General Topics
QUESTIONS
Before continuing, try to answer the following questions. The answers can be found at the end of the article, together with an explanation.
- The intraocular pressure is increased by
- Methohexitone
- Suxamethonium
- Ecothiopate
- Atracurium
- Acetazolomide
- Contraindications to local anaesthesia for eye surgery include
- Glaucoma
- Inability to lie flat
- Procedures that last more than 90 minutes
- Penetrating eye injury
- Retinal detachment
- The following drugs decrease intraocular pressure
- Enflurane
- Nitrous oxide
- Etomidate
- Ketamine
- Suxamethonium
- The oculocardiac reflex
- Occurs on traction of the medial rectus
- Does not occur with retrobulbar block
- May be obtunded by local anaesthetic infiltration of ocular muscles
- Is most active in the elderly
- Precipitates non-sinus dysrhythmias
- The following will raise the intraocular pressure in the normal eye
- Hypercarbia
- Acetazolomide
- Atropine
- Hypotension
- Respiratory obstruction
Ophthalmic surgery can be performed under either regional or general anaesthesia. Part I describes the relevant anatomy and physiology for the anaesthetist before discussing regional anaesthetic techniques. Part II will focus on general anaesthesia for eye surgery.
Please also refer to the other relevant TOTW article Sub-Tenon’s Anaesthesia for Ophthalmic Procedures (Discussion of this technique will not be repeated here)
Anatomy
Some basic knowledge of the anatomy of the orbit and its contents is necessary for the successful performance of regional anaesthesia for ophthalmic surgery. If possible carefully examine the orbit in a skull whilst reading this article. This will make understanding the techniques described easier.
Each orbit is in the shape of an irregular pyramid with its base at the front of the skull and its axis pointing postereo-medially towards the apex. At the apex lies the optic foramen, transmitting the optic nerve and accompanying vessels and the superior and inferior orbital fissures transmitting the other nerves and vessels.
The orbit measures 40-50mm deep with a volume of approximately 30ml, 7ml of which is occupied by the globe and its muscular cone with the remainder composed of loose connective tissue. The axial length of the globe is the distance from the corneal surface to the retina and in adults measures roughly 25mm (range 12-35mm) and is often measured preoperatively. As the eye becomes more elongated, as in high myopes, the sclera becomes thinned and staphylomata or outpouchings of it can occur. This increases the risk of perforation of the globe especially for peribulbar or retrobulbar approaches. Care should be taken for axial lengths >26mm and a sub-Tenon or GA technique considered. It is important to note that a sub-Tenon approach still carries a small risk of globe perforation under these circumstances.
The angle between the lateral walls of the two orbits is approximately 90° (and the angle between the lateral and medial walls of each orbit is nearly 45° (Fig 1). Thus the medial walls of the orbit are almost parallel to the sagittal plane. (The sagittal plane passes directly from front to back of the body).
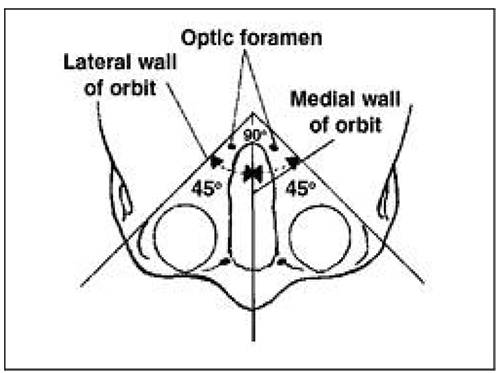
Figure 1
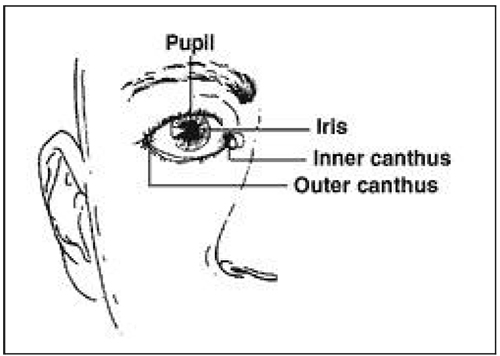
Figure 2
The orbit contains the globe, orbital fat, extraocular muscles, nerves, blood vessels and part of the lacrimal apparatus.
