Obstetrics Anaesthesia
A series of three tutorials exploring the management of caesarean section.
- Part 1: Introduction and Overview
- Part 2: Caesarean Section under Regional Anaesthesia
- Part 3: Caesarean Section under General Anaesthesia
SELF ASSESSMENT: MCQ’S
T/F
Q1: Regarding the physiological changes of pregnancy:
- Cardiovascular changes do not occur until the second trimester?
- Cardiac output (CO) can increase as much as 50% at term from the pre-pregnant state?
- Functional Residual Capacity (FRC) decreases to 80% of its pre-pregnant level at term?
- Oxygen consumption is increased by 10% compared with pre-pregnant state?
- Glomerular Filtration Rate (GFR) decreases during pregnancy?
Q2: Regarding endotracheal intubation for caesarean section:
- The incidence of difficult intubation is twice that of the general surgical population?
- Under no circumstances should anaesthesia continue after a failed intubation as the mother will be put at an unacceptable risk?
- Cricoid pressure although reducing risk of passive regurgitation may make larnygoscopic view worse?
- In the term pregnant patient undergoing GA for caesarean section, desaturation is likely to occur faster following induction compared with a non-pregnant patient?
- The majority of cases of failed intubations have a high morbidity and mortality?
Q3: The following are methods of reducing acid aspiration syndrome (Mendelson’s)?
- Cricoid pressure?
- Perioperative H2 antagonists?
- Nil by mouth prior to caesarean section?
- Oral administration of Sodium Citrate?
- Head up tilt on operating table during induction of anaesthesia?
Q4: Concerning agents used at induction of general anaesthesia for caesarean section:
- a) Propofol is the commonest agent used in obstetric practice in the UK?
- b) Ketamine is useful in obstetric practice because of its analgesic properties and definite endpoint of induction of anaesthesia?
- c) Neuromuscular blocking drugs other than suxamethonium are not used because they are able to cross the placenta and produce apnoea in the newborn baby?
- d) If a second dose of suxamethonium is required a tachycardia should be anticipated?
- e) Etomidate has the advantage of maintaining cardiovascular stability to a greater extent than thiopentone during induction of anaesthesia?
KEY POINTS
- General anaesthesia in the obstetric patient is associated with an increased risk of morbidity and mortality including airway difficulties and failed intubation.
- Maternal mortality as a direct result of anaesthesia has fallen as more caesareans are performed under regional anaesthesia. As a consequence of this trend, trainee anaesthetists are now more limited in their exposure to general anaesthesia for caesarean section.
CONSIDERATIONS
There are significant challenges associated with general anaesthesia (GA) in the pregnant woman.
