Paediatric Anaesthesia
QUESTIONS
Before continuing, try to answer the following questions. The answers can be found at the end of the article, together with an explanation.
- Pierre Robin syndrome is associated with the following conditions:
a. Cardiac anomalies
b. Macroglossia
c. Cleft palate
d. Micrognathia
e. Severe obstructive sleep apnoea occasionally requiring tracheostomy - The following are useful in predicting the difficult airway in the paediatric patient:
a. Mallampati
b. Thyromental distance
c. Mouth opening
d. Neck mobility
e. Size of tongue - Apert’s syndrome is associated with the following conditions:
a. Cardiac anomalies
b. Midface hypoplasia
c. Micrognathia
d. Increased incidence of difficult bag mask ventilation
e. Syndactyly - Down’s syndrome (trisomy 21) is commonly associated with the following conditions:
a. Atlanto-axial subluxation
b. Atrioventricular septal defects
c. Difficult bag mask ventilation
d. Difficult intubation
e. Micrognathia - The Airtraq:
a. Is an indirect laryngoscope
b. Is not suited to children with limited mouth opening
c. Is useful where neck movement is limited
d. Is a single use device
INTRODUCTION
A difficult airway in anaesthesia is defined as the clinical situation in which a conventionally trained anaesthetist experiences difficulties with facemask ventilation, tracheal intubation, or both (1).
The incidence of difficult mask ventilation in adults is 1.4 – 5% (2,3) but is fortunately less common in the non-obese child (4). This failure to achieve adequate mask ventilation is very important; evidence from closed claim studies suggests that the commonest cause of morbidity and mortality due to airway problems in paediatric patients is due to inability to ventilate rather than to intubate (5).
There are anatomical and physiological differences between the infant, child and adult that make even the normal paediatric airway difficult for the inexperienced anaesthetist, particularly in children under one year of age. The presence of a congenital or acquired problem involving the airway increases the risk to the patient and anxiety of the anaesthetist. Good preoperative assessment and preparation is therefore key to success of the management of the difficult airway in children.
The Association of Paediatric Anaesthetists of Great Britain and Ireland is developing guidelines on the management of the difficult paediatric airway, and these should be available in the near future (see www.apagbi.org).
PREDICTION OF DIFFICULT AIRWAYS IN CHILDREN
As in adults, difficult airways in children may be anticipated or unanticipated. Some form of difficult airway, either difficult bag-mask ventilation, or difficult intubation, may be anticipated in the following congenital or acquired disorders
Congenital disorders associated with difficult airways in children
Congenital disorders are rare and include genetic and chromosomal disorders. Conditions typically associated with difficult airways can be divided into those conditions associated with hypoplasia of the mandible, hypoplasia of the midface, or associated with a large tongue (macroglossia):
Hypoplastic mandible (micrognathia) – difficult intubation
- Pierre Robin sequence
- Treacher Collins
- Hemifacial microsomia (Goldenhar syndrome)
Midface hypoplasia – difficult bag-mask ventilation
- Apert syndrome
- Crouzon syndrome
- Pfeiffer syndrome
- Saethre-Chotzen syndrome
Macroglossia – difficult bag-mask ventilation AND difficult intubation
- Hurler’s/Hunter’s syndrome (mucopolysaccharidoses)
- Beckwith-Wiedemann syndrome
- Down’s syndrome
A brief description of some of the common syndromes associated with difficult airways is given in appendix 1
Acquired disorders associated with difficult airways in children
- Chronic obstruction:
- Tonsillar hypertrophy
- Glottic web
- Haemangioma
- Subglottic stenosis
- Acute obstruction:
- Infection (epiglottitis, retropharyngeal abscess)
- Foreign body aspiration
- Trauma
- Poor mouth opening or mobility of jaw, neck
- Temporomandibular joint disease e.g infection
- Spinal fusion
- Burns contractures
- Measles stomatitis.
PREOPERATIVE ASSESSMENT OF THE AIRWAY
Essential information can be gathered by careful pre-operative assessment through the history, physical examination and investigations. An important question to ask yourself is whether ventilation by facemask is likely to be difficult.