The globe (Figs 1&2): is situated in the anterior part of the orbital cavity closer to the roof than the floor and nearer the lateral than the medial wall. The sclera is the fibrous layer of the eyeball completely surrounding the globe except the cornea. It is relatively tough but can be pierced easily by needles. The optic nerve penetrates the sclera posteriorly 1-2 mm medial to, and above, the posterior pole. The central retinal artery and vein accompany the optic nerve. The cone refers to the cone shaped structure formed by the extraocular muscles of the eye.
The orbital fat is divided into central (retrobulbar/intraconal) and peripheral (peribulbar/periconal) compartments by the cone of the recti muscles. The central space contains the optic, oculomotor, abducens and nasociliary nerves. The peripheral space contains the trochlear, lacrimal, frontal and infraorbital nerves. All the motor and sensory nerves can be blocked by an injection into the orbital
fat.
The extraocular muscles: The intraconal space is bounded by the four rectus muscles, from the annulus of Zinn at the orbital apex, to their penetration through Tenon’s capsule before attaching to the globe. The combined actions of these four rectus and two oblique muscles on each eyeball allow elevation, depression, adduction and abduction. Under normal circumstances unmodified activity of one muscle is rare, but testing individual muscle function becomes necessary after local anaesthetic block to identify the unblocked nerve when some movement is still present.
Nerve supply to the eyes (Table 1)
The motor nerve supply to the extraocular muscles is easy to remember using the pseudoformula LR6(SO4)3 – lateral rectus by the sixth (abducens) cranial nerve, superior oblique by the fourth (trochlear) and the remainder by branches of the third (oculomotor) nerve.
The sensory supply is mainly from the ophthalmic division of the fifth (trigeminal) cranial nerve. The lacrimal branch innervates the conjunctiva and the nasociliary branch the cornea, sclera, iris and ciliary body. The second cranial nerve (optic) conveys vision.
The parasympathetic supply is from the Edinger-Westphal nucleus accompanying the third nerve to synapse with the short ciliary nerves in the ciliary ganglion. The sympathetic fibres are from T1 and synapse in the superior cervical ganglion before joining the long and short ciliary nerves.
Injection of local anaesthetic solution into the lateral adipose compartment from an inferotemporal needle insertion normally blocks the nasociliary, lacrimal, frontal, supraorbital and supratrochlear branches of the ophthalmic division of the trigeminal nerve and the infraorbital branch of the maxillary division.
Injection into the medial compartment through a needle placed between the caruncle and the medial canthal angle usually blocks the medial branches of the nasociliary nerve, the long ciliary nerves, the infratrochlear nerve and medial components of the supraorbital and supratrochlear nerves.
