Regional Anaesthesia
QUESTIONS
Before continuing, try to answer the following questions. The answers can be found at the end of the article, together with an explanation.
- Regarding the properties of sound waves, which of the following statements is correct?
- ‘Wavelength’ refers to the time taken for one complete wave cycle to occur.
- The speed of a sound wave is unrelated to the medium through which it travels.
- Frequency is inversely related to wavelength.
- Frequency is directly related to the period
- The SI unit of frequency is the candela.
- When considering clinical ultrasound, which of the following statements are correct?
- Clinical ultrasound uses sound waves in the frequency range 1 – 20 MHz.
- The average velocity of clinical ultrasound through the soft tissues of the body is 1540 m/s
- B-mode is the most commonly used image modality.
- Piezo-electrical materials are unaffected by pressure changes.
- The Doppler effect refers to the change in frequency for an observer moving relative to the source of the sound wave.
- The difference in acoustic impedance between the air/soft tissue interface is?
- Large.
- Small.
- Smaller than the muscle/liver interface.
- Smaller than the blood/water interface
- Not detectable.
INTRODUCTION
Imaging with ultrasound is finding ever increasing applications in modern medicine. The use of oesophageal doppler to monitor cardiac output and guide fluid therapy is now widespread and the use of ultrasound devices in ICU extends to assessment of cardiac function via trans-thoracic/ transoesophageal ECHO. In anaesthesia the utilization of ultrasound is well established for obtaining vascular access and performing a myriad of peripheral nerve blocks.Ultrasound-guided techniques are helping to increase success rates and reduce complications.
Understanding the physical principles of ultrasound forms part of the core knowledge in training in anaesthesia.
BASIC PRINCIPLES OF SOUND WAVES
Sound is mechanical energy that is transmitted through a medium by vibration of molecules. Sound waves are termed „longitudinal‟ waves, which refers to the fact that the molecules oscillate in a line which is in the same direction as the propagated wave.
Sound waves are characterized by the following parameters:
- Wavelength (λ) –This is the distance over which a wave‟s shape repeats, determined by measuring the distance between two consecutive corresponding points of the same phase. It is expressed in units of distance (m, cm, mm, etc.)
- Amplitude (A) –This is a measure of the maximum height of the wave and refers to the particle displacement.
- Period (τ) – This is the time taken for one complete wave cycle to occur.
- Frequency (f) – This is the number of complete cycles per second. The SI unit of frequency is the hertz (Hz). One hertz equals one cycle per second. Humans hear sound within a range of 20 Hz to 20 kHz. Ultrasound has a frequency above 20 kHz, i.e. above the threshold of human hearing. Clinical ultrasound is in the range 1 – 20 MHz (1 MHz = 1000000 Hz). Frequency is inversely related to the period.