- Changes in maternal physiology and anatomy present their own challenges but can also exacerbate pre-existing medical problems.
- Specific conditions such as pre-eclampsia and massive maternal haemorrhage significantly increase the risks of GA.
- GA in the obstetric population is often performed in a stressful and pressured emergency situation.
- As the proportion of caesareans performed under GA has fallen, anaesthetic trainees are less experienced in managing this challenging situation.
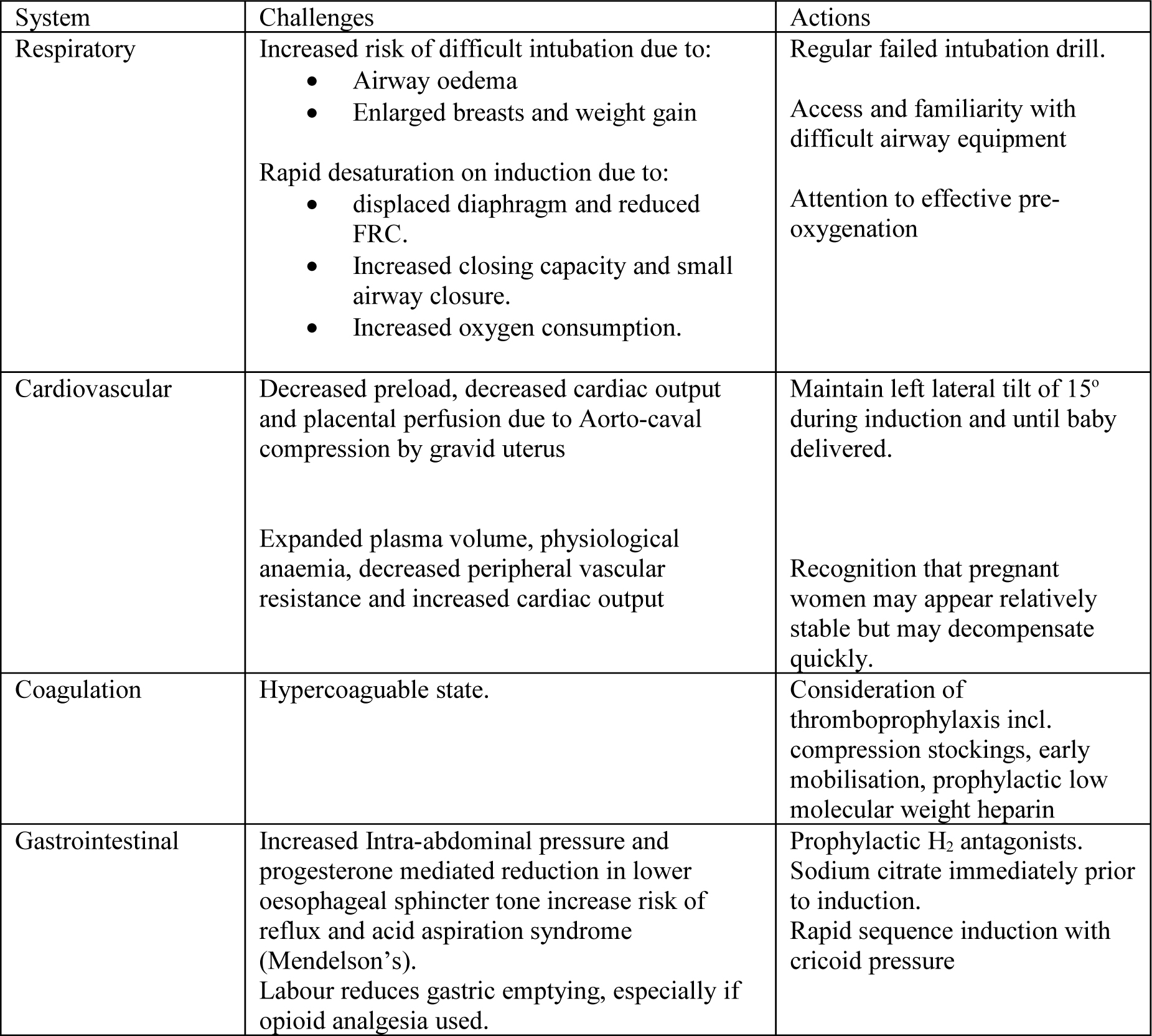
The physiological changes of pregnancy which contribute to the challenges of general anaesthesia are considered below:
Over 80% of caesarean sections in the UK are now performed under neuraxial anaesthesia. General anaesthesia is indicated if the woman refuses a regional technique, if there is a specific medical condition which precludes neuraxial blockade (e.g. coagulopathy) or when it is felt there is not enough time available to provide a regional anaesthetic.
Induction time to delivery is important as it dictates the amount of volatile anaesthetic agent that transfers to the neonate. Uterine incision to delivery is important as placental blood flow may be disrupted by uterine incision and if prolonged may increase the risk of fetal acidosis.
THE GENERAL ANAESTHETIC
Antacid prophylaxis
Pregnant women are at risk of acid regurgitation and aspiration (Mendelson’s syndrome) and measures to prevent this are essential.
Lower oesophageal sphincter tone is reduced by progesterone and the intra-gastric pressure of the pregnant anaesthetised and ventilated patient is twice that of the non-pregnant patient. The risk of developing acid aspiration is related to the pH and volume of aspirate and measures to modulate these and reduce risk include:
- Restricting oral intake, especially solids for women in labour. Nil by mouth for those women considered likely to require GA
- Use of prokinetics (e.g. metoclopramide 10 mg I.V)
- Use of H2 antagonists (e.g. Ranitidine 150mg p.o if time permits or 50mg I.V prior to an emergency)
- Sodium citrate (30ml) p.o just prior to induction
Antacid prophylaxis should be considered in all patients undergoing caesarean section as a caesarean under neuraxial anaesthesia may require conversion to GA.
Large Bore Intravenous Access
Ideally at least one reliable 16G cannula for rapid fluid resuscitation if required.
Preoxygenation
The upward displacement of the diaphragm due to increased intra-abdominal pressure reduces functional residual capacity (FRC) by up to 20%. The closing capacity encroaches on the FRC resulting in closure of the dependent airways. This combined with increased oxygen consumption, leads to rapid desaturation. Attention to pre-oxygenation is essential with 3-5 minutes of tidal breathing or 5 vital capacity breaths of high flow oxygen via a tight fighting face mask.