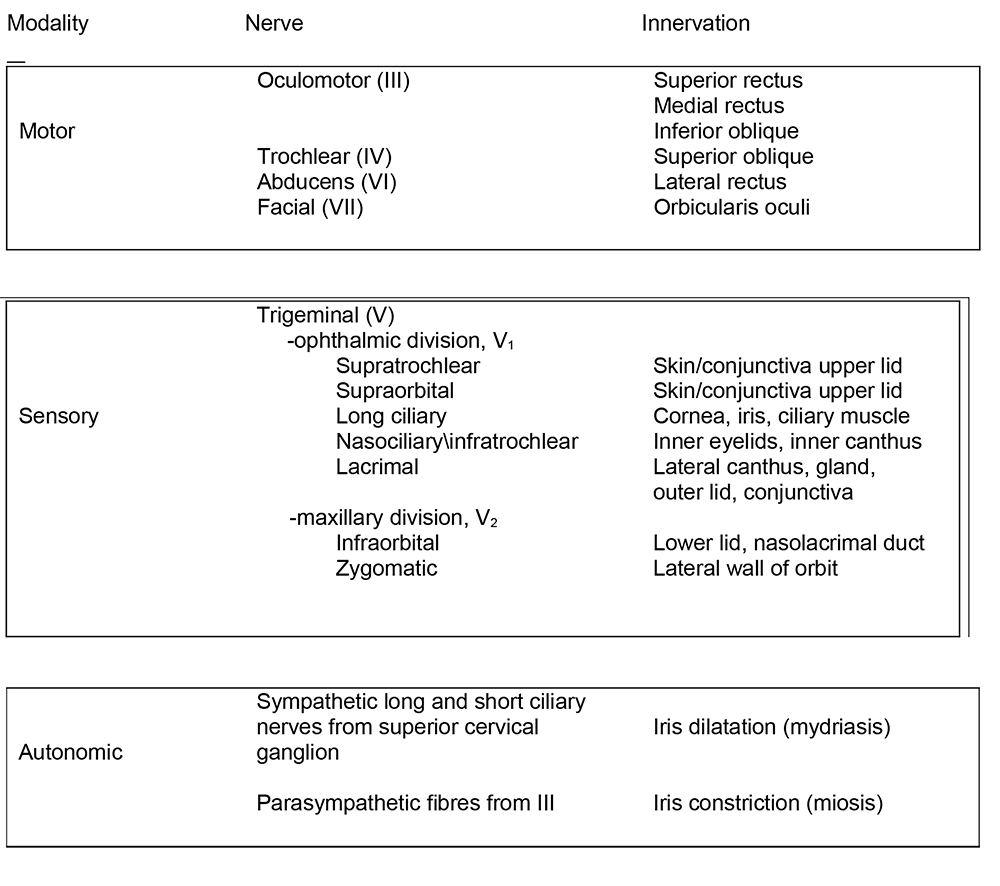
Table 1. Summary of nerve supply to orbit
Blood vessels: The main arterial supply to the globe and orbital contents is from the ophthalmic artery which is a branch of the internal carotid artery and passes into the orbit through the optic canal inferolateral to the optic nerve and within the meningeal sheath of that nerve. In the elderly and hypertensive patient it is tortuous and vulnerable to needle trauma when it may bleed profusely. Venous drainage is via the superior and inferior ophthalmic veins.
The lacrimal apparatus has orbital and palpebral components. The orbital part lies in the lacrimal fossa on the anterolateral aspect of the orbital roof, and the palpebral part is situated below the levator palpebrae superioris aponeurosis and extends into the upper eyelid secreting tear fluid into the superior conjunctival fornix.
Lacrimal drainage occurs through superior and inferior lacrimal puncta near the medial ends of both lid margins which form entrances to the 10mm long lacrimal canaliculi medially passing through the lacrimal fascia to enter the lacrimal sac. The nasolacrimal duct connects the inferior end of the lacrimal sac to the inferior meatus of the nose.
The anatomical features of the orbit described above permit the passage of needles into fibro-adipose compartments in the orbit avoiding close contact with the globe, major blood vessels, extraocular muscles and the lacrimal apparatus.
Physiology
Intraocular pressure – IOP
Defined as the tension exerted by the contents of the globe on the surrounding corneo-scleral envelope.
Normal range between 10-20 mmHg.
Increases with age.
Equal values between sexes in age groups 20-40.
Positive correlation between IOP and axial length.
Normal diurnal variation of 2-3 mmHg with higher pressures in the morning.
IOP may differ by up to 5 mmHg between eyes.
IOP changes from sitting to supine position from between 0.3-6 mmHg.
Transient rises in IOP are seen with coughing, straining and vomiting, but are of no consequence to the intact eye. Prolonged rises in IOP however, may cause progressive loss of vision.
Aqueous humour
This is a clear fluid that fills the anterior and posterior chambers of the eye. Its volume is about 250 μL and is produced at a rate of 2.5μL/min. Its composition is similar to that of plasma except for a much higher concentration of ascorbate, pyruvate and lactate and a lower of concentration of protein, urea and glucose.
IOP is a function of the rate at which aqueous humour enters the eye (inflow) and leaves it (outflow). When these flow rates are equal the IOP remains fairly constant. Inflow is related to the rate of aqueous humour production, whilst outflow depends on the resistance to flow of aqueous from the eye and the pressure in the episcleral veins.