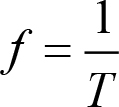
- Velocity (c) –This is the speed at which sound waves pass through a medium. The velocity of a sound wave is determined by the physical properties of the medium it is passing through and may be calculated using the equation:
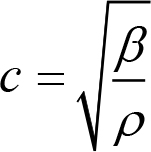
Where c is the speed,β is the stiffness (Bulk Modulus) and ρis the density. Audible sound waves are transmitted through air at a speed of 330 m/s. Clinical ultrasound is transmitted through the soft tissues of the body at an average speed of 1540 m/s. The typical speed for different tissues is:
- Liver 1580 m/s
- Muscle 1575 m/s
- Blood 1570 m/s
- Fat 1430 m/s
- Bone 4080 m/s
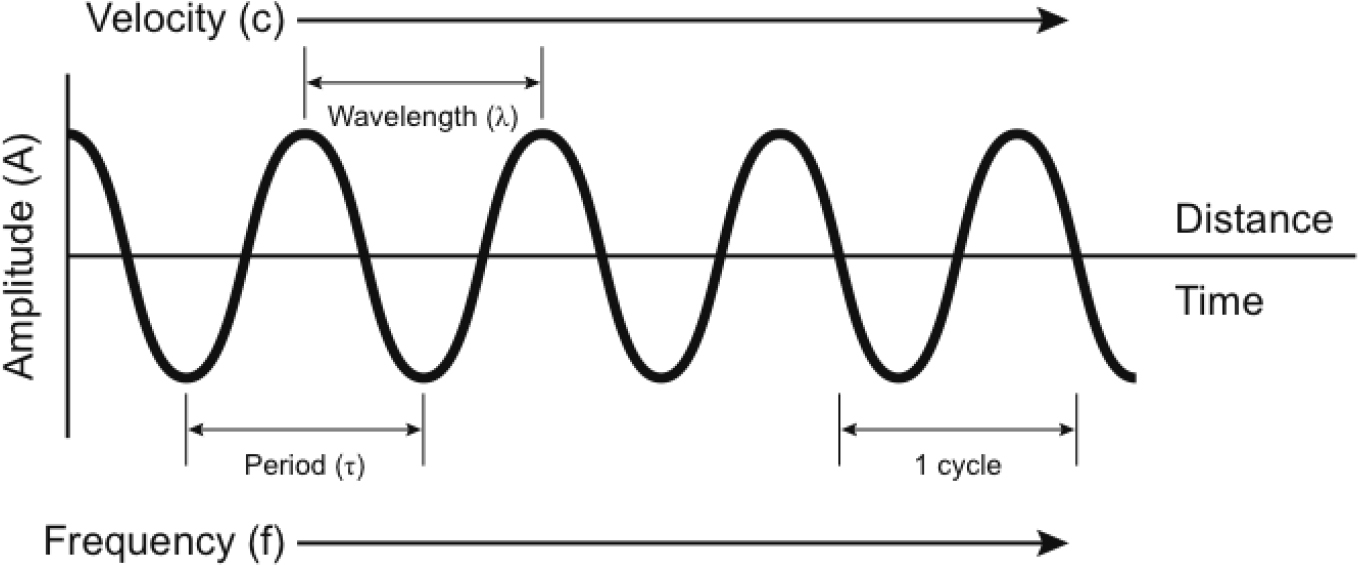
Figure 1: The Parameters of a Sound Wave
The Wave Equation
The wave equation relates frequency (f), wavelength (λ) and velocity (c). See Figure 1.
c = λ f
Velocity through soft tissue is assumed to be constant (1540 m/s) hence there is an inverse relationship between frequency and wavelength, so that as frequency increases, wavelength decreases and vice versa. In clinical ultrasound resolution is related to wavelength, whilst frequency is related to depth of penetration and attenuation.
GENERATING ULTRASOUND AND IMAGE PRODUCTION
Structure of the probe
The ultrasound probe contains a large number of individual transducers arranged in a line called an array. Each transducer transmits a short burst of ultrasound and then is silent until it detects the waves returning. This is termed „pulsed ultrasound‟. Small groups of transducers are activated in turn so that some part of the probe head is always emitting or receiving.
The piezo-electric effect
Some materials, most notably crystals and certain ceramics, change shape when an electric charge is applied across them. These materials also exhibit the converse effect whereby when pressure is applied they change shape and an electrical charge is created. This phenomenon is known as the piezo-electric effect and such piezo-electrical materials form the transducers in the array of the ultrasound probe, allowing it to act as both a sound transmitter and receiver. The emitted ultrasound signal is produced by applying an electrical charge to each individual transducer. The generated sound wave then propagates into the tissues under examination and is either reflected or scattered. The reflected portion returns to the probe where it distorts the shape of the transducer and creates an electrical charge that can be processed to produce an image.
Image Production
Two-dimensional images are formed one line at a time, by sweeping the ultrasound beam across the imaging plane. The lines are then added together to produce a frame. The frames are repeated to produce a real-time image. The brightness of the image depends upon the amplitude of the returning echo from the anatomical interfaces. The position is dependent on the round-trip time of the pulse which in turn is determined by the density and therefore velocity of the medium under examination.
