Basic Sciences
Questions
- In the fetal circulation:
- There are two umbilical arteries and one umbilical vein?
- Over 90% of blood passes the liver via the ductus venosus
- The foramen ovale divides the left and right ventricle
- The umbilical artery carries oxygenated blood from the placenta to the fetus
- The foramen ovale allows oxygenated blood to bypass the pulmonary circulation
- In the fetal circulation:
- The oxygen dissociation curve of fetal haemoglobin is shifted to the left compared with adult haemoglobin ensuring oxygen delivery to the fetus despite low oxygen partial pressures
- It is the presence of the ductus arteriosus and large pulmonary vascular resistance which ensures most of the right ventricular output passes into the aorta
- The patency of the ductus arteriosus is maintained by high oxygen tensions
- The patency of the ductus arteriosus is maintained by the vasodilating effects of prostaglandin G2
- 2,3-DPG levels are higher in fetal haemoglobin compared with adult haemaglobin
- Changes at birth include:
- a fall in pulmonary vascular resistance
- a rise in systemic vascular resistance with clamping of the cord
- an increase in hypoxic pulmonary vasoconstriction
- a rise in left atrial pressure
- closure of the ductus arteriosus within 24 hours
- The following congenital heart lesions are cyanotic:
- Ventricular septal defect
- Atrial septal defect
- Patent ductus arteriosus
- Tetralogy of Fallot
- Transposition of the great arteries
MCQ answers at end
Key points
- The fetal circulation supplies the fetal tissues with oxygen and nutrients from the placenta. It bypasses the fetal lungs.
- The presence of fetal haemoglobin (which has an oxygen dissociation curve shifted to the left compared with adult haemoglobin) ensures that oxygen delivery is maintained despite low oxygen partial pressures.
- At birth, the circulation of the fetal blood through the placenta ceases, acute changes in the pulmonary and systemic vascular resistance occur and the lungs begin to function.
- Subsequently the foramen ovale, ductus arteriosus and umbilical vessels close or transform into the corresponding ligaments.
- Neonates may revert to a persistent fetal circulation (PFC) with decreased pulmonary blood flow and a right to left shunt in response to certain stimuli such as hypoxia, hypercarbia, acidosis and cold.
- There are two categories of congenital heart disease (acyanotic and cyanotic) that result from structural, valvular and vascular abnormalities.
- Fetus (not foetus) is the etymologically correct spelling according to the Oxford English Dictionary.
Circulation in the fetus
- Deoxygenated fetal blood is conducted to the placenta via the two umbilical arteries. The umbilical arteries arise from the internal iliac arteries.
- Gas exchange occurs in placenta.
- Oxygenated blood from the placenta passes through the single umbilical vein and enters the inferior vena cava (IVC).
- About 50% of the blood in the IVC passes through the liver and the rest bypasses the liver via the ductus venosus. The IVC also drains blood returning from the lower trunk and extremities.
- On reaching the heart, blood is effectively divided into two streams by the edge of the interatrial septum (crista dividens) (1) a larger stream is shunted to the left atrium through the foramen ovale (lying between IVC and left atrium) (2) the other stream passes into right atrium where it is joined by blood from SVC which is blood returning from the myocardium and upper parts of body. This stream therefore has a lower partial pressure of oxygen.
- Because of the large pulmonary vascular resistance and the presence of the ductus arteriosus most of the right ventricular output passes into the aorta at a point distal to the origin of the arteries to the head and upper extremities. The diameter of the ductus arteriosus is similar to the descending aorta. The patency of the ductus arteriosus is maintained by the low oxygen tension and the vasodilating effects of prostaglandin E
- Blood flowing through the foramen ovale and into left atrium passes into the left ventricle where it is ejected into the ascending aorta. This relatively oxygen rich blood passes predominantly to the head and upper extremities.
