Intensive Care Medicine
QUESTIONS
Before continuing, try to answer the following questions. The answers can be found at the end of the article, together with an explanation.
- Name the triad of features associated with serotonin syndrome.
- How is serotonin syndrome diagnosed?
- What syndrome is a common misdiagnosis in the serotonergic patient?
- What is the most common combination of drugs associated with severe serotonin syndrome?
INTRODUCTION
Serotonin syndrome (SS) or serotonin toxicity was first described in the 1950’s. It is a spectrum of clinical findings ranging from benign to lethal that arise from an excess of serotonin in the CNS. Classically it involves a triad of abnormalities including; a) change in mental status, b) autonomic dysfunction and, c) neuromuscular excitability. The increasing use of serotonergic agents in the general community, most notably selective serotonin reuptake inhibitors (SSRIs), coupled with the fact the syndrome is a clinical diagnosis, may mean SS is under diagnosed. Multiple drugs used in daily anaesthetic practice involve manipulation of serotonin and hence it is important that anaesthetists consider this syndrome as a potential possibility when administering relevant drugs to susceptible patients. It is important to consider if the benefits of a drug’s administration outweigh the risks.
SEROTONIN
Production and metabolism
Serotonin (5-Hydroxytryptamine) is produced by hydroxylation and decarboxylation of tryptophan, an essential amino acid. Much of the serotonin released by serotonergic neurones undergoes reuptake and is inactivated by monoamine oxidase (MAO) to produce 5-hydroxyindoleacetic acid which is renally excreted. Serotonin can be found in platelets, in the gastrointestinal tract (primarily in enterochromaffin cells), and also in the brain (the hypothalamus, limbic system, spinal cord, retina and cerebellum).
Function
Seven distinct families of serotonin receptors have been identified (named, 5-HT1 through to 5-HT7). Some of these also have further subtypes. Most of the receptors are coupled to G proteins and produce an effect via adenyl cyclase or phospholipase C. The one exception is 5HT3, an ion channel. The effect of serotonin varies with each receptor. For example 5-HT2 receptors mediate platelet aggregation and smooth muscle contraction. 5-HT3 receptors are concentrated in the GI tract and the area postrema and are involved in vomiting. 5-HT6 and 7 receptors are involved in limbic function.
Serotonin syndrome is thought to particularly involve over stimulation of 5-HT1a and 5-HT2 receptors in the central grey nuclei and medulla.
SEROTONIN SYNDROME
Incidence and epidemiology
The incidence of serotonin syndrome is largely unknown and likely to be underestimated, however it has been increasing. This is thought to parallel the increasing use of serotonergic agents in medical practice. The reasons behind this unknown incidence have been described by Jones and Story (1). First, the diagnostic criteria are purely clinical and poorly validated. Second, many medical practitioners prescribing selective serotonin reuptake inhibitor (SSRI) antidepressants are unaware of the syndrome, mild cases may go undetected/reported and the signs and symptoms of the syndrome are often non-specific.
Signs and symptoms
A simple means of remembering the signs and symptoms of SS is to remember that patients CAN develop SS.
C Changes in conscious state (agitation, delirium, restlessness, disorientation, anxiety, lethargy, seizures, hallucinations).
A Autonomic dysfunction (diaphoresis, hypertension, hyperthermia, vomiting, tachycardia, dilated pupils, unreactive pupils, diarrhea, abdominal pain).
N Neuromuscular changes (myoclonus, tremor, muscle rigidity, hyperreflexia, nystagmus).
Other manifestations can include, rhabdomyolysis, acute renal failure, disseminated intravascular coagulation and circulatory failure. It is these more severe manifestations that are associated with fatal cases of the syndrome. Clinical features are highly variable but usually correlate with degree of toxicity and the onset can be dramatic or insidious in nature.
Diagnosis
The diagnosis is purely clinical. Several diagnostic criteria however have been proposed, the most validated is the Hunter Criteria. The Hunter area toxicology Service prospectively documented over 2000 cases of serotonergic drug overdose and from this devised a series of decision rules, as below:
The Hunter Criteria for Serotonin syndrome are fulfilled if the patient has taken a serotonergic agent and has one of the following:
- Spontaneous clonus
- Inducible clonus and agitation or diaphoresis
- Ocular clonus and agitation or diaphoresis
- Tremor and hyperreflexia
- Hypertonia
- Temperature above 38 degrees Celsius and ocular clonus or inducible clonus
The above criteria are stated to be 84% sensitive and 97% specific. The gold standard of diagnosis is examination by a medical toxicologist. Given it is a clinical diagnosis, history and examination are vital. The history should concentrate on prescription and other medications, illicit substance abuse, alternative medications and any recent changes to medications.
