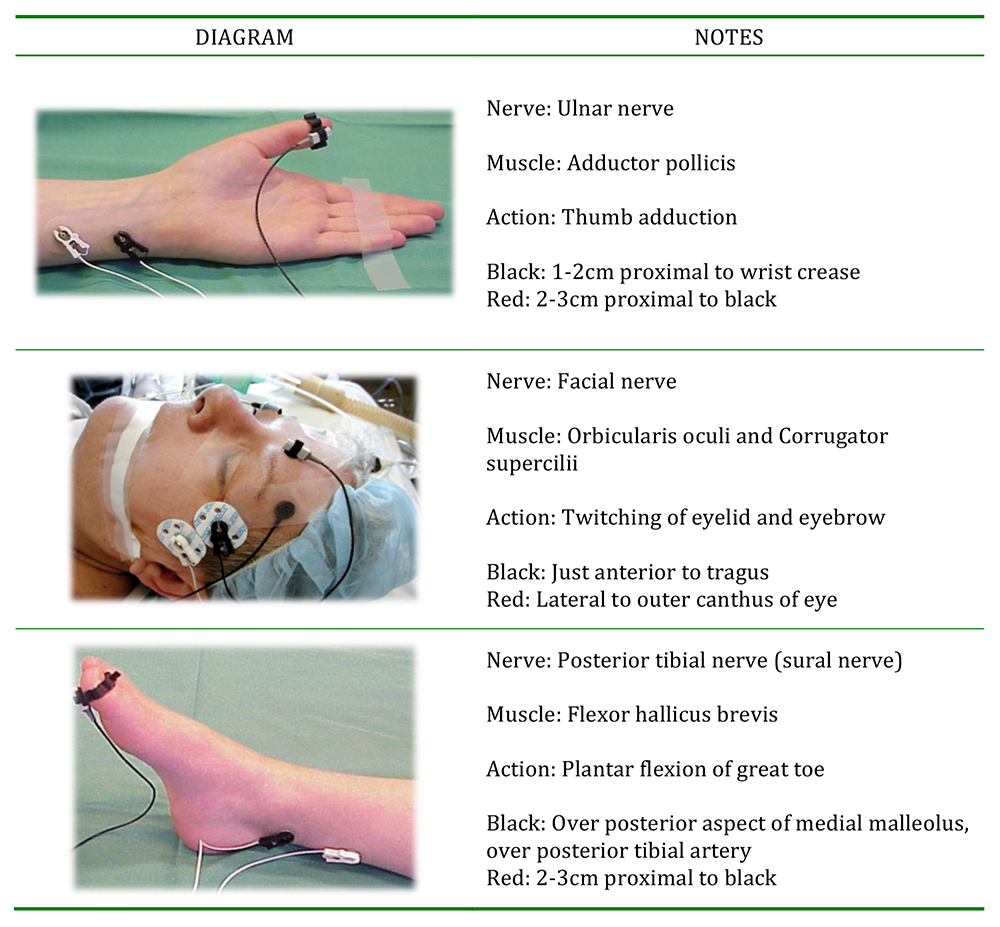
Table 5: Common sites of peripheral nerve stimulation (photos courtesy of Dr Sorin J Brull, MD)
Placement of electrodes is also an important aspect of accurate and successful neuromuscular monitoring. The electrodes should be placed over the path of the peripheral nerve. The negative (black) electrode is the active stimulating electrode, and the most effective stimulation is obtained when placed closest to the muscle terminus. The positive (red) electrode is placed 2cm proximally. The sites should be clean, dry, and shaved. A supramaximal stimulus of 60mA should be used.