INTERACTION OF ULTRASOUND WITH TISSUES
Focus and Resolution
Axial resolution relates to the distance between two points in the path-line of the beam. If two points are close together and in the same line of the beam, the scanner relies on the different times of echo delay to distinguish the distance between them. The ability to separate two points, or axial delay, depends on pulse duration (PD)
PD = N τ
N = number of cycles in the pulse
τ= duration of each wave or the wave period = 1/ frequency
This equation shows that the higher the ultrasound frequency, the lower the pulse duration which leads to better axial resolution. A lower frequency increases the possibility that two close points in the line of a beam will not be seen as separate points. The frequency of ultrasound pulses must be carefully selected to provide a proper balance between image detail and depth of penetration. Ultrasound waves penetrate tissues to different depths based on probe frequency. Higher frequency probes, which emit waves at a frequency between 5 and 13 MHz, provide images with greater resolution but do not penetrate deeply into tissue. Lower frequency probes, with frequencies between 2 and 5 MHz, can penetrate tissue deeply ( up to 30 cm depth ), but the resolution is far less than that of the high frequency probes.
Images produced by ultrasound machines depend on both the density of the tissue being visualised and its ability to reflect ultrasound waves back to the transducer. These properties are referred to as the echogenicity of the tissue.Hyperechoic structures are those with greater propensity to reflect ultrasound energy, and hypoechoic structures tend to absorb this energy. Hyperechoic structures such as bone, vascular walls and other connective tissues, therefore appear brighter on the screen, and hypoechoic structures such