The control of IOP is therefore a function of:
- production of aqueous humour
- resistance to aqueous outflow
- episcleral venous outflow
Factors affecting IOP
Arterial blood pressure – blood flow in the human eye remains constant over a range of perfusion pressures due to autoregulation of retinal and choroidal circulations. A fall in systemic blood will reduce IOP, but only becomes significant at pressures below 90 mmHg. A decrease in choroidal blood volume is thought to cause the reduction in IOP.
Venous pressure – coughing, straining, vomiting and Valsalva manoeuvre will cause venous congestion thereby increasing intraocular vessel volume and reducing episcleral venous drainage causing a rise in IOP. Head up tilt decreases venous congestion reducing IOP and vice versa.
Partial pressures of oxygen (pO2) and carbon dioxide (pCO2) affect intraocular tone and hence IOP. A rise in pCO2 secondary to any cause of hypoventilation and hypoxia results in dilation of the choroidal vessels and a rise in IOP, the converse is also true. Metabolic acidosis decreases IOP and metabolic alkalosis increases IOP.
Drugs – opioids, hypnotics, major tranquilisers and volatile agents are associated with a fall in IOP with the exception of ketamine which causes a rise. Depolarising muscle relaxants cause a small, transient, but consistent rise in IOP whilst non-depolarisers produce no change or a decrease in IOP. Other drugs which reduce IOP include mannitol (0.5mg/kg iv) which works by removing fluid from the vitreous and acetazolamide (500mg iv) which acts to decrease aqueous humour production by the ciliary body.
In summary, anaesthetic drugs may act via a number of ways to reduce IOP :
- a direct effect on the central diencephalic control centre
- reduction of aqueous humour production
- facilitation of aqueous drainage
- relaxation of extraocular muscle tone
Injection of local anaesthesia following a peribulbar or retrobulbar block will cause a definite, albeit variable, rise in IOP. This increase in pressure is transient and depends on the rate and volume of injection.
General anaesthesia and the physical intervention by the anaesthetist also affects IOP. Laryngoscopy and intubation causes a rise in IOP and to a lesser degree the insertion of a laryngeal mask airway. Any coughing or gagging during extubation also causes a rise in IOP.
Oculomedullary reflexes
Oculocardiac reflex – causes bradycardia, nodal rhythms, ectopic beats or sinus arrest due to pressure, torsion or traction on the extraocuar muscles. It is a trigemino-vagal reflex – the afferent arc is via long and short ciliary nerves to the ciliary ganglion and the ophthalmic division of the trigeminal nerve with the efferent impulses conveyed by the vagus.
This reflex most commonly occurs in paediatric squint patients. Local anaesthetic blocks may attenuate the afferent arc and muscarinic antagonists block the efferent limb at the level of the heart. Hypercarbia sensitises the reflex and should be avoided.
Oculorespiratory reflex – may cause shallow breathing, reduced respiratory rate and even full respiratory arrest. The afferent pathways are similar to the above reflex and it is thought that a connection exists between the trigeminal sensory nucleus and the pneumotactic centre in the pons and medullary respiratory centre. Again this reflex is commonly seen in strabismus surgery and atropine has no effect. If controlled ventilation is not routinely employed then extra attention is needed.
Oculoemetic reflex – is likely responsible for the high incidence of vomiting after squint surgery (60- 90%). Again this is a trigemino-vagal reflex with traction on the extraocular muscles stimulating the afferent arc. Whilst antiemetics may reduce the incidence, a regional block technique provides the best prophylaxis.
Types of regional anaesthesia for ophthalmic surgery:
- Sub-Tenon block
- Peribulbar block (Extra-conal block)
- Retrobulbar block (Intra-conal block)
The most popular technique for regional anaesthesia in eye surgery is now a sub-Tenon block. This has largely replaced peribulbar blocks and general anaesthesia for many types of eye surgery. Due to the relatively higher risks of retrobulbar blocks this technique is quickly becoming obsolete. Whilst the sub-Tenon approach is arguably safer still than the peribulbar block, the latter still has its place as a regional technique for those patients in whom a sub-Tenon block is relatively contraindicated.
These include patients with previous scleral banding and detachment surgery, medial rectus or pterygium surgery and care must also be taken in high myopes because of the occasional presence of staphylomata (outpouched areas) and/or scleral thinning.
If there is any doubt take advice from the surgeon.
