Paediatric Anaesthesia
QUESTIONS
Before continuing, try to answer the following questions. The answers can be found at the end of the article, together with an explanation. Please answer True or False:
- Pulmonary dysfunction can occur in spinal deformity. In regards to pulmonary function and scoliosis:
a. Restrictive lung disease may be diagnosed with pulmonary function testing showing elevated total lung capacity (TLC) and decreased forced expiratory volume (FEV1)
b. A preoperative FEV1 < 40% predicts a low risk of pulmonary complications after scoliosis repair
c. Preexisting pulmonary dysfunction improves rapidly in the immediate postoperative period after scoliosis correction
d. Postoperative pulmonary complications are greater in non-idiopathic compared to idiopathic forms of scoliosis
e. Residual volume is greatly decreased in patients with scoliosis - Surgical scoliosis correction has several potential complications. Regarding these complications:
a. Cardiac complications are more common with certain forms of non-idiopathic scoliosis
b. Postoperative pain is rarely an issue in scoliosis correction
c. Surgical correction of scoliosis is generally indicated with a Cobb angle greater than 40-45 degrees
d. Temperature monitoring is generally not necessary during scoliosis repair
e. Central retinal artery occlusion can occur with direct compression of the eye for a prolonged period of time - Regarding intraoperative neuromonitoring:
a. Volatile anaesthetics have no effect on SSEP or MEP monitoring
b. SSEP monitoring involves measuring signal transduction that begins with a stimulus at a peripheral nerve that generates a signal in the somatosensory cortex
c. Hypotension can cause changes in SSEP and MEP signals
d. Propofol has a greater effect on SSEP signals than Sevoflurane
e. Neuromuscular blockers rarely interfere with MEP monitoring
Key Points
- Scoliosis is common, occurring in 2-3% of the population. It may be classified as idiopathic, congenital or neuromuscular
- Advanced scoliosis can cause significant pulmonary or cardiac dysfunction. A thorough preoperative assessment must be performed and should include exercise tolerance and pulmonary function testing, which may reveal restrictive pulmonary disease
- Intraoperative considerations for scoliosis correction include careful patient positioning, preparing for significant bleeding, and considering options for intraoperative nerve monitoring
- Postoperative respiratory complications can occur and are more likely with congenital scoliosis and syndromic children, a greater degree of baseline curvature and pulmonary dysfunction
INTRODUCTION
Scoliosis is a condition of abnormal lateral curvature of the spinal column that affects nearly 2-3% of the population in varying degrees. It is distinct from hyperkyphosis, sometimes referred to as simply kyphosis, which is an abnormal anterior-posterior curvature in the thoracic region. The onset of scoliosis can be at birth but often begins manifesting itself in childhood or early adolescence, most often becoming evident between ages 10 and 15 years. It occurs slightly more often in females compared to males, and in females progresses to require surgical correction eight times as often. Scoliosis has been classified into several different types, which includes congenital, neuromuscular (cerebral palsy, spinal cord trauma, spinal muscular atrophy, spina bifida, muscular dystrophy, and others), and idiopathic (the most common form, 65% of cases).
Advanced curvature in scoliosis can lead to pain and multiple organ dysfunction. Prior to surgical correction, a thorough preoperative evaluation must be performed to assess the existing neurological status, and extent of organ system dysfunction. A detailed intraoperative and postoperative plan must be developed that takes into account patient comorbidities, need for intraoperative spinal cord monitoring, potential for blood loss, as well as anticipation of potential postoperative complications.
PREOPERATIVE EVALUATION
Because of the potential for significant pulmonary, cardiac, and neurologic comorbidities associated with advanced scoliosis, a detailed past medical history and physical exam for patients undergoing surgical correction is essential. Baseline exercise tolerance and respiratory function should be noted and serves as a general predictor of the ability to withstand the stress of a major operation. In evaluating the spine, it should be noted that the lateral curvature is usually right-sided (right convex) and commonly involves 7-10 vertebrae. If the curvature is left-sided (left convex) there is an increased likelihood of other comorbidities or congenital conditions e.g. of the spinal cord (20%), genitourinary system (20-33%), and cardiac conditions (10 -15%).