REVERSAL AGENT
It is good practice to always consider giving a reversal agent, unless there is objective neuromuscular monitoring demonstrating a TOF >0.9 (giving neostigmine to fully recovered patients may decrease upper airway muscle activity and tidal volume)2. Presently, anticholinesterases are one of the most common techniques for reversing neuromuscular blockade – neostigmine, pyridostigmine, edrophonium. It should be noted that there is a great deal of variability in the time to onset and duration of neostigmine reversal. Given given after TOFC of two, the average time to adequate reversal is 15 minutes, with some patients still demonstrating residual neuromuscular blockade (TOF<0.9) after 30 minutes!2
Adequate spontaneous recovery of train of four count should be established BEFORE giving reversal. When using anaesthetic techniques that do not potentiate neuromuscular blockers, eg. TIVA, a minimum TOFC of 2 should be established. When using anaesthetic techniques that do potentiate neuromuscular blockers, eg. inhalational volatiles, a TOFC of 4 should be established. This is to ensure adequate antagonism by the reversal agent of the additional depth of neuromuscular blockade.
It is important to remember the estimated physiological correlations with TOF:
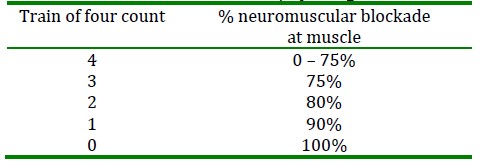

Table 5: Train of four count and physiological correlation
Suggestions for neuromuscular reversal in clinical practice2.
Reversal with subjective neuromuscular monitoring
- TOFC 1 or zero = delay reversal
- TOFC 2 or 3 = give reversal
- TOFC 4 with fade = give reversal
- TOFC 4 with no perceived fade = give reversal, consider low dose (20 μg/kg) neostigmine
- TOFC 4 and >0.9 = withhold reversal
Reversal with objective neuromuscular monitoring
- TOFC 0 or 1 = delay reversal
- TOFC 2 or 3 = give reversal
- TOFC 4 with < 0.4 = give reversal
- TOFC 4 with 0.4-0.9 = give reversal, consider low dose neostigmine
- TOFC 4 and >0.9 = withhold reversal
Reversal guidelines with clinical neuromuscular monitoring
- Only consider reversal when spontaneous muscle activity is present
- Remember that clinical tests of adequate reversal are unreliable indicators of neuromuscular blockade
NEUROMUSCULAR BLOCKERS (NMB)
It is worth making note of the factors that have been shown to contribute to residual neuromuscular blockade
- Use of NMBs. They should only be used when indicated.
- Dose. High dose NMB (3-4 ED95) used for modified rapid sequence inductions, will prolong the duration (50-300%) of blockade compared with normal-dose (1-2 ED95)1. Dosing should also always be individualized to the patient and surgical necessity.
- Type. The use of long acting NMB (such as pancuronium) is associated with a 3-fold higher risk of TOF<0.7 in the post-operative period3. Intermediate acting NMB (such as rocuronium and vecuronium) should be preferred when feasible.
- Depth. Routine maintenance of deep intra-operative paralysis (TOFC zero and PTC 0-5) is associated with residual neuromuscular blockade3.
Special attention to appropriate NMB use must be taken with patients at high risk: those with neuromuscular disease, respiratory disease, sleep apnoea, the elderly, and the obese3.
TREATMENT OF RESIDUAL NEUROMUSCULAR BLOCKADE
- ABC. Basic resuscitation is the foundation on which the following steps are to be considered: support the patient’s airway, breathing, and circulation.
- Rule out other potential causes. Is this really residual neuromuscular blockade? Check nerve stimulator, use a different nerve-muscle combination.
- Consider giving reversal. In some institutions, it is still not routine for reversal to be used, largely due to concerns of cholinergic symptoms of nausea and bradycardia with cholinesterase inhibition.
- Wait. Have you given enough time for the reversal to have effect? Is the patient stable enough to tolerate watchful waiting.
- Consider giving additional reversal. Note however, that if there is already complete inhibition of acetylcholinesterase, giving further neostigmine will not serve any useful purpose.
- Treat potentiating factors. Many factors prolong neuromuscular blockade, such as inhalational agents, opioids, acidosis, hypothermia, hypercarbia, hypoxia.
- Consider alternative methods of reversal (Sugammadex if available) (see below).