Laboratory investigations are of very little use in the diagnosis. Serum serotonin levels do not correlate with toxicity and other findings are generally non specific. For example, there may be an elevated white cell count and increased CK.
Differential diagnosis
Given the broad spectrum of signs and symptoms of SS there are multiple differential diagnoses including; neuroleptic malignant syndrome, anticholinergic toxicity, malignant hyperthermia, sympathomimetic toxicity and encephalitis. SS is most often mistaken for neuroleptic malignant syndrome. The table below highlights a few key differences.
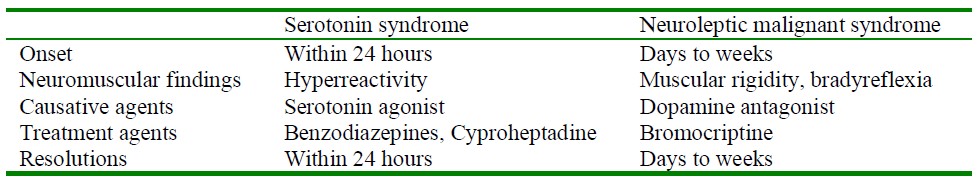

Table 1: Serotonin syndrome and neuroleptic malignant syndrome: distinguishing features. (Source: Up-to-date internet based resource).
Treatment
The first step in treatment is recognizing that the patient could have serotonin syndrome. Many references state that ceasing culprit drugs and supportive care is all that is required for treatment however as Gillman highlights, when both a MAOI and a SSRI have been co-ingested (even in low doses) rapid deterioration and death is well documented if appropriate intervention is not promptly initiated (2). The principles of treatment involve:
- Ceasing all drugs acting on serotonin (see list below).
- Supportive care including supplemental oxygen, intravenous fluids and cardiac monitoring.
- Agitation may be addressed using benzodiazepines which also have a positive effect on mild elevations of blood pressure and heart rate.
- Management of autonomic instability may be difficult but can be addressed with short acting agents such as esmolol.
- Controlling hyperthermia, which may require intubation, and ventilation with paralysis.
- Serotonin antagonists may be considered if available.
Cyproheptadine is the serotonin antagonist that has been used in cases of SS as an antidote. It is a histamine 1 receptor antagonist and has non specific 5HT-1 and 5HT-2 antagonistic properties. Cyproheptadine exists only in oral form, which complicates its use (but it can be given via a nasogastric tube). Substantial evidence to support cyproheptadine’s effectiveness is lacking. Chlorpromazine has also been used as an intravenous antidote given its 5HT-2 antagonistic properties.
Outcomes in serotonin syndrome are generally favorable as long as the syndrome is recognised and treated accordingly. As part of the treatment process once symptoms have resolved the need to reinitiate any serotonin based medications needs to be carefully considered.
SEROTONIN SYNDROME AND ANAESTHESIA
Serotonin drugs
The list of drugs that may precipitate serotonin syndrome is extensive and many are used on a daily basis in anaesthesia (See list below). The syndrome typically occurs with the co-administration of two serotonergic agents especially if the dose of one is escalated. It can also occur with monotherapy in susceptible patients and with overdose. The drug combination most commonly associated with severe reactions is that of monoamine oxidase inhibitors (MAOI) and selective serotonin reuptake inhibitors (SSRI).