History
A clear history should be obtained to look for the following:
- Respiratory problems – such as snoring, noisy breathing, change of voice, recurrent croup, or sleep apnoea
- A history of feeding problems
- Prior surgery to face and neck
- History of previous anaesthetics. If possible, review the anaesthetic chart to assess ease of bag mask ventilation, grade of intubation and airway adjuncts used and any difficulties encountered
Physical Examination
A thorough preoperative examination should be performed and should include assessment of:
- Severity of respiratory distress
- Presence of hypoxemia (pulse oximetry, cyanosis)
- Inspiratory or expiratory stridor.
Physical examination of the airway should begin at the nares and proceed down the airway. Choanal stenosis can occur as an isolated finding and be life threatening in the newborn; it can also be associated with craniofacial anomalies, such as Apert and Crouzon syndromes. It is useful to assess the patency of the nasal airway if nasal intubation is to be carried out.
Airway examination should also assess:
- Mouth opening
- Presence of loose or protruding teeth
- Size of the tongue
- Presence of other soft tissue mass such as cystic hygroma or cysts in the mouth
- Mandibular size
- Neck mobility
- Temporomandibular joint movement
Many attempts have been made to predict difficult laryngoscopy in paediatric patients. These methods have variable sensitivity in children. The Mallampati score, described by Cormack and Lehane, is not practical to use in infants and young children due to poor cooperation. Kopp et al (6) studied the use of the Mallampati classification to predict to the glottic view on laryngoscopy in children and found that the Mallampati score does not accurately predict a poor view of the glottis during direct laryngoscopy in paediatric patients.
Standard values for thyromental and horizontal mandibular lengths do not exist for the paediatric population. Mandibular space assessment is used to predict difficult airways in older children only Careful clinical evaluation of the patient is essential, particularly examination of the child from the side to assess for micrognathia (7).
PRE-OPERATIVE INVESTIGATIONS
Measurement of oxygen saturation with a pulse oximeter is essential; other investigations may be useful. Most special investigations will require cooperation from the child, which is not always possible and therefore limits their use.
- Arterial blood gases may be useful to assess severity and progress of respiratory distress.
- Respiratory function tests may help to differentiate extrathoracic from intrathoracic obstruction
- Plain X-ray, CT scan or MRI may be useful in selected cases to diagnose of the cause or site of obstruction, or bony or soft tissue abnormalities.
- A sleep study may be useful to assess the severity of sleep apnoea, but is not routine. Overnight pulse oximetry may be more practical.
- It may be possible to visualise the larynx using nasoendoscopy if the child is co-operative.
THE ANAESTHETIC PLAN
Complications in airway management most commonly result from a failure to plan. Always have a plan A, B and C!
Consider:
- Signs suggesting congenital or acquired abnormality?
- Condition of the patient
- Well settled?
- Respiratory distress?
- In extremis?
- Upper respiratory tract infection?
- What are the surgical requirements – is an endotracheal tube mandatory?
- Do you have help?
- Do you have the appropriate equipment/ experience/personnel?
- Do you have ENT cover if necessary?
The anaesthetic plan should be individualised to the patient and the situation and expertise of the practitioner. A strong recommendation is made to maintain spontaneous respiration initially and to intervene in a step-wise manner. If difficulty with a mask airway is anticipated, the method of induction of anaesthesia should be considered carefully – for instance in children with Apert’s syndrome or adenotonsillar hypertrophy, breathing spontaneously on a facemask often leads to obstruction, but intubation is not usually a problem, so it would be reasonable to proceed with intravenous induction rather than inhalational induction. Conversely, children with Hunter or Hurler’s syndrome have a difficult mask airway AND difficult intubation – a careful inhalational induction is the wisest course.
Patient Preparation
Starvation times must be strictly adhered to prior to elective surgery.
A variety of premedication drugs are available:
- EMLA/Ametop cream to aid early intravenous cannulation
- Midazolam – 0.5 mg/kg PO, max dose 20mg. Sedatives may diminish genioglossus tone and worsen obstruction if present. Contraindicated in many patients with airway problems, particularly those with severe OSA.