No more discussion will be made on the sub-Tenon approach – please refer to the TOTW article entitled “Sub-Tenon’s Anaesthesia for Ophthalmic Procedures”
Preparation
- Best practice dictates an intravenous cannula is inserted to allow immediate venous access in case of emergency.
- The conjunctival sac is anaesthetised with proxymetacaine 0.5% or amethocaine 1%. Three drops are instilled and this is repeated 3 times at 1 minute intervals. For patient comfort these drops are best applied at the medial or lateral aspects of the eye rather than dropped directly onto the cornea.
- A 10ml syringe is prepared with the preferred local anaesthetic mixture. Popular choices include 2% lignocaine with or without adrenaline 1:200,000, however bupivacaine 0.5% can be added to prolong the analgesic and anaesthetic effects. Hyaluronidase 2-30 units/ml is usually added to this mixture to improve diffusion of the anaesthetic mixture within the orbit.
- A 25 gauge, 2.5 cm disposable needle is attached to the syringe.
- The patient lies supine and is asked to look directly up focussing on a fixed point on the ceiling, so that the eyes are in the neutral position.
Performance of the block
Whilst one injection will usually suffice it is possible to perform two, at separate sites, should a ‘top-up’ be required. These injections can be made either via a trans-conjunctival or trans-cutaneous route.
Infero-temporal injection (Figs 3-5)
The lower lid is retracted manually and the needle is placed halfway between the lateral canthus and the lateral limbus (edge of the iris). The injection is not painful as it is passing through an already anaesthetised conjunctiva. If there is not enough room for the needle to be positioned correctly then the injection may be made directly through the skin. Classically the point of needle insertion was made in line with the edge of the limbus, however more recently a point midway between here and the lateral canthus has been adopted. The needle is advanced in the sagittal plane, parallel to the orbital floor passing under the globe. There is no need to apply pressure to the syringe as it will easily advance without resistance.
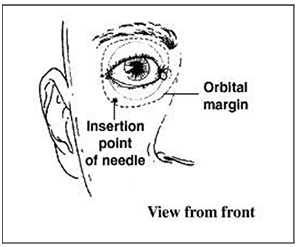
Figure 3
When the needle tip is judged to be past the equator of the globe the direction is changed to point slightly medial (20°) and cephalad (10° upwards) to avoid the bony orbital margin. Advance the needle until the hub (which is at 2.5 cm) is at the same depth as the iris. It is important to orientate the bevel of the needle facing the globe and any movement of the eye during needle insertion should alert the anaesthetist to possible globe penetration. Avoid any tendancy to ‘wiggle’ the needle to confirm the globe is disengaged as this only increases the risk of perforation.
Following negative aspiration, 5-8 ml of the solution is slowly injected. There should not be any resistance while injecting. If resistance is encountered, the tip of the needle may be in one of the extraocular muscles and should be repositioned. During the injection the lower lid may fill with the anaesthetic mixture and there may be some conjunctival oedema (chemosis).
Should the upper lid close quickly or the globe become tense or proptosed after only small volumes of local anaesthetic mixture the needle point is likely to be retrobulbar, and caution should be taken not
to inject further.
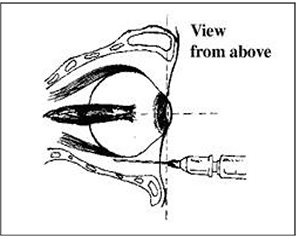
Figure 4
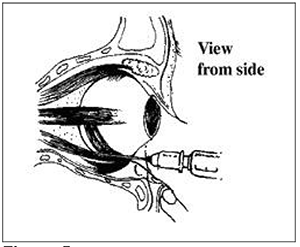
Figure 5
Within 5-10 minutes of this injection, most patients will develop adequate anaesthesia and akinesia. Some patients however may not and a top up injection can be given either at the same site or via a nasal approach.
Nasal injection (Figs 6 & 7)
The same needle is inserted through the conjunctiva on the nasal side, medial to the caruncule and directed straight back parallel to the medial orbital wall pointing slightly cephalad (20°) until the hub of the needle is at the same level as the iris.