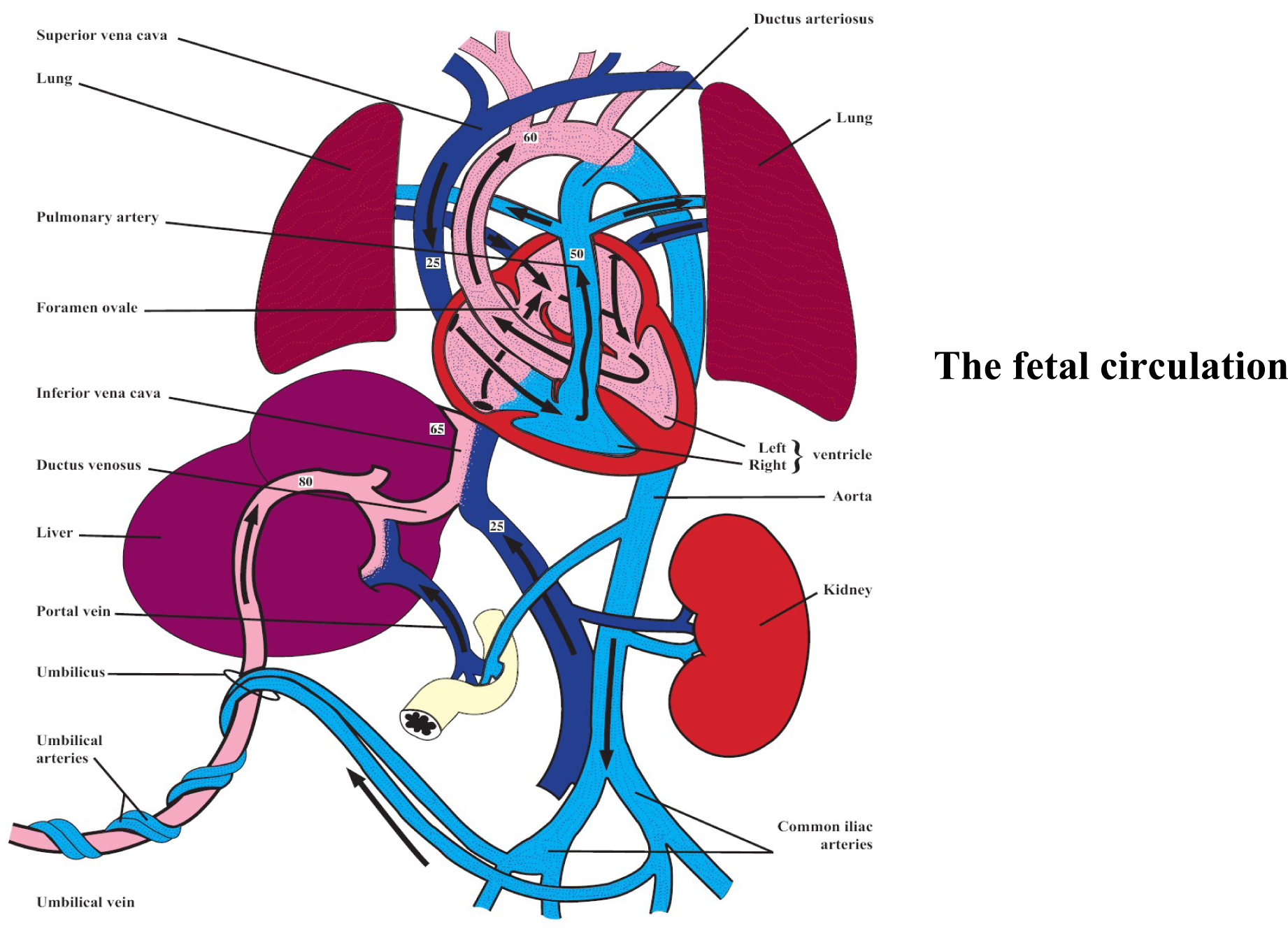
Murphy PG. The fetal circulation. Continuing Education in Anaesthesia, Critical Care & Pain 2005; vol 5 no 4: 107112. The Board of Management and Trustees of the British Journal of Anaesthesia. Reproduced by permission of Oxford University Press/British Journal of Anaesthesia.
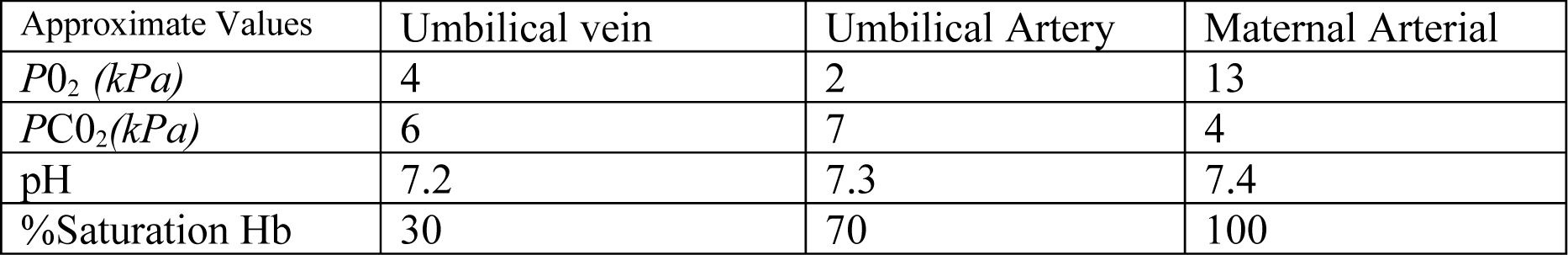
Fetal versus adult haemoglobin
- Fetus has high percentage (75%) of haemoglobin F (HbF).