as blood vessel lumens, other fluid filled structures and lung tissue, appear darker. The term acoustic impedance refers to the reduction in ultrasound wave energy that occurs as the wave passes through structures andaccounts for the depth limits that ultrasound can penetrate tissues.
In order to create a clear image of all the tissue detail from the reflected ultrasound, the beam needs to be adjusted to focus at the same depth as the points under investigation. In addition there also needs to good lateral and axial resolution.
There are three zones in an ultrasound beam. In the first zone the beam narrows and in the third it starts widening out again. The middle zone, where the beam is at its narrowest, is called the focal zone, and the depth of the tissue under examination should ideally be in this zone for optimum focus.See Figure 2.
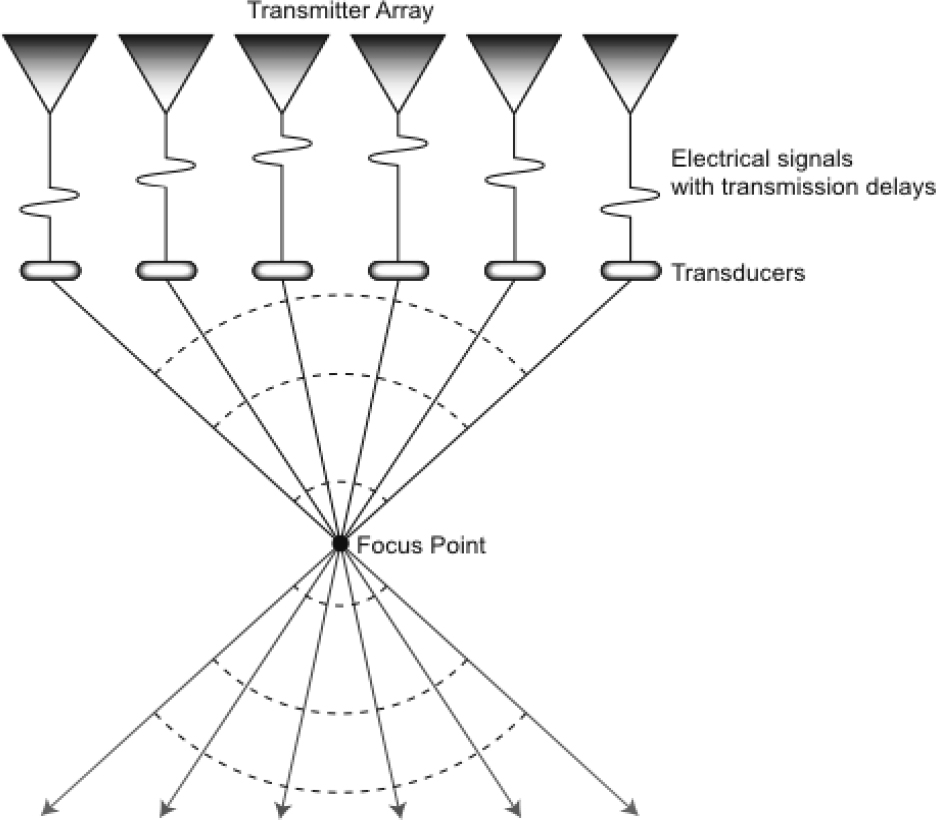
Figure 2: Electronic beam focusing by the staggering of transmission times from outer to inner elements
In the far zone, resolution is reduced and it becomes more difficult to distinguish between two points that are close together and at right angles to the beam. This is referred to as lateral resolution and such objects are more likely to appear as a single point if they are not focussed in the narrow zone of the ultrasound beam. See Figure 3.
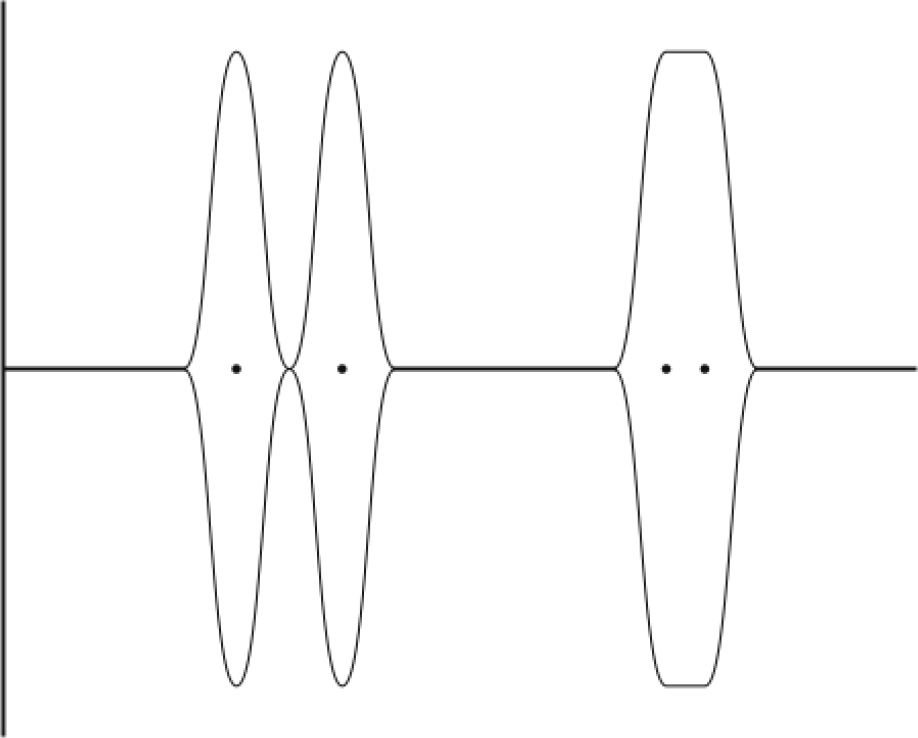
Figure 3: When the distance between two features approaches the pulse length of the received ultrasound wave they fuse into one thicker feature.
Reflection and Acoustic Impedance
Ultrasound images are created by reflection of the ultrasound beam at the interface between two tissue boundaries or media. The amount of ultrasound reflected depends upon the relative changes in the acoustic impedance (resistance at the interface) between the two media or tissues.