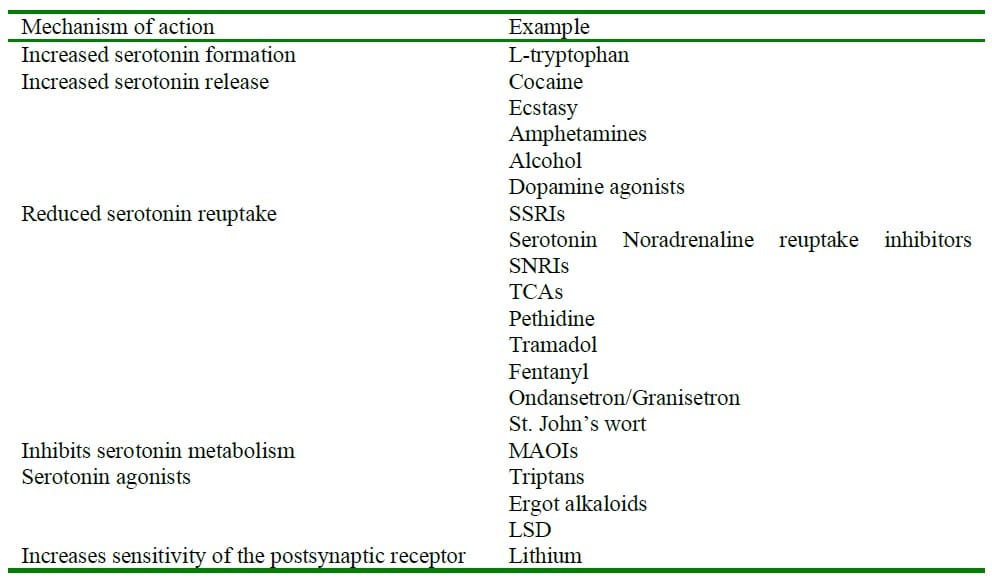
Table 2: Drugs that can precipitate serotonin syndrome
Implications for anaesthesia
Serotonin syndrome is uncommon, but is often undiagnosed in milder cases. Drugs that alter serotonin are given routinely in anaesthetic practice and are done so on a background of increasing use of SSRIs and SNRIs (serotonin noradrenaline reuptake inhibitors) amongst the general public. Tramadol is also gaining wider use among the public for acute and chronic pain in keeping with the theme of multimodal analgesia. Anaethetists are often the doctor prescribing/administering a second serotonergic agent. In order to avoid serotonin syndrome these combinations of drugs should be avoided, however, for various reasons this is not always possible. What is possible is to consider serotonin syndrome as a risk and then to assess the individual risk-benefit for each patient.
Recent case reports
Two recent case reports which illustrate these principles include:
- C.S.Altman, M.F. Jahangiri, Serotonin in the Perioperative Period; Anesth Analg; 2009
- S.L. Guo, T.J.Wu, C.C. Liu, C.C. NG, C.C. Chien and H.L.Sun, Merperidine-induced serotonin syndrome in a susceptible patient; British Journal of Anaesthesia; 2009;103 (3):369- 70.
IMPORTANT POINTS/SUMMARY BOX –
• Patients CAN develop serotonin syndrome after exposure to drugs prescribed by anaesthetists.
• Signs: Conscious state changes, Autonomic dysfunction, Neuromuscular dysfunction.
• The diagnosis is clinical and thus based on a thorough history and examination.
• Individual patient risk benefit analysis is vital when prescribing drugs that may cause serotonin syndrome.
ANSWERS TO QUESTIONS
- Classically serotonin syndrome involves a triad of abnormalities including a) change in mental status, b) autonomic dysfunction and, c) neuromuscular excitability.
- The diagnosis is purely clinical. Several diagnostic criteria for serotonin syndrome have been proposed, however the most validated is the Hunter Criteria.
- Serotonin syndrome is most often mistaken for neuroleptic malignant syndrome.
- The drug combination most commonly associated with severe reactions is those of monoamine oxidase inhibitors (MAOI) and selective serotonin reuptake inhibitors (SSRI).
WEBLINKS
REFERENCES and FURTHER READING
- D. Jones, D.A.Story, Serotonin syndrome and the Anaesthetist; Anaesth Intensive Care; 2005; 33:181-187.
- P.K.Gillman, Monoamine oxidase inhibitors, opioid analgesics and serotonin toxicity; British Journal of Anaesthesia; 2005; 95(4): 434-441.
- S. Chinniah, J.LH. French, D.M.Levy, Serotonin and anaesthesia; Continuing Education in Anaesthesia, Critical Care & Pain; 2008; 8 (2) 43-45.
- M. Hall, N. Buckley, Serotonin syndrome; Australian Prescriber; 2003; 26: 62-63.
- C.S.Altman, M.F. Jahangiri, Serotonin in the Perioperative Period; Anesth Analg; 2009
- S.L. Guo, T.J.Wu, C.C. Liu, C.C. NG, C.C. Chien and H.L.Sun, Merperidine-induced serotonin syndrome in a susceptible patient; British Journal of Anaesthesia; 2009;103 (3):369-70.
- M.T. Keegan, D.R. Brown, A.A.Rabinstein, Serotonin syndrome from the Interaction of Cyclobenzaprine with Other Serotonergic Drugs; Anesth Analg; 2006; 103: 1466-8.
- E.W.Boyer, Serotonin Syndrome. UpToDate. (www.uptodate.com)
- J.S. Jahr, J.D. Pisto, M.C. Gitlin, P.T. O’Neill, The Serotonin Syndrome in a Patient Receiving Sertraline After an Ankle Block; Anesth Analg; 1994; 79: 189-91.
- W.F. Ganong. Review of Medical Physiology; 2005 McGraw-Hill Companies.