Pulmonary function
Preoperative evaluation should include assessment for the presence and severity of pulmonary dysfunction from restrictive lung disease. A thorough preoperative evaluation of pulmonary function is important, but not always possible, especially with severe cerebral palsy. The degree and severity of respiratory impairment depends on the underlying cause of scoliosis and associated comorbidities (such as neuromuscular disease), the speed of onset of scoliosis, and the degree of curvature. Decreased lung volumes, from restriction of diaphragm and chest wall movement due to alteration of the thoracic cavity from spine curvature, cause poor distribution of ventilation leading to hypercarbia, hypoxaemia, and infection.
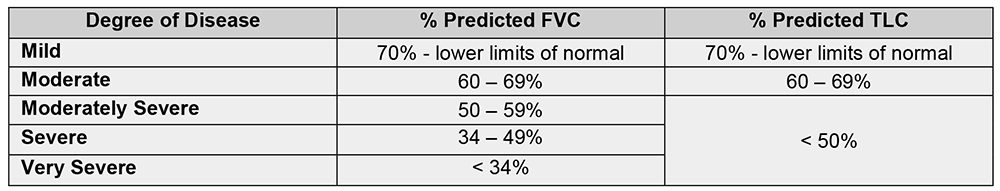
TABLE 1: Assessment of severity of restrictive lung disease using PFTs. FVC – Forced vital capacity, TLC – Total lung capacity
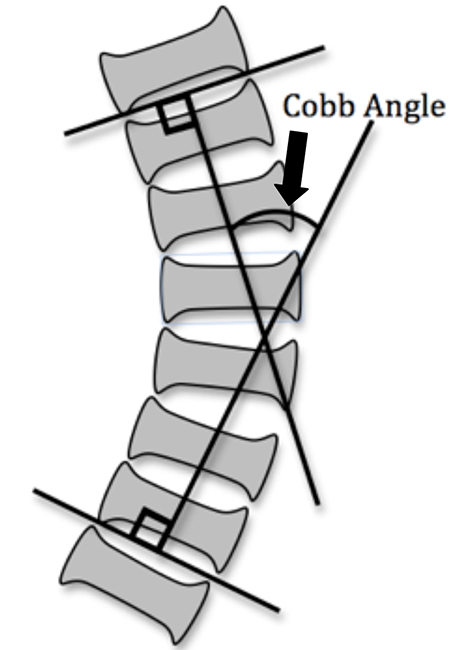
Figure 1: Assessment of Cobb angle for the degree of spinal curvature in scoliosis
Clinical signs and symptoms of significant respiratory impairment include dyspnoea with activity or at rest and inability to cough or clear secretions. Reduced chest wall compliance results in restrictive pulmonary disease, and exercise tolerance may be reduced even if lung volumes are normal. Pulmonary function testing (PFTs) can diagnose restrictive pulmonary deficits by demonstrating decreased forced expiratory volume in one second (FEV1), decreased forced vital capacity (FVC) with a normal FEV1/FVC ratio. Total lung capacity (TLC) is also decreased in patients with restrictive pulmonary disease. Residual volume is generally maintained in these patients.
A chest X-ray and other radiographic imaging can be helpful in assessing the severity of disease as well as the need for surgery. The Cobb angle is a measure of the greatest curvature of the spine, and surgery is generally indicated if the angle is greater than 45-50 degrees. In patients with idiopathic scoliosis, pulmonary function may remain normal until the curvature reaches 65 degrees. However, in patients with congenital and neuromuscular causes of scoliosis, pulmonary dysfunction is likely to occur at lesser angles. A curve of ≥ 100 degrees is likely to cause severe cardiac and respiratory dysfunction.
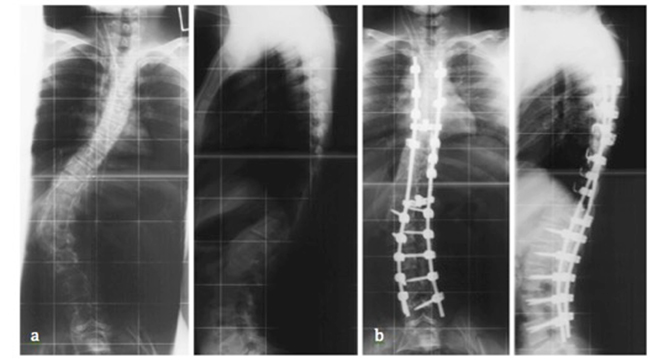
Figure 2. 16 year old female patient with an adolescent idiopathic scoliosis. a. Preoperative Cobb angle 50°, b, Postoperative Cobb angle 10 degrees. (J Child Orthop. Feb 2013; 7(1): 3–9 use approved by Creative Commons license http://creativecommons.org/licenses/by/2.0/legalcode).