- Atropine (0.02 mg/kg- max 500mg PO) or glycopyrrolate (0.05 mg/kg IV)
- H2 blockers such as ranitidine and/or metoclopramide may be given to those patients felt to be at risk for gastric aspiration.
If a difficult airway is anticipated it may be beneficial to obtain intravenous access on the ward prior to the child coming to theatre, to reduce tension for all concerned at the time of induction of anaesthesia.
In older children or adolescents, awake intubation with sedation may be considered. Judicious use of sedatives such as midazolam, remifentanil or fentanyl provide a cooperative, amnesic patient. However, this is technique is rarely performed in children as few will tolerate such a procedure.
ANAESTHETIC TECHNIQUE
Inhalation induction is usually our technique of choice in children with a difficult airway. Effective preoxygenation can be difficult in children so inhalational induction should be carried out with an FiO2 of 1.0 to maximise safety. Inhalational induction may be slow, and airway obstruction may occur or worsen due to the loss of airway tone as anaesthesia deepens. This can generally be resolved by careful positioning, opening the mouth, gentle application of jaw thrust, the use of an oro/nasopharyngeal airway or the application of 10-15 cm H2O of CPAP.
As the depth of anaesthesia increases the child’s ventilation can be gradually assisted and controlled. Once controlled mask ventilation has been demonstrated, neuromuscular blockade may be an option, depending on planned technique of intubation.
In rare cases, for example measles stomatitis or burns contractures causing severe neck flexion, surgical release of soft tissues may be carried out under a combination of ketamine sedation and local anaesthesia to facilitate intubation by conventional means.
Laryngeal Mask Airway (LMA)
The LMA plays an important role in the anaesthetic plan for management of difficult airway in children. It can be utilized to maintain the airway during inhalational anaesthesia or as a conduit for intubation using a fibreoptic scope. It can also be used in a cannot intubate/cannot ventilate situation.
INTUBATION TECHNIQUE
It is important to remember that a tool is not a plan. Having sophisticated equipment available is not sufficient; a clear management strategy should discussed in advance with the team.
Bougies
Bougies are available in a number of sizes and are used in the same way as in adults. They can be an excellent aid in difficult intubations. Paediatric bougies are often flimsy due to their decreased diameter and may require someone to steady the proximal end.
Direct Laryngoscopy
The first attempt at laryngoscopy should be performed under optimal conditions, with the head and neck placed in the optimal position (neck flexed, head extended). Neonates have a large occiput and may benefit from a shoulder roll; a pillow should not be used for infants and small children, as this tends to flex the neck too much. The level of anaesthesia should be adequate and the patient should be well oxygenated. The paediatric larynx is more anterior and cephalad than in an adult, and external laryngeal manipulation may be useful to obtain a good view at laryngoscopy (8). A straight blade laryngoscope is recommended in neonates due to their large U-shaped floppy epiglottis, using the blade to pick up the epiglottis. If muscle relaxants are not used, take care that you do not provoke laryngospasm during manipulation of the airway; if muscle relaxants are used, an adequate depth of anaesthesia must be maintained at all times, and the relative merits of suxamethonium versus a short-acting non-depolarising muscle relaxant should be considered.
There are currently no published algorithms for managing difficult intubation in the paediatric population. In line with adult practice, we suggest that total intubation attempts should be limited to three as the paediatric airway is very susceptible to trauma, and a can’t intubate situation may develop quickly into can’t intubate and can’t ventilate if the airway becomes oedematous. Children and infants will desaturate more quickly than adults, and the child must be ventilated between each intubation attempt to maintain oxygenation as well as an adequate level of anaesthesia (8).
When to use direct laryngoscopy:
- Suspected but not confirmed difficult direct laryngoscopy.
- Previously difficult airway but history, examination and interval since last intubation attempt suggests direct laryngoscopy may be feasible.
When not to use direct laryngoscopy:
- Recent direct laryngoscopy confirms very difficult view
- History/examination is highly predictive
- When direct laryngoscopy risks making the airway oedematous e.g. planned fibreoptic intubation
Fibreoptic intubation
This can be done either awake (rare in paediatric practice) or after inhalational induction, with the bronchoscope introduced via a special adapter valve connected to the breathing circuit (either via a facemask or LMA).