- HbF has lower affinity 2,3-diphosphoglycerate (2,3-DPG).
- Fetus has a higher haemoglobin concentration (18g/dl-1) at birth.
- The oxyhaemaglobin dissociation curve for HbF is shifted to the left compared with adult haemoglobin due to a lower affinity for 2,3-DPG. This favours oxygen uptake in the placenta.
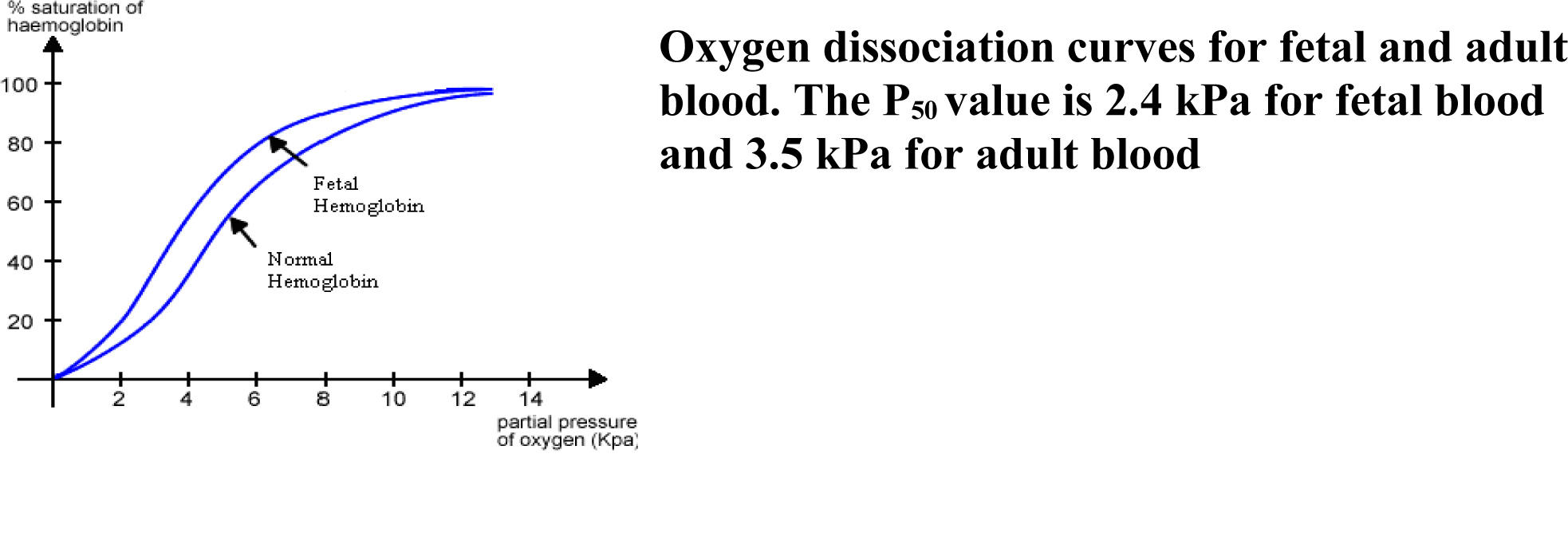
Reproduced by permission of Oxford University Press/British Journal of Anaesthesia.
Changes at birth
Several cardiopulmonary adaptations occur which result in gas exchange being transferred from placenta to the lungs.