Cardiac function
Cardiac function is an important consideration in certain cases. Although rare, in severe cases of scoliosis pulmonary dysfunction can progress to cause significant cardiac disease. Regional hypoventilation caused by abnormal diaphragm movement and, in severe cases, chronic hypercarbia and hypoxemia from advanced pulmonary disease can lead to pulmonary hypertension and failure of the right ventricle. In patients with scoliosis associated with neuromuscular diseases such as Duchenne muscular dystrophy and long chain acetyl carnation deficiency, their primary disease process can cause dilated cardiomyopathy with significant dysfunction. A history of significant exercise intolerance or physical examination evidence of jugular vein distension, hepatic congestion or lower extremity oedema should prompt evaluation of cardiac function with echocardiography, if available. Additionally, mitral valve prolapse may be present in 25% of children with scoliosis.
Non-idiopathic scoliosis
Patients presenting with non-idiopathic scoliosis require special consideration given the high likelihood of complex comorbidities related to their underlying disease process. Often, these patients have received specialised care with ongoing evaluation, which must be obtained and reviewed prior to surgery.
Non-idiopathic scoliosis can occur in several conditions, and three of the more common forms will be detailed here. Cerebral palsy is a non-progressive neurologic disease of foetal and neonatal brain development that presents with movement limitation and spastic paralysis often resulting in scoliosis. Patients with cerebral palsy often have some degree of cognitive impairment, which may be severe and limit their ability to cooperate with certain preoperative testing (such as pulmonary function testing) and preoperative preparation. Duchene muscular dystrophy (DMD) is a genetic disorder leading to progressive muscle degeneration. DMD presents with symptoms of proximal muscle weakness and pseudohypertrophy beginning in early childhood and advancing to skeletal deformity (including scoliosis), paralysis and cardiorespiratory failure. Mitochondrial diseases are a set of conditions that cause multiorgan dysfunction from inadequate cellular energy. These are genetic diseases caused by defects in mitochondrial metabolism, and can affect every body system, in some cases causing profound neuromuscular disease leading to scoliosis.
PREOPERATIVE PREPARATION
Because scoliosis correction is never an emergent operation, there is often time to optimise patients in preparation for surgery. This is of most benefit in patients with significant comorbidities. Nutritional status should be optimised to aid recovery and help correct any underlying anaemia. Any reversible causes of pulmonary disease such as asthma or pneumonia should be treated and controlled prior to surgery. Cardiac function should be optimised by ensuring adequate volume status and blood pressure control. Additionally, services that may be required in caring for the patient during and after surgery, such as the blood bank and intensive care unit, should be notified in advance to have time for adequate preparation and allocation of resources.
INTRAOPERATIVE MANAGEMENT
Surgical approach
There are three surgical approaches to scoliosis correction. The first is posterior spinal fusion with contoured or adjustable rods, which are commonly used for younger children and allow for lengthening over time. Fixed rods are more commonly used in older children. The second approach is anterior through a thoracoabdominal incision and involves removal of intervertebral discs or hemivertebrae contributing to abnormal curvature. Finally, a combined posterior fusion and anterior release sometimes employed, with the option of endoscopic anterior release in rare selected cases.
Monitoring and positioning for surgery
Standard monitors including ECG, NIBP, pulse oximetry, temperature, and capnography should be used as well as a Foley catheter for urine monitoring. Arterial catheterisation for blood pressure monitoring, cardiac output monitoring (e.g. LidCO) and intraoperative blood tests can also be considered if the patient has significant comorbidities or higher than normal blood loss is expected. Central venous pressure monitoring is used to help guide fluid resuscitation or when peripheral intravenous access is difficult, particularly in patients with syndromes or moderate to severe pulmonary or cardiac dysfunction. Central access is not usually required for patients with idiopathic scoliosis. BIS (EEG) monitoring is reassuring when using TIVA rather than volatile anaesthesia. For patients with cardiac failure related to an underlying disease, such as muscular dystrophy, close attention should be paid to factors that increase pulmonary vascular resistance, which could exacerbate right heart strain. These include acidosis, hypoxaemia, hypercarbia, and hypothermia.