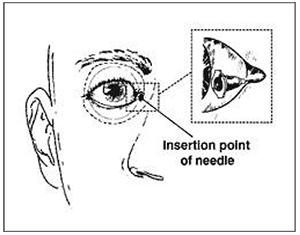
Figure 6
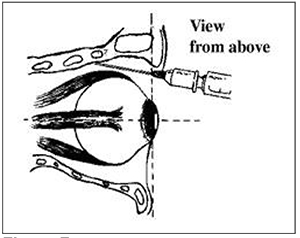
Figure 7
The needle traverses the tough medial canthal ligament and may require firm gentle pressure. This may cause the the eye to be pulled medially briefly. After negative aspiration up to 5ml of the anaesthetic mixture is injected.
The eye is then closed with adhesive tape. A piece of gauze is placed over the lids and pressure applied with a Macintyre oculopressor or Honan balloon for 10 minutes at a pressure of 30 mmHg. If no oculopressor is available gently press on the eye with the fingers of one hand. This is to lower intraocular pressure (IOP) by reducing aqueous humour production and increasing its reabsorbtion. Assessment of the block is usually judged after an interval of 10 minutes.
The signs of a succesful block are:
- Ptosis (drooping of the upper lid with inability to open the eyes)
- Either no eye movement or minimal movement in any direction (akinesia)
- Inability to fully close the eye once opened.
A simple akinesia score known as the Brahma score can be used for assessment of the block. Eye movement is assessed in four directions – inferior, superior, medial and lateral. Normal movement is scored at 3, partial movement at 2 and and flickering movement at 1 and no movement is scored at zero. A score of less than 2 is acceptable.
Since the local anaesthetic is placed outside the muscle cone the concentration around the optic nerve may not be sufficient to abolish vision completely. Some light perception will therefore remain, however the patient is not able to see the operation.
If, after 10 minutes the block is inadequate a supplementary injection of 2-5 ml of the anaesthetic mixture may be required. If the residual eye movements are downward and lateral, the supplementary injection is given at the inferotemporal site and if upward and medial, at the nasal site. Pressure is then reapplied for a further 10 minutes.
Care of patient. The patient must be made comfortable in the operating theatre using pillows and pads as required. An assistant should remain with the patient monitoring their condition and giving reassurance. Patients should be asked to remain silent and to squeeze the assistant’s hand before any movements are made in order to warn the surgeon. A right angle screen can be used to keep the drapes away from the patient’s face and to support an oxygen delivery system. A high flow of oxygen (8L/min) can be used to increase the FiO2 and prevent CO2 accumulation. Sedation is rarely required and should be limited to small increments of midazolam (1mg) or propofol (10mg). Oxygen saturation, ECG and blood pressure should be monitored throughout. Avoid oversedation of patients who may then wake up and move during the operation. The best approach is a thorough discussion with the patient of what will happen and what is required of them during the surgery. Any remaining doubts or worries should prompt consideration of a general anaesthetic approach.
Retrobulbar block. The conjunctiva is first anaesthetised as described under peribulbar block. The same 25G x 25mm needle is inserted half way between the lateral canthus and the lateral limbus in the lower conjunctiva. It is first directed backwards under the globe and then after the equator of the globe has been passed the needle direction is changed upwards and inwards to enter the space behind the globe between the inferior and lateral recti muscles. After confirming negative aspiration, 4-5 ml of local anaesthetic solution is injected slowly. The retrobulbar approach has largely been replaced by peribulbar block because of the higher incidence of complications (see below).
Complications
Complications of regional blocks for ophthalmic surgery may result either from the agents used or the block technique itself.
Intravascular injection and anaphylaxis can occur, hence resuscitation facilities must always be readily available.
Haemorrhage – retrobulbar haemorrhage is characterised by rapid orbital swelling and proptosis along with a sudden rise of IOP and usually requires surgery to be postponed. The surgeon should be informed immediately and the pulsation of the central retinal artery assessed. A lateral canthotomy can be performed to alleviate the rise in IOP. It is very rare with shallow retrobulbar or peribulbar injections (0.07%). Subconjunctival haemorrhage is less significant as it will eventually be absorbed.