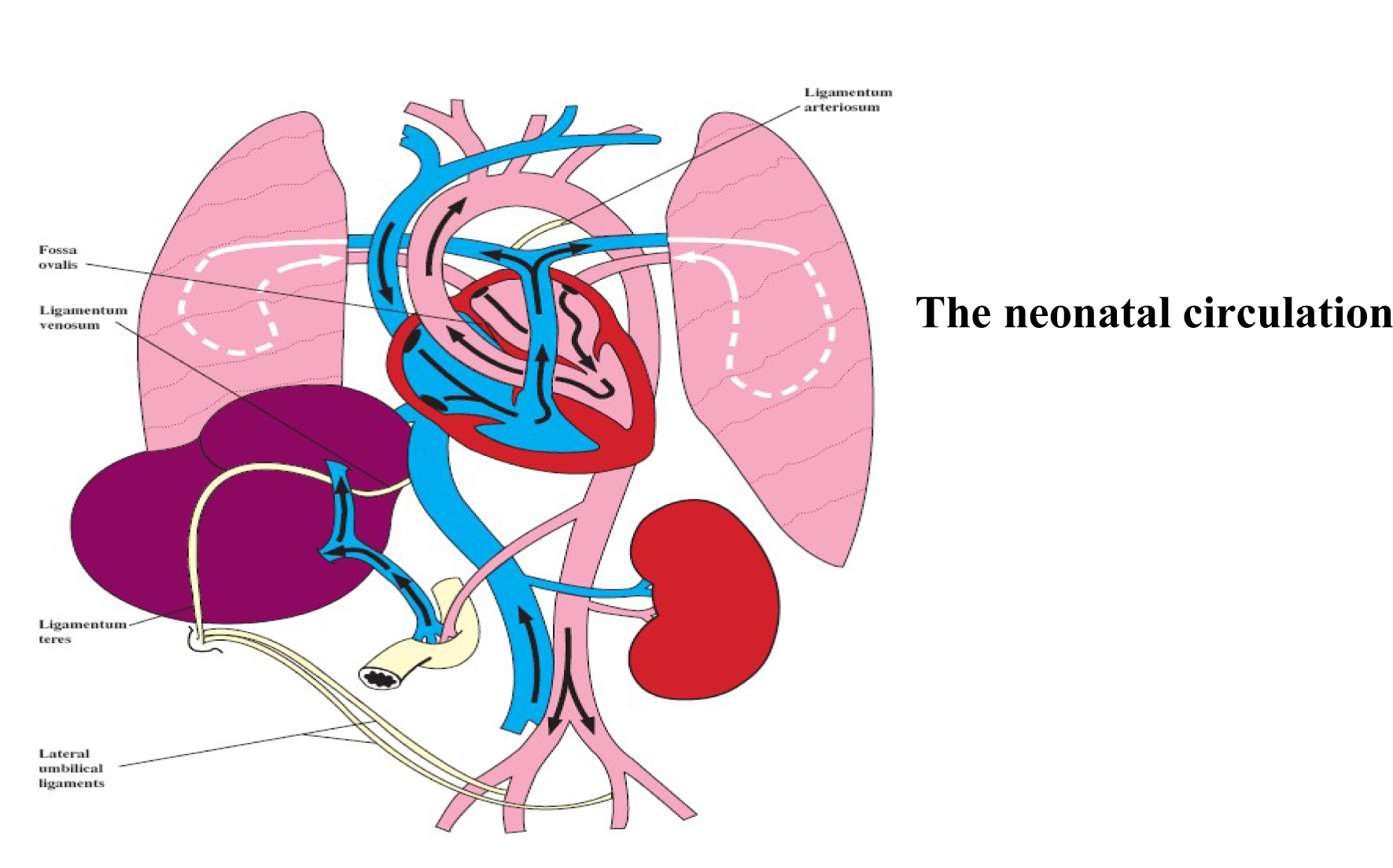
Reproduced by permission of Oxford University Press/British Journal of Anaesthesia.
- The umbilical vessels are obliterated when the cord is clamped externally.
- There is therefore a fall in blood flow through the IVC and the ductus venosus, the latter subsequently closes passively over the next 3-10 days.
- A dramatic fall in the pulmonary vascular resistance (PVR) occurs with lung expansion (opening up the pulmonary vessels). A reduction in hypoxic pulmonary vasoconstriction and stimulation of pulmonary stretch receptors contribute to this process.
- The increase in pulmonary blood flow leads to a large rise in pulmonary venous return to the left atrium.
- The left atrial pressure therefore exceeds the right atrial pressure. This reversal of pressure gradient across the atria allows the flap of the foramen ovale to push against the atrial septum and the atrial shunt is effectively closed. Although the initial closure of the foramen ovale occurs within minutes to hours of birth, anatomical closure by tissue proliferation takes several days. As a result, all blood from the right atrium now passes into the right ventricle.
- The ductus arteriosus constricts due to the high partial pressure of oxygen. The process is usually complete within 2 days after birth.
- Other changes over several weeks include a reduction in the thickness of the walls of right ventricle and the muscle layer of the pulmonary arterioles; and an increase in the left ventricular wall.
Persistent fetal circulation
Under certain circumstances, the newborn may revert back to a fetal-type circulation, a pathophysiological state termed Persistent Fetal Circulation (PFC).