Cricoid Pressure
A manoeuvre to reduce passive regurgitation. The optimum recommended force is 10N whilst awake increasing to 30N on induction. When applying cricoid pressure to the pregnant woman it should be recognised that the patient is tilted to the left and the direction of force should be adjusted accordingly. Incorrectly applied cricoid pressure can distort the view at laryngoscopy and increase the risk of difficult intubation.
Rapid Sequence Induction
Rapid sequence induction is recommended for all cases of general anaesthesia for caesarean section.
The agents used most frequently in the UK are thiopentone 3-5mg/kg and suxamethonium 1-1.5mg/kg.
Confirmation of tracheal intubation is essential as maternal deaths still occur from unidentified oesophageal intubation. Correct endotracheal tube placement can be confirmed in the following ways:
- Clinical
- Visualising the endotracheal tube passing through the cords
- Misting of the tube during ventilation
- Observation and auscultation of bilateral chest expansion and absence of sound over the stomach
- Capnography
- Confirmation of expired CO2 with capnography is the gold standard and appropriate equipment should be available.
Alternative agents and methods of induction
There is controversy over the best choice of anaesthetic agents to most effectively and safely secure the airway in the obstetric patient. The ‘traditional’ approach of cricoid pressure, thiopentone, suxamethonium and avoidance of opioids is common in the UK; however the emergence of new agents and techniques may challenge this accepted technique in the future.
Choice of Induction Agent
Thiopentone
There is vast experience with the use of thiopentone in this setting and it is currently the induction agent of choice for caesarean section under GA. A dose of 4 mg/kg has been suggested to balance avoidance of maternal awareness and hypertension and prevent delayed waking in the event of a failed intubation.
Propofol
Propofol is the most likely alternative to thiopentone and has been used for caesarean section under GA. One study demonstrated more maternal hypotension, possibly increased risk of maternal awareness and lower Apgar scores when compared with thiopentone. Other studies have shown no difference. No studies have shown superiority of propofol over thiopentone.
Ketamine
There is less experience of ketamine compared with thiopentone and propofol in the UK. A dose of 1.5-2mg/kg should be used. It may be indicated in the hypovolaemic obstetric patient.
Etomidate
The use of etomidate is decreasing in the UK as a result of its deleterious effect on adrenal function.
Inhalational Induction
Inhalational induction for caesarean section is uncommon in the UK because of the risk of aspiration and the increased risk of uterine atony and haemorrhage due to uterine muscle relaxation caused by volatile agents.
Neuromuscular Blockade
Depolarising (Suxamethonium)
Suxamethonium is currently the muscle relaxant of choice due to its fast onset and rapid offset which is important in the event of a failed intubation. The use of total rather than lean weight is recommended for calculation of the required dose. Psuedocholinesterase activity is decreased during pregnancy and a dose of 1-1.5mg/kg is recommended.
There are inherent risks with suxamethonium:
- Anaphylaxis
- Post-operative myalgia
- Hyperkalaemia
- Malignant hyperpyrexia
- Prolonged muscle relaxation in individuals with plasma cholinesterase deficiency.
- Bradycardia with repeated doses of suxamethonium without administration of atropine.
Serious reaction rate is of the order of 1:4000.
Non-Depolarising (Rocuronium)
Rocuronium (an aminosteroid) is becoming increasingly popular among obstetric anaesthetists to provide muscle relaxation for caesarean section under GA. Rocuronium produces equivalent intubating conditions to suxamethonium but the onset of block may be slower. It has notably fewer side effects than suxamethonium but in the event of a failed intubation, a prolonged period of face mask ventilation will be required.
Sugammadex is a new drug that specifically and permanently reverses the neuromuscular block produced by rocuronium. The arrival of this drug on the market may result in a significant reduction in the use of suxamethonium for general anaesthesia for caesarean section
Opioids
Although not routinely used at induction because of fears of neonatal respiratory depression, short acting opioids have a place in general anaesthesia for patients with hypertensive disorders, primarily pre-eclampsia, to reduce the risk of cerebral complications from the pressor response of laryngoscopy.
Paediatricians should be in attendance at all caesarean sections under general anaesthesia and should be informed of the risk of potential neonatal respiratory depression due to pre-delivery maternal administration of opioids.