Ultra-thin fibreoptic bronchoscopes are available with external diameter of 2.2 mm, which can accommodate a 2.5 endotracheal tube. For older children, a paediatric fibreoptic bronchoscope is utilized that can accommodate size 4.5 endotracheal tube. If there is only an adult scope available, or if the scope is too large to place in the trachea, a wire may be passed through the suction port to facilitate anterograde intubation with a small tube. It can be particularly frustrating using the oral approach due to the lack of plastic airway guides for paediatric patients; the tongue may fall back and defeat the endoscopist. It is helpful to use the nasal route or have an assistant to pull the tongue forward using forceps or a laryngoscope.
Alternatively, intubation using an LMA and exchange catheter may be performed. The LMA provides a patent airway, a conduit for the bronchscope and a means to control ventilation at the same time. The greatest challenge encountered when intubating through an LMA is its removal without dislodging the endotracheal tube, since the length of the endotracheal tube and LMA are similar. The proximal end of the tube tends to disappear into the LMA once the tube has passed through the vocal cords. A technique of LMA guided fibreoptic intubation with the use of a guide wire has been described (9). In this technique the fibreoptic scope is inserted through the LMA and the guide wire passed through the suction port of the scope (see fig 1). Once the guide wire is advanced into the trachea both the LMA and fibreoptic scope are removed, holding the guide wire in place. The endotracheal tube is then advanced over the wire and the guide wire is removed.
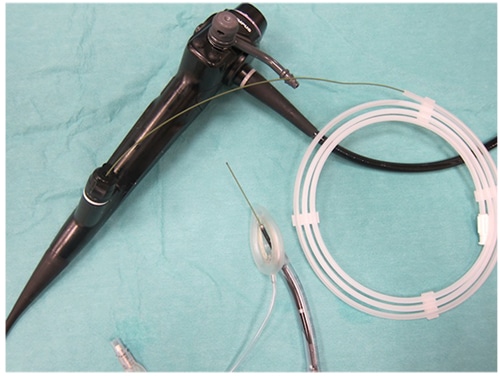
Figure 1: Use of LMA for difficult intubation. The guide wire is passed through the suction port of the fibreoptic bronchoscope.
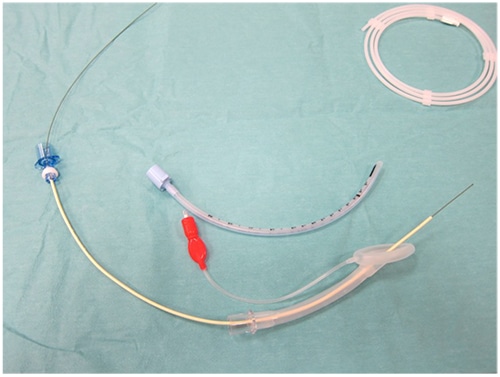
Figure 2. An airway exchange catheter may be passed over the guide wire to assist intubation
An airway exchange catheter can be used in older children (figure 2). This device is specifically designed for difficult intubation. It fits over the guide wire and incorporates a connector for a breathing circuit that may be used during intubation. The fibreoptic scope is passed into the trachea via the LMA, and the wire passed down the suction port as already described. The fibreoptic scope and LMA can then be safely removed and the exchange catheter is passed over the guide wire. A breathing circuit is attached allowing the child to be ventilated gently before the endotracheal tube is passed over the exchange catheter and the catheter is removed. The exchange catheter is long and relatively rigid and great care should be taken not to advance the catheter beyond the trachea.
The advantages of fibreoptic intubation:
- The “gold standard” for difficult airway management
- The most versatile instrument
- Improved image quality with new scopes increase success
- Especially useful when decreased mouth opening is present
- The LMA may be a useful adjunct in fibreoptic bronchoscopy
Limitations:
- Optical problems with fogging, blood, or secretions
- Not intuitive
- Significant learning curve
- Requires practice to acquire and maintain skills
- Expensive
- Fragile
- Not always available
Indirect Laryngoscopy
While similar to direct laryngoscopy, the use of specialised laryngoscopes for indirect visualisation of the larynx requires a different skill set. Indirect laryngoscopy may be useful for children with fixed flexion deformities, and the equipment is portable and can be used from neonates to adults. A common problem encountered is that the anaesthetist can obtain an excellent view of the glottis but still has trouble advancing the tube into the trachea.