Patient positioning can be challenging in these operations for several reasons, including the abnormal body habitus of patients with advanced disease and the need for exposure of a large area of the spine for posterior approaches. As with any patient in the prone position, the endotracheal tube and intravenous lines should be well secured and monitored for movement during the case. All pressure points should be padded. The chest and pelvis should be supported in such a way that the abdomen is free to move. Any increase in abdominal pressure can compromise venous return via the inferior vena cava. This may raise pressure in the epidural veins resulting in increased operative blood loss. Careful attention to avoid placing any pressure on the eyes during the operation is critical. Specialised tables (e.g. the Allen table) can be helpful.
Finally, these patients often have a large surface area exposed for a prolonged amount of time and require careful temperature monitoring to avoid hypothermia. Warmed intravenous fluids, forced air warmers, and elevated room temperature are commonly used to maintain normothermia.
Haemorrhage
Scoliosis correction often requires a large incision with removal of vertebral bone at multiple levels and can take many hours. In prone positioning the vertebral veins become engorged from abdominal pressure and can contribute to increased blood loss. Loss of up to one half of a patient’s blood volume or more is not unexpected, and planning for large volume haemorrhage throughout the case is necessary. This may include preoperative iron supplementation or erythropoietin for patients who are found to be anaemic prior to surgery. Autologous blood donation may be considered in institutions equipped with this capability. Intraoperative acute normovolaemic haemodilution is a technique used occasionally in adult patients in which 2-3 units of blood are removed at the beginning of the operation and an equal volume of colloid or three times the volume of crystalloid are infused into the patient making blood lost during the operation more dilute. At the conclusion of the operation, the blood removed at the beginning is transfused back into the patient. Cell salvage techniques (e.g. a Cell Saver machine, which suctions blood lost to be processed and available for transfusion) may also be considered.
Induced hypotension is a pharmacological technique that aims to maintain systolic blood pressure at or near 80. Some centres have utilised this technique to reduce the amount of bleeding during an extensive operation such as scoliosis correction. It is presumed that a lower perfusion pressure will lead to decreased blood loss during the surgery. However, this technique is associated with complications such as post-operative visual loss and anterior spinal ischaemia leading to postoperative paralysis, and therefore should be avoided in any patient with a high risk of complications from a relatively decreased blood flow to vital organs (kidneys, eyes, brain, heart)..
In patients with arterial access for blood pressure monitoring, stroke volume and cardiac output monitors using waveform analysis can provide more detailed information about haemodynamic status and help guide resuscitation. The Lithium Dilution Cardiac Output (LiDCO) System uses a measurement of lithium indicator dilution from venous to arterial circulation to provide an accurate assessment of cardiac output, and has been increasingly utilised to gauge volume status and guide resuscitation.
Respiratory function
As previously discussed, patients with severe forms of scoliosis may have worsened baseline respiratory status. This is unlikely to improve during or immediately after scoliosis correction and may make intraoperative and postoperative ventilation challenging. Significant postoperative atelectasis should be anticipated, and in severe cases of scoliosis controlled ventilation postoperatively may be required. Neuromuscular causes of scoliosis contribute to greater respiratory dysfunction than other causes due to respiratory muscle involvement. Finally, for intrathoracic approaches to correction, lung isolation using a double lumen tube, bronchial blocker, or endobronchial intubation may be required.
Nerve monitoring
Because scoliosis correction requires operation near the spinal cord, and thoracic and lumbar nerve roots, various techniques for intraoperative monitoring of nerve function have been developed. The goal of intraoperative neuromonitoring is to identify disruption in nerve signals quickly so that surgical adjustments can be made before the final spinal column configuration is set.
Specialised spinal cord function monitoring can be achieved by measuring evoked potentials. These are created by stimulating a peripheral nerve and measuring signals generated in the somatosensory cortex (somatosensory evoked potentials – SSEPs) or stimulating near the motor cortex and measuring signals at the target muscle (motor evoked potentials – MEPs). Intraoperative monitoring of these pathways allows for continuous assessment of the entire signal transduction pathway including cortex, spinal cord, and peripheral nerves, and allows the surgeon to make adjustments in real time during the operation if signals change. Importantly, our anaesthetic agents can have varying influence on the reliability of these signals developed for neuromonitoring. SSEPs and MEPs are disrupted by inhalational agents at greater than 0.5 MAC and also by nitrous oxide. Neuromuscular blockade disrupts MEP signals and nondepolarising neuromuscular blockers should be avoided with MEP monitoring. Because of the potential for signal disruption with volatile anaesthetics, cases with SSEP or MEP monitoring most commonly are done with a total intravenous anaesthetic (TIVA) technique. In order to assess the depth of anaesthesia more adequately, and avoid intraoperative awareness in the absence of MAC values based on end-tidal anaesthetic, a processed EEG monitor (e.g. Bispectral Index or BIS monitor) should be used during a TIVA. There are other factors that influence signal transduction and it is critical that the depth of anaesthesia be constantly maintained throughout the procedure. Hypoxia, hypercarbia, hypothermia and hypotension must be avoided. If the signal is disrupted, the surgeon should be notified immediately.