Failed Intubation
Concerns have been raised about the reduction in exposure of anaesthetists to emergency general anaesthesia in obstetrics. The incidence of failed obstetric intubation is reported at 1:250, 8 times higher than for the general surgical population. This is equivalent to 180 cases in the UK each year and up to 9% of these cases may be associated with failure to ventilate. The risk of failed intubation is greater at emergency compared with elective caesarean section under GA. When failed intubation occurs it is often unexpected and the increased maternal oxygen demand and decreased FRC lead to rapid desaturation. Fortunately, the majority of failed intubations do not result in adverse maternal outcome.
It is essential to thoroughly assess the airway prior to caesarean section, even if regional anaesthesia is planned.
Obstetric anaesthetists should be familiar with and undergo regular training in failed intubation drills. Difficult intubation equipment, with a variety of airway devices and a method of cricothyroid puncture and ventilation should be available at all times. Attention to how the patient is positioned is paramount to provide the best possible intubating conditions at the first attempt. Because clinical opportunities for training are limited, a simulator is a good environment to undergo training in failed intubation and management of other obstetric emergencies.
Example of a difficult intubation drill:
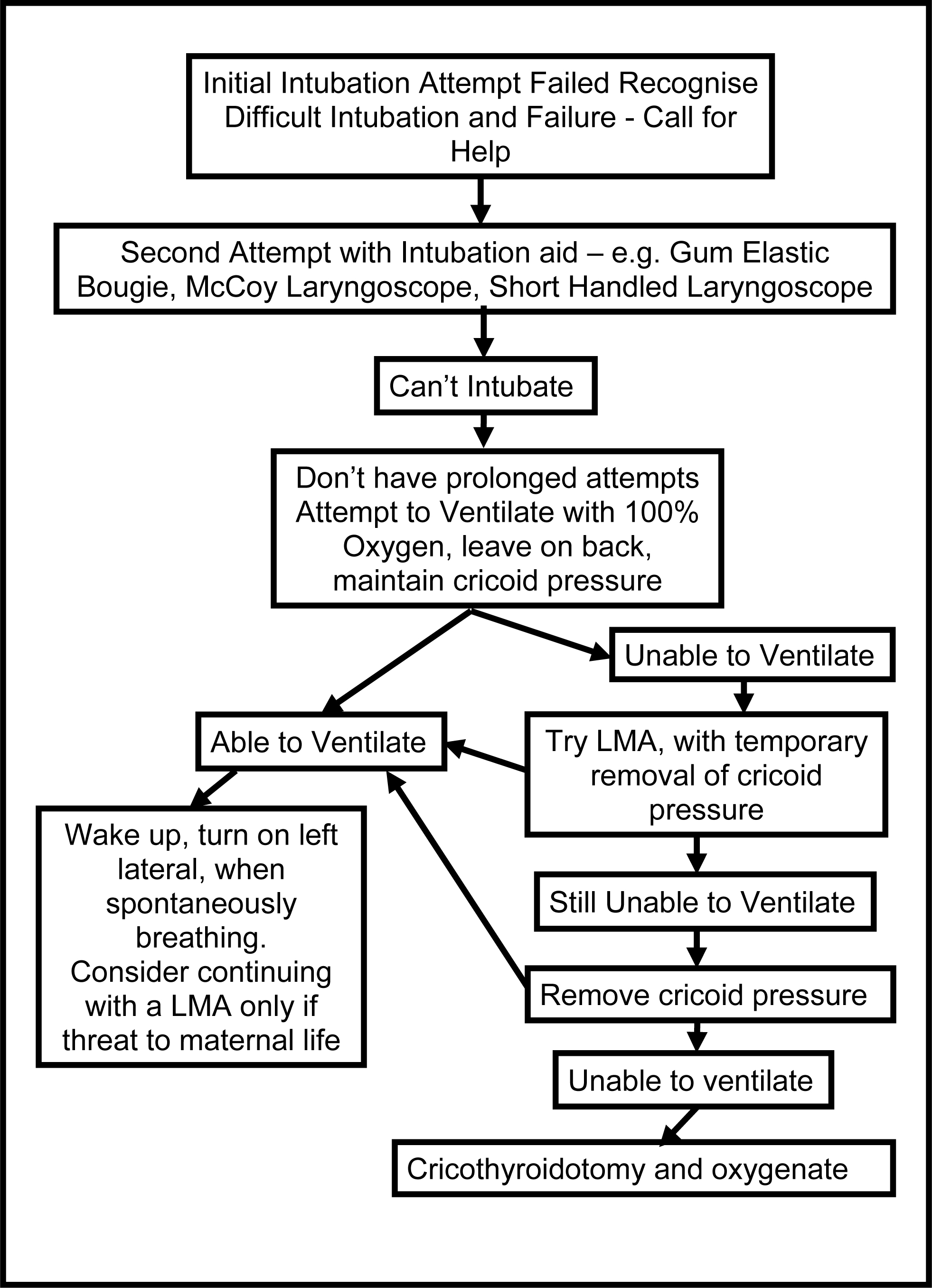
In the event of a difficult intubation patients should be counselled to inform future anaesthetists of potential airway difficulties. A clear warning sticker should be placed on the notes and the general practitioner informed.