In the presence of certain stimuli, the pulmonary arterioles will constrict and lead to an increase in Pulmonary Vascular Resistance (PVR). These stimuli include:
- Hypoxia
- Hypercarbia
- Acidosis
- Cold
The increase in PVR favours a right to left shunt and the foramen ovale and ductus arteriosus subsequently remain patent. In the absence of a placenta for gas exchange, it is clear that this scenario can lead to a catastrophic outcome in the newborn.
Congenital heart disease
Approximately 1% of neonates may be born with some degree of congenital heart disease although its effects may not be immediately obvious. Some babies will suffer catastrophic sequelae although others may lead an entirely normal life with the heart disease being discovered as an incidental finding (e.g. a small VSD). There are two broad categories of congenital heart disease – acyanotic and cyanotic congenital heart disease and it can be caused by a structural, valvular, vascular or mixed abnormality.
Acyanotic
Acyanotic is the most common type (75%) and is due to either obstructive lesions or left to right shunts
Structural
- Atrial septal defect (ASD) – defect between the two atria leading to oxygenated blood leaking from left to right atria.
- Ventricular septal defect (VSD) – defect between the two ventricles leading to oxygenated blood leaking from left to right ventricle. These lesions often close on their own in childhood or adolescence, however they may lead to pulmonary hypertension if there is a large defect, due to increased blood flow through the pulmonary circulation.
- Atrioventricular Septal Defect (AVSD)
- Patent Ductus Arteriosus (PDA) – If a large PDA is not closed, then increased flow will lead to increased pressure in the pulmonary arteries and can lead to Eisenmenger`s syndrome. This is a situation in which a reversal of flow (a right to left shunt) occurs.
Valvular
- Aortic Stenosis (AS)
- Pulmonary Stenosis (PS)
Vascular
- Coartctation of Aorta – narrowing of the aorta, usually, occurs distal to the arteries supplying the head and upper extremities.
Cyanotic
Cyanotic heart disease is due to abnormal blood flow from the right to the left part of the circulatory system (either at the level of the atria, the ventricles or the great vessels). This right to left shunt results in poor oxygenation of the tissues.
Structural
- Tetralogy of Fallot – This consists of four things; VSD, pulmonary stenosis, overriding aorta (which lies directly over the VSD) & right ventricular hypertrophy. A tetralogy requires surgical correction.
- Hypo-plastic left heart syndrome – Is underdevelopment of the left side of the heart chamber characterized by aortic valve atresia, hypo-plastic ascending aorta, hypo-plastic mitral valve and endocardial fibroelastosis (diffuse thickening of endocardium causing a restrictive cardiomyopathy).
Valvular
- Tricuspid atresia
- Pulmonary atresia – Children with tricuspid atresia and pulmonary atresia do not have effective forward flow of blood to the pulmonary arteries from the right ventricle. Survival is dependent on the patency of the ductus arteriosus (possibly augmented by prostaglandins) and blood flow to the aorta into the pulmonary arteries to ensure some oxygenation. Urgent palliation is undertaken by a modified Blalock-Taussig shunt which permits blood flow via the subclavian artery. Further surgery is subsequently required.
- Ebstein`s anomaly – Abnormal tricuspid valve leaflets which can lead to regurgitation of blood flow
Vascular
- Transposition of the great vessels – The aorta and pulmonary artery are reversed. The aorta therefore receives oxygen-poor blood from the right ventricle but it carries it back to the body without it becoming more oxygenated. Likewise, the pulmonary artery receives the well oxygenated blood from the left ventricle but carries it back to the lungs. Requires surgical correction early in life for survival
- Total anomalous pulmonary venous return – consists of an abnormality of blood flow in which all four pulmonary veins drain into systemic veins or the right atrium.
Mixed
- Truncus arteriosus – large VSD over which a large, single great vessel (truncus) arises. This single vessel carries blood both in systemic and pulmonary circulation
- Double outlet right ventricle – Both great arteries arise from left ventricle
Acknowledgments
We would like to thank Dr P Murphy for his permission us to use the illustrations featuring in this article
Suggested further reading
- Murphy PG. The fetal circulation. Continuing Education in Anaesthesia, Critical Care & Pain 2005; vol 5 no 4: 107-112
- Berne RM, Levy MN. Principles of Physiology 2000; 284-288
- Yentis SM, Hirsch NP, Smith GB. Anaesthesia and Intensive Care A-Z 2000; 206
Answers
- a) T b) F c) F d) F e) T
- a) T b) T c) F d) F e) F
- a) T b) T c) F d) T e) F
- a) F b) F c) F d) T e) T