Acoustic impedance (Z) is dependant upon tissue density (ρ) and the propagation of speed through the tissue or medium (c) this is represented by the following equation:
Z = ρ c
A medium with high acoustic impedance is a good reflector of sound. If the acoustic impedance happens to be the same between two media, all the ultrasound will be transmitted without reflection, but when there is a difference, some will be reflected and the rest transmitted.
A measure of the amount of ultrasound which will be reflected at the interface is given by the ratio of the reflected to the incident intensity which is known as the Reflection Coefficient (R)
R = (Z 2 – Z 1 / Z2 + Z1 )2
Z1 = acoustic impedance for the first tissue
Z2 = acoustic impedance for the second tissue
Large differences in acoustic impedance are found at bone/soft tissue as well as at air/soft tissue interfaces leading to very high reflection coefficients at these sites and virtually 100% of the sound waves are reflected. Because of the high reflection bone cortex has for ultrasound, it appears white on the screen. Fluid, on the other hand, transmits sound waves and appears black. Due to the poor transmission of ultrasound energy through air, gel is used as a coupling agent for transmission of the ultrasound waves at the transducer/skin interface.
Contrast
If two materials have similar echo intensities, the lack of contrast resolution can make distinguishing the two materials from each other difficult. This can be overcome by adjusting the scanner settings and identifying characteristic tissue structures to assist in differentiating between the two materials.
Attenuation
The echo energy reflected from deeper structures will be weaker than that reflected from more superficial ones. This happens because the deeper the signal travels, the more energy is lost to absorption and scatter. This can make deeper structures appear a different grey image quality compared to other structures when in fact they are the same. Time gain compensation is used to overcome this problem.
Refraction
When ultrasound travels through different mediums, its change in velocity can alter its direction to one different from its propagation course. It is important to note that refraction of the ultrasound beam is determined by changes in velocity and not to differences in acoustic impedance. The degree of bending the sound wave undergoes as it travels through media of different velocities is dictated by Snell’s Law:
![]()
- sin θi = incident angle
- sin θt = transmit angle
- Сi = propagation of sound in the incident medium
- Сt = propagation speed in the transmitted medium
Refraction of ultrasound beams can produce artefacts whereby returning echoes are located incorrectly.
Diffraction
This term refers to the spreading out of a beam as it moves farther from the ultrasound source and its power intensity is weakened as it spreads over a larger area.
Scattering
Ultrasound beams striking an object at right angles are reflected directly back and most of the energy is lost to surrounding tissues. Scatter is a common occurrence and alters the echo image that comes from within an organ. Regions of increased scatter compared to adjacent tissues are hyperechoic and appear whiter. The reverse is true for hypoechoic appearances.
Rayleigh scatterers are special reflectors that reflect ultrasound energy concentrically, that is equally in all directions Red blood cells are an example of Rayleigh scatterers and scattering of ultrasound when these cells move in blood forms the basis for Doppler echocardiography.
Speckle
This refers to the grainy appearance to tissues on an ultrasound image. Speckle is not an anatomical feature, but a form of “visual noise” (artefact) and arises due to scattered wave returning at different velocities. It has the advantage of being able to distinguish homogenous structures from fluid filled spaces that are devoid of scattering centres. The appearance of speckles depends on the nature of the tissue and its depth.
SCANNING MODES
A-mode (amplitude mode)
This displays a single echo signal against time to measure depth. It is still used to determine dimensions of the eye.
B-mode (brightness mode)
This is the most commonly used image modality. It is a 2D image using multiple beam positions and a series of reflected echoes, producing a black and white image that is similar to an anatomical slice.
M-mode (motion mode)
This is a specialized case of B-mode imaging where one particular line (known as the m-line) is ensonified repeatedly to examine a moving structure (e.g. a heart valve), plotting out how the structure moves with time.See Figure 4.