The most basic intraoperative test of nerve function is the wake-up test. Although not routinely used, awareness of the technique is important for historical reasons and for use in settings where neuromonitoring may not be available. In this test, the patient is awakened after correction rod placement to assess basic lower extremity nerve function. If neurological function is deemed intact, the patient’s anaesthetic is deepened and the operation completed. In order to be reliable, the patient must be able to follow simple motor commands. Anaesthetic technique should allow for rapid wake-up during and after the operation, and may be achieved with careful titration of an opioid-based general anaesthesia. If the patient does not respond during the wake-up test due to excessive opioid administration then gradual titration of naloxone until the patient is responsive to verbal commands may be necessary. Rapid-acting opioids such as remifentanil or sedatives that maintain responsiveness like dexmedetomidine may also be employed.
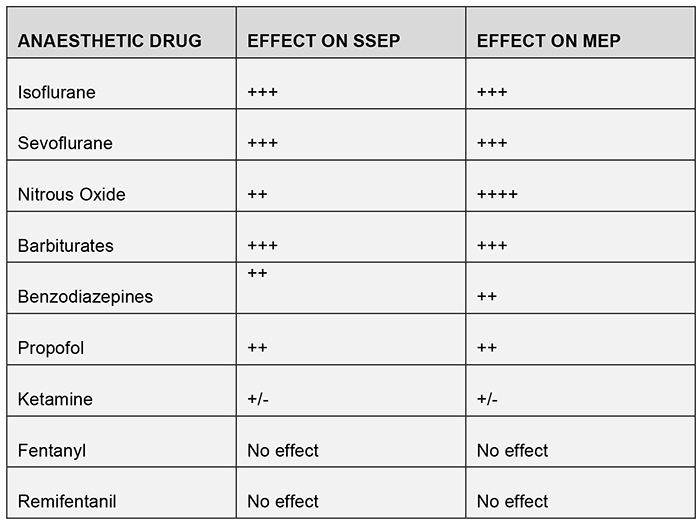
Table 2: Effect of different anaesthetic agents on neuromonitoring signals used in scoliosis correction
POSTOPERATIVE COMPLICATIONS
As previously mentioned, postoperative pulmonary complications can occur in scoliosis correction and are more likely in more severe disease or syndromic patients. While scoliosis correction may prevent further decline in respiratory status it is not likely to improve baseline function particularly in the immediate postoperative period. A patient with a preoperative vital capacity or FEV1 < 40% of expected may require postoperative controlled ventilation, while a VC or FEV1 ≥ 70% should have adequate pulmonary reserve to allow for immediate postoperative extubation. Respiratory status should be optimised postoperatively because atelectasis, hypoventilation, secretion retention, immobilisation, and analgesic medications can all worsen underlying pulmonary disease. Patients should be managed in a high dependency or specialised postoperative area familiar with spinal corrective surgery.
Postoperative pain management after scoliosis surgery can be challenging due to the large skin incisions and multiple osteotomies. Optimizing pain control for patient satisfaction and prevention of respiratory complications from hypoventilation is an important consideration. A multimodal approach to analgesia using acetaminophen (paracetamol), NSAIDs, gabapentin, ketamine, opioids and other available analgesics may improve outcomes. Patient-controlled analgesia has been reported to improve patient satisfaction. Intrathecal opioids or intraoperative epidural placement may also be considered, but must be weighed against the risk of pruritus in the case of intrathecal opioids and hypotension and impaired postoperative neurologic examination in the case of epidural catheter placement.
Another rare but potentially devastating postoperative complication from scoliosis correction that deserves attention is postoperative visual loss (POVL). POVL is rare in paediatric patients but can occur in any operation and is more common in operations where patients are prone or in steep Trendelenberg position for extended periods. It occurs in two distinct forms—ischaemic optic neuropathy (ION) and central retinal artery occlusion (CRAO). ION may be anterior (ischaemia of the optic nerve near the orbit) or posterior (ischemia of the optic tract towards the occiput) with posterior ION occurring three times as frequently. ION is associated with blood loss > 1000mL or 45% of estimated blood volume, operations lasting > 6 hours, preoperative anaemia, intraoperative hypotension, and intraoperative haematocrit < 30. Periorbital oedema from high volume crystalloid resuscitation may also contribute to ION. CRAO occurs from direct compression of the eye causing retinal ischemia. To prevent CRAO any direct pressure on the eye must be avoided.