Bullard laryngoscope:
This was the first indirect laryngoscope designed for difficult airways. It incorporates a fibreoptic bundle at the end of a broad hockey shaped blade. The tip is inserted into the vallecula and the device used to lift the base of the tongue upward to expose the larynx.
AirTraq®
The AirTraq Optical Laryngoscope® is an intubation device that uses magnifying wide-angle mirrors, a LED light source, and a tracheal tube guide channel to aid visualization and passage of an endotracheal tube. The AirTraq® is available in adult and paediatric sizes and may also be used to guide the placement of a bougie over which the tracheal tube can then be passed (figure 3 and 4)

Figure 3 AirTraq laryngoscopes in adult and paediatric sizes
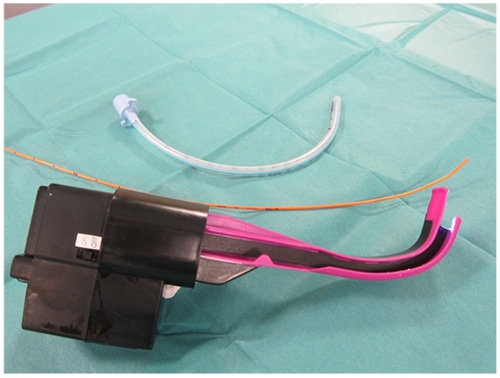
Figure 4. AirTraq may be used to guide placement of a bougie over which the tracheal tube is passed
Advantages of the AirTraq®:
- Incorporates a lens warmer that prevents fogging
- Only completely disposable single-use optical laryngoscope
- Inexpensive
- Portable
- Easy to set up
- Well suited for non-operating room settings
Limitations of the Airtraq®
- Best for oral intubations
- Good mouth opening is required
- Learning curve
- Can lose landmarks when attention is directed through the eyepiece
- Needs caution with insertion into the mouth
- Sometimes difficult to pass tracheal tube despite excellent view
Glidescope®
The Glidescope® is another indirect laryngoscope that is available for use in children.
- Reusable video baton that slides into disposable plastic blades/handles
- Similar to Macintosh blade design
- Warming at lens limits fogging
- Relatively portable
- Simple to set up
- Intuitive use
Limitations of the Glidescope®:
- Some mouth opening is required
- Learning curve
- Sometimes difficult to pass tracheal tube despite excellent view
- Caution required when inserting scope and styletted tube
It would be difficult to master every technique mentioned above. It is advisable to familiarise yourself with one technique and one escape route and gain expertise on healthy patients with normal airways. Fibreoptic intubation is useful in virtually all difficult airway patients.
Once the airway has been secured, it is important to document findings and the methods used to secure the airway on the anaesthetic chart, describing which techniques worked and which did not. The parents should be informed of the difficulties encountered, and they should be given a written record to pass on to the next anaesthetist.
ESCAPE ROUTE
Waking the child up should always be considered if a difficult airway is encountered.
As already mentioned, the LMA is an excellent escape route in the cannot intubate /cannot ventilate situation.
Every anaesthetist should be familiar with a technique for emergency transtracheal oxygenation. The use of emergency percutaneous techniques are controversial in children, mainly due to technical difficulties both with identifying the cricothyroid membrane (CTM) and insertion of a transtracheal airway. Although cricothyroidotomy as a rescue technique is very rarely employed in children, it may on occasion prove to be life saving, so every anaesthetising location must have the necessary equipment. The recommended technique is to insert a large bore intravenous cannula through the CTM or in infants, between the tracheal rings, and connect it to some form of ventilation. Adequate oxygenation can be maintained until a formal airway is secured (tracheostomy, endotracheal tube or wake the patient up). It is important to allow adequate exhalation time to avoid over inflation of the lungs, especially if upper airway obstruction exists.
Audit of airway complications in children in the UK in NAP4 has shown that formal surgical tracheostomy is used in most cases rather than cricothyroidotomy (10).