SUGAMMADEX
Sugammadex is a modified gamma-cyclodextrin (ie. cyclic sugar) that has recently become available throughout numerous countries and is being trialled for approval in many others. Chemically, it has a hydrophilic periphery and a negatively charged lipophilic core that selectively binds aminosteroid NMB (rocuronium > vecuronium >> pancuronium). It is unique as an SRBA (selective relaxant binding agent) and at 2mg/kg, when given at TOFC 2, will reliably produce TOF >0.9 in 2 minutes. There is no biotransformation and elimination is by renal excretion only.
Its availability and cost are factors limiting more widespread use of this drug at present, but its potential to rapidly reduce neuromuscular blockade and concomitantly reduce the incidence of residual blockade make it an important pharmacological agent to be familiar with.
IMPORTANT POINTS
Residual neuromuscular blockade is a common problem. Although usually well tolerated, there can be serious consequences. The use of objective neuromuscular monitoring should be routine. Clinical knowledge of neuromuscular blockers and reversal agents should be an essential component of any perioperative provider. Clinicians should familiarise themselves with the necessary steps in treating residual neuromuscular blockade.
- Be aware that a significant number of patients currently have residual neuromuscular blockade
- TOF ratios up to 0.9 have been associated with increased morbidity.
- Be familiar with how to appropriately use and monitor neuromuscular blockers
- Remember the pharmacokinetics and dynamics behind the commonly used reversal agents
- Be alert to, and ready to treat, residual neuromuscular blockade
ANSWERS TO QUESTIONS
- Which of the following is most reliable in assessment of residual neuromuscular blockade?
a. Incorrect. TOF <0.9 constitutes residual neuromuscular blockade.
b. Correct. TOF >0.9 constitutes adequate reversal of neuromuscular blockade
c. Incorrect. Clinical signs are very variable.
d. Incorrect. Patient symptoms are very variable. - When monitoring the adductor pollicis muscle, which statements are correct?
a. Incorrect. The ulnar nerve is being stimulated.
b. Correct. The positive (red/white) electrode should be placed proximally on the forearm
c. Correct. It is more accurate to use tactile assessment for twitches and fade
d. Incorrect. The diaphragm recovers earlier. - Select true or false for these statements
a. False. Long-acting NMB are high risk for residual neuromuscular blockade
b. False. Use of neostigmine at TOF >0.9 can decrease upper airway muscle activity
c. True. Sugammadex offers markedly superior reversal.
d. False. Residual neuromuscular blockade is a very common problem, and although serious consequences are uncommon, they can be fatal.
REFERENCES and FURTHER READING
- Murphy GS, Brull SJ. Residual neuromuscular block: lessons learned. Part 1: definitions, incidence, and adverse physiologic effects of residual neuromuscular block. Anesth Analg 2010;111:120-8.
- Brull SJ, Murphy GS. Residual neuromuscular block: lessons unlearned. Part 2: Methods to reduce the risk of residual weakness. Anesth Analg 2011;111:129-40.
- Naguib M, Kopman AF, Ensor JE. Neuromuscular monitoring and postoperative residual curarisation: a meta-analysis. BJA 2007;98(3):302-16.
- Donati F. Neuromuscular monitoring: more than meets the eye [comment]. Anesthesiology 2012;117(5):934-6. Comment on: Anesthesiology 2012;117:964-72.
- Viby-Mogensen J, Jorgensen B, Ording H. Residual curarization in the recovery room. Anesthesiology 1979;50:539-41.
- Viby-Mogensen J, Jensen NH, Engbaek J, Ording H, Skovgaard LT, et al. Tactile and visual evaluation of the response to train-of-four nerve stimulation. Anesthesiology 1985;63:440-443.
- Brull SJ, Silverman DG. Visual and tactile assessment of neuromuscular fade. Anesth Analg 1993;77:352-5.
- Drenck NE, Ueda N, Olsen NV, Engbaek J, Jensen E, et al. Manual evaluation of residual curarization using double burst stimulation: a comparison with train-of-four. Anesthesiology 1989;70:578-81.