If difficult intubation is anticipated and neuraxial anaesthesia is contraindicated then awake fibre optic intubation may be indicated. The nasal route for intubation is less favourable in obstetric patients because of engorgement of the nasal mucosa and higher risk of bleeding. The technique is more difficult to perform in an emergency situation.
Laryngeal Mask Airway
The laryngeal mask airway (LMA) is a very useful device in the event of a failed intubation with subsequent difficult facemask ventilation. The Proseal LMA offers potential advantages as it provides a tighter seal against the glottis and has an oesophageal drain tube which may reduce aspiration risk in the event of regurgitation. Practice and familiarity at insertion are required prior to its use in an emergency.
Extubation
The risks of extubation are often overlooked but it is associated with airway difficulties, including upper airway obstruction, laryngospasm and aspiration. The left lateral position is recommended prior to extubation to allow passive drainage of secretions and stomach contents in the event of regurgitation. The patient should be adequately awake and muscle relaxation reversed to allow return of airway reflexes. In cases considered high risk for aspiration, drainage of gastric contents via a nasogastric tube before extubation may be advisable.
Depth of Anaesthesia Monitoring
Although anaesthetic requirements are reduced in pregnancy, general anaesthesia for obstetric patients is associated with a higher incidence of awareness compared with the general population. This is probably due to reduced administration of volatile agent at caesarean section due to concerns that excessive concentrations may be detrimental to the fetus and may relax uterine muscle increasing the risk of haemorrhage. Concerns about awareness have led to consideration of depth of anaesthesia monitoring for this patient group. There are several commercially available devices, most based on technology that processes EEG waves and presents them in a readily interpretable manner e.g. Bispectral Index (BIS) monitoring. Although depth of anaesthesia monitoring in caesarean section is not routinely practiced in the UK, its use may potentially increase in the future.
Conclusion
General anaesthesia for caesarean section in the emergency setting is stressful and demands clear communication and situational management (patient partners, midwives, obstetricians) as well as an organised anaesthetic plan.
With the increasing caesarean section rate in the developed world it is likely that the absolute number of complications from obstetric surgery and anaesthesia will increase. Best practice must be constantly debated, adopted and audited to reduce morbidity and mortality.
The issues and advances above are relevant to obstetric anaesthesia throughout the world though clearly, limitations in availability of equipment and resources may preclude their implementation. Africa accounts for 47% of global maternal mortality; this can be reduced with systematic improvement in education, training, funding and resources.
Self Assessment: Answers / Discussion
A1: Physiology of Pregnancy
- a) F – Cardiovascular changes start to occur as early as 4/40. They are mediated by the hormonal effects of progesterone and oestrogen released initially by the ovary for the first trimester and subsequently the placenta.
- b) T – Heart rate and stroke volume are increased by up to 25% each. The left ventricle is mildly dilated and hypertrophied in response to the increased demand. CO can be increased a further 30% during labour.
- c) T – The increased intra-abdominal pressure and diaphragmatic displacement by the gravid uterus decreases FRC by up to 20%. The closing capacity will encroach on the FRC in approximately 50% of pregnant women in the 3rd trimester, leading to small airway collapse.
- d) F – Oxygen consumption is increased by 40% compared with pre-pregnancy levels.
- e) F – GFR is increased by 50% during pregnancy which may have implications for drug elimination. Renal blood flow is also increased.
A2: Concerning intubation of the pregnant patient
- a) F – The incidence is up to 8 times higher than in the general population. It is more common in the emergency situation. It is probably due to a combination of factors including anatomical changes such as weight gain and upper airway oedema which increase the Mallampati score and make intubation technically more difficult. Other factors including the decrease in exposure of anaesthetic trainees to general anaesthesia for caesarean section are also important.