THE “DIFFICULT EXTUBATION”
An awake extubation is generally indicated in the difficult airway. Consider the possibility of airway oedema, especially after repeated attempts at intubation and administer dexamethasone 0.25 mg/kg IV, (maximum 8 mg) after the airway is secured.
A plan for a failed extubation should also be formulated. Consider short-term use of a reintubation guide, in the form of an airway exchange catheter in adolescents or a guide wire in infants and children. This can be placed via the endotracheal tube prior to extubation, and in the case of a failed extubation an endotracheal tube can be railroaded back into the trachea.
SUMMARY AND IMPORTANT LEARNING POINTS
- Micrognathia is a common feature of difficult intubation in children
- The most important consideration is whether ventilation by facemask will be possible.
- Always have a plan A, B and C.
- Whenever possible use an inhalational technique and keep the child breathing spontaneously
- Repeated attempts using a technique which has failed has little logic. Alternative techniques should be considered.
- Familiarize yourself with one technique of indirect laryngoscopy by practicing it in children with normal airways.
ANSWERS TO QUESTIONS
- TFTTT
Pierre Robin Sequence is characterised by micrognathia, glossoptosis and cleft palate. It is sometimes associated with cardiac anomalies. - FFTTT
Mallampati score does not accurately predict a poor view of the glottis during direct laryngoscopy in paediatric patients. Standard values for thyromental and horizontal mandibular lengths do not exist for the paediatric population. - TTFTT
Children with Apert’s syndrome have midface hypoplasia/hypertelorism, syndactyly and a 10% incidence of cardiac defects/genitourinary anomalies. Bag mask ventilation may be difficult but intubation is not usually difficult. A smaller size endotracheal tube may be required - TTTFF
Children with Down’s syndrome have macroglossia, atlanto-axial subluxation and cardiac anomalies. They can often be difficult to bag mask ventilate due to the macroglossia but are not usually difficult to intubate. - TTTT
The Airtraq is an example of a single use indirect laryngoscope. It is useful in situations where neck movement is limited. However good mouth opening is required for it to be used successfully.
FURTHER READING
- American Society of Anesthesiologists Task Force on Difficult Airway Management. Practice Guidelines for Management of the Difficult Airway: An Updated Report by the American Society of Anesthesiologists Task Force on Management of the Difficult Airway. Anesthesiology 2003 98: 1269-1277
- Kheterpal et al. Incidence and predictors of difficult and impossible mask ventilation. Anesthesiology 2006; 105:885-913.
- Langeron et al. Prediction of difficult mask ventilation. Anesthesiology 2000 92:1229 –36
- Tait AR et al. Incidence and risk factors for perioperative adverse respiratory events in children who are obese. Anesthesiology 2008 108:375-80.
- Jimenez N, Posner KL, Cheney FW et al. An update on pediatric anesthesia liability: a closed claims analysis. Anesth Analg 2007 104: 147–153
- Kopp VJ, Bailey A, Valley RD et al. Utility of the Mallampati classification for predicting difficult intubation in paediatric patients. Anesthesiology 1995 83: A1146.
- Gupta S, Sharma R, Jain D Airway Assessment: Predictors of difficult airways. Indian J. Anaesth. 2005 49 (4): 257 – 262
- Weiss M. and Engelhart T. Proposal for the management of the unexpected difficult pediatric airway. Pediatric Anesthesia 2010 20: 454–464.
- Welburn MB, Cornes J. Ryder IG. Fibreoptic intubation through a laryngeal mask airway facilitated by a guide wire. Anaesthesia 2000 55: 1027-28
- The Royal College of Anaesthetists National Audit Project: Major complications of airway management in the UK(NAP4) http://www.rcoa.ac.uk/docs/NAP4_Section1.pdf (accessed 31st December 2011)
- Paediatric Anaesthesia: The paediatric airway. Themed edition. 2009 19: 1-197 (http://onlinelibrary.wiley.com.libproxy.ucl.ac.uk/doi/10.1111/pan.2009.19.issue-s1/issuetoc)
APPENDIX 1
Syndromes associated with mandibular hypoplasia
Pierre Robin sequence
Features:
- Micrognathia
- Glossoptosis (backward displacement of the tongue)
- U-shaped cleft palate
- Associated cardiac abnormalities – pulmonary stenosis, patent ductus arteriosus, patent foramen ovale
These patients may present for tracheostomy in early infancy if the glossoptosis or micrognathia causes airway obstruction with apnoea. Cleft palate repair is usually performed at around 9 months of age.