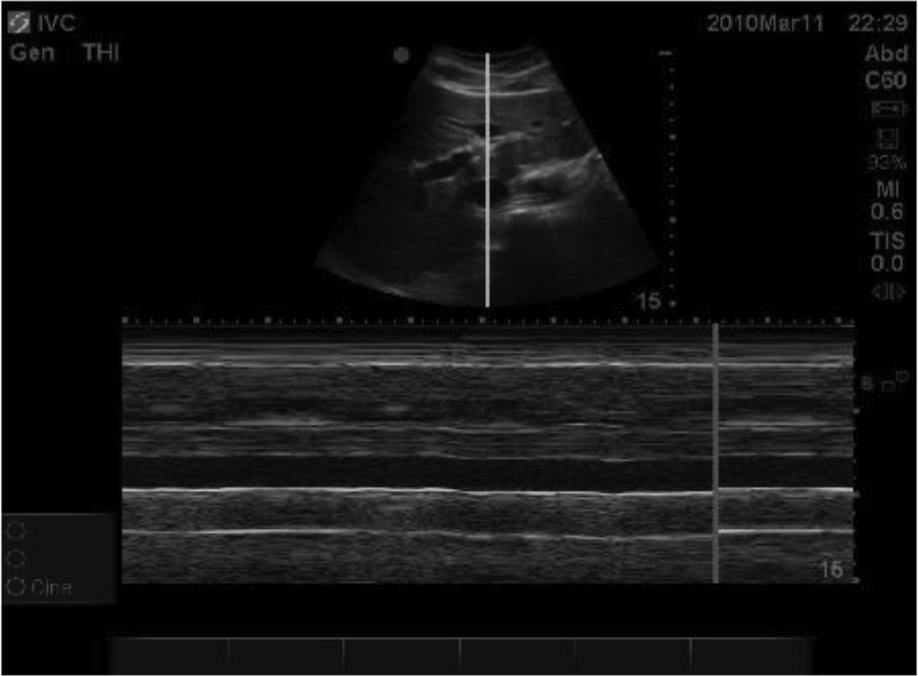
Figure 4: M Mode Ultrasound showing Inferior Vena Cava Cross-Section
PRACTICAL APPLICATION OF THE PHYSICAL PRINCIPLES
The ultrasound controls
Modern ultrasound devices are equipped with a number of adjustable controls in order to allow the user optimize the images they produce. It is important for the user to be familiar with their own machine and how to optimize the image before using ultrasound to guide peripheral nerve blocks. Some of the most commonly used controls are explained below:
Gain – This affects the brightness of the image by amplifying the overall received signal. It may be useful to increase the overall gain when scanning in a bright room or if the images on the screen appear too dark. It can be compared to turning up a dimmer switch in a light.See Figure 5.