- b) F – In cases where the mother’s life is at risk, anaesthesia can be continued. The anaesthetist’s primary duty of care is to the mother and this must be considered in deciding whether to continue with anaesthesia for caesarean section in the event of a failed intubation.
- c) T – Cricoid pressure is an important manoeuvre to reduce passive regurgitation and risk of acid aspiration in the term mother. If incorrectly applied it can obscure the view at laryngoscopy. The commonest reason for this is over zealous pressure in a stressful situation. With the patient placed in the left tilted position the application of force of the cricoid pressure needs to be carefully considered and observed. In the event of failed intubation, cricoid pressure will need to be reduced if an LMA is inserted and may need to be released if face mask ventilation is impossible.
- d) T – The combination of a decreased functional residual capacity secondary to increased intra- abdominal pressure and an increased oxygen consumption conspire to make the term parturient desaturate rapidly. For this reason it is important to preoxygenate effectively, recognise a failed intubation early and call for help immediately
- e) F – Only a small proportion of failed intubations come to harm. It is possible to safely ventilate the majority of women, the priority being to wake them up safely and consider an alternative regime for securing the airway.
A3: The following are methods of reducing acid aspiration syndrome (Mendelson’s)?
- a) T- Cricoid pressure may prevent passive regurgitation.
- b) T- Ideally H2 antagonists should be given prior to caesarean section but this is not always possible in the emergency situation. There is some value to giving them intraoperatively as it may reduce the possibility and impact of aspiration at extubation.
- c) T- This is feasible for the elective caesarean section and it is possible to identify some high risk pregnancies on the labour ward that will require a caesarean section. In cases of failure to progress it may be more challenging. These patients, by definition, have often been labouring for a long time and require rehydration and calories. The only patients to die in Mendelson’s original series were those who had complete airway obstruction from solid matter. A recommendation for these patients would be to use isotonic high calorie sports drinks instead of solid foods.
- d) T- This alkali raises the pH of stomach contents and should be given immediately prior to induction of anaesthesia. H2 antagonists will suppress subsequent acid production but will not treat acid already present in the stomach.
- e) T – Head up tilt on the table has been suggested as an alternative, or in addition to, cricoid pressure in reducing passive regurgitation. It may also improve respiratory dynamics for preoxygenation. However if the patient vomits it theoretically increases the chances of aspiration from the effects of gravity, rather than particulate matter draining from the mouth.
A4: Concerning agents used at induction of general anaesthesia for caesarean section
- a) F – Although gaining popularity as an induction agent for rapid sequence induction in the non- obstetric patient, most obstetric anaesthetists in the UK still use thiopentone for induction.
- b) F – Ketamine is rarely used in UK obstetric practice but should be considered for a shocked patient with massive haemorrhage requiring caesarean section under GA.
- c) F – Placental transfer of a drug is reliant on its molecular weight, lipid solubility and the extent of ionisation and protein binding in the maternal circulation. Non-depolarising muscle relaxants are large, highly ionised molecules that do not readily cross the placenta. Suxamethonium is commonly used at induction due to its rapid onset of action. It also has the advantage of wearing off quickly in the event of failed intubation, allowing return of spontaneous breathing.
- d) F – If a second dose of suxamethonium is given a bradycardia should be anticipated and may be prevented by pre-emptive administration of atropine. In the event of a failed intubation following muscle relaxation with suxamethonium, it is safer to wake the patient up rather than continue further attempts at intubation. Repeated doses of suxamethonium are therefore not recommended.
- e) T – This is the main advantage of etomidate. It has fallen out of favour in UK practice because of concerns that even a single dose can significantly inhibit corticosteroid production.
Recommended reading
- Yentis S, May A, Alhotra S. Analgesia, anaesthesia and pregnancy. A Practical Guide. Cambridge University Press. 2007
- Levy DM. Emergency Caesarean Section: Best Practice. Anaesthesia. 2006; 61: 786-791
- Confidential Enquiry into Maternal and Child Health http://www.cemach.org.uk/
- Royal College of Obstetricians and Gynaecologists’ Clinical Effectiveness Support Unit. The National Sentinel Caesarean Section Audit Report. London RCOG, 2001 http://www.rcog.org.uk/resources/public/pdf/nscs_audit.pdf
- NICE guidelines for caesarean section http://www.nice.org.uk/guidance/index.jsp?action=download&o=29331
For fully referenced version of tutorial please contact author via email: jprb_brum@yahoo.com