Subconjunctival oedema (chemosis): This is un-desirable as it may interfere with suturing. It can be minimised by slowing the rate of injection. It rapidly disappears when gentle pressure is applied to the closed eye.
Penetration or perforation of the globe (<0.1%) – this is more likely to occur in myopic eyes which are longer but also thinner than normal and may have developed staphylomata. A diagnosis of perforation may be made if there is pain at the time the block is performed, sudden loss of vision, hypotonia, a poor red reflex or vitreous haemorrhage. Perforation may be avoided by carefully inserting the needle tangentially and by not going “up and in” until the needle tip is clearly past the equator of the globe.
Central spread of local anaesthetic – this is due to either direct injection into the dural cuff which accompanies the optic nerve to the sclera or to retrograde arterial spread. A variety of symptoms may follow including drowsiness, vomiting, contra-lateral blindness caused by reflux of the drug to the optic chiasma, convulsions, respiratory depression or arrest, neurological deficit and even cardiac arrest. These symptoms usually appear within about 5min.
Oculomedullary reflexes – discussed above
Optic nerve atrophy. Optic nerve damage and retinal vascular occlusion may be caused by direct damage to the optic nerve or central retinal artery, injection into the optic nerve sheath or haemorrhage within the nerve sheath. These complications may lead to partial or complete visual loss.
Regional versus general anaesthesia
Advantages –
May be performed as day cases.
Produce good akinesia and anaesthesia.
Minimal affect on IOP.
Requires minimum equipment.
Disadvantages –
Not suitable for some patients (children, mentally handicapped, deaf, language barrier).
Complications as above.
Depends on the skill of anaesthetist.
Unsuitable for certain types of surgery (e.g. open eye surgery, dacrocystorhinostomy-DCR).
Answers to MCQs
1. FTFFF
IOP is 1.3-2 kPa
Methohexitone is a short acting barbiturate used for induction of anaesthesia. It produces global depression of the CNS but may cause hyperexcitable phenomena and convulsions.
All intravenous induction drugs reduce IOP.
Suxamethonium may increase the pressure during the fasciculation phase.
Ecothiopate is an organophosphorus compound used to reduce plasma cholinesterase and reduce IOP in glaucoma
Atracurium and all non depolarising muscle relaxants reduce IOP. All volatile agents reduce IOP.
Atropine, if given as drops in glaucoma-prone eyes, increases IOP.
Acetazolomide inhibits carbonic anhydrase which leads to a reduction in the amount of aqueous humour produced in the eye to relieve glaucoma.
2. FTTFF
All types of eye surgery can be performed under local anaesthesia. The following are considered contraindications: 90 mins or longer duration, infants or children, mental retardation, excessive anxiety, uncontrolled cough and inability to lie flat.
3. TFTFF
4. TFTFT
The oculocardiac reflex is bradycardia following traction on the extraocular muscles especially the medial rectus. Although bradycardia is the commonest arrhythmia, ventricular ectopics or a nodal rhythm can also occur. It is most active in children. Retrobulbar block does not reliably obtund the reflex whereas local anaesthetic infiltration around the muscle does.
5. TFFFT
References
- A Varvinskiy, R Eltringham, Anaesthesia for Ophthalmic Surgery, Update in Anaesthesia, Issue 6 (1996), Article 3
- C Kumar, C Dodds & G Fanning -Eds, Ophthalmic Anaesthesia, Taylor & Francis, 2006
- K Allman & I Wilson – Eds, Oxford Handbook of Anaesthesia, Second Edition, Oxford University Press, 2006
- H Fischer & C Pinnock, Fundamentals of Regional Anaesthesia, Cambridge University Press, 2004
- Brahma AK, Pemberton CJ, Ayeko M et al. Single medial injection peribulbar anaesthesia using prilocaine. Anaesthesia 1994; 49: 1003-1005
- K. Elfituri, G Arthurs, L Gemmell, MCQs for the Primary FRCA, Cambridge University Press, 2008
- E Hammond, A McIndoe, QBase Anaesthesia 2, Greenwich Medical Media, 2005
- H Paw, QBase Anaesthesia 4, Greenwich Medical Media, 1998
- T Isitt, S Chieveley-Williams, Final FRCA Practice Papers, Pastest, 1999