OTHER NOTES ON SCOLIOSIS AND ANAESTHESIA
Patients with scoliosis often present for procedures unrelated to scoliosis correction with several significant implications for anaesthesia care. When patients with scoliosis are anaesthetized and positioned for surgery, careful attention must be paid to pressure points to avoid the development of nerve injuries and skin ulceration. Extra padding and support may be necessary to accommodate these patients whose spinal curvature may prevent usual positioning on a flat operating room table. Often a specialised operating table (e.g. an Allen table) with a chest pad, hip pad, thigh pad, head support and leg supports arranged on a frame is used.
Epidural and spinal drug placement in patients with lumbar or thoracic scoliosis presenting for procedures other than scoliosis repair can be particularly challenging. If possible, an area of the spine that has minimal abnormal curvature but still provides adequate coverage for anaesthesia or pain control should be selected for epidural placement. If this is not possible, then epidural or spinal placement may still be attempted but patients should be aware of the possibility of multiple attempts and increased risk of accidental dural puncture. When attempting neuraxial anaesthesia in a patient with scoliosis the trajectory of spinal curvature should be delineated by tracing the spinous processes around the desired level of approach. The intervertebral space is then often larger more laterally in the direction of the curvature away from midline (toward the convexity). If available, ultrasound may provide useful information about the best approach to the epidural or intrathecal space, alternatively injection may be done intraoperatively by the surgeon. Even after successful placement spread of medication into the epidural space may be unpredictable and often patchy or one-sided. Post operatively epidural anaesthesia may cause confusion when assessing neurological function and is now rarely used for this reason.
ANSWERS TO QUESTIONS
- a. False. Restrictive pulmonary disease is diagnosed by pulmonary function testing showing a decreased forced vital capacity (FVC) and decreased forced expiratory volume (FEV1). The total lung capacity (TLC) is also reduced.
b. False. A preoperative FEV1 < 40% indicates several pulmonary disease and may require postoperative ventilation after scoliosis repair.
c. False. Post-operative atelectasis, pain, opioid medications, sedation and other factors contribute to diminished post- operative pulmonary status in scoliosis repair.
d. True.
e. False. Although total lung capacity is reduced, residual volume is generally maintained in scoliosis. - a. True.
b. False. Because of the large incisions and multiple osteotomies required in scoliosis correction post-operative pain can be significant. Multimodal approaches to pain control can improve outcomes.
c. True.
d. False. Often a large surface area is exposed during scoliosis correction and temperature must be monitoring closely for hypothermia, especially is high volume resuscitation or transfusion is required.
e.True. - a. False. Volatile anesthetics disrupt both SSEP and MEP monitoring especially above 0.5 MAC and an opioid infusion or TIVA should be considered when neuromonitoring is used.
b. True.
c. True.
d. False. Sevoflurane and other volatile anesthetics have a greater effect on SSEP signals than propofol.
e. False. MEP monitoring relies on measuring signals conducted at the neuromuscular junction and will not be reliable with neuromuscular blockade.
WEBLINKS
- Anaesthesia for Spinal Surgery. Anaesthesia UK. http://www.frca.co.uk/article.aspx?articleid=100377. Accessed 3 Feb 2015.
- Scoliosis. Wheeless’ Textbook of Orthopedics. http://www.wheelessonline.com/ortho/scoliosis. Accessed 3 Feb 2015.
REFERENCES and FURTHER READING
- Davis PJ, Cladis PF, Motoyama EK. Smith’s Anesthesia for Infants and Children. “Anesthesia for Orthopedic Surgery.” Mosby Publishing, Philadelphia, PA. 2011.
- Gibson PR. Anaesthesia for the correction of scoliosis in children. Anaesth Intensive Care. 2004;32:548-559.
- Raw DA, Beattie JK, Hunter JM. Anaesthesia for spinal surgery in adults. Br. J. Anaesth. (2003) 91 (6):886-904.
- Sloan TB, Heyer EJ. Anesthesia for intraoperative neurophysiologic monitoring of the spinal cord. J Clin Neurophysiol. 2002 Oct;19(5):430-43.