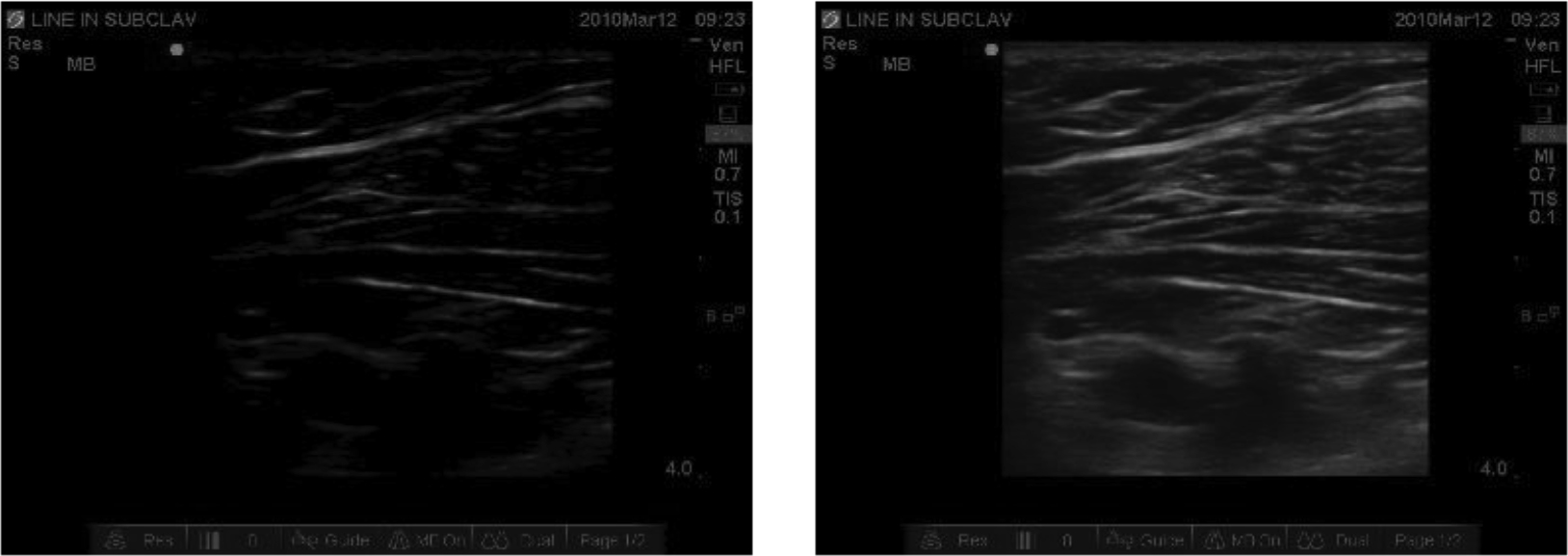
Figure 5: The Effect on Images of Gain Increase
Time-Gain Compensation (TGC) – Due to attenuation, weaker signals are received from structures that lie deep and stronger signals from those that are superficial, even though these structures may have the same physical properties. TGC differentially amplifies signals from different depths, allowing equal amplitudes from all depths to be displayed.
Focus –This adjusts the beam to be at its narrowest at the required depth to image the region of interest. It thereby improves lateral resolution.
Frequency – For superficial work a higher frequency will ensure better axial resolution. A lower frequency will allow much deeper penetration at the expense of poorer axial resolution.
Depth – The depth can be adjusted. It is best to have the structure that is being examined/targeted to be in the centre of the screen.
SUMMARY
- Ultrasound is sound with a frequency above 20 kHz
- The physical properties of sound waves (wavelength, frequency, velocity) dictate the limits of clinical ultrasound
- Ultrasound is generated using piezo-electrical materials.
- The image created is dependent on the physical properties of the tissue being examined.
- Having a good understanding of the physics of ultrasound allows the operator to manipulate machine settings to produce the optimal image.
ANSWERS TO QUESTIONS
- Regarding the properties of sound waves, which of the following statements is correct?
- False– Wavelength is the distance over which a wave‟s shape repeats.
- False– The speed of a sound wave is determined by the physical properties of the medium through which it passes.
- True– Frequency is inversely related to wavelength.
- False– Frequency is inversely related to the period.
- False– The SI unit of frequency is the hertz (Hz).
- When considering clinical ultrasound, which of the following statements are correct?
- True– Clinical ultrasound uses sound waves in the frequency range 1 – 20 MHz.
- True– The average velocity of clinical ultrasound through the soft tissues of the body is 1540 m/s
- True– B-mode is the most commonly used image modality.
- False– Piezo-electrical materials produce an electrical charge when pressure is applied to them.
- True– The Doppler effect refers to the change in frequency for an observer moving relative to the source of the sound wave.
- The difference in acoustic impedance at the air/soft tissue interface is?
- True– Large
- False– Small
- False– Smaller than the muscle/liver interface
- False– Smaller than the blood/water interface
- False– Is not detectable