Airway problem:
- Difficult bag mask ventilation and intubation
Treacher Collins syndrome
Features:
- Bilateral malar and mandibular hypoplasia associated with obstructive sleep apnoea (OSA) or airway obstruction whilst awake
- Malformation of external pinna and ear canal
These patients may present in early childhood for mandibular and maxillary advancement osteotomies for functional and cosmetic benefit.
Airway problem:
- Difficult intubation, which may be worsened by corrective surgery
Goldenhar syndrome
Features:
- Asymmetrical malar, maxillary and mandibular hypoplasia
- Auricular and ocular defects
- Cardiac defects – ventricular septal defect or tetralogy of Fallot
These children present for reconstructive surgery of their mandible or external ear
Airway problems:
- Induction of anaesthesia may be difficult – including maintaining an airway, laryngoscopy and intubation
- Mouth opening has cleft like extension on the affected side – mask fit may be a problem
Syndromes associated with midface hypoplasia
Crouzon syndrome
Features:
- Premature fusion of multiple cranial sutures
- Maxillary hypoplasia
- Orbital proptosis
- Hypertelorism (widely spaced eyes)
These children present for craniofacial surgery and for maxillary advancement osteotomies
Airway problem:
- Difficult facemask ventilation, intubation not usually difficult
Apert syndrome
Features:
- Irregular premature fusion of multiple cranial sutures
- Midface hypoplasia/hypertelorism
- Syndactyly
- Possible choanal stenosis
- Progressive calcification of hands, feet and cervical spine
- 10% incidence of cardiac defects/genitourinary anomalies
These children present for craniofacial surgery, microlaryngobronchoscopy (MLB), stenting of choanal stenosis, as well as for repeated hand surgery
Airway problem:
- Bag mask ventilation may be difficult but intubation is usually straightforward. A smaller size endotracheal tube may be required
Conditions associated with limited neck movement
Down’s syndrome
Features:
- Macroglossia
- Atlanto-axial subluxation
- Cardiac anomalies, particularly atrioventricular septal defect
These children commonly present for cardiac, ENT and dental related procedures. They may also present for treatment of haematological malignancy, duodenal atresia, Hirschsprung’s disease, or for spinal fixation.
- May be difficult bag mask ventilation due to macroglossia. In children with atlanto-axial instability, need to maintain in-line neck stabilisation
Osteopetrosis
Features:
- Bones become increasingly dense
- Limited mouth opening
- Limited neck movement
- OSA
These children may present for tracheostomy due to OSA or for vascular access for feeding
Airway problem:
- Difficult bag mask ventilation and intubation
Tracheal abnormalities
Children with laryngeal or tracheal abnormalities present difficulties with passage of a tracheal tube through the larynx, although visualisation of the larynx may not be difficult.
Congenital subglottic stenosis
Features:
- Incomplete recanalization of the laryngotracheal airway during the third month of gestation
Clinical presentation: stridor. These children present with recurrent stridor that becomes worse with upper respiratory infection or as the child grows. Differential diagnosis is recurrent croup. They may present for MLB +/- dilatation, laryngeotracheal reconstruction or tracheostomy.
Airway problem:
- Difficult intubation (laryngoscopy usually normal); requiring smaller size endotracheal tube
Acquired subglottic stenosis
Caused by trauma to the subglottic structure secondary to endotracheal intubation, but may also be due to a foreign body, infection or chemical irritation. Scar tissue is formed when healing takes place that may contract circumferentially to produce narrowing or severe stenosis.
As for children with congenital subglottic stenosis, these children present with stridor that may become worse with upper respiratory infection. MLB required for diagnosis. Severe subglottic stenosis may require laryngeotracheal reconstruction as for congenital subglottic stenosis.